Xerostomia - Parched Prelude
- Subjective sensation of dry mouth due to ↓ saliva.
- Etiology:
- Medications (Most Common in Elderly): Anticholinergics, antihistamines, diuretics, antihypertensives, antidepressants.
⭐ Medications (anticholinergics, antihistamines, diuretics) are the most common cause of xerostomia in older adults.
- Sjögren's syndrome (autoimmune destruction of salivary/lacrimal glands).
- Radiation therapy (head & neck cancer).
- Systemic diseases: Diabetes mellitus, HIV/AIDS, dehydration, anxiety/depression.
- Salivary gland aplasia/agenesis (rare).
- Medications (Most Common in Elderly): Anticholinergics, antihistamines, diuretics, antihypertensives, antidepressants.
- Consequences: ↑ Dental caries, oral candidiasis, dysphagia, dysgeusia, difficulty with speech/dentures.
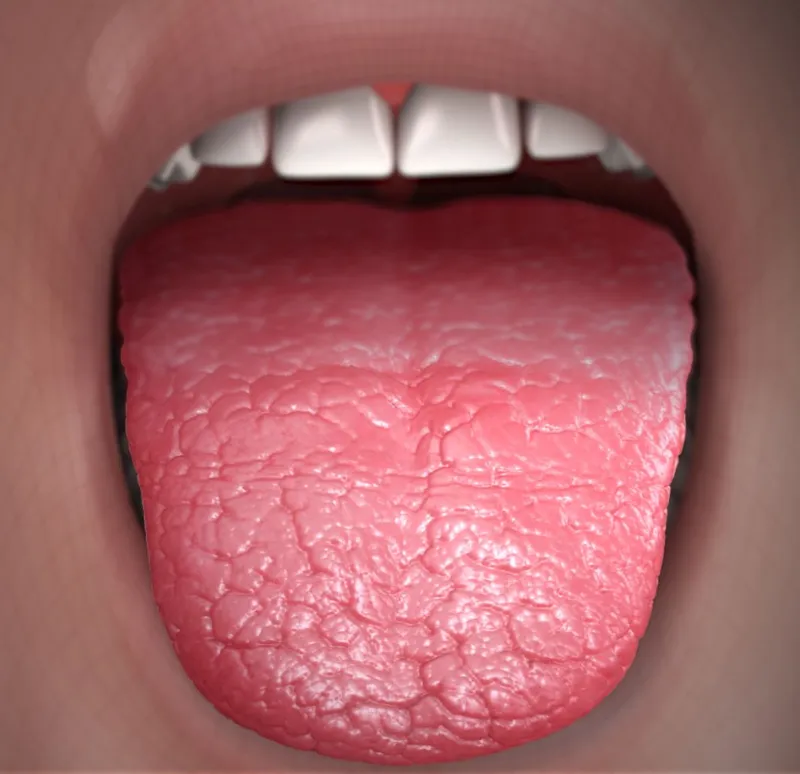
Xerostomia - Dry Detectives
-
Definition: Subjective sensation of dry mouth.
-
Etiology: Medications (anticholinergics, diuretics), Sjögren's syndrome, radiation therapy (head & neck), dehydration, systemic diseases (diabetes, HIV).
-
Clinical Features:
- Difficulty swallowing (dysphagia), speaking (dysphonia), & chewing.
- Oral soreness, burning sensation.
- Altered taste (dysgeusia).
- Increased dental caries (especially cervical & root caries).
- Oral mucosal dryness, atrophy, fissuring.
- Lobulated/fissured tongue, depapillation.
- Thick, ropy, or scanty saliva.
- Halitosis.
-
Diagnosis:
- Detailed history (medications, systemic conditions).
- Clinical examination: Mirror adherence to buccal mucosa, frothy saliva.
- Sialometry: Measurement of salivary flow rates.
⭐ Unstimulated whole salivary flow rate < 0.1 mL/min is a key diagnostic criterion for hyposalivation.
- Stimulated whole salivary flow rate < 0.5-0.7 mL/min.
- Salivary gland biopsy (minor glands, labial): Focal lymphocytic sialadenitis in Sjögren's.
- Serology: Anti-SSA/Ro, Anti-SSB/La antibodies for Sjögren's.
