Diseases of the Oral Cavity and Salivary Glands

On this page
🦠 Sialadenitis: The Glandular Battlefield
Salivary glands quietly orchestrate digestion, immunity, and oral health until infection or obstruction transforms them into inflamed battlegrounds. You'll learn how sialadenitis emerges from bacterial invasion or ductal blockage, master the clinical patterns that distinguish acute from chronic presentations, and deploy diagnostic tools from imaging to microbiology. Understanding the inflammatory cascade, recognizing systemic connections like Sjögren syndrome, and selecting targeted therapies will equip you to restore glandular function and prevent complications that threaten both local tissue and patient well-being.
📌 Remember: SPAM for Sialadenitis causes - Stones (sialolithiasis 40%), Parotitis (viral 35%), Autoimmune (Sjögren's 15%), Medications (anticholinergics 10%)
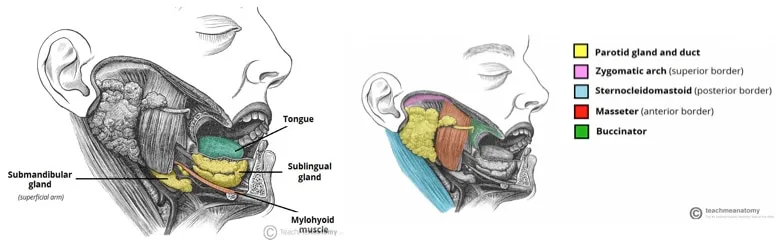
The pathophysiology centers on ductal obstruction or direct glandular infection. Bacterial sialadenitis occurs when salivary flow decreases below 0.1 mL/min (normal: 0.3-0.4 mL/min), creating stagnant conditions favoring Staphylococcus aureus (50% of cases) and Streptococcus viridans (30%). Viral sialadenitis, predominantly mumps, affects bilateral parotids in 70% of cases with 2-3 day prodromal period.
| Parameter | Acute Bacterial | Viral (Mumps) | Chronic Sclerosing | Autoimmune | Recurrent Juvenile |
|---|---|---|---|---|---|
| Age Peak | 50-60 years | 5-15 years | 40-50 years | 45-55 years | 3-6 years |
| Gland Affected | Parotid 60% | Bilateral parotid 70% | Submandibular 80% | Bilateral parotid 90% | Parotid 85% |
| Pain Severity | Severe (8-10/10) | Moderate (4-6/10) | Mild-moderate (3-5/10) | Mild (2-4/10) | Moderate (5-7/10) |
| Swelling Duration | 3-7 days | 7-10 days | Persistent months | Progressive years | Episodic 2-5 days |
| Fever Pattern | High (101-104°F) | Moderate (99-101°F) | Absent | Low-grade | Variable |
| Ductal Discharge | Purulent thick | Clear/cloudy | Scanty thick | Scanty clear | Variable |
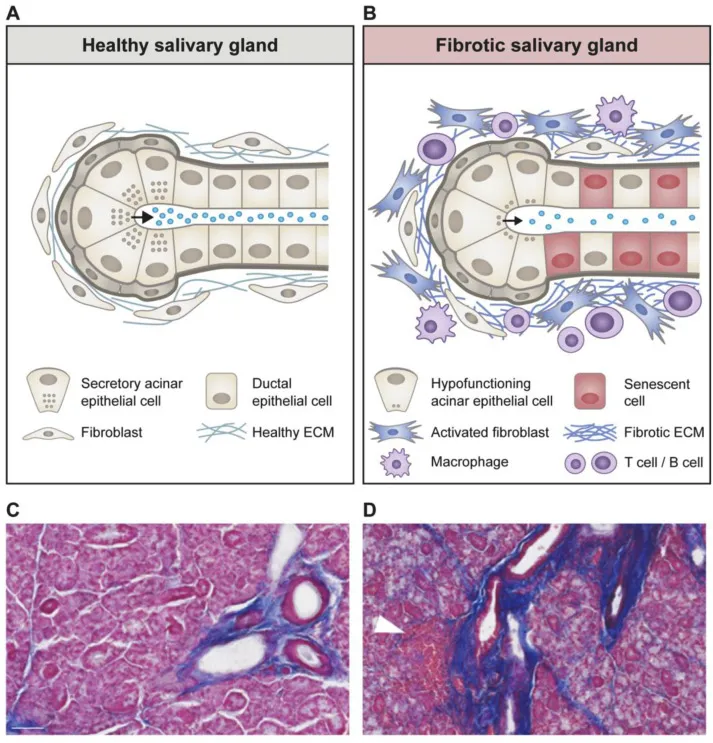
Chronic sialadenitis develops through recurrent inflammatory cycles causing progressive fibrosis and acinar atrophy. Sjögren's syndrome represents the most significant autoimmune variant, affecting 0.5-1% of the population with female predominance of 9:1. The focus score (lymphocytic infiltrates per 4mm² of glandular tissue) exceeds 1 in 95% of confirmed cases.
