Otolaryngology Basics

On this page
🎯 ENT Mastery: Your Clinical Command Center
You'll master the integrated systems that govern hearing, balance, taste, smell, voice, and swallowing-six sensory and motor networks that define how patients interact with their world. This lesson builds your clinical command from molecular receptors through mechanical transmission to diagnostic reasoning, equipping you to recognize pathology at each level. By connecting anatomy to function and dysfunction, you'll develop the pattern recognition that distinguishes competent from exceptional ENT assessment. Prepare to think like an otolaryngologist, moving seamlessly between microscopic chemoreception and macroscopic airway protection.
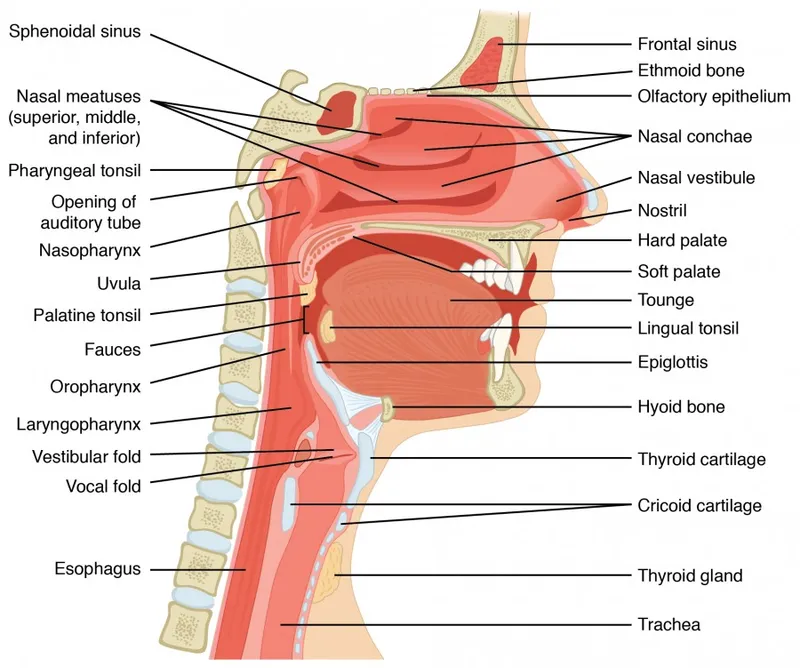
Otolaryngology represents the convergence of 12 distinct anatomical regions, each with unique embryological origins, vascular territories, and clinical presentations. Master these foundational relationships, and you possess the framework for understanding every ENT pathology from conductive hearing loss to laryngeal cancer.
The ENT Anatomical Trinity: Integrated Systems Architecture
The head and neck region contains 3 primary functional units that work in seamless coordination:
-
Auditory-Vestibular Complex
- External ear: Sound collection and amplification (10-15 dB gain)
- Middle ear: Mechanical impedance matching (25-30 dB gain)
- Inner ear: Transduction and balance integration (20,000+ hair cells)
- Cochlear frequency mapping: 20 Hz to 20,000 Hz
- Vestibular acceleration detection: 0.01 m/s² threshold
- Endolymphatic pressure: +80 to +90 mV
-
Respiratory-Olfactory Network
- Nasal cavity: Air conditioning and filtration (500+ L/hour airflow)
- Paranasal sinuses: Resonance and humidification (4 paired chambers)
- Olfactory system: Chemical detection (10 million receptor cells)
- Olfactory threshold: 10⁻¹² molar concentrations
- Regeneration cycle: 30-60 days for receptor turnover
- Neural pathway: Direct to limbic system (2 synapses)
-
Phonatory-Deglutition Apparatus
- Larynx: Voice production and airway protection (3 functional levels)
- Pharynx: Swallowing coordination (4-phase sequence)
- Oral cavity: Articulation and mastication (32 teeth, 4 salivary glands)
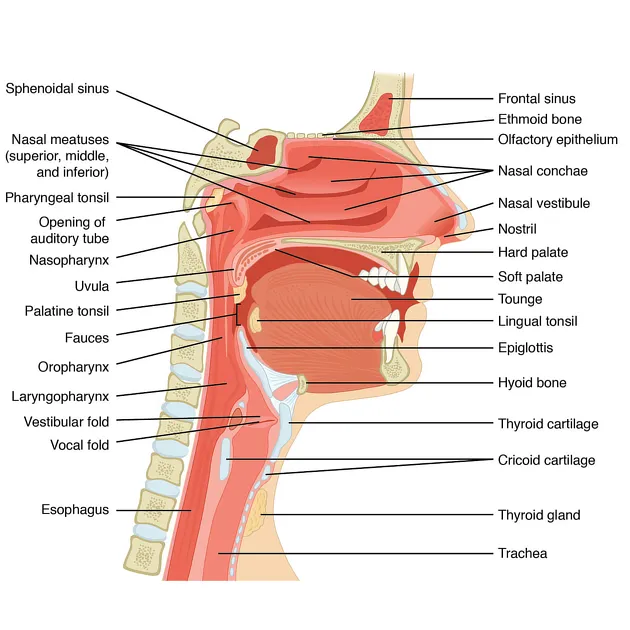
📌 Remember: HEAL - Hearing, Equilibrium, Airway, Larynx represent the four core ENT functions, each requiring distinct diagnostic approaches and specialized treatment protocols
ENT Embryological Foundation: Developmental Precision
Understanding ENT embryology predicts 90% of congenital anomalies and explains anatomical variations:
| Embryological Origin | Structures Formed | Timeline | Clinical Significance | Anomaly Risk |
|---|---|---|---|---|
| 1st Branchial Arch | Maxilla, mandible, middle ear ossicles | Week 6-8 | Treacher Collins syndrome | 1:50,000 |
| 2nd Branchial Arch | Stapes, facial nerve, hyoid | Week 7-9 | Branchial cyst formation | 1:150,000 |
| Neural Crest | Olfactory epithelium, cranial nerves | Week 4-6 | Kallmann syndrome | 1:30,000 |
| Endoderm | Thyroid, parathyroid, thymus | Week 5-7 | DiGeorge syndrome | 1:4,000 |
| Otic Placode | Inner ear labyrinth | Week 3-5 | Congenital hearing loss | 3:1,000 |
Neurovascular Architecture: The ENT Lifeline Network
The head and neck contains 60% of the body's cranial nerves, creating complex neurovascular territories:
- Cranial Nerve Distribution
- CN I (Olfactory): Smell transduction, 40 million axons
- CN VII (Facial): Facial expression, taste (anterior 2/3 tongue)
- CN VIII (Vestibulocochlear): Hearing and balance, 30,000 nerve fibers
- Cochlear division: 95% afferent, 5% efferent
- Vestibular division: 5 distinct end organs
- CN IX (Glossopharyngeal): Posterior tongue sensation, carotid body innervation
- CN X (Vagus): Laryngeal motor control, recurrent laryngeal nerve
- Superior laryngeal nerve: cricothyroid muscle innervation
- Recurrent laryngeal nerve: All other intrinsic laryngeal muscles
💡 Master This: The recurrent laryngeal nerve travels 45 cm on the left side (around aortic arch) versus 5 cm on the right (around subclavian artery), explaining why left-sided vocal cord paralysis is 3x more common and often indicates thoracic pathology
Vascular Territory Mapping: Blood Supply Mastery
ENT regions receive blood from 3 major arterial systems with extensive collateral circulation:
⚠️ Warning: Kiesselbach's plexus (Little's area) contains 5 arterial convergences in a 1 cm² area, making it the source of 90% of epistaxis cases. Dry air reduces mucosal thickness by 40%, dramatically increasing bleeding risk
The systematic understanding of ENT anatomy, embryology, and neurovascular relationships creates the foundation for recognizing pathological patterns and implementing targeted interventions. Connect these structural principles through functional physiology to understand how sound transduction, chemical sensation, and airway protection work in clinical practice.
