Neurotology

On this page
🧠 Neurotology: The Inner Ear's Command Center
Neurotology bridges the delicate interface where the inner ear's sensory machinery meets the brain's processing networks, governing balance, hearing, and spatial orientation. You'll learn how disruptions in this command center create distinct clinical patterns, master the diagnostic tools that pinpoint lesions from labyrinth to cortex, and build treatment algorithms that restore function or compensate for loss. This lesson transforms abstract vestibular and auditory physiology into practical clinical reasoning, equipping you to confidently navigate vertigo, hearing loss, and the multisensory disorders that challenge even experienced clinicians.
The Neurotologic Territory: Anatomical Foundations
The neurotologic domain encompasses several critical anatomical regions:
-
Temporal Bone Complex
- Petrous pyramid: houses the entire inner ear apparatus
- Internal auditory canal (IAC): 8mm diameter conduit for cranial nerves VII and VIII
- Jugular foramen: 12-15mm opening for cranial nerves IX, X, XI
- Pars nervosa: medial compartment for CN IX
- Pars vascularis: lateral compartment for jugular bulb
-
Inner Ear Architecture
- Cochlea: 2.5 turns, 35mm total length when uncoiled
- Vestibular labyrinth: 3 semicircular canals + 2 otolith organs
- Endolymphatic system: 150μL total volume with +80mV potential
- Perilymph: high sodium (140mEq/L), low potassium (5mEq/L)
- Endolymph: low sodium (1mEq/L), high potassium (150mEq/L)

📌 Remember: SCALP for temporal bone layers - Skin, Connective tissue, Aponeurosis, Loose connective tissue, Pericranium. Each layer has specific surgical implications for neurotologic approaches.
Cerebellopontine Angle: The Neurotologic Crossroads
The cerebellopontine angle (CPA) represents neurotology's most critical anatomical region, where 85% of acoustic neuromas arise:
| Structure | Dimension | Clinical Significance | Pathology Risk |
|---|---|---|---|
| CPA Cistern | 15-20mm depth | CSF cushioning space | Tumor expansion zone |
| Facial Nerve | 23-25mm length | Motor function preservation | Surgical injury risk |
| Cochlear Nerve | 8-10mm to cochlea | Hearing preservation | Compression vulnerability |
| Trigeminal Nerve | 17-20mm cisternal | Facial sensation | Neurovascular conflict |
| AICA Loop | Variable position | Vascular supply | Surgical landmark |
💡 Master This: The 50-50-90 rule for acoustic neuromas: 50% grow significantly, 50% remain stable, and 90% of growing tumors require intervention within 5 years of diagnosis.
Understanding neurotologic anatomy provides the foundation for recognizing how pathological processes disrupt normal function, leading to the characteristic symptom complexes that define this subspecialty.
🧠 Neurotology: The Inner Ear's Command Center
⚡ Pathophysiology: The Disruption Cascade
Vascular Compromise: The Ischemic Cascade
The inner ear's exquisite vascular supply makes it vulnerable to ischemic injury:
-
Labyrinthine Artery Territory
- Single end-artery system with no collateral circulation
- Supplies 100% of cochlear and vestibular function
- Occlusion causes immediate and irreversible hearing loss
- Sudden sensorineural hearing loss: 90% unilateral
- Recovery potential: <30% without treatment
- Steroid response: 65% improvement if started within 72 hours
-
Vertebrobasilar Insufficiency
- Affects central vestibular pathways
- Causes episodic vertigo lasting minutes to hours
- Associated symptoms: diplopia (40%), dysarthria (35%), ataxia (60%)
📌 Remember: HINTS examination for central vs peripheral vertigo - Head impulse test, Inystagmus pattern, Test of skew, Standing balance. Central patterns show normal head impulse, direction-changing nystagmus, positive skew deviation.