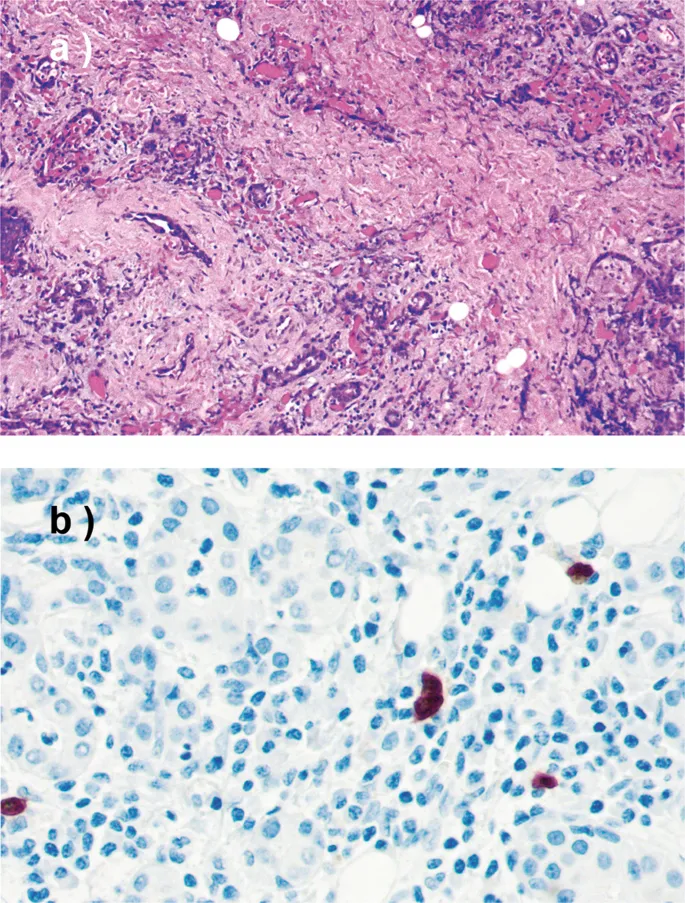
💡 Master This: Meal-related pain occurs in 90% of obstructive sialadenitis cases due to increased secretory pressure against blocked ducts. This gustatory stimulation test - offering lemon juice and observing pain response - provides 85% sensitivity for ductal pathology.
Risk stratification identifies high-risk populations: elderly patients (>65 years) with 40% higher bacterial infection rates, immunocompromised individuals with 3-fold increased severity, and medication-induced xerostomia patients showing 60% greater recurrence rates. Dehydration reduces salivary flow by 50-70%, while poor oral hygiene increases bacterial load 10-fold.
⭐ Clinical Pearl: Bilateral parotid swelling in children suggests viral etiology (85% mumps), while unilateral involvement in adults indicates bacterial infection (70% probability). Trismus (jaw limitation) occurs in 60% of severe parotitis cases due to masseter muscle inflammation.