🎯 ENT Mastery: Your Clinical Command Center
🔧 Sound Engineering: The Auditory Transmission System
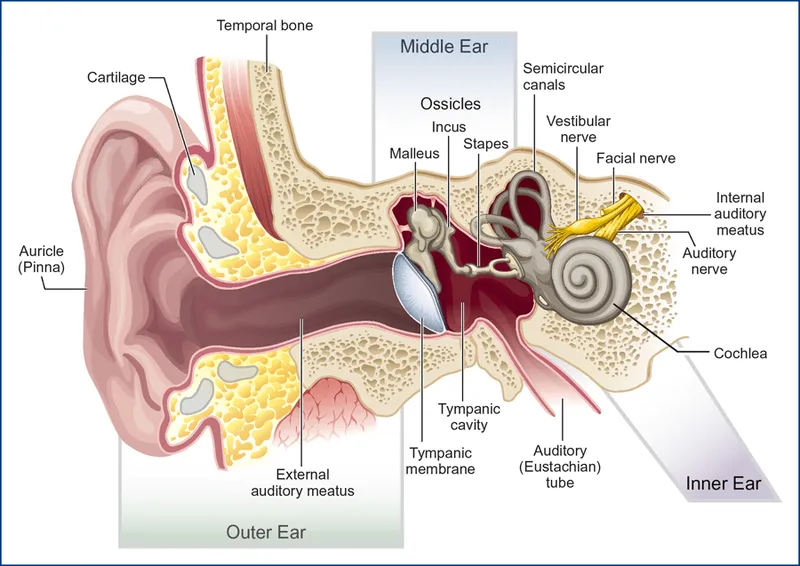
The hearing mechanism transforms air pressure variations as small as 10⁻¹² watts/m² into neural signals, representing a dynamic range of 120 decibels - from the threshold of hearing to the pain threshold. Understanding this process reveals why specific frequencies are lost first in pathological conditions and how targeted interventions can restore function.
Mechanical Amplification Cascade: Three-Stage Sound Processing
The ear functions as a biological amplifier system with precise impedance matching:
-
Stage 1: External Ear Collection
- Pinna: 10-15 dB gain for 2-5 kHz frequencies
- External auditory canal: Resonance amplification at 2.5 kHz
- Canal length: 2.5 cm, creating quarter-wave resonance
- Optimal frequency response: 1,000-4,000 Hz
- Cerumen production: 1-2 mm/month lateral migration
- Temperature regulation: Maintains 37°C regardless of ambient conditions
-
Stage 2: Middle Ear Transformation
- Tympanic membrane: Surface area 55 mm², effective area 43 mm²
- Ossicular chain: Mechanical advantage 1.3:1 (lever arm ratio)
- Oval window: Surface area 3.2 mm²
- Total amplification: 25-30 dB gain
- Impedance matching: Air (400 ohms) to fluid (1,500,000 ohms)
- Frequency response: Optimal 500-4,000 Hz
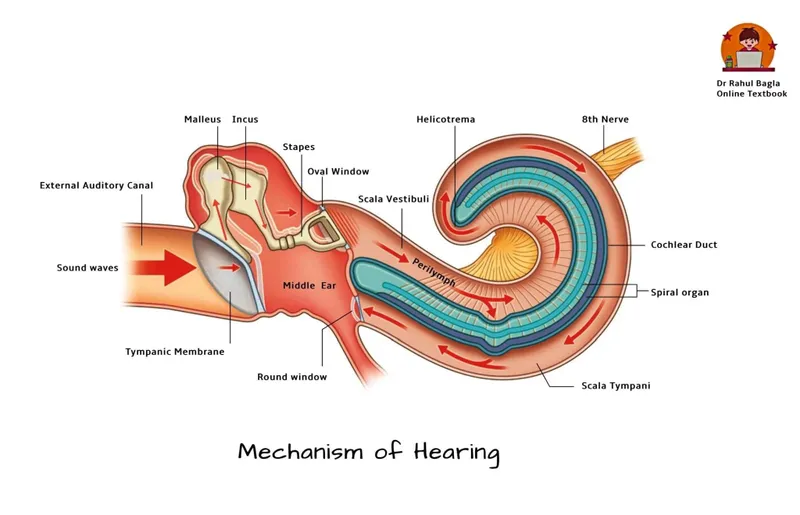
📌 Remember: MIST - Malleus, Incus, Stapes, Tympanic membrane create a mechanical transformer with 17:1 pressure amplification (area ratio) × 1.3:1 lever advantage = 22:1 total mechanical gain
Cochlear Transduction: Hair Cell Engineering Marvel
The cochlea contains 16,000 hair cells arranged in precise tonotopic organization:
| Cochlear Location | Frequency Range | Hair Cell Type | Stereocilia Count | Clinical Significance |
|---|---|---|---|---|
| Basal Turn | 8,000-20,000 Hz | Outer: 12,000 | 50-70 per cell | First lost in presbycusis |
| Middle Turn | 1,000-8,000 Hz | Inner: 3,500 | 40-60 per cell | Speech frequency range |
| Apical Turn | 20-1,000 Hz | Supporting cells | 30-50 per cell | Low frequency hearing |
| Organ of Corti | Full spectrum | Total: 16,000 | Variable height | Irreplaceable when damaged |
| Spiral Ganglion | Neural interface | 30,000 neurons | Type I: 95% | Cochlear implant target |
Neural Pathway Architecture: Central Auditory Processing
Auditory information travels through 6 synaptic levels before reaching auditory cortex:
-
Brainstem Processing Stations
