Pediatric Sleep Apnea - Tiny Snorers Big Problems
- Recurrent partial/complete upper airway obstruction during sleep.
- Prevalence: 1-4% children; peak age 2-8 years.
- Main cause: Adenotonsillar hypertrophy (ATH).
- Signs: Habitual snoring, apneas, restless sleep, daytime neurobehavioral issues.
⭐ Pediatric OSA involves repeated episodes of upper airway obstruction during sleep, leading to intermittent hypoxia and sleep fragmentation. Crucially, it impacts child neurocognition, behavior, growth, and cardiovascular status.
Pediatric Sleep Apnea - Who's Blocking Airway?
- Most Common: Adenotonsillar hypertrophy (ATH) - enlarged tonsils & adenoids.
⭐ Most common cause is adenotonsillar hypertrophy.
- Other Key Factors:
- Obesity: ↑ pharyngeal fat, ↓ airway patency.
- Craniofacial anomalies: e.g., micrognathia (Pierre Robin), midface hypoplasia (Down syndrome, Apert, Crouzon), choanal atresia.
- Neuromuscular weakness: e.g., cerebral palsy, muscular dystrophy.
- Mucosal factors: Allergic rhinitis, laryngomalacia (infants).
- Macroglossia: e.g., Beckwith-Wiedemann, Down syndrome. oka
Pediatric Sleep Apnea - The Suffocation Story

- Primary Cause: Adenotonsillar hypertrophy (ATH) obstructing upper airway.
- Mechanism: Obstruction → ↓O₂, ↑CO₂ (intermittent hypoxia/hypercapnia) → frequent arousals, fragmented sleep.
- Clinical Impact:
- Neurocognitive: ADHD-like symptoms, learning issues.
- Cardiovascular: ↑Pulmonary/systemic BP.
- Growth: Failure to thrive.
⭐ Intermittent hypoxia and hypercapnia are key drivers of systemic inflammation and endothelial dysfunction in pediatric OSA.
Pediatric Sleep Apnea - Night & Day Woes
- Nocturnal Symptoms:
- Snoring (habitual, loud)
- Witnessed apneas, gasping, snorting
- Restless sleep, unusual sleep positions (hyperextension of neck)
- Enuresis (secondary)
- Sweating
- Daytime Symptoms:
- Mouth breathing
- Nasal obstruction/hyponasal speech
- Difficulty waking up, morning headaches
- Excessive daytime sleepiness (less common than in adults)
- Learning difficulties, poor school performance
⭐ Neurobehavioral consequences like ADHD-like symptoms (hyperactivity, inattention) are common and can be mistaken for primary ADHD. 📌 SNORE: Snoring, Nocturnal arousals/apneas, Obesity/adenotonsillar hypertrophy, Restless sleep, Enuresis/Excessive daytime sleepiness/Evolving behavior issues.
Pediatric Sleep Apnea - Sleep Study Secrets
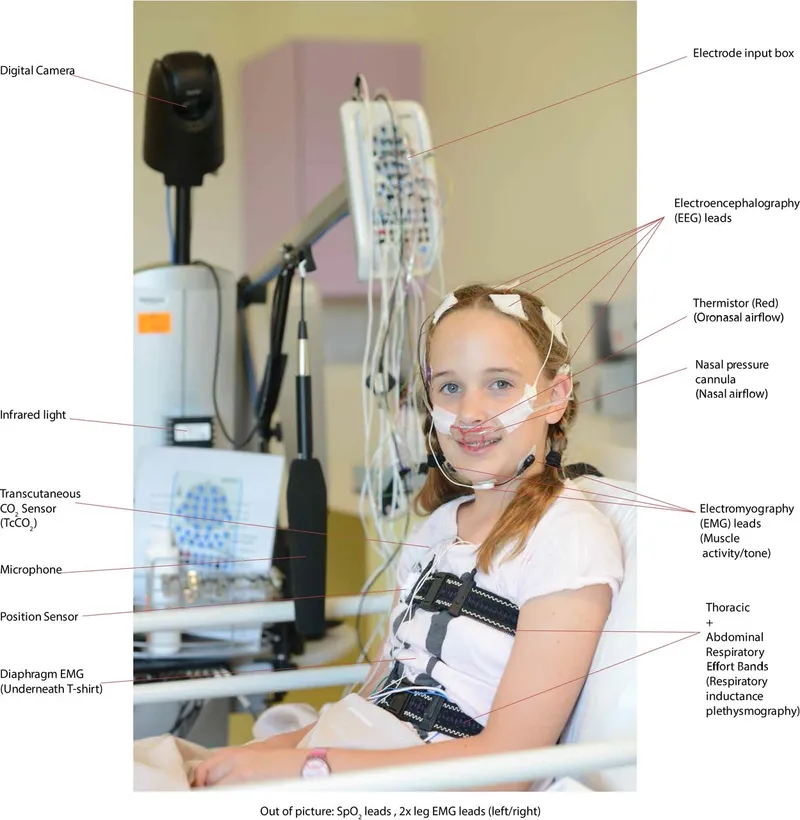
- Polysomnography (PSG): Gold standard; overnight, in-lab.
- Monitors: EEG, EOG, EMG, ECG, airflow, respiratory effort, SaO2.
- Apnea-Hypopnea Index (AHI) for diagnosis & severity:
- Normal: <1 event/hr
- Mild OSA: 1-5 events/hr
- Moderate OSA: >5-10 events/hr
- Severe OSA: >10 events/hr
- Overnight oximetry: Useful for screening, but not definitive.
⭐ Polysomnography (PSG) is the gold standard for diagnosis. An AHI ≥1 event/hr is diagnostic in children.
Pediatric Sleep Apnea - Clearing The Path
⭐ Adenotonsillectomy (T&A) is the first-line treatment for most children with OSA due to adenotonsillar hypertrophy (AHI >5).
- Initial Management:
- Watchful waiting (mild OSA: AHI <5).
- Weight management (if obese).
- Intranasal corticosteroids (allergic rhinitis).
- Medical: Montelukast (mild OSA or adjunctive).
- Primary Surgical: Adenotonsillectomy (T&A); success ~70-80%. Consider for AHI ≥1 with symptoms.
- Persistent OSA Post-T&A (Residual OSA):
- Repeat PSG 6-8 weeks post-op.
- CPAP/BiPAP is gold standard for medical management.
- DISE to guide further surgery (e.g., lingual tonsillectomy, supraglottoplasty).
- Orthodontics: Rapid Maxillary Expansion (RME).

High‑Yield Points - ⚡ Biggest Takeaways
- Adenotonsillar hypertrophy is the primary cause of pediatric Obstructive Sleep Apnea (OSA).
- Overnight polysomnography (PSG) is the gold standard diagnostic test.
- An Apnea-Hypopnea Index (AHI) > 1 event/hour is considered abnormal in children.
- Key symptoms include habitual snoring, mouth breathing, witnessed apneas, and daytime hyperactivity.
- Adenotonsillectomy (T&A) is the first-line surgical treatment with high success rates.
- Complications include failure to thrive, neurocognitive impairment, and rarely cor pulmonale.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