Connect these inflammatory patterns through ductal anatomy to understand obstruction mechanisms and predict treatment responses.
🦠 Sialadenitis: The Glandular Battlefield
⚙️ Sialadenitis: The Inflammatory Cascade Engine
📌 Remember: FIRE describes acute inflammation phases - Fluid extravasation (2-4 hours), Immune cell infiltration (6-12 hours), Repair initiation (24-48 hours), Either resolution or Established chronicity (72+ hours)
Bacterial pathogenesis follows retrograde ductal invasion when salivary flow drops below critical threshold of 0.1 mL/min. Staphylococcus aureus demonstrates high ductal affinity through fibronectin-binding proteins, while Streptococcus pneumoniae utilizes pneumolysin for epithelial invasion. Biofilm formation occurs within 24-48 hours, creating antibiotic resistance in 60-80% of chronic cases.
| Inflammatory Phase | Timeline | Key Mediators | Clinical Manifestation | Reversibility | Treatment Window |
|---|---|---|---|---|---|
| Initiation | 0-2 hours | IL-1β, TNF-α | Pain onset, mild swelling | 95% reversible | Optimal intervention |
| Amplification | 2-12 hours | IL-6, CXCL8 | Marked swelling, fever | 80% reversible | Good response |
| Peak Response | 12-48 hours | IFN-γ, IL-17 | Maximum symptoms | 60% reversible | Moderate response |
| Resolution | 48-96 hours | IL-10, TGF-β | Symptom decline | 90% reversible | Recovery phase |
| Chronic Phase | >7 days | PDGF, collagen | Fibrosis, dysfunction | 20% reversible | Limited options |
⭐ Clinical Pearl: Gustatory stimulation during acute inflammation increases intraductal pressure from normal 5-10 mmHg to 40-60 mmHg, explaining meal-related pain exacerbation. This pressure-pain correlation provides 90% diagnostic accuracy for obstructive etiology.
Autoimmune mechanisms in Sjögren's syndrome involve molecular mimicry between viral proteins and salivary antigens. Ro52/SSA and La/SSB antibodies appear months to years before clinical symptoms, with anti-centromere antibodies predicting limited cutaneous systemic sclerosis overlap in 25% of cases.
💡 Master This: Complement activation through classical pathway occurs in 70% of bacterial sialadenitis cases, while alternative pathway dominates autoimmune variants. C3 consumption correlates with disease severity and treatment response - levels below 50 mg/dL predict complicated course in 85% of cases.
Chronic inflammation perpetuation involves failed resolution mechanisms when specialized pro-resolving mediators (resolvins, protectins) become deficient. Lipoxin A4 levels decrease 60-80% in chronic sialadenitis, while resolvin D1 shows 70% reduction, explaining persistent inflammatory state despite pathogen clearance.
Connect these inflammatory mechanisms through treatment algorithms to understand why early intervention within 24-48 hours achieves 90% resolution rates compared to 40% success in established chronic disease.
⚙️ Sialadenitis: The Inflammatory Cascade Engine
🎯 Sialadenitis: The Clinical Recognition Matrix
Pattern Recognition Framework begins with "See-Think-Act" correlations that guide immediate clinical decisions. Unilateral parotid swelling + purulent ductal discharge + fever >101°F = bacterial sialadenitis (90% probability). Bilateral parotid involvement + prodromal symptoms + age 5-15 years = viral mumps (85% likelihood). Recurrent episodes + dry mouth + dry eyes = Sjögren's syndrome (80% correlation).