- Cochlear nuclei: First central synapse, tonotopic preservation
- Superior olivary complex: Binaural processing, sound localization
- Lateral lemniscus: Temporal processing, gap detection
- Interaural time difference: 10 microseconds detection threshold
- Interaural level difference: 1 dB discrimination capability
- Sound localization accuracy: 1-2 degrees in horizontal plane
-
Midbrain Integration
- Inferior colliculus: Frequency integration, reflexive responses
- Medial geniculate body: Thalamic relay, attention modulation
- Response latency: 8-12 milliseconds from stimulus
- Frequency tuning: Sharpened compared to peripheral
- Plasticity: Experience-dependent modifications
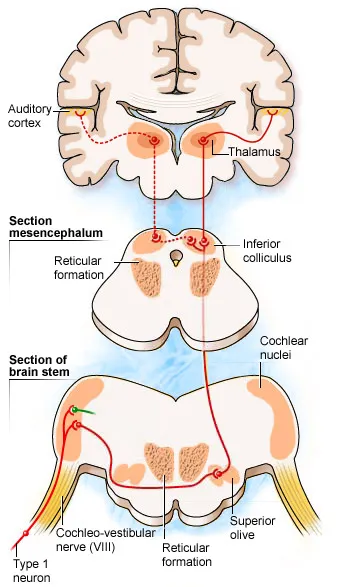
💡 Master This: Retrocochlear pathology (acoustic neuroma, brainstem lesions) disrupts temporal processing more than frequency detection, explaining why speech discrimination deteriorates disproportionately to pure tone thresholds in these conditions
Protective Mechanisms: Acoustic Reflex System
The middle ear contains 2 protective muscles that activate within 40-100 milliseconds of loud sounds:
-
Stapedius Muscle (CN VII innervation)
- Activation threshold: 70-90 dB above hearing threshold
- Attenuation: 10-15 dB for low frequencies (<2,000 Hz)
- Reflex decay: <50% in 10 seconds (normal)
-
Tensor Tympani (CN V innervation)
- Voluntary activation: During swallowing, speaking
- Protection: Against self-generated sounds
- Clinical testing: Acoustic reflex threshold and decay
⚠️ Warning: Acoustic reflex absence with normal hearing suggests facial nerve pathology (stapedius muscle paralysis), while elevated thresholds indicate cochlear dysfunction. Reflex decay >50% in 10 seconds suggests retrocochlear pathology
The auditory system's sophisticated engineering enables frequency discrimination of 0.2% and temporal resolution of 2-3 milliseconds. Connect this mechanical precision through vestibular physiology to understand how balance and spatial orientation integrate with hearing function.
🔧 Sound Engineering: The Auditory Transmission System
🎪 Balance Mastery: The Vestibular Control Network
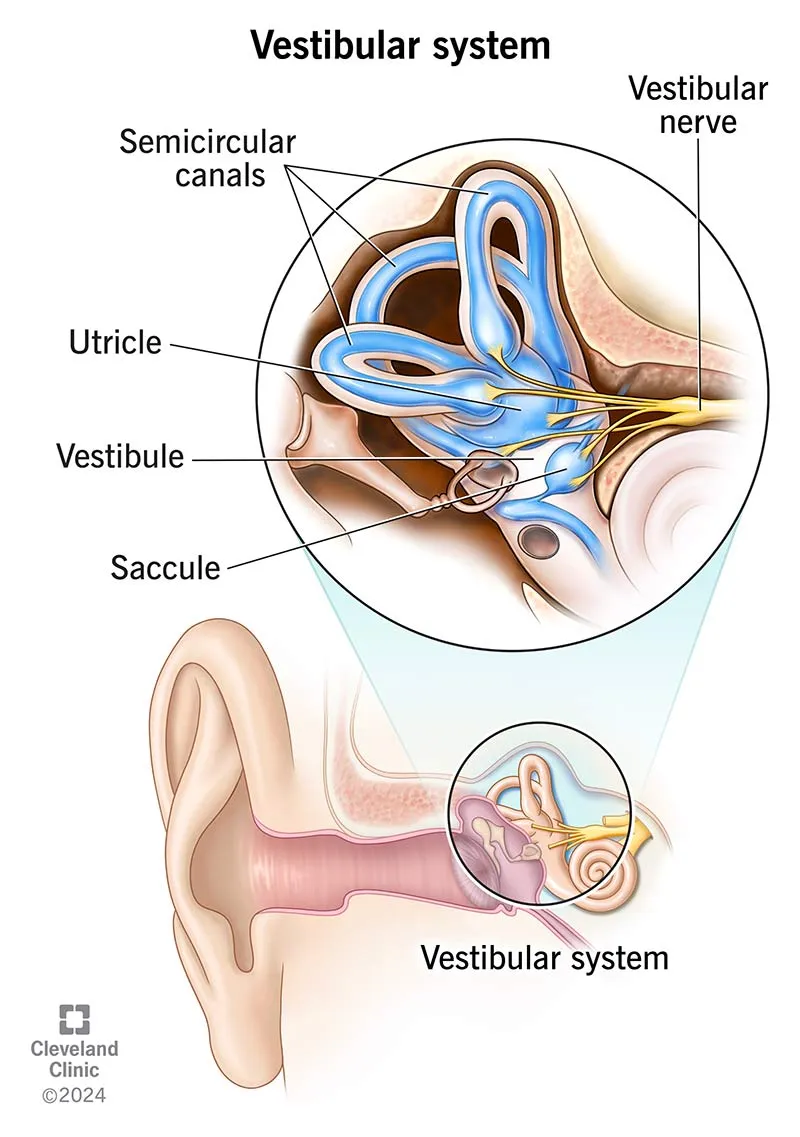
The vestibular apparatus contains 5 distinct sensory organs that detect rotational and linear motion with mathematical precision. Each semicircular canal responds to specific planes of rotation, while otolith organs detect gravity and linear acceleration through calcium carbonate crystals that are 3x denser than surrounding endolymph.
