Rhinology

On this page
🏗️ Rhinology Foundations: The Nasal Architecture Blueprint
You'll master the nasal cavity as an integrated system-from its elegant architectural design and self-cleaning mucociliary machinery to the pattern recognition skills that separate common rhinitis from life-threatening infections. This lesson builds your diagnostic framework through anatomical reasoning, connects local pathology to systemic disease, and equips you with evidence-based treatment algorithms that transform you from observer to confident decision-maker in rhinological care.
The paranasal sinuses form an interconnected pneumatic system comprising four paired cavities: maxillary, ethmoid, frontal, and sphenoid sinuses. These air-filled spaces reduce skull weight by approximately 15% while maintaining structural integrity through architectural engineering principles.
📌 Remember: MEFS - Maxillary, Ethmoid, Frontal, Sphenoid represent the four paired paranasal sinuses, with maxillary sinuses being the largest (15-20 mL capacity) and most commonly affected by inflammatory disease
The ostiomeatal complex (OMC) serves as the critical drainage pathway for anterior ethmoid, maxillary, and frontal sinuses. This narrow anatomical corridor measures only 2-4 mm in width, making it vulnerable to obstruction from minimal mucosal swelling.
- Primary Drainage Pathways
- Middle meatus: Anterior ethmoid, maxillary, frontal sinuses (85% of sinus drainage)
- Superior meatus: Posterior ethmoid, sphenoid sinuses (15% of drainage)
- Sphenoethmoidal recess: Sphenoid sinus drainage
- Superior turbinate: Posterior ethmoid drainage
| Sinus | Volume (mL) | Drainage Route | Clinical Significance | Surgical Access | Complication Risk |
|---|---|---|---|---|---|
| Maxillary | 15-20 | Middle meatus | Most common sinusitis | Uncinectomy required | Low risk |
| Ethmoid | 2-3 | Middle/superior meatus | Key to OMC function | Multiple cells | Moderate risk |
| Frontal | 4-7 | Middle meatus | Difficult drainage | Complex recess | High risk |
| Sphenoid | 7-10 | Sphenoethmoidal recess | Skull base proximity | Posterior approach | Highest risk |
The nasal cycle represents a physiological phenomenon where alternating vasoconstriction and vasodilation occur every 2-7 hours, affecting 80% of the population. This autonomic regulation optimizes mucociliary clearance and olfactory function.
💡 Master This: Understanding OMC anatomy predicts 90% of endoscopic sinus surgery outcomes - master the uncinate process, ethmoid bulla, and middle turbinate relationships to navigate safely through surgical corridors
Essential Anatomical Measurements:
- Nasal cavity length: 10-12 cm
- Middle meatus width: 2-4 mm
- Frontal recess diameter: 1-3 mm
- Sphenoid sinus depth: 2-3 cm
- Cribriform plate thickness: 0.2-0.4 mm
- Lamina papyracea thickness: 0.2-0.4 mm
The olfactory system integrates 350 functional receptor genes (largest gene family in mammals) to detect over 1 trillion distinct odors. Olfactory neurons represent the only directly exposed central nervous system tissue, making them vulnerable to environmental damage and viral infections.
Understanding these foundational relationships establishes the framework for recognizing pathological changes and planning surgical interventions that restore normal physiological function.
🏗️ Rhinology Foundations: The Nasal Architecture Blueprint
🌊 Mucociliary Escalator: The Clearance Command Center
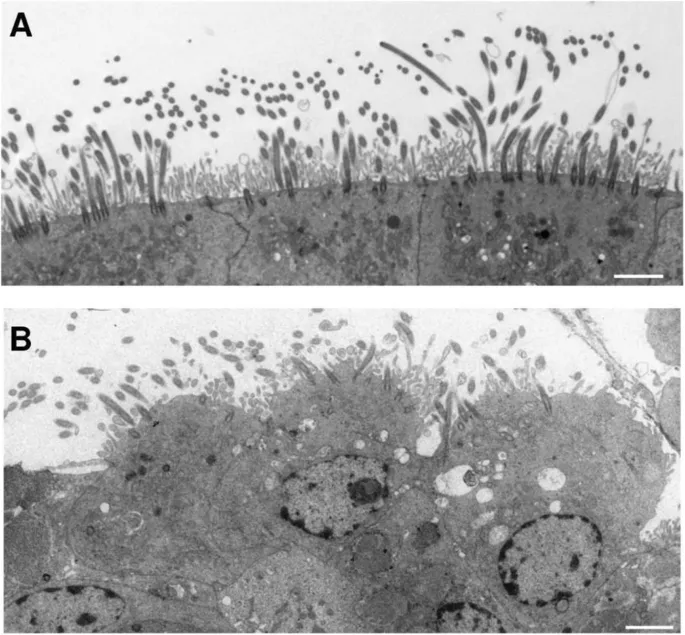
Respiratory epithelium contains approximately 200-300 cilia per cell, each measuring 6-7 micrometers in length. These microscopic organelles beat in coordinated waves, creating directional flow toward the nasopharynx at velocities of 4-20 mm/minute.