Inflammatory Processes: The Immune Response
Neurotologic inflammation follows distinct patterns based on anatomical involvement:
| Condition | Location | Timeline | Recovery Rate | Key Features |
|---|---|---|---|---|
| Vestibular Neuritis | Superior vestibular nerve | 7-14 days acute | 85% compensation | Horizontal nystagmus |
| Labyrinthitis | Entire labyrinth | 3-7 days acute | 60% full recovery | Hearing loss + vertigo |
| Autoimmune Inner Ear | Bilateral cochlea | Weeks to months | 70% steroid response | Progressive SNHL |
| Meningogenic Labyrinthitis | Cochlea via modiolus | Hours to days | 10% hearing recovery | Bacterial spread |
| Ramsay Hunt Syndrome | Geniculate ganglion | 2-5 days progression | 50% facial recovery | Vesicular eruption |
Mechanical Disruption: The Pressure Paradigm
Mechanical forces create characteristic neurotologic syndromes through pressure-related mechanisms:
-
Endolymphatic Hydrops (Ménière's Disease)
- Endolymphatic volume increases 2-3 fold
- Reissner's membrane distension and rupture
- Fluctuating hearing loss in low frequencies initially
- Attacks last 20 minutes to 24 hours
- Tinnitus precedes 85% of attacks
- Drop attacks (Tumarkin crisis) in 10% of patients
-
Perilymphatic Fistula
- Round window (60%) or oval window (40%) rupture
- Pressure-induced symptoms: Hennebert's sign positive
- Pneumolabyrinth on CT in <5% of cases
💡 Master This: The glycerol test demonstrates >10dB hearing improvement in 70% of Ménière's patients by temporarily dehydrating endolymphatic hydrops - positive test confirms diagnosis with 85% specificity.
These pathophysiological mechanisms create the clinical patterns that enable systematic diagnostic approaches in neurotologic practice.
⚡ Pathophysiology: The Disruption Cascade
🎯 Clinical Recognition: The Pattern Matrix

The Vertigo Discrimination Matrix
Vertigo presentations follow predictable patterns based on anatomical involvement and temporal characteristics:
-
Peripheral Vertigo Patterns
- Acute onset: seconds to minutes to peak intensity
- Rotatory quality: patient feels room spinning
- Nausea/vomiting: present in >90% of acute cases
- Hearing symptoms: tinnitus (70%), fullness (60%), hearing loss (40%)
- Duration: hours to days for vestibular neuritis
- Triggers: positional for BPPV (<60 seconds)
- Associated symptoms: minimal neurological signs
-
Central Vertigo Patterns
- Gradual onset: minutes to hours progression
- Imbalance quality: patient feels self-moving
- Nausea/vomiting: mild or absent
- Neurological symptoms: diplopia (45%), dysarthria (35%), facial numbness (25%)
- Duration: days to weeks persistent
- Triggers: non-positional or multiple positions
- Associated symptoms: brainstem or cerebellar signs
📌 Remember: STANDING for peripheral vertigo features - Sudden onset, Tinnitus present, Auditory symptoms, Nystagmus horizontal, Duration limited, Intense nausea, No neurological signs, Gaze-evoked absent.
Hearing Loss Classification Framework
Sensorineural hearing loss patterns provide crucial diagnostic information:
| Pattern | Onset | Frequencies | Recovery | Associated Features | Likely Diagnosis |
|---|---|---|---|---|---|
| Sudden | <72 hours | All frequencies | 30% spontaneous | Unilateral, tinnitus | Viral labyrinthitis |
| Fluctuating | Episodic | Low frequency | Variable | Vertigo, fullness | Ménière's disease |
| Progressive | Months-years | High frequency | None | Unilateral | Acoustic neuroma |
| Bilateral | Gradual | High frequency | None | Family history | Presbycusis |
| Conductive | Variable | All frequencies | Surgical | Middle ear signs | Otosclerosis |
Facial Nerve Localization Patterns
Facial nerve dysfunction localizes precisely based on associated symptoms:
-
Cerebellopontine Angle Lesions
- Gradual onset facial weakness over weeks to months
- Hearing loss precedes facial symptoms in 85%
- Corneal reflex diminished in 60%
- Acoustic reflex absent in >90%
-
Internal Auditory Canal Lesions
- Sudden onset facial paralysis
- Hearing loss concurrent with facial symptoms
- Vestibular symptoms in 70%
- Taste preserved (chorda tympani spared)
-
Tympanic Segment Lesions
- Facial paralysis with hyperacusis
- Taste loss in anterior 2/3 tongue
- Lacrimation decreased
- Acoustic reflex absent
💡 Master This: The House-Brackmann scale grades facial function from I (normal) to VI (complete paralysis) - Grade III or worse at 3 weeks predicts <50% chance of complete recovery without intervention.