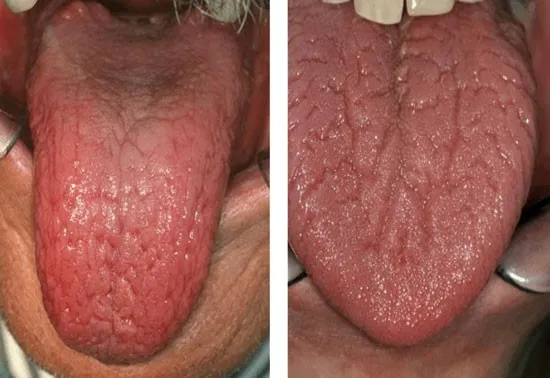
Xerostomia - Arid Aftermath
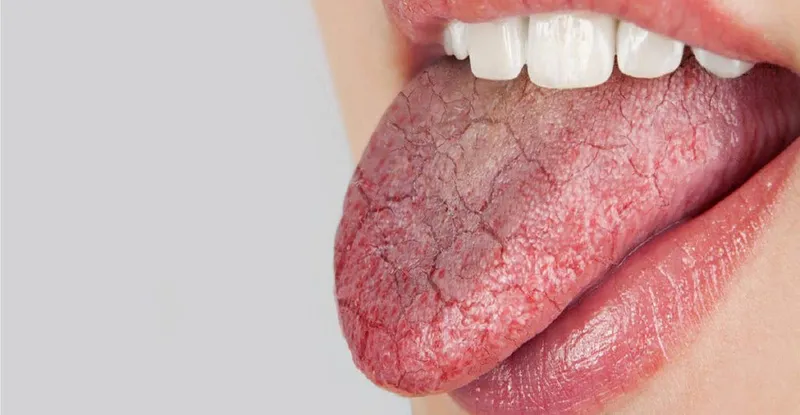
- Definition: Subjective sensation of dry mouth due to ↓ saliva.
- Etiology:
- Medications (anticholinergics, diuretics, antihistamines, antidepressants).
- Sjögren's syndrome.
- Radiation therapy (head & neck).
- Systemic diseases (diabetes, HIV/AIDS).
- Dehydration, anxiety.
- Clinical Features:
- Difficulty swallowing (dysphagia), speaking (dysphonia), & tasting (dysgeusia).
- Oral burning, soreness.
- Dry, fissured tongue; atrophic oral mucosa.
- Dental caries, oral candidiasis.
- Management:
- Symptomatic: Saliva substitutes, sialogogues (pilocarpine, cevimeline).
- Address underlying cause.
- Oral hygiene, frequent sips of water.
⭐ Xerostomia significantly increases the risk of oral candidiasis and rapidly progressive dental caries, particularly root caries.
Xerostomia - Moisture Makeover
Management aims to relieve symptoms, prevent complications, and stimulate saliva if possible.
- Symptomatic Relief:
- Saliva substitutes (e.g., carboxymethylcellulose, mucin-based products).
- Oral lubricants, mouth-wetting agents. Frequent sips of water.
- Salivary Stimulation (if glands functional):
- Gustatory/Masticatory: Sugar-free candies/gum (xylitol beneficial).
- Pharmacological (Sialogogues):
- Pilocarpine (cholinergic agonist).
- Cevimeline (selective M3 muscarinic receptor agonist).
- Preventive Care:
- Meticulous oral hygiene, topical fluoride application, regular dental visits.
- Etiology-Specific:
- Address underlying systemic diseases (e.g., Sjögren's syndrome).
- Review and modify potentially xerostomic medications.
⭐ Pilocarpine (5mg TID) is a commonly prescribed cholinergic agonist for stimulating salivary flow in patients with residual salivary gland function.
High‑Yield Points - ⚡ Biggest Takeaways
- Xerostomia: subjective sensation of oral dryness; a symptom, not a disease.
- Key causes: medications (anticholinergics, diuretics), Sjögren's syndrome, head/neck radiation.
- Clinical impact: ↑ risk of dental caries, oral candidiasis, dysphagia, dysgeusia.
- Diagnosis: Primarily clinical; sialometry (unstimulated flow < 0.1 mL/min) confirms.
- Management: Treat cause, symptomatic relief (saliva substitutes), sialagogues (e.g., pilocarpine).
- Pilocarpine (cholinergic agonist) stimulates saliva; meticulous oral hygiene is crucial.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