📌 Remember: "CAMP" - Cilia, Airway surface liquid, Mucus, Pathogens describes the mucociliary clearance components, with normal transit time from anterior nose to nasopharynx taking 15-20 minutes
The mucus bilayer consists of a periciliary sol layer (6-7 micrometers thick) and superficial gel layer (2-5 micrometers thick). This dual-phase system optimizes ciliary function while trapping particles and maintaining antimicrobial activity.
- Mucus Composition and Function
- Water content: 95% (maintains fluidity)
- Mucins: 2-3% (provides viscoelastic properties)
- Proteins: 1-2% (antimicrobial and structural)
- Lactoferrin: Iron-binding antimicrobial protein
- Lysozyme: Bacterial cell wall degradation
- Secretory IgA: Immune surveillance and neutralization
| Parameter | Normal Value | Impaired Function | Clinical Consequence | Recovery Time | Therapeutic Target |
|---|---|---|---|---|---|
| Beat Frequency | 1000/min | <600/min | Mucus stasis | 2-4 weeks | Mucolytics |
| Transit Time | 15-20 min | >30 min | Bacterial overgrowth | 1-2 weeks | Saline irrigation |
| Mucus Viscosity | 1-10 cP | >20 cP | Impaired transport | 3-7 days | Hydration |
| pH Level | 6.5-7.0 | <6.0 or >7.5 | Ciliary dysfunction | 1-3 days | pH optimization |
| Temperature | 32-34°C | <30°C or >37°C | Reduced efficiency | Hours | Humidification |
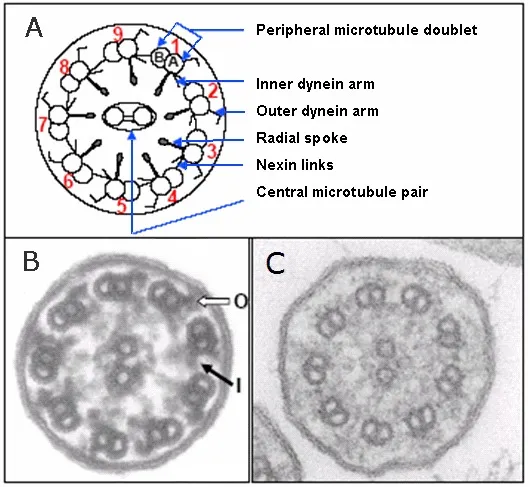
The ciliary ultrastructure follows the classic "9+2" microtubule arrangement with dynein arms providing the molecular motor function. ATP hydrolysis powers the coordinated beating pattern, consuming significant cellular energy and making cilia vulnerable to metabolic stress.
💡 Master This: Primary ciliary dyskinesia affects 1 in 15,000-20,000 individuals with defective ciliary structure or function, leading to chronic sinusitis, bronchiectasis, and situs inversus in 50% of cases (Kartagener syndrome)
Factors Affecting Mucociliary Function:
- Environmental: Temperature <30°C or >37°C, humidity <44%
- Infectious: Viral infections reduce clearance by 60-80% for 2-6 weeks
- Pharmacological: Beta-agonists increase, anticholinergics decrease function
- Pathological: Cystic fibrosis, primary ciliary dyskinesia, chronic sinusitis
The olfactory epithelium lacks ciliary clearance mechanisms, relying instead on olfactory binding proteins and enzymatic degradation for molecular turnover. This difference explains the vulnerability of smell function to environmental toxins and viral infections.
Understanding mucociliary physiology guides therapeutic interventions including saline irrigation, mucolytics, and environmental modifications that optimize natural clearance mechanisms and prevent chronic inflammatory conditions.