Semicircular Canal Mechanics: Rotational Motion Detection
The 3 semicircular canals form orthogonal planes for comprehensive angular motion detection:
-
Horizontal (Lateral) Canal
- Plane orientation: 30° tilted from true horizontal
- Optimal stimulus: Yaw rotation (head turning)
- Cupula deflection: Ampullopetal = excitation, Ampullofugal = inhibition
- Time constant: 5-20 seconds for cupula return
- Sensitivity threshold: 0.1°/second² angular acceleration
- Dynamic range: 0.1-500°/second angular velocity
-
Anterior (Superior) Canal
- Plane orientation: 45° to sagittal plane
- Paired function: With contralateral posterior canal
- Clinical testing: Dix-Hallpike maneuver activation
- BPPV involvement: 15% of cases (posterior canal: 80%)
- Nystagmus pattern: Rotatory with upbeating component
-
Posterior Canal
- Plane orientation: 45° to sagittal plane (opposite anterior)
- BPPV predilection: Most common otoconia deposition site
- Anatomical advantage: Most dependent position when upright
- Canalithiasis: Free-floating otoconia in canal
- Cupulolithiasis: Adherent otoconia on cupula
📌 Remember: HAP - Horizontal (yaw), Anterior (pitch + roll), Posterior (pitch + roll) canals detect all possible rotational movements through push-pull paired responses across bilateral vestibular organs
Otolith Organ Function: Gravity and Linear Acceleration
The utricle and saccule contain specialized hair cells embedded in otoconia-laden gelatinous membranes:
| Otolith Organ | Orientation | Primary Function | Hair Cell Count | Otoconia Properties |
|---|---|---|---|---|
| Utricle | Horizontal plane | Horizontal acceleration, head tilt | 30,000 | Calcium carbonate crystals |
| Saccule | Vertical plane | Vertical acceleration, gravity | 16,000 | 3x denser than endolymph |
| Macula | Sensory epithelium | Mechanotransduction | Variable density | 1-30 μm diameter |
| Striola | Central dividing line | Morphological polarization | Bidirectional | Kinocilium orientation |
| Otoconia | Calcium carbonate | Inertial mass enhancement | N/A | Specific gravity 2.7 |
Vestibulo-Ocular Reflex: Gaze Stabilization Engineering
The VOR maintains visual stability during head movements with remarkable precision:
-
VOR Gain Characteristics
- Normal gain: 0.8-1.2 (eye velocity/head velocity ratio)
- Latency: 5-10 milliseconds (fastest human reflex)
- Frequency response: Optimal 1-5 Hz (natural head movements)
- High-frequency VOR: Semicircular canal mediated
- Low-frequency VOR: Otolith and visual supplementation
- VOR suppression: Cerebellum-mediated during tracking
-
Clinical VOR Testing
- Head impulse test: High-frequency VOR assessment
- Caloric testing: Low-frequency horizontal canal function
- Rotary chair: Comprehensive frequency response analysis
- Abnormal gain: <0.6 or >1.4 indicates dysfunction
- Phase lag: >10° suggests central pathology
- Asymmetry: >25% between sides indicates unilateral loss
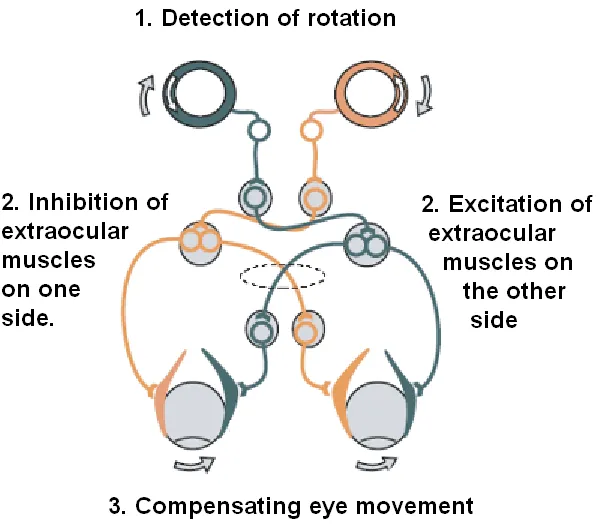
Central Vestibular Integration: Brainstem Processing Networks
Vestibular information integrates at 4 major brainstem nuclei with extensive connections:
- Vestibular Nuclear Complex
- Superior nucleus: VOR and vertical eye movements
- Lateral nucleus: Vestibulospinal reflexes, postural control
- Medial nucleus: Horizontal VOR, head-eye coordination
- Inferior nucleus: Velocity storage, commissural connections
- Commissural inhibition: Maintains baseline firing rates
- Velocity storage: Extends VOR time constant to 15-20 seconds
- Neural integrator: Converts velocity to position signals
💡 Master This: Unilateral vestibular loss creates asymmetric neural activity, causing spontaneous nystagmus beating away from the lesioned side. Central compensation occurs over 6-12 weeks through commissural rebalancing and substitution strategies
Vestibular Pathophysiology: Pattern Recognition Framework
Understanding vestibular dysfunction patterns enables rapid differential diagnosis:
-
Peripheral Vestibular Patterns
- Horizontal-rotatory nystagmus: Unidirectional, suppressed by fixation
- Hearing loss association: Common in labyrinthine disorders
- Severe vertigo: Acute onset, gradual improvement
- BPPV: Positional, fatigable, <60 seconds duration
- Vestibular neuritis: Continuous, days to weeks, no hearing loss
- Meniere's disease: Episodic, fluctuating hearing, aural fullness
-
Central Vestibular Patterns
- Pure vertical nystagmus: Direction-changing, not suppressed
- Neurological signs: Ataxia, diplopia, dysarthria
- Mild vertigo: Chronic imbalance, poor compensation
⚠️ Warning: Pure vertical nystagmus, direction-changing nystagmus, or nystagmus not suppressed by visual fixation suggests central pathology requiring immediate neurological evaluation
The vestibular system's mathematical precision enables spatial navigation and postural control through multisensory integration. Connect these balance mechanisms through olfactory and gustatory physiology to understand how chemical sensation contributes to environmental awareness and safety.