These recognition patterns enable rapid triage and appropriate diagnostic workup in neurotologic emergencies.
🎯 Clinical Recognition: The Pattern Matrix
🔬 Diagnostic Precision: The Investigation Arsenal
Audiological Assessment: The Hearing Detective
Comprehensive audiological evaluation provides the foundation for neurotologic diagnosis:
-
Pure Tone Audiometry Standards
- Frequency range: 250Hz to 8000Hz minimum
- Threshold precision: 5dB increments
- Bone conduction: essential for air-bone gap calculation
- Speech audiometry: SRT within 10dB of PTA
- Word recognition: >90% normal, <50% suggests retrocochlear
- Rollover phenomenon: >20% decrease suggests acoustic neuroma
-
Tympanometry Patterns
- Type A: normal middle ear function (0.3-1.5mL compliance)
- Type B: flat curve suggests effusion or perforation
- Type C: negative pressure (<-150daPa) suggests Eustachian dysfunction
- Type As: reduced compliance (<0.3mL) suggests otosclerosis
- Type Ad: hypercompliance (>1.5mL) suggests ossicular disruption
📌 Remember: TORCH for acoustic reflex testing - Tensor tympani (CN V), Ossicular chain, Recurrent laryngeal (stapedius via CN VII), Cochlear nerve, Hearing threshold. Absent reflexes with normal hearing suggest retrocochlear pathology.
Vestibular Function Testing: The Balance Laboratory
Sophisticated vestibular testing localizes dysfunction within the vestibular system:
| Test | Normal Values | Abnormal Findings | Clinical Significance |
|---|---|---|---|
| Caloric Testing | 20-50°/sec peak SPV | >25% weakness | Horizontal canal function |
| Head Impulse Test | Corrective saccades absent | Saccades present | High-frequency VOR |
| Rotary Chair | Phase <10°, Gain 0.4-1.0 | Abnormal phase/gain | Low-frequency VOR |
| VEMP Testing | P1-N1 >10μV | Absent/reduced | Otolith function |
| Posturography | <2° sway, 85% equilibrium | Increased sway | Balance integration |
Advanced Imaging: The Structural Revelation
High-resolution imaging reveals structural abnormalities with extraordinary detail:
-
MRI Protocol Specifications
- T1 with gadolinium: 1mm slices through IAC
- T2 FIESTA/CISS: 0.5mm slices for cranial nerve visualization
- FLAIR sequences: detect endolymphatic hydrops after gadolinium
- DWI sequences: differentiate epidermoid from arachnoid cyst
-
CT Temporal Bone Indications
- 0.5mm slice thickness with bone algorithm
- Conductive hearing loss workup
- Trauma evaluation
- Chronic otitis media complications
- Congenital anomalies assessment
Electrophysiological Testing: The Neural Network
Electrophysiological studies assess neural pathway integrity:
-
Auditory Brainstem Response (ABR)
- Wave I: cochlear nerve (1.5ms)
- Wave III: superior olivary complex (3.5ms)
- Wave V: lateral lemniscus/inferior colliculus (5.5ms)
- Interwave intervals: I-III (2.0ms), III-V (2.0ms), I-V (4.0ms)
- Prolonged latencies: suggest retrocochlear pathology
- Absent waves: indicate severe neural dysfunction
-
Electrocochleography (ECochG)
- SP/AP ratio: >0.37 suggests endolymphatic hydrops
- Sensitivity: 60% for Ménière's disease
- Specificity: 90% when combined with clinical criteria
💡 Master This: ABR wave V latency increases 0.1ms per decade after age 30 - age-corrected interaural differences >0.2ms suggest retrocochlear pathology with 85% sensitivity for acoustic neuromas >1cm.