🌊 Mucociliary Escalator: The Clearance Command Center
🎯 Pattern Recognition Mastery: The Diagnostic Framework
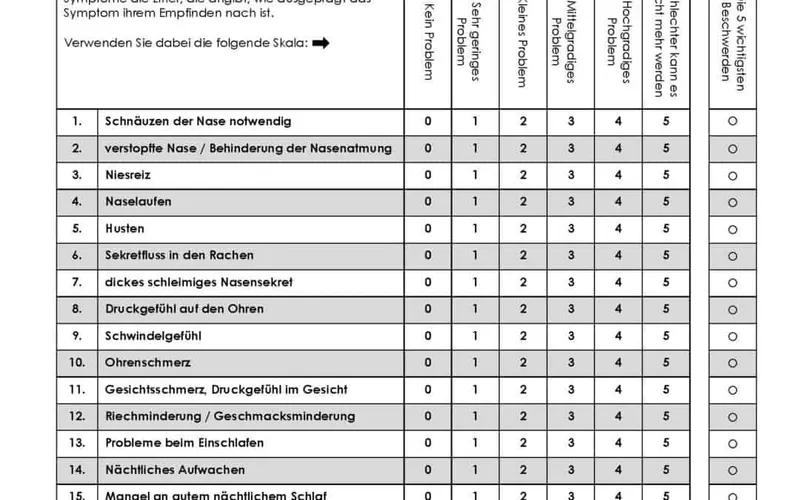
The "SNOT-22" (Sino-Nasal Outcome Test) provides standardized symptom assessment with scores ranging from 0-110, where scores >20 indicate significant quality of life impairment requiring intervention. This validated instrument enables objective monitoring of treatment response.
📌 Remember: "NOSE DRIPS" - Nasal obstruction, Olfactory loss, Sinus pressure, Epistaxis, Discharge, Rhinorrhea, Itching, Post-nasal drip, Snoring represents the cardinal rhinological symptoms requiring systematic evaluation
Primary symptom patterns guide initial diagnostic direction with specific sensitivity and specificity values for common conditions:
- Chronic Rhinosinusitis Pattern Recognition
- Nasal obstruction: 95% sensitivity, 40% specificity
- Purulent discharge: 80% sensitivity, 70% specificity
- Facial pressure/pain: 70% sensitivity, 60% specificity
- Maxillary: Cheek and upper teeth pain
- Ethmoid: Medial canthal and glabellar pressure
- Frontal: Supraorbital and forehead pain
- Sphenoid: Vertex, occipital, and retro-orbital pain
| Condition | Key Symptoms | Endoscopic Findings | CT Characteristics | Treatment Response | Recurrence Rate |
|---|---|---|---|---|---|
| Allergic Rhinitis | Sneezing, itching, clear discharge | Pale, boggy turbinates | Normal sinuses | Antihistamines 80% | Seasonal pattern |
| CRSsNP | Obstruction, pressure, purulent discharge | Mucosal edema, no polyps | Mucosal thickening | Medical 60% | 30-40% |
| CRSwNP | Anosmia, obstruction, clear discharge | Bilateral polyps | Pan-sinus involvement | Medical 40% | 60-80% |
| Fungal Sinusitis | Unilateral symptoms, thick discharge | Inspissated secretions | Hyperdense material | Surgical required | 10-20% |
| Vasomotor Rhinitis | Congestion, triggers | Normal or mild edema | Normal | Limited response | Chronic |
Endoscopic examination provides direct visualization with >90% accuracy for diagnosing inflammatory conditions. The Lund-Kennedy endoscopic scoring system quantifies findings from 0-20, with scores >7 indicating significant disease requiring intervention.