🎪 Balance Mastery: The Vestibular Control Network
🧪 Chemical Sensation: The Molecular Detection Network
Olfactory Transduction: Molecular Lock-and-Key Precision
The olfactory epithelium contains 6 million receptor cells expressing 350 different receptor proteins:
-
Olfactory Receptor Organization
- Receptor cell lifespan: 30-60 days (continuous regeneration)
- Cilia per cell: 10-30 with receptor proteins
- Axon convergence: 1,000:1 ratio to glomeruli
- Molecular detection: Shape-selective binding
- Threshold sensitivity: 10⁻¹² molar for some odorants
- Dynamic range: 10⁶-fold concentration differences
-
Signal Transduction Cascade
- G-protein coupling: Golf protein activation
- cAMP elevation: Adenylyl cyclase III activation
- Ion channel opening: Cyclic nucleotide-gated channels
- Depolarization: Na+ and Ca2+ influx
- Amplification: 1 molecule → 1,000+ ions
- Adaptation: Calcium-dependent desensitization
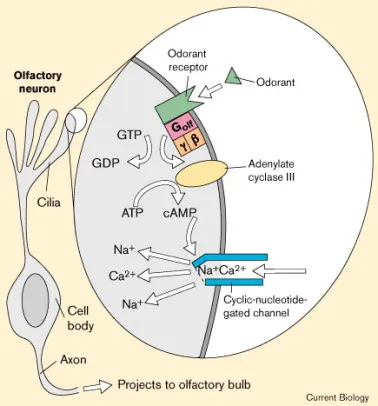
📌 Remember: CAGE - Cilia (detection), Axon (transmission), Glomerulus (integration), Epithelium (regeneration) represent the 4 key components of olfactory function, each vulnerable to specific pathological processes
Olfactory Pathway: Direct Limbic Access
Olfactory information travels the shortest sensory pathway to consciousness:
| Pathway Level | Structure | Function | Clinical Significance | Processing Time |
|---|---|---|---|---|
| Primary | Olfactory nerve | Axon bundles through cribriform | Trauma vulnerability | <5 ms |
| Secondary | Olfactory bulb | Glomerular processing | Tumor compression | 10-15 ms |
| Tertiary | Piriform cortex | Primary olfactory cortex | Seizure focus | 20-30 ms |
| Quaternary | Orbitofrontal | Conscious perception | Neurodegenerative loss | 50-100 ms |
| Limbic | Amygdala/hippocampus | Emotional/memory association | PTSD triggers | 30-50 ms |
Gustatory System: Five-Taste Integration Network
Taste perception involves 5 basic tastes processed through specialized receptor mechanisms:
-
Taste Receptor Distribution
- Sweet receptors: T1R2/T1R3 heterodimer, anterior tongue
- Umami receptors: T1R1/T1R3 heterodimer, widespread
- Bitter receptors: T2R family (25 subtypes), posterior tongue
- Evolutionary significance: Toxin detection mechanism
- Genetic variation: 25% population are supertasters
- Threshold sensitivity: 10⁻⁶ M for quinine
-
Salt and Sour Transduction
- Salt taste: ENaC channels (epithelial sodium channels)
- Sour taste: Acid-sensing ion channels and K+ channels
- Sodium detection: Direct ion channel activation
- Acid detection: pH-sensitive mechanisms
- Physiological role: Electrolyte and pH monitoring
Gustatory Pathways: Trigeminal Integration
Taste information travels through 3 cranial nerves with brainstem integration:
-
Peripheral Taste Innervation
- CN VII (Facial): Anterior 2/3 tongue via chorda tympani
- CN IX (Glossopharyngeal): Posterior 1/3 tongue and circumvallate papillae
- CN X (Vagus): Epiglottis and laryngeal taste buds
- Taste bud count: 10,000 total, 50-100 cells per bud
- Cell turnover: 7-10 days (rapid regeneration)
- Innervation density: 1 nerve fiber per 5 taste cells
-
Central Gustatory Processing
- Nucleus tractus solitarius: Primary gustatory nucleus
- Ventral posterior medial thalamus: Thalamic relay
- Primary gustatory cortex: Insula and frontal operculum
- Flavor integration: Olfactory + gustatory + trigeminal
- Hedonic processing: Orbitofrontal cortex evaluation
- Memory association: Hippocampal flavor-context linking
💡 Master This: Flavor perception requires integration of taste (5 basic tastes), smell (thousands of odorants), and trigeminal sensation (temperature, texture, irritation). Anosmia reduces flavor perception by 80%, explaining why patients report "taste loss" when olfaction is impaired
Clinical Chemical Sensation Disorders
Understanding chemosensory dysfunction patterns enables targeted diagnosis:
-
Olfactory Disorders (Prevalence: 5-15%)
- Conductive anosmia: Nasal obstruction, rhinosinusitis
- Sensorineural anosmia: Viral infection, head trauma, aging
- Central anosmia: Neurodegenerative disease, brain tumor
- Post-viral anosmia: 40% recovery rate over 2 years
- Traumatic anosmia: 10% recovery rate (cribriform plate injury)
- Parosmia: Distorted smell perception during nerve regeneration
-
Gustatory Disorders (Prevalence: 1-5%)
- Medication-induced: >250 drugs affect taste
- Nutritional deficiency: Zinc, vitamin B12, folate
- Neurological damage: Bell's palsy, stroke, tumor
- Zinc deficiency: Hypogeusia in 15% of elderly
- Medication effects: ACE inhibitors, antibiotics, chemotherapy
- Recovery potential: Variable depending on etiology
⚠️ Warning: Sudden anosmia in young patients may indicate anterior skull base tumor or CSF leak. Unilateral anosmia requires MRI evaluation to exclude olfactory groove meningioma or cribriform plate pathology
Chemical sensation disorders significantly impact quality of life and nutritional status. Connect these molecular detection systems through laryngeal anatomy and physiology to understand how voice production and airway protection integrate with chemical sensing for comprehensive upper airway function.
🧪 Chemical Sensation: The Molecular Detection Network
🎵 Voice Production: The Laryngeal Instrument Mastery
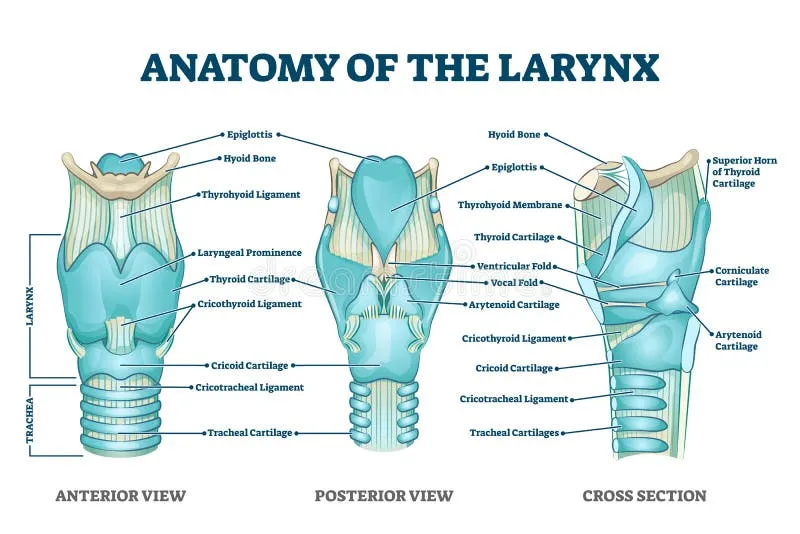
The larynx serves 3 primary functions: phonation (voice production), respiration (airway maintenance), and deglutition (aspiration prevention). Understanding the biomechanics of vocal fold vibration and neural control of laryngeal muscles reveals how voice disorders develop and guides therapeutic interventions.