These diagnostic tools create a comprehensive assessment framework that localizes neurotologic pathology with remarkable precision.
🔬 Diagnostic Precision: The Investigation Arsenal
⚕️ Treatment Algorithms: The Therapeutic Precision
Medical Management Protocols
Evidence-based medical therapy targets specific pathophysiological mechanisms:
-
Sudden Sensorineural Hearing Loss Protocol
- Oral prednisone: 1mg/kg/day (max 80mg) for 7 days, then taper
- Intratympanic steroids: 40mg/mL methylprednisolone if oral contraindicated
- Hyperbaric oxygen: 2.5 ATA for 90 minutes if started within 3 months
- Salvage therapy: intratympanic steroids if <50% recovery at 4 weeks
- Success rates: 65% with oral steroids, 45% with intratympanic
- Time window: maximum benefit within 72 hours
-
Ménière's Disease Management Ladder
- Dietary modification: <2g sodium/day, caffeine restriction
- Diuretics: hydrochlorothiazide 25mg + triamterene 37.5mg daily
- Betahistine: 16mg TID (not FDA approved in US)
- Intratympanic steroids: 40mg/mL every 3-4 weeks × 3 doses
- Vertigo control: 85% with dietary changes, 70% with diuretics
- Hearing preservation: 60% maintain stable thresholds
📌 Remember: VITAMINS for Ménière's medical management - Vestibular suppressants (acute), Intratympanic steroids, Triamterene/HCTZ, Avoid caffeine, Meclizine PRN, Injections (gentamicin), No salt diet, Surgery (last resort).
Surgical Decision Algorithms
Surgical intervention follows evidence-based algorithms considering multiple factors:
| Condition | Surgical Threshold | Procedure Options | Success Rates | Complications |
|---|---|---|---|---|
| Acoustic Neuroma | >2.5cm or symptoms | Microsurgery vs SRS | 95% tumor control | 15% facial weakness |
| BPPV (refractory) | Failed canalith repositioning | Posterior canal occlusion | 90% vertigo cure | 30% SNHL risk |
| Ménière's (intractable) | Failed medical therapy | Endolymphatic sac surgery | 70% vertigo control | 10% hearing loss |
| Otosclerosis | >30dB conductive loss | Stapedectomy | 90% hearing improvement | 1% dead ear |
| Chronic otitis media | Cholesteatoma present | Mastoidectomy | 85% dry ear | 5% facial nerve injury |
| flowchart TD |
Start["<b>🩺 Acoustic Neuroma</b><br><span style='display:block; text-align:left; color:#555'>• Vestibular Schwannoma</span><span style='display:block; text-align:left; color:#555'>• Cranial nerve 8</span>"]