📌 Remember: SWOLLEN assessment protocol - Size progression (acute vs chronic), Warmth presence (bacterial indicator), Ostium examination (ductal discharge), Location pattern (unilateral vs bilateral), Lymphatic involvement (regional nodes), Eye dryness (autoimmune marker), Neurological signs (facial nerve proximity)
Pain Pattern Analysis provides diagnostic specificity through temporal characteristics and trigger identification. Meal-related pain occurs in 95% of obstructive cases due to increased secretory pressure against blocked ducts. Constant throbbing pain suggests bacterial infection with tissue tension from inflammatory edema. Intermittent discomfort indicates chronic inflammation with episodic exacerbations.
| Clinical Feature | Acute Bacterial | Viral Mumps | Chronic Sclerosing | Sjögren's Syndrome | Juvenile Recurrent |
|---|---|---|---|---|---|
| Onset Speed | Hours (2-6) | Days (2-3) | Weeks-months | Years | Hours-days |
| Pain Quality | Severe throbbing | Moderate aching | Mild pressure | Minimal discomfort | Moderate cramping |
| Swelling Consistency | Firm, tender | Soft, elastic | Hard, non-tender | Variable firmness | Soft, fluctuant |
| Skin Changes | Erythema, warmth | Minimal changes | Normal appearance | Dry, atrophic | Transient erythema |
| Ductal Discharge | Thick purulent | Clear/absent | Scanty mucoid | Minimal clear | Variable |
| Systemic Features | High fever, malaise | Moderate fever | None | Dry eyes, arthritis | Low-grade fever |
⭐ Clinical Pearl: Facial nerve function assessment is mandatory in parotid inflammation due to anatomical proximity. House-Brackmann grading documents baseline function - Grade I (normal) in 98% of uncomplicated cases, Grade II-III (mild-moderate dysfunction) suggests deep lobe involvement or malignancy requiring urgent imaging.
Ductal Assessment Techniques provide immediate diagnostic information through ostium examination and secretion analysis. Stensen's duct opens opposite upper 2nd molar with punctate opening in normal states. Purulent discharge indicates bacterial infection (sensitivity 85%, specificity 92%), while blood-tinged secretions suggest malignancy (positive predictive value 60%).
- Normal Ductal Flow Assessment:
- Unstimulated flow: 0.3-0.4 mL/min per gland
- Stimulated flow: 1.0-1.5 mL/min with citric acid
- pH range: 6.2-7.4 (alkaline shift with inflammation)
- Bacterial infection: pH drops to 5.5-6.0
- Autoimmune disease: pH remains 6.8-7.2
- Obstruction: pH varies with stasis duration
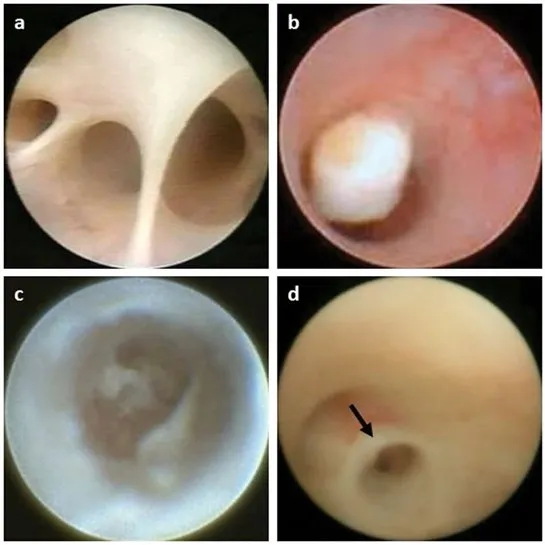
💡 Master This: Gustatory stimulation test using lemon juice or citric acid differentiates obstructive from non-obstructive causes. Pain increase >50% within 30 seconds indicates ductal obstruction (sensitivity 90%, specificity 85%). Absent pain response suggests glandular parenchymal disease or neural dysfunction.
Lymphatic Examination reveals regional involvement patterns that guide antibiotic selection and predict complications. Preauricular lymphadenopathy accompanies parotitis in 70% of bacterial cases but only 30% of viral infections. Submandibular lymph nodes enlarge in 80% of submandibular sialadenitis with size correlation to infection severity.