Laryngeal Framework: Cartilaginous Architecture
The laryngeal skeleton consists of 9 cartilages forming a 3-level functional unit:
-
Major Cartilages
- Thyroid cartilage: Largest, forms anterior prominence (Adam's apple)
- Cricoid cartilage: Only complete ring, foundation of larynx
- Arytenoid cartilages (paired): Vocal process and muscular process
- Vocal fold attachment: Anterior vocal process
- Muscle attachment: Posterior muscular process
- Cricoarytenoid joint: Sliding and rotating movements
-
Accessory Cartilages
- Epiglottis: Aspiration protection during swallowing
- Corniculate cartilages: Arytenoid apex extensions
- Cuneiform cartilages: Aryepiglottic fold support
- Elastic cartilage: Epiglottis, corniculate, cuneiform
- Hyaline cartilage: Thyroid, cricoid, arytenoid
- Ossification: Begins age 20, complete by 65
📌 Remember: TRACE - Thyroid (shield), Ring (cricoid), Arytenoid (ladles), Corniculate (horns), Epiglottis (lid) form the laryngeal framework with specific joint movements enabling vocal fold positioning
Intrinsic Laryngeal Muscles: Vocal Fold Control System
5 paired intrinsic muscles control vocal fold position, tension, and length:
| Muscle | Innervation | Action | Clinical Significance | Paralysis Effect |
|---|---|---|---|---|
| Cricothyroid | Superior laryngeal nerve | Vocal fold elongation/tension | Pitch control | Pitch limitation |
| Posterior cricoarytenoid | Recurrent laryngeal nerve | Vocal fold abduction | Only abductor | Airway obstruction |
| Lateral cricoarytenoid | Recurrent laryngeal nerve | Vocal fold adduction | Voice initiation | Breathy voice |
| Transverse arytenoid | Recurrent laryngeal nerve | Posterior glottal closure | Cough effectiveness | Aspiration risk |
| Thyroarytenoid/vocalis | Recurrent laryngeal nerve | Vocal fold shortening | Voice quality | Vocal instability |
Vocal Fold Vibration: Biomechanical Oscillation
Vocal fold vibration follows myoelastic-aerodynamic principles with complex wave propagation:
-
Vibratory Cycle Phases
- Opening phase: Subglottic pressure overcomes vocal fold resistance
- Closing phase: Bernoulli effect and elastic recoil restore closure
- Closed phase: Pressure buildup for next cycle
- Fundamental frequency: Male 85-180 Hz, Female 165-265 Hz
- Vibratory amplitude: 1-2 mm lateral excursion
- Mucosal wave: Inferior to superior propagation
-
Vocal Fold Histology
- Epithelium: Stratified squamous, protective barrier
- Superficial lamina propria: Reinke's space, loose connective tissue
- Intermediate lamina propria: Elastic fibers
- Deep lamina propria: Collagen fibers
- Vocalis muscle: Thyroarytenoid muscle body
- Cover-body model: Epithelium + superficial LP = cover
- Transition zone: Intermediate + deep LP = ligament
- Body: Vocalis muscle = tension control
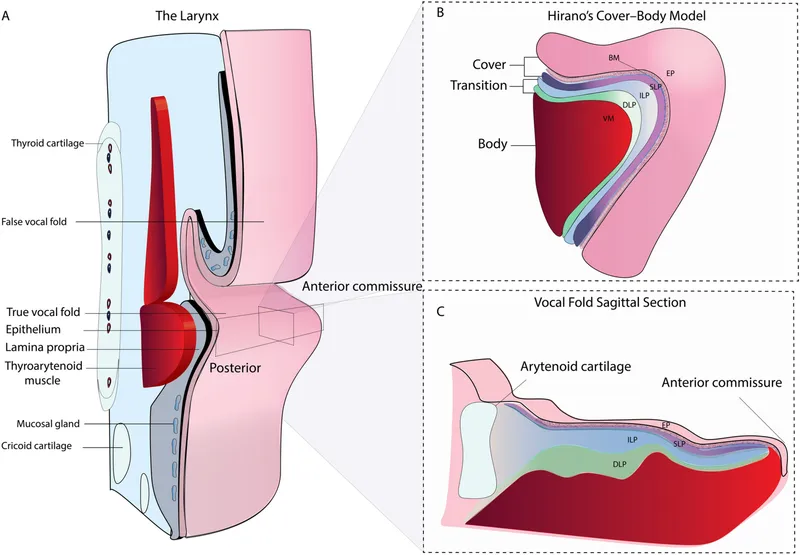
Neural Control: Laryngeal Innervation Precision
Laryngeal function requires precise neural coordination through 2 branches of the vagus nerve:
-
Superior Laryngeal Nerve
- Internal branch: Sensory innervation above vocal folds
- External branch: Motor innervation to cricothyroid muscle
- Sensory function: Aspiration protection reflex
- Motor function: Vocal fold tensing for pitch control
- Clinical testing: Laryngeal cough reflex
-
Recurrent Laryngeal Nerve
- Motor innervation: All intrinsic muscles except cricothyroid
- Sensory innervation: Below vocal folds
- Left RLN: 45 cm course around aortic arch
- Right RLN: 5 cm course around subclavian artery
- Vulnerability: Thyroid surgery, cardiac surgery, lung cancer
💡 Master This: Superior laryngeal nerve injury causes pitch limitation and aspiration (loss of sensation), while recurrent laryngeal nerve injury causes vocal fold paralysis with voice changes and potential airway compromise. Bilateral RLN paralysis is a surgical emergency
Voice Production Physiology: Acoustic Engineering
Voice production involves 3 subsystems working in coordinated precision:
-
Respiratory Subsystem
- Subglottic pressure: 5-10 cm H2O for conversational speech
- Airflow rate: 100-200 mL/second during phonation
- Vital capacity: 3,000-5,000 mL (speech breathing reserve)
- Inspiratory reserve: Quick inspiration between phrases
- Expiratory control: Prolonged controlled expiration
- Speech breathing: 10-15% inspiration, 85-90% expiration
-
Phonatory Subsystem
- Vocal fold contact: 40-60% of vibratory cycle
- Glottal resistance: Variable with vocal fold adduction
- Harmonic structure: Fundamental + overtones
- Jitter: <1% cycle-to-cycle frequency variation
- Shimmer: <3% cycle-to-cycle amplitude variation
- Noise-to-harmonic ratio: <0.15 for normal voice
-
Resonatory Subsystem
- Vocal tract length: Male 17 cm, Female 14 cm
- Formant frequencies: Vowel identification markers
- Resonance modification: Articulatory adjustments
- F1 (first formant): Tongue height correlation
- F2 (second formant): Tongue advancement correlation
- Vocal tract filtering: Harmonic enhancement/suppression
⚠️ Warning: Voice overuse or trauma can cause vocal fold hemorrhage, polyps, or nodules. Hoarseness >2 weeks requires laryngoscopic evaluation to exclude malignancy, especially in smokers >40 years
Voice production represents the integration of respiratory drive, laryngeal biomechanics, and acoustic resonance. Connect these phonatory principles through swallowing physiology to understand how the larynx coordinates airway protection with voice production in comprehensive upper airway management.