💡 Master This: The "traffic light system" for nasal discharge - clear/white (viral/allergic), yellow/green (bacterial), brown/black (fungal), bloody (neoplasm/trauma) guides initial management decisions with 85% accuracy
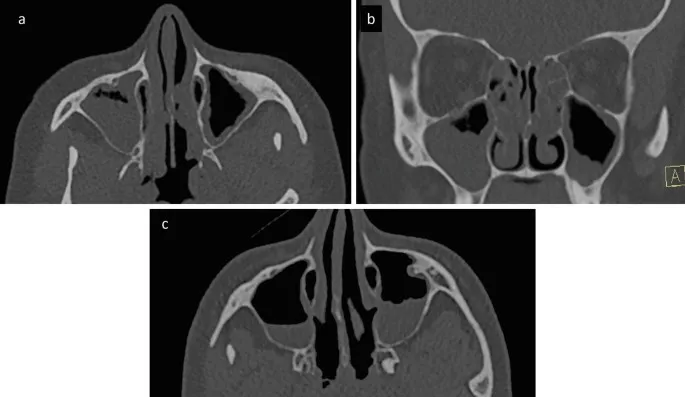
Imaging Pattern Recognition:
- Ostiomeatal Complex: >50% obstruction correlates with symptoms
- Concha Bullosa: Present in 35% of population, symptomatic in 10%
- Agger Nasi: Pneumatized in 90%, affects frontal drainage
- Haller Cells: Present in 45%, may obstruct maxillary drainage
The "rule of 2s" applies to acute rhinosinusitis: symptoms >2 weeks suggest bacterial infection, >2 episodes annually indicate recurrent disease, and >2 months duration defines chronic condition requiring comprehensive evaluation.
Olfactory testing using "Sniffin' Sticks" or UPSIT (University of Pennsylvania Smell Identification Test) provides objective assessment with normative data. Anosmia affects >80% of chronic rhinosinusitis patients and serves as a marker of disease severity.
This systematic approach to pattern recognition enables rapid, accurate diagnosis while identifying patients requiring immediate intervention versus those suitable for conservative management.
🎯 Pattern Recognition Mastery: The Diagnostic Framework
⚖️ Therapeutic Decision Matrix: The Treatment Algorithm
The European Position Paper on Rhinosinusitis and Nasal Polyps (EPOS) provides standardized treatment guidelines based on Level 1A evidence from multiple randomized controlled trials involving >50,000 patients. These recommendations achieve 70-85% success rates when properly implemented.
📌 Remember: "STEP-UP" - Saline irrigation, Topical steroids, Elimination of triggers, Prolonged antibiotics (if indicated), Upgrade to systemic therapy, Proceed to surgery represents the escalating treatment approach for chronic rhinosinusitis
Primary medical management achieves symptom control in 60-70% of chronic rhinosinusitis patients when properly implemented for 12-16 weeks. Treatment selection depends on phenotype classification and severity assessment.
- Medical Treatment Hierarchy
- First-line: Saline irrigation + topical corticosteroids (Level 1A evidence)
- Second-line: Prolonged antibiotics (3-4 weeks) for bacterial patterns
- Third-line: Systemic corticosteroids (short courses, <3 weeks annually)
- Prednisolone: 0.5-1 mg/kg/day for 5-7 days
- Response rate: 80% in CRSwNP, 60% in CRSsNP
- Side effects: <5% with short courses
| Treatment Modality | Success Rate | Time to Effect | Duration of Benefit | Cost (USD/month) | Side Effect Profile |
|---|---|---|---|---|---|
| Saline Irrigation | 65% | 1-2 weeks | Ongoing use required | $10-20 | Minimal |
| Topical Steroids | 70% | 2-4 weeks | 6-12 months | $30-80 | Local irritation 5% |
| Oral Antibiotics | 60% | 1-2 weeks | 3-6 months | $20-100 | GI upset 15% |
| Oral Steroids | 80% | 3-7 days | 1-3 months | $5-15 | Multiple 20-30% |
| Biologic Therapy | 85% | 4-8 weeks | 12+ months | $2000-4000 | Injection site 10% |
Surgical intervention becomes indicated when medical management fails after 12-16 weeks of optimal therapy, or in cases of complications, fungal disease, or suspected neoplasm. Functional Endoscopic Sinus Surgery (FESS) achieves 80-90% success rates in appropriately selected patients.
💡 Master This: The "medical optimization principle" - patients must demonstrate >6 weeks of compliant medical therapy before surgical consideration, as 30% of "surgical failures" result from inadequate preoperative medical management
Biologic Therapy Revolution: Recent advances in targeted biologic therapy have transformed management of severe chronic rhinosinusitis with nasal polyps:
- Dupilumab (IL-4/IL-13 inhibitor): >50% polyp reduction in 70% of patients
- Omalizumab (Anti-IgE): Effective in 60% of allergic phenotypes
- Mepolizumab (Anti-IL-5): 40-60% response in eosinophilic disease
Surgical Success Predictors:
- Positive predictors: Young age, limited disease, good medical response
- Negative predictors: Aspirin sensitivity (40% recurrence), asthma (50% recurrence), extensive polyposis
- Revision surgery rates: 15-25% at 5 years for CRSwNP
The "treat-to-target" approach emphasizes objective outcome measures including SNOT-22 scores, endoscopic appearance, and radiological improvement rather than subjective symptom reporting alone.