Red Flag Recognition identifies complications requiring immediate intervention. Facial nerve weakness suggests deep parotid involvement or malignancy. Trismus (mouth opening <35mm) indicates masticator space involvement. Neck swelling below hyoid bone suggests Ludwig's angina development requiring emergency airway management.
⭐ Clinical Pearl: Bilateral parotid enlargement in adults raises systemic disease suspicion - Sjögren's syndrome (40%), sarcoidosis (15%), diabetes mellitus (10%), alcoholism (8%), bulimia (5%). Unilateral adult presentation suggests bacterial infection (60%) or neoplasm (25%).
Connect these recognition patterns through diagnostic algorithms to understand when clinical diagnosis suffices versus imaging requirements for treatment planning.
🎯 Sialadenitis: The Clinical Recognition Matrix
🔬 Sialadenitis: The Diagnostic Precision Laboratory
Diagnostic Algorithm Hierarchy follows evidence-based decision trees that optimize resource utilization while maximizing diagnostic yield. Clinical assessment provides initial probability estimates - high pretest probability (>80%) for typical presentations requires minimal testing, while intermediate probability (40-80%) demands targeted investigations, and low probability (<40%) necessitates comprehensive workup to exclude mimics.
Laboratory Investigation Strategy targets specific diagnostic questions rather than routine screening. Complete blood count reveals leukocytosis (>12,000/μL) in 85% of bacterial cases with left shift (bands >10%). C-reactive protein exceeds 50 mg/L in 90% of acute bacterial infections but remains <10 mg/L in viral sialadenitis.
📌 Remember: LABS for sialadenitis workup - Leukocyte count (bacterial vs viral), Autoantibodies (Sjögren's screening), Blood cultures (severe infections), Salivary flow studies (functional assessment)
Autoimmune Marker Panel becomes essential when bilateral involvement, dry symptoms, or recurrent episodes suggest Sjögren's syndrome. Anti-Ro/SSA antibodies appear in 60-70% of cases, Anti-La/SSB in 40-50%, while rheumatoid factor shows positivity in 70-80%. Antinuclear antibodies demonstrate homogeneous or speckled patterns in 95% of seropositive patients.
| Diagnostic Test | Bacterial Sialadenitis | Viral Sialadenitis | Sjögren's Syndrome | Sialolithiasis | Malignancy |
|---|---|---|---|---|---|
| WBC Count | >12,000/μL (85%) | Normal-mild ↑ | Normal (90%) | Normal-mild ↑ | Variable |
| CRP Level | >50 mg/L (90%) | <10 mg/L (80%) | <20 mg/L (70%) | 20-40 mg/L | Variable |
| ESR | >40 mm/hr (75%) | <20 mm/hr (85%) | >30 mm/hr (60%) | <30 mm/hr | Often elevated |
| Anti-Ro/SSA | Negative (98%) | Negative (99%) | Positive (65%) | Negative (99%) | Negative (95%) |
| Salivary Flow | Reduced 50-70% | Reduced 30-50% | Severely reduced >80% | Variable | Variable |
Ultrasound Interpretation Framework identifies key sonographic patterns that correlate with pathology. Acute bacterial sialadenitis shows hypoechoic enlargement with increased vascularity on Doppler studies. Chronic inflammation demonstrates heterogeneous echogenicity with ductal dilatation >2mm diameter. Autoimmune involvement reveals multiple hypoechoic areas creating "honeycomb appearance".
- Advanced Imaging Indications:
- CT with contrast: Suspected abscess formation or deep space involvement
- MR sialography: Ductal anatomy assessment without contrast injection
- Conventional sialography: Gold standard for ductal pathology (when not acutely inflamed)
- Strictures: Focal narrowing with proximal dilatation
- Sialectasis: Globular or punctate ductal dilatation patterns
- Mass effect: Ductal displacement or obstruction
⭐ Clinical Pearl: MR sialography provides non-invasive ductal imaging without contrast injection, ideal for acute inflammation when conventional sialography is contraindicated. 3D-CISS sequences achieve 0.5mm resolution for detailed ductal anatomy assessment.