Size["<b>📋 Size Assessment</b><br><span style='display:block; text-align:left; color:#555'>• MRI measurement</span><span style='display:block; text-align:left; color:#555'>• Max diameter cm</span>"]
Obs["<b>💊 Observation vs SRS</b><br><span style='display:block; text-align:left; color:#555'>• Wait and watch</span><span style='display:block; text-align:left; color:#555'>• Radiosurgery opt</span>"]
SrsSurg["<b>💊 SRS vs Surgery</b><br><span style='display:block; text-align:left; color:#555'>• Gamma Knife SRS</span><span style='display:block; text-align:left; color:#555'>• Microsurgery opt</span>"]
Resection["<b>💊 Surgical Resection</b><br><span style='display:block; text-align:left; color:#555'>• Large tumor mass</span><span style='display:block; text-align:left; color:#555'>• Brain compression</span>"]
MRI["<b>👁️ Annual MRI</b><br><span style='display:block; text-align:left; color:#555'>• Monitor growth</span><span style='display:block; text-align:left; color:#555'>• Repeat yearly</span>"]
Hearing["<b>📋 Hearing Status?</b><br><span style='display:block; text-align:left; color:#555'>• Audiogram check</span><span style='display:block; text-align:left; color:#555'>• Speech discrim</span>"]
Approach["<b>💊 Approach Selection</b><br><span style='display:block; text-align:left; color:#555'>• Translabyrinthine</span><span style='display:block; text-align:left; color:#555'>• Retrosigmoid</span>"]
Preserve["<b>✅ Hearing Preservation</b><br><span style='display:block; text-align:left; color:#555'>• Conserve function</span><span style='display:block; text-align:left; color:#555'>• Subtotal goal</span>"]
Removal["<b>✅ Total Removal</b><br><span style='display:block; text-align:left; color:#555'>• Complete excision</span><span style='display:block; text-align:left; color:#555'>• Cure-focused</span>"]
Start --> Size
Size -->|'<' 1.5cm| Obs
Size -->|1.5-2.5cm| SrsSurg
Size -->|'>' 2.5cm| Resection
Obs --> MRI
SrsSurg --> Hearing
Resection --> Approach
Hearing -->|Good| Preserve
Hearing -->|Poor| Removal
style Start fill:#F7F5FD, stroke:#F0EDFA, stroke-width:1.5px, rx:12, ry:12, color:#6B21A8
style Size fill:#FEF8EC, stroke:#FBECCA, stroke-width:1.5px, rx:12, ry:12, color:#854D0E