🎵 Voice Production: The Laryngeal Instrument Mastery
🛡️ Airway Protection: The Swallowing Safety Network
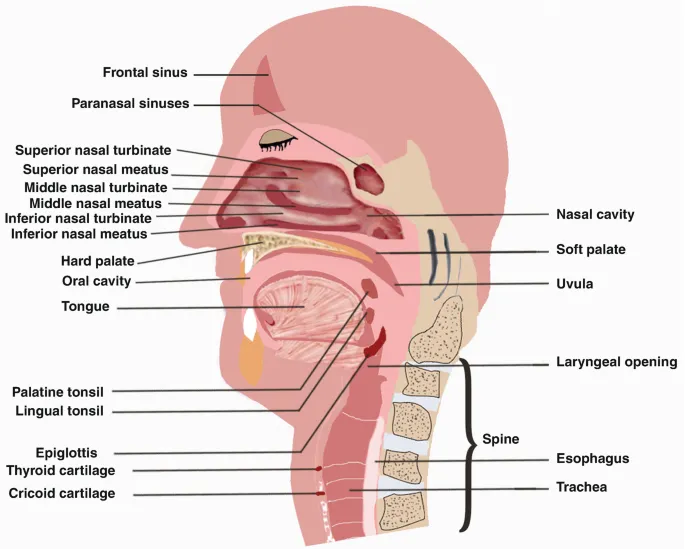
Swallowing represents the most complex motor act performed by humans, requiring precise temporal coordination between respiratory, phonatory, and digestive systems. Understanding the sequential muscle activation and protective mechanisms reveals how dysphagia develops and guides therapeutic interventions to prevent aspiration pneumonia.
Swallowing Phase Architecture: Four-Stage Coordination
The swallowing process involves 4 distinct phases with specific timing and muscle coordination:
-
Oral Preparatory Phase (Variable duration)
- Mastication: 15-25 chews per bolus (solid food)
- Bolus formation: Tongue manipulation and saliva mixing
- Voluntary control: Conscious initiation and timing
- Saliva production: 1-2 L/day, pH 6.5-7.5
- Enzyme activity: Amylase begins starch digestion
- Bolus consistency: Optimal 1,000-50,000 cP viscosity
-
Oral Transit Phase (1-2 seconds)
- Tongue propulsion: Sequential anterior-to-posterior contraction
- Bolus transport: Tongue-palate contact creates pressure gradient
- Trigger initiation: Faucial arch stimulation
- Pressure generation: Up to 200 mmHg tongue-palate contact
- Transit velocity: 10-25 cm/second bolus movement
- Volume accommodation: 5-20 mL typical bolus size
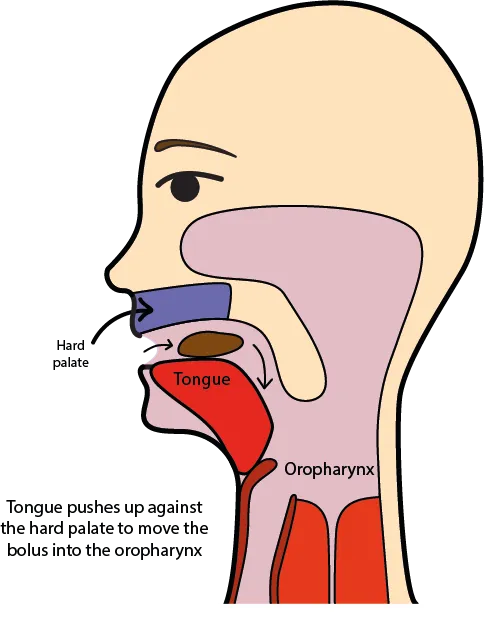
📌 Remember: TOPS - Tongue (propulsion), Oral (transit), Pharyngeal (protection), Swallow (safety) represent the 4 critical elements of safe deglutition with precise timing and muscle coordination
Pharyngeal Phase: Rapid Protective Sequence
The pharyngeal phase lasts 1 second but involves >20 coordinated actions:
| Protective Action | Timing (ms) | Muscle Groups | Clinical Significance | Failure Consequence |
|---|---|---|---|---|
| Soft palate elevation | 0-200 | Levator veli palatini | Nasal regurgitation prevention | Nasopharyngeal reflux |
| Laryngeal elevation | 100-300 | Suprahyoid muscles | Airway protection | Aspiration risk |
| Vocal fold closure | 150-250 | Intrinsic laryngeal | Glottic seal | Penetration/aspiration |
| Epiglottic inversion | 200-400 | Passive mechanism | Laryngeal vestibule protection | Laryngeal penetration |
| Pharyngeal contraction | 300-700 | Pharyngeal constrictors | Bolus propulsion | Pharyngeal residue |
Neural Control Networks: Brainstem Swallowing Centers
Swallowing coordination involves multiple brainstem nuclei with bilateral innervation:
-
Central Pattern Generator
- Nucleus tractus solitarius: Sensory integration and swallow initiation
- Nucleus ambiguus: Motor output to pharyngeal and laryngeal muscles
- Reticular formation: Timing coordination and respiratory integration
- Bilateral representation: Stroke rarely causes complete dysphagia
- Sensory threshold: Decreased with aging and neurological disease
- Motor coordination: Millisecond precision required
-
Cranial Nerve Integration
- CN V (Trigeminal): Mastication and oral sensation
- CN VII (Facial): Lip seal and buccal control
- CN IX (Glossopharyngeal): Pharyngeal sensation and swallow trigger
- CN X (Vagus): Pharyngeal and laryngeal motor control
- CN XII (Hypoglossal): Tongue movement and bolus manipulation
Airway Protection Mechanisms: Multi-Level Safety System
The larynx employs 3 levels of airway protection during swallowing:
-
Level 1: Epiglottis (Supraglottic)
- Passive deflection: Bolus flow and laryngeal elevation
- Coverage: Laryngeal inlet protection
- Effectiveness: Reduces but doesn't eliminate aspiration risk
- Epiglottectomy: Compatible with safe swallowing
- Primary function: Bolus direction rather than complete seal
-
Level 2: False Vocal Folds (Glottic)
- Active adduction: Muscle contraction creates tight seal
- Pressure resistance: Withstands high pharyngeal pressures
- Duration: Sustained closure throughout pharyngeal phase
-
Level 3: True Vocal Folds (Subglottic)
- Final barrier: Last protection against aspiration
- Cough reflex: Expulsive force if penetration occurs
- Sensitivity: Highest sensory innervation density
💡 Master This: Silent aspiration occurs when sensory feedback is impaired (stroke, intubation, aging), preventing cough reflex activation. Videofluoroscopy or FEES (fiberoptic endoscopic evaluation) can detect silent aspiration in 40% of dysphagic patients
Dysphagia Assessment: Clinical Pattern Recognition
Understanding dysphagia patterns enables targeted intervention strategies:
-
Oral Phase Dysfunction
- Poor bolus control: Premature spillage into pharynx
- Reduced tongue strength: Incomplete oral transit
- Oral residue: Food pooling in oral cavity
- Stroke prevalence: 25-50% of acute stroke patients
- Tongue pressure: <20 kPa indicates significant weakness
- Recovery potential: Good with targeted therapy
-
Pharyngeal Phase Dysfunction
- Delayed swallow initiation: >1 second trigger delay
- Reduced laryngeal elevation: <2 cm hyoid movement
- Incomplete glottic closure: Vocal fold paralysis or weakness
- Aspiration pneumonia: 50% mortality in elderly
- Penetration-Aspiration Scale: 8-point severity rating
- Therapeutic options: Swallow therapy, diet modification, surgical intervention
⚠️ Warning: New-onset dysphagia in adults requires comprehensive evaluation to exclude structural lesions (tumors, strictures) and neurological disorders (stroke, Parkinson's disease, ALS). Progressive dysphagia with weight loss mandates urgent endoscopic or radiographic evaluation
The swallowing mechanism represents evolutionary perfection in airway protection while maintaining nutritional function. These protective reflexes and coordinated muscle actions ensure safe deglutition across millions of swallows throughout life, with failure leading to life-threatening complications.