Microbiological Studies guide targeted antimicrobial therapy in severe or recurrent cases. Ductal secretion culture yields positive results in 70-80% of bacterial infections when properly collected. Anaerobic cultures identify Peptostreptococcus and Bacteroides species in 20-30% of chronic cases.
Functional Assessment through salivary flow studies quantifies glandular function and monitors treatment response. Unstimulated whole saliva collection over 15 minutes normally yields >1.5 mL total volume. Stimulated flow using 2% citric acid should produce >10 mL in 10 minutes. Flow rates below 50% of normal values indicate significant dysfunction.
💡 Master This: Schirmer's test for tear production complements salivary assessment in suspected Sjögren's syndrome. <5mm wetting in 5 minutes suggests keratoconjunctivitis sicca (sensitivity 85%, specificity 92%). Combined positive salivary and lacrimal tests increase diagnostic probability to >95%.
Biopsy Considerations become necessary when malignancy suspicion arises or autoimmune diagnosis requires histological confirmation. Minor salivary gland biopsy from lower lip provides safer alternative to major gland sampling with equivalent diagnostic yield for Sjögren's syndrome. Focus score ≥1 (lymphocytic foci per 4mm²) confirms diagnosis in appropriate clinical context.
⭐ Clinical Pearl: Bilateral parotid enlargement with negative autoantibodies requires tissue diagnosis to exclude lymphoma - MALT lymphoma develops in 5-10% of Sjögren's patients with 40-fold increased risk compared to general population.
Connect these diagnostic frameworks through treatment algorithms to understand how test results guide therapeutic decisions and monitoring strategies.
🔬 Sialadenitis: The Diagnostic Precision Laboratory
⚡ Sialadenitis: The Therapeutic Command Center
Treatment Algorithm Architecture follows severity-based stratification that optimizes outcomes while minimizing complications. Mild cases (pain <5/10, minimal swelling, no systemic symptoms) respond to conservative management in 85-90% of cases. Moderate severity (pain 5-7/10, visible swelling, low-grade fever) requires targeted antimicrobial therapy with 90-95% success rates. Severe presentations (pain >7/10, marked swelling, high fever, complications) demand aggressive intervention including possible hospitalization.
Antimicrobial Selection Strategy targets predominant pathogens while considering resistance patterns and tissue penetration characteristics. First-line therapy for outpatient bacterial sialadenitis includes amoxicillin-clavulanate 875/125mg twice daily achieving excellent ductal penetration with 90% efficacy against Staphylococcus aureus and Streptococcus species.
📌 Remember: DRUGS for sialadenitis antibiotics - Dicloxacillin (staph coverage), Roxithromycin (atypical organisms), Unafyn (amoxicillin-clavulanate first-line), Gentamicin (severe gram-negative), Sulbactam-ampicillin (broad spectrum)
Conservative Management Protocol forms the foundation for mild cases and adjunctive therapy for all severities. Hydration with 2-3 liters daily increases salivary flow by 40-60%, while warm compresses 15 minutes four times daily improve local circulation and reduce inflammation. Glandular massage from posterior to anterior promotes ductal drainage and prevents stasis.