style Obs fill:#F1FCF5, stroke:#BEF4D8, stroke-width:1.5px, rx:12, ry:12, color:#166534
style SrsSurg fill:#F1FCF5, stroke:#BEF4D8, stroke-width:1.5px, rx:12, ry:12, color:#166534
style Resection fill:#F1FCF5, stroke:#BEF4D8, stroke-width:1.5px, rx:12, ry:12, color:#166534
style MRI fill:#EEFAFF, stroke:#DAF3FF, stroke-width:1.5px, rx:12, ry:12, color:#0369A1
style Hearing fill:#FEF8EC, stroke:#FBECCA, stroke-width:1.5px, rx:12, ry:12, color:#854D0E
style Approach fill:#F1FCF5, stroke:#BEF4D8, stroke-width:1.5px, rx:12, ry:12, color:#166534
style Preserve fill:#F6F5F5, stroke:#E7E6E6, stroke-width:1.5px, rx:12, ry:12, color:#525252
style Removal fill:#F6F5F5, stroke:#E7E6E6, stroke-width:1.5px, rx:12, ry:12, color:#525252
### Rehabilitative Strategies: The Recovery Framework
Vestibular rehabilitation accelerates compensation through targeted exercises:
* **Vestibular Rehabilitation Therapy (VRT)**
- **Gaze stabilization**: **×1** and **×2** exercises
- **Habituation training**: **graded exposure** to provocative movements
- **Balance training**: **static** and **dynamic** postural challenges
- **Substitution strategies**: **visual** and **somatosensory** enhancement
+ **Success rates**: **85%** improvement in **dizziness handicap**
+ **Duration**: **6-8 weeks** of **supervised therapy**
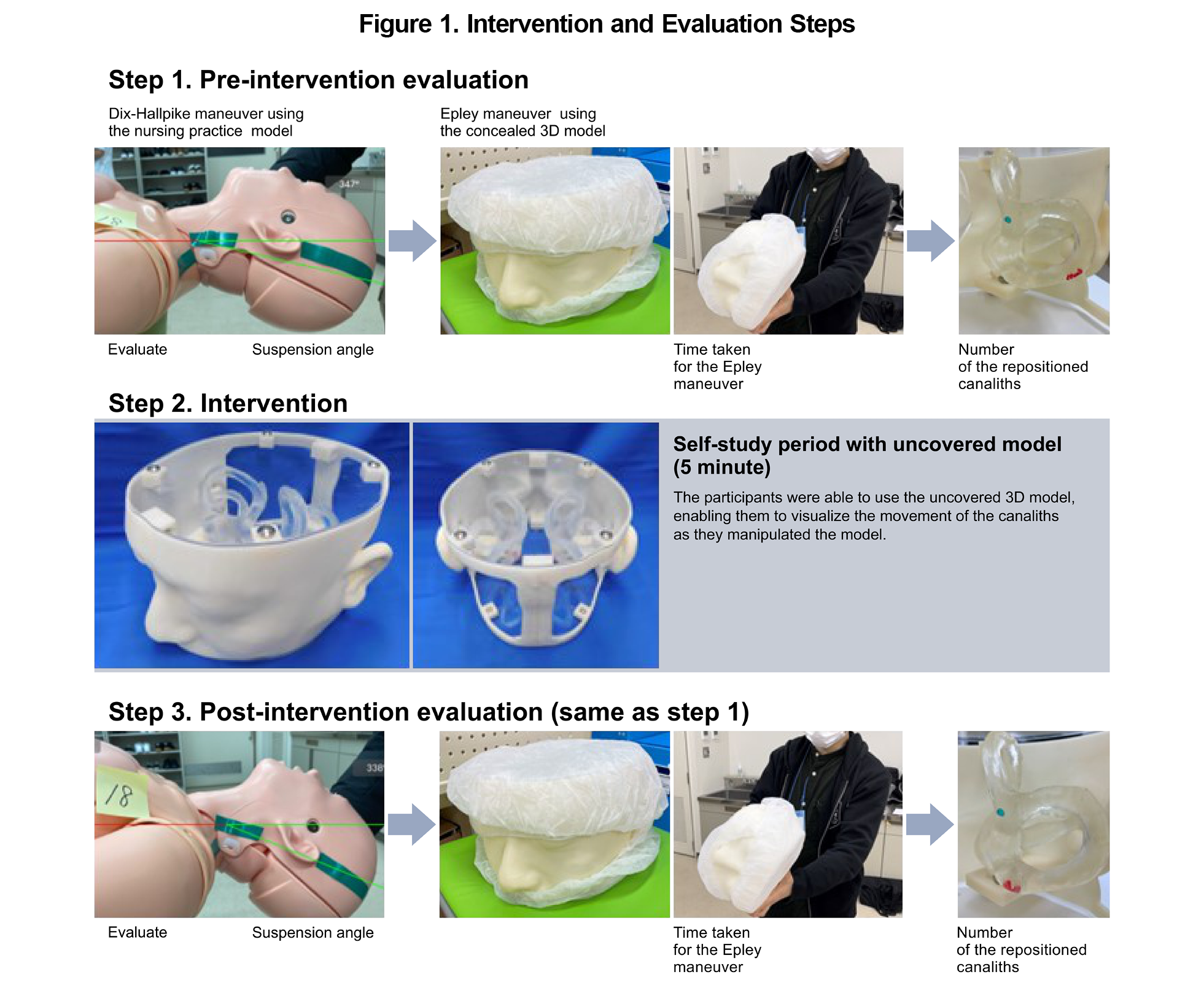
* **Canalith Repositioning Procedures**
- **Epley maneuver**: **posterior canal** BPPV (**80%** single-treatment success)
- **Semont maneuver**: **alternative** for **posterior canal** (**75%** success)
- **Barbecue roll**: **horizontal canal** BPPV (**90%** success)
- **Yacovino maneuver**: **anterior canal** BPPV (**70%** success)
> ⭐ **Clinical Pearl**: **Post-maneuver restrictions** (sleep upright, avoid head movements) show **no benefit** in randomized trials - patients can resume **normal activities immediately** after **successful repositioning**.
> 💡 **Master This**: **Gamma knife radiosurgery** for acoustic neuromas uses **12-13 Gy** marginal dose with **>95%** tumor control at **10 years** - **hearing preservation** rates of **70%** for tumors **<2cm** with **good preoperative hearing**.
These treatment algorithms provide systematic approaches that optimize outcomes while minimizing complications in neurotologic disorders.