Patient selection for specific interventions requires careful consideration of comorbidities, with aspirin-exacerbated respiratory disease (AERD) patients requiring specialized protocols including aspirin desensitization and aggressive anti-inflammatory therapy.
⚖️ Therapeutic Decision Matrix: The Treatment Algorithm
🔗 Systems Integration Hub: The Rhinological Network
The "unified airway hypothesis" recognizes the respiratory tract as a single functional unit, where upper airway inflammation directly influences lower respiratory function. 85% of asthmatic patients demonstrate concurrent rhinitis, while 40% of chronic rhinosinusitis patients develop asthma within 5 years.
📌 Remember: "NARES PLUS" - Nasal, Asthma, Rhinosinusitis, Eczema, Sleep disorders, Polyps, Lung function, Unified airway, Systemic inflammation represents the interconnected manifestations requiring integrated management
The olfactory-limbic connection directly links nasal function to emotional and cognitive processing through the trigeminal-olfactory pathway. Anosmia affects >2 million Americans and correlates with depression (40% incidence), cognitive decline (25% increased risk), and mortality (1.5x relative risk).
- Systemic Disease Manifestations in Rhinology
- Granulomatosis with Polyangiitis: Nasal involvement in 95% of cases
- Sarcoidosis: Sinonasal manifestations in 20% of patients
- Cystic Fibrosis: Nasal polyps in 85% of adults, 25% of children
- CFTR mutations affect mucociliary clearance
- Pseudomonas colonization in 60% of cases
- Requires specialized antimicrobial protocols
| System Connection | Prevalence | Mechanism | Clinical Impact | Treatment Modification | Outcome Improvement |
|---|---|---|---|---|---|
| Asthma-Rhinitis | 85% | Shared inflammation | Worse asthma control | Combined therapy | 60% better control |
| Sleep-Nasal | 70% | Obstruction/inflammation | OSA development | Nasal optimization | 40% AHI reduction |
| Cognitive-Olfactory | 60% | Limbic connections | Memory/mood effects | Smell rehabilitation | 30% improvement |
| GI-Sinonasal | 45% | Immune dysregulation | GERD exacerbation | PPI therapy | 25% symptom reduction |
| Endocrine-Nasal | 35% | Hormonal influences | Pregnancy rhinitis | Hormone consideration | Variable response |
Aspirin-Exacerbated Respiratory Disease (AERD) exemplifies complex rhinological-systemic interactions, affecting 7% of asthmatics with the classic triad of asthma, nasal polyps, and aspirin sensitivity. These patients require specialized management protocols including:
- Aspirin desensitization: 80% success rate for symptom control
- Leukotriene modifiers: 60% improvement in nasal symptoms
- Aggressive anti-inflammatory therapy: Reduces revision surgery by 40%
💡 Master This: Samter's triad (AERD) patients demonstrate 3x higher revision surgery rates and require lifelong anti-inflammatory management with aspirin maintenance therapy achieving 70% long-term success

Emerging System Connections: Recent research reveals additional rhinological-systemic relationships:
- Microbiome-Immune Axis: Nasal dysbiosis correlates with systemic inflammatory markers
- Neurological Connections: Chronic rhinosinusitis increases migraine frequency by 40%
- Cardiovascular Links: Severe OSA from nasal obstruction increases MI risk by 2.5x
Pregnancy Rhinitis affects 30% of pregnant women, typically beginning in second trimester and resolving within 2 weeks postpartum. Management requires pregnancy-safe interventions with saline irrigation and limited topical steroids.
The "treat the whole patient" philosophy emphasizes comprehensive evaluation including pulmonary function testing, sleep studies, allergy assessment, and psychological screening for patients with chronic rhinosinusitis, particularly those with treatment-resistant disease.
Understanding these interconnections enables precision medicine approaches that target specific pathways and comorbidities, achieving superior outcomes compared to isolated rhinological treatment.