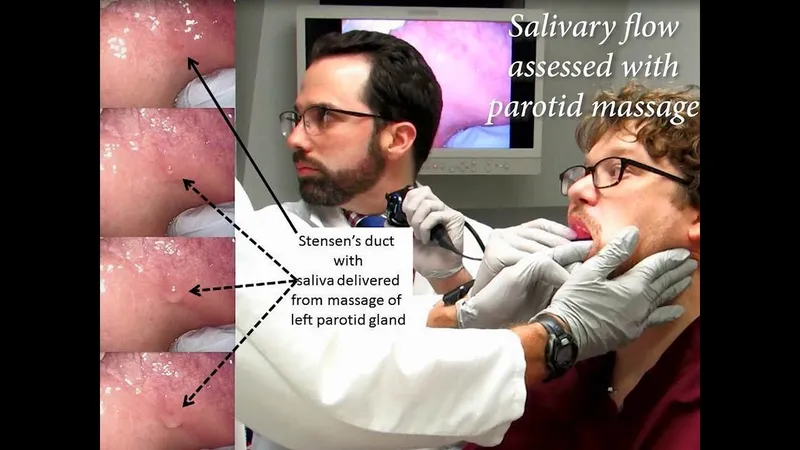
| Treatment Modality | Mechanism | Dosing/Frequency | Success Rate | Onset of Action | Duration |
|---|---|---|---|---|---|
| Amoxicillin-Clavulanate | β-lactamase inhibition | 875/125mg BID × 7-10 days | 90% mild-moderate | 24-48 hours | Complete course |
| Clindamycin | Protein synthesis inhibition | 300mg QID × 7-10 days | 85% (PCN allergy) | 24-48 hours | Complete course |
| Cephalexin | Cell wall synthesis inhibition | 500mg QID × 7-10 days | 80% (mild cases) | 48-72 hours | Complete course |
| Warm Compresses | Vasodilation, drainage | 15 min QID | 70% adjunctive | Immediate | Ongoing |
| Sialagogues | Stimulate salivary flow | Lemon drops PRN | 60% supportive | Minutes | As needed |
⭐ Clinical Pearl: Ductal irrigation with normal saline through lacrimal probes can dislodge mucus plugs and improve drainage in obstructive cases. Success rate reaches 70-80% when performed within 48 hours of symptom onset, but contraindicated during acute inflammation due to tissue trauma risk.
Chronic Sialadenitis Management focuses on symptom control and function preservation rather than cure. Pilocarpine 5mg three times daily stimulates residual glandular function in Sjögren's syndrome with 40-50% response rates. Cevimeline 30mg three times daily provides alternative cholinergic stimulation with fewer side effects but similar efficacy.
Surgical Intervention Criteria include recurrent episodes (>4 per year), chronic pain affecting quality of life, ductal strictures amenable to repair, or suspected malignancy. Sialendoscopy allows minimally invasive ductal exploration and intervention with 80-90% success for stone removal and stricture dilation.
- Surgical Options by Indication:
- Sialendoscopy: Ductal stones <4mm, strictures, mucus plugs
- Lithotripsy: Stones 4-7mm in main ducts
- Ductal repair: Traumatic injuries, iatrogenic damage
- End-to-end anastomosis: <2cm defects
- Ductal reimplantation: Longer defects
- Gland preservation: Priority in young patients
💡 Master This: Gland preservation should be prioritized in patients <50 years due to long-term functional implications. Total parotidectomy carries 15-20% permanent facial nerve injury risk, while submandibular gland excision has 5-10% lingual nerve damage probability.
Autoimmune Disease Management requires multidisciplinary approach combining symptomatic relief with systemic immunomodulation. Hydroxychloroquine 400mg daily provides mild immunosuppression with 60% symptom improvement in Sjögren's syndrome. Methotrexate 15-20mg weekly reserved for severe systemic involvement with regular monitoring.
Complication Prevention through early recognition and appropriate escalation prevents life-threatening sequelae. Abscess formation occurs in 10-15% of untreated bacterial cases, requiring surgical drainage and prolonged antibiotics. Facial nerve monitoring essential in parotid procedures with intraoperative nerve stimulation reducing injury rates to <5%.
⭐ Clinical Pearl: Recurrent juvenile parotitis often resolves spontaneously by puberty in 80-90% of cases. Conservative management with symptomatic treatment and infection prevention preferred over aggressive intervention that may damage developing glands.
Connect these therapeutic strategies through outcome monitoring to understand treatment response patterns and long-term prognosis factors.