---
⚕️ Treatment Algorithms: The Therapeutic Precision
🧩 System Integration: The Multisensory Network

The Vestibular-Ocular Integration Matrix
The vestibular-ocular reflex (VOR) represents one of the most precise motor systems in the human body:
-
VOR Pathway Architecture
- Semicircular canals detect angular acceleration (0.1°/sec² threshold)
- Vestibular nuclei process bilateral input with 3ms latency
- Oculomotor nuclei generate compensatory eye movements
- VOR gain: 0.8-1.0 (eye velocity/head velocity ratio)
- High-frequency response: >2Hz maintained by direct pathways
- Low-frequency response: <0.1Hz requires velocity storage
-
Central Compensation Mechanisms
- Vestibular nuclei plasticity: synaptic weight adjustments
- Cerebellar modulation: flocculus fine-tunes VOR gain
- Visual-vestibular interaction: optokinetic system supplements VOR
- Commissural inhibition: bilateral balance maintenance
- Compensation timeline: 50% recovery in 3 days, 80% in 6 weeks
- Age effects: >65 years show 30% slower compensation
📌 Remember: CANVAS syndrome (Cerebellar Ataxia, Neuropathy, Vestibular Areflexia) - bilateral vestibular loss with normal hearing, sensory neuropathy, and cerebellar signs due to RFC1 gene mutations.
Auditory-Cognitive Integration Networks
Auditory processing extends far beyond simple sound detection, involving complex cognitive networks:
| Processing Level | Location | Function | Integration Time | Clinical Correlation |
|---|---|---|---|---|
| Peripheral | Cochlea | Frequency analysis | <1ms | Hearing thresholds |
| Brainstem | Superior olive | Binaural processing | 3-5ms | Sound localization |
| Midbrain | Inferior colliculus | Feature extraction | 10-15ms | Auditory reflexes |
| Thalamic | Medial geniculate | Relay processing | 15-20ms | Attention gating |
| Cortical | Auditory cortex | Pattern recognition | 50-100ms | Speech understanding |
- Sound localization: 3-5° accuracy in horizontal plane
- Noise suppression: 3-6dB improvement in signal-to-noise ratio
- Summation effects: 3dB threshold improvement with bilateral input
- Squelch effect: 2-3dB additional benefit in competing noise
Vestibular-Autonomic Connections
The vestibular system maintains extensive connections with autonomic centers:
-
Vestibular-Autonomic Pathways
- Parabrachial nucleus: cardiovascular responses to motion
- Hypothalamus: stress hormone release during vestibular dysfunction
- Dorsal motor nucleus: vagal responses causing nausea/vomiting
- Locus coeruleus: arousal and anxiety responses
- Motion sickness: vestibular-visual mismatch triggers autonomic storm
- Chronic dizziness: >6 months leads to anxiety disorders in 45%
-
Postural Control Integration
- Vestibular input: 15% of postural control (increases with visual/proprioceptive loss)
- Visual input: 10% in normal lighting, 40% in challenging conditions
- Proprioceptive input: 70% from ankle/hip mechanoreceptors
- Central integration: cerebellum and brainstem weighting of inputs
⭐ Clinical Pearl: Persistent postural-perceptual dizziness (PPPD) affects 25% of patients after acute vestibular disorders - characterized by >3 months of dizziness, unsteadiness, and visual motion sensitivity without active vestibular pathology.
Neuroplasticity and Adaptation
The neurotologic system demonstrates remarkable adaptive capacity:
-
Vestibular Compensation Mechanisms
- Static compensation: resting discharge rebalancing (hours to days)
- Dynamic compensation: response symmetry restoration (weeks to months)
- Substitution strategies: visual and somatosensory enhancement
- Behavioral adaptation: movement strategies to minimize symptoms
- Factors enhancing compensation: early mobilization, vestibular exercises
- Factors impairing compensation: sedatives, immobility, bilateral loss
-
Auditory Plasticity Phenomena
- Cochlear implant adaptation: speech recognition improves for >2 years
- Hearing aid acclimatization: 6-12 weeks for optimal benefit
- Tinnitus habituation: 18-24 months for significant improvement
- Cross-modal plasticity: visual cortex activation in congenital deafness
💡 Master This: Vestibular migraine affects 1% of the population and 10% of migraine patients - diagnosis requires episodic vestibular symptoms, migraine history, and temporal association between headache and vestibular symptoms in >50% of episodes.
These integration networks explain how focal neurotologic pathology creates complex, multisystem symptom patterns that require comprehensive management approaches.
