Definition & Basics - Voice Interrupted
- Spasmodic Dysphonia (SD): A chronic neurological voice disorder; specifically a focal laryngeal dystonia.
- Nature: It's task-specific, primarily affecting speech, and is action-induced.
- Mechanism: Characterized by involuntary, spasmodic contractions of laryngeal muscles during voice production.
- Voice Quality: Results in a strained, tight, choked, or breathy voice; often with voice breaks. Singing or laughing may be unaffected.
⭐ SD is often misdiagnosed as muscle tension dysphonia or psychogenic voice disorder, delaying appropriate treatment.
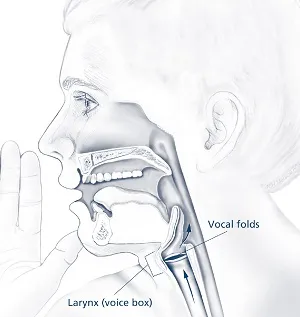
Pathophysiology & Etiology - Brain's Vocal Glitch
- Neurological Origin: Considered a focal laryngeal dystonia; not a psychogenic disorder.
- Core Defect: Basal ganglia dysfunction (e.g., putamen, globus pallidus) leading to faulty sensorimotor integration for precise voice modulation.
- Etiology Spectrum:
- Predominantly idiopathic (most common).
- Genetic predisposition: Rare, but familial cases exist.
- Possible Triggers: Upper Respiratory Infections (URI), significant stress, or prolonged voice overuse can precipitate onset in susceptible individuals.

⭐ Though neurological in origin, structural brain imaging (MRI/CT) is typically normal in Spasmodic Dysphonia.
Types & Clinical Features - Strained or Breathy?
Spasmodic Dysphonia (SD) presents primarily in three forms based on laryngeal muscle involvement:
| Feature | Adductor SD (ADSD) | Abductor SD (ABSD) |
|---|---|---|
| Voice Quality | Strained, strangled, effortful | Breathy, whispery, weak |
| Voice Breaks | On voiced sounds (e.g., vowels, /z/) | On voiceless sounds (e.g., /s/, /p/) |
- Mixed SD: Features of both ADSD and ABSD.
- Task Specificity: Symptoms are typically worse during connected speech and often improve or disappear during activities like singing, laughing, or shouting.
⭐ Adductor Spasmodic Dysphonia (ADSD) is the most common type, accounting for approximately 80-90% of cases.
Diagnosis - Pinpointing the Spasms
- Clinical History: Detailed patient interview focusing on voice symptoms.
- Perceptual Voice Assessment: Subjective evaluation of voice quality (e.g., GRBAS scale).
- Flexible Nasolaryngoscopy: To visualize vocal fold movement and identify spasms during speech.
- Adductor SD: Cords slam shut.
- Abductor SD: Cords open inappropriately.
- Laryngeal Electromyography (LEMG): Confirmatory test showing excessive, involuntary laryngeal muscle activity.
⭐ Laryngeal Electromyography (LEMG) is the gold standard for confirming SD, especially in ambiguous cases.
- Acoustic Analysis: Objective measures of voice parameters (jitter, shimmer, voice breaks).
- Rule Out: Exclude other neurological or structural voice disorders.
Management - Taming the Tremors
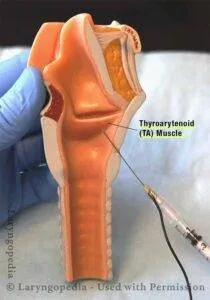
- Botulinum Toxin (Botox) Injections: Mainstay treatment. 📌 Botox: Bottles Toxic spasms.
- Provides temporary relief (3-4 months).
- Target Muscles:
- Adductor SD (ADSD): Thyroarytenoid (TA) muscle - 1.25-2.5 U.
- Abductor SD (ABSD): Posterior Cricoarytenoid (PCA) muscle - 2.5-10 U.
⭐ Botulinum toxin injection into laryngeal muscles is the current gold standard treatment for Spasmodic Dysphonia, providing symptomatic relief for 3-4 months.
- Voice Therapy: Adjunctive role; helps manage symptoms and optimize voice post-Botox.
- Surgical Options (Limited Use/Controversial):
- Recurrent Laryngeal Nerve (RLN) denervation-reinnervation.
- Selective Laryngeal Adductor Denervation-Reinnervation (SLAD-R).
- Thyroplasty Type II (for ABSD).
High‑Yield Points - ⚡ Biggest Takeaways
- Spasmodic Dysphonia (SD) is a focal laryngeal dystonia; etiology often unknown.
- Two main types: Adductor SD (common, strained-strangled voice) and Abductor SD (breathy, whispery voice).
- Voice is task-specific: worsens with speech, often improves with laughing or singing.
- Diagnosis is primarily clinical, aided by laryngoscopy showing vocal fold spasms.
- Botulinum toxin (Botox) injections are the mainstay of treatment.
- Adductor SD: Botox into thyroarytenoid (TA) muscle.
- Abductor SD: Botox into posterior cricoarytenoid (PCA) muscle.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