🛡️ Airway Protection: The Swallowing Safety Network
🎯 ENT Clinical Arsenal: Rapid Mastery Framework
This clinical arsenal synthesizes anatomical knowledge, physiological understanding, and pathological recognition into actionable frameworks for immediate clinical application. Master these essential tools and critical thresholds to transform theoretical knowledge into clinical expertise.
Essential Clinical Thresholds: The Numbers That Matter
Critical quantitative landmarks for immediate clinical decision-making:
-
Hearing Assessment Thresholds
- Normal hearing: ≤25 dB HL across speech frequencies
- Mild hearing loss: 26-40 dB HL (difficulty in noise)
- Moderate hearing loss: 41-70 dB HL (requires amplification)
- Severe hearing loss: 71-90 dB HL (limited speech understanding)
- Profound hearing loss: >90 dB HL (cochlear implant candidate)
- Speech frequencies: 500, 1000, 2000, 4000 Hz
- Word recognition: >90% normal, <50% suggests retrocochlear
- Acoustic reflex: Absent at >90 dB sensation level
-
Vestibular Function Markers
- Normal VOR gain: 0.8-1.2 (head impulse test)
- Caloric asymmetry: <25% between ears (normal)
- Spontaneous nystagmus: >5°/second suggests acute vestibular loss
- BPPV duration: <60 seconds per positional episode
- Dix-Hallpike: Rotatory-upbeating nystagmus (posterior canal)
- Supine roll test: Horizontal nystagmus (horizontal canal)
- Recovery time: 80% resolve within 6 months
📌 Remember: HAVN - Hearing (25 dB), Acoustic reflex (90 dB), VOR gain (0.8-1.2), Nystagmus (<25% asymmetry) represent critical thresholds for normal function across ENT subspecialties
Rapid Pattern Recognition: See This, Think That
High-yield clinical correlations for immediate diagnostic consideration:
| Clinical Presentation | Think First | Key Discriminators | Urgent Actions | Success Rate |
|---|---|---|---|---|
| Sudden hearing loss | Viral labyrinthitis | Unilateral, sensorineural | Steroids within 72 hours | 85% recovery |
| Vertigo + hearing loss | Meniere's disease | Episodic, fluctuating | Low-sodium diet, diuretics | 70% control |
| Facial paralysis | Bell's palsy | Acute onset, no other signs | Steroids within 48 hours | 90% recovery |
| Hoarseness >2 weeks | Laryngeal pathology | Smoking history, age >40 | Laryngoscopy immediately | 95% detection |
| Unilateral nasal obstruction | Structural abnormality | Progressive, unilateral | Endoscopy + imaging | 90% diagnosis |
Treatment Algorithm Mastery: Evidence-Based Protocols
Systematic treatment approaches with quantified outcomes:
-
Acute Otitis Media Management
- Observation: 48-72 hours if >2 years old, non-toxic
- Antibiotic indication: <6 months, bilateral, severe symptoms
- First-line therapy: Amoxicillin 80-90 mg/kg/day × 10 days
- Treatment failure: 48-72 hours no improvement
- Second-line: Amoxicillin-clavulanate or cephalexin
- Recurrent AOM: ≥3 episodes in 6 months (consider tubes)
-
Chronic Rhinosinusitis Protocol
- Medical therapy: Nasal steroids + saline irrigation × 12 weeks
- Antibiotic course: Doxycycline 100 mg BID × 3 weeks
- Surgical indication: Failed medical therapy + CT evidence
- Symptom improvement: 80% with appropriate medical therapy
- Surgical success: 85-90% symptom resolution/improvement
- Revision rate: 10-15% require additional procedures
Emergency ENT Recognition: Red Flag Protocols
Life-threatening conditions requiring immediate intervention:
-
Airway Emergencies
- Stridor at rest: Impending airway obstruction
- Bilateral vocal fold paralysis: Surgical airway required
- Epiglottitis: Avoid examination, secure airway in OR
- Tracheostomy indications: Unable to intubate, prolonged intubation
- Cricothyrotomy: Emergency surgical airway access
- Success rate: >95% when performed correctly
-
Hemorrhage Control
- Posterior epistaxis: Sphenopalatine artery ligation
- Post-tonsillectomy bleeding: Return to OR if active bleeding
- Carotid blowout: Immediate vascular surgery consultation
💡 Master This: Stridor indicates >50% airway obstruction. Inspiratory stridor suggests supraglottic pathology, expiratory stridor indicates subglottic narrowing, and biphasic stridor suggests glottic or subglottic obstruction requiring immediate airway assessment
Surgical Decision Framework: When to Operate
Evidence-based surgical indications with outcome predictions:
-
Tympanoplasty Indications
- Hearing improvement goal: >15 dB air-bone gap
- Success rate: 85-95% graft take rate
- Hearing improvement: 70-80% achieve <20 dB gap
- Contraindications: Active infection, poor Eustachian tube function
- Revision rate: 10-15% require additional surgery
-
Functional Endoscopic Sinus Surgery
- Medical therapy failure: 12 weeks appropriate treatment
- CT scan evidence: Mucosal thickening, obstruction
- Quality of life: Significant functional impairment
- Complication rate: <5% in experienced hands
- Major complications: CSF leak (<1%), orbital injury (<1%)
- Symptom improvement: 80-90% patients report benefit
⚠️ Warning: Unilateral nasal polyps in adults require biopsy to exclude malignancy. Inverted papilloma has 10-15% malignant transformation rate and requires complete excision with negative margins
This clinical arsenal provides systematic frameworks for ENT diagnosis and management, enabling rapid pattern recognition and evidence-based treatment decisions across the full spectrum of otolaryngologic disorders.
🎯 ENT Clinical Arsenal: Rapid Mastery Framework
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app