🧩 System Integration: The Multisensory Network
🎯 Clinical Mastery: The Expert's Arsenal
The Rapid Assessment Protocol
Expert neurotologic evaluation follows systematic protocols that maximize diagnostic yield:
-
The 5-Minute Neurotologic Screen
- History: SOCRATES for vertigo + hearing assessment (2 minutes)
- Examination: HINTS + Dix-Hallpike + Weber/Rinne (2 minutes)
- Risk stratification: stroke risk vs peripheral vs central (1 minute)
- High-yield questions: sudden onset, neurological symptoms, bilateral involvement
- Critical examination: head impulse, nystagmus pattern, hearing asymmetry
-
Emergency Red Flags
- Acute hearing loss + vertigo = labyrinthitis vs stroke
- Vertical nystagmus = central pathology until proven otherwise
- Bilateral vestibular loss = ototoxicity vs autoimmune vs genetic
- Facial weakness + hearing loss = CPA tumor vs Ramsay Hunt
📌 Remember: AEIOU for neurotologic emergencies - Acute hearing loss, Episodic vertigo with neurological signs, Intractable vomiting, Oscillopsia, Unilateral facial weakness with hearing loss.
Diagnostic Probability Matrix
Expert clinicians use Bayesian reasoning to refine diagnostic probabilities:
| Presentation | Most Likely (>50%) | Possible (10-50%) | Rare (<10%) | Key Discriminators |
|---|---|---|---|---|
| Acute vertigo + hearing loss | Viral labyrinthitis | Ménière's, stroke | Autoimmune, tumor | Age, bilaterality |
| Positional vertigo | BPPV | Vestibular migraine | Central positional | Nystagmus pattern |
| Progressive hearing loss | Presbycusis | Acoustic neuroma | Autoimmune | Asymmetry, age |
| Episodic vertigo | Vestibular migraine | Ménière's, BPPV | TIA, seizure | Duration, triggers |
| Facial weakness + hearing | Bell's palsy | Ramsay Hunt, tumor | Stroke, Lyme | Onset, vesicles |
Treatment Decision Algorithms
Expert management follows evidence-based algorithms that optimize outcomes:
- Acoustic Neuroma Management Algorithm
- <1cm + good hearing: observation with annual MRI
- 1-2.5cm + good hearing: stereotactic radiosurgery vs observation
- >2.5cm or symptoms: microsurgical resection
- Poor hearing: surgery for complete removal
- Hearing preservation: 70% with <1.5cm tumors
- Facial nerve preservation: >95% in experienced hands
The Expert's Mental Models
Master clinicians use sophisticated mental frameworks:
-
The Anatomical Localization Model
- Conductive loss = middle ear pathology
- Symmetric SNHL = cochlear pathology
- Asymmetric SNHL = retrocochlear pathology
- Central vertigo = brainstem/cerebellar pathology
- Pattern recognition: immediate anatomical localization
- Differential refinement: systematic exclusion of alternatives
-
The Temporal Pattern Model
- Seconds: BPPV, orthostatic
- Minutes to hours: Ménière's, migraine
- Hours to days: vestibular neuritis, labyrinthitis
- Constant: acoustic neuroma, central lesions
💡 Master This: The "Rule of 2000s" for acoustic neuromas - 2000 new cases/year in US, 2cm average size at diagnosis, 2mm/year average growth, $200,000 average treatment cost, 20% require intervention within 5 years.
Quality Metrics and Outcomes
Expert practice focuses on measurable outcomes:
-
Diagnostic Accuracy Benchmarks
- Vertigo diagnosis: >90% accuracy with systematic approach
- Hearing loss etiology: >85% correct classification
- Surgical candidacy: >95% appropriate selection
- Treatment response: >80% predicted outcomes
-
Patient-Reported Outcome Measures
- Dizziness Handicap Inventory: >18 point improvement = clinically significant
- Tinnitus Handicap Inventory: >20 point improvement = meaningful change
- Hearing Handicap Inventory: >18 point improvement = significant benefit
These mastery frameworks transform complex neurotologic presentations into systematic, evidence-based clinical decisions that optimize patient outcomes while minimizing unnecessary interventions.
🎯 Clinical Mastery: The Expert's Arsenal
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app
