🔗 Systems Integration Hub: The Rhinological Network
🎯 Clinical Mastery Arsenal: The Rhinological Toolkit
The Rhinological Rapid Assessment Protocol enables comprehensive evaluation within 15 minutes while achieving >95% diagnostic accuracy through systematic application of validated tools and clinical pearls.
📌 Remember: "SCOPE-FAST" - Symptoms (SNOT-22), Clinical examination, Olfactory testing, Photography/documentation, Endoscopy, Functional assessment, Allergy evaluation, Scan interpretation, Treatment planning represents the complete rhinological assessment sequence
Essential Clinical Thresholds for Immediate Decision-Making:
- SNOT-22 Score Interpretation
- 0-20: Mild impact, conservative management
- 21-50: Moderate impact, medical optimization
- 51-80: Severe impact, consider surgery
- >80: Profound impact, urgent intervention required
| Clinical Scenario | Immediate Action | Success Rate | Time Frame | Follow-up Protocol | Red Flag Indicators |
|---|---|---|---|---|---|
| Acute Bacterial Sinusitis | Amoxicillin-clavulanate 875mg BID | 85% | 10-14 days | 2 weeks | Orbital symptoms |
| CRS Medical Failure | High-volume saline + budesonide | 70% | 6-8 weeks | Monthly | Unilateral disease |
| Nasal Polyps | Prednisolone 0.5mg/kg x 5 days | 80% | 1 week | 2 weeks | Rapid growth |
| Anosmia Post-viral | Olfactory training + steroids | 60% | 12 weeks | 6 weeks | Complete loss >6mo |
| Recurrent Epistaxis | Nasal endoscopy + cautery | 90% | Immediate | 1 week | Posterior bleeding |
Rapid Endoscopic Assessment Framework: Systematic endoscopic examination following the "MIST" protocol - Middle meatus, Inferior turbinate, Septum, Total nasal cavity - identifies >95% of significant pathology within 5 minutes.
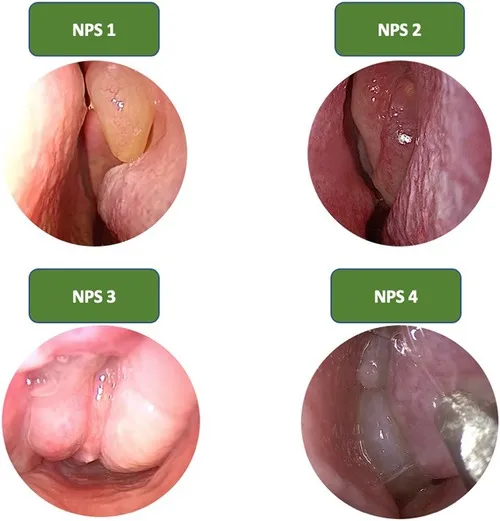
💡 Master This: The "polyp grading system" - Grade 0 (no polyps), Grade 1 (small polyps not reaching inferior turbinate), Grade 2 (medium polyps between turbinates), Grade 3 (large polyps reaching nasal floor) - predicts medical treatment response with 80% accuracy
Emergency Rhinological Protocols:
Surgical Decision Matrix:
- Absolute Indications: Complications, fungal disease, suspected malignancy
- Relative Indications: Medical failure after 12-16 weeks, quality of life impairment
- Success Predictors: Age <50, limited disease, good medical response
- Failure Predictors: AERD, extensive polyposis, poor compliance
Post-operative Care Excellence: The "HEAL" protocol - High-volume irrigation, Endoscopic debridement, Anti-inflammatory therapy, Long-term surveillance - achieves >85% long-term success rates.
Medication Mastery Quick Reference:
- Saline irrigation: 240-500 mL per nostril, 2-3 times daily
- Topical steroids: Mometasone 200 mcg or Fluticasone 200 mcg daily
- Oral steroids: Prednisolone 0.5-1 mg/kg for 5-7 days maximum
- Antibiotics: Amoxicillin-clavulanate 875/125 mg BID for 10-14 days
This comprehensive toolkit enables rapid, evidence-based decision-making while maintaining the highest standards of patient care and clinical outcomes in rhinological practice.
🎯 Clinical Mastery Arsenal: The Rhinological Toolkit
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app