⚡ Sialadenitis: The Therapeutic Command Center
🔗 Sialadenitis: The Systemic Integration Network
Systemic Disease Interconnections reveal how sialadenitis serves as a clinical window into broader pathological processes. Sjögren's syndrome affects 0.5-1% of the population with 9:1 female predominance, but secondary Sjögren's develops in 15-20% of rheumatoid arthritis patients and 10-15% of systemic lupus erythematosus cases. Diabetes mellitus increases sialadenitis risk 3-fold through reduced salivary flow and impaired immune function.
Medication-Induced Xerostomia contributes to 40-50% of chronic sialadenitis cases in elderly populations. Anticholinergic medications reduce salivary flow by 60-80%, while diuretics cause dehydration-related flow reduction of 30-50%. Antidepressants, particularly tricyclics and SSRIs, affect 70% of users with dose-dependent xerostomia severity.
📌 Remember: MEDS causing xerostomia - Muscarinic antagonists (anticholinergics 80% incidence), Emotional medications (antidepressants 70%), Diuretics (fluid loss 50%), Sedatives (antihistamines 60%)
Autoimmune Disease Spectrum demonstrates overlapping presentations requiring careful differentiation. Primary Sjögren's syndrome presents with isolated glandular dysfunction, while secondary forms accompany connective tissue diseases in 60% of cases. Sarcoidosis causes bilateral parotid enlargement in 10-15% of patients, often mimicking Sjögren's but with different histological patterns.
| Systemic Condition | Sialadenitis Pattern | Associated Features | Diagnostic Markers | Treatment Implications |
|---|---|---|---|---|
| Sjögren's Primary | Bilateral chronic | Dry eyes, arthritis | Anti-Ro/La, RF | Immunosuppression |
| Sjögren's Secondary | Variable presentation | Underlying CTD | Disease-specific Ab | Treat primary disease |
| Sarcoidosis | Bilateral parotid | Lung involvement | ACE, Ca²⁺ elevated | Corticosteroids |
| Diabetes Mellitus | Recurrent bacterial | Poor glycemic control | HbA1c >7% | Glucose optimization |
| HIV/AIDS | Chronic lymphocytic | CD4 <200 | Viral load, CD4 count | HAART therapy |
Nutritional Deficiency Impacts on salivary function often overlooked in clinical assessment. Vitamin A deficiency reduces mucin production by 40-60%, while iron deficiency affects salivary enzyme function. Protein-energy malnutrition decreases total salivary output by 50-70% with delayed recovery even after nutritional rehabilitation.
- Age-Related Physiological Changes:
- Salivary flow reduction: 25% decrease per decade after age 60
- Medication burden: Average 5-7 medications in elderly
- Immune senescence: Reduced infection resistance
- T-cell dysfunction: Delayed pathogen clearance
- Antibody production: Decreased specific responses
- Inflammatory resolution: Prolonged recovery phases
⭐ Clinical Pearl: Bilateral parotid enlargement in alcoholic patients results from fatty infiltration and chronic inflammation, affecting 60-70% of chronic alcoholics. Abstinence leads to partial resolution in 40-50% of cases within 6-12 months.
Genetic Predisposition Factors influence disease susceptibility and treatment responses. HLA-DR3 and HLA-DQ2 haplotypes increase Sjögren's syndrome risk 8-10 fold, while complement deficiencies predispose to recurrent bacterial infections. Familial clustering occurs in 15-20% of autoimmune sialadenitis cases.
Environmental Trigger Integration reveals modifiable risk factors for prevention strategies. Viral infections trigger autoimmune responses in genetically susceptible individuals - Epstein-Barr virus detected in salivary glands of 80% of Sjögren's patients. Stress-induced cortisol elevation reduces salivary IgA by 30-40%, increasing infection susceptibility.
Pregnancy Considerations affect both disease activity and treatment options. Sjögren's syndrome may improve during pregnancy due to immunological tolerance, but anti-Ro/SSA antibodies cross placental barrier causing neonatal lupus in 2-5% of exposed infants. Congenital heart block represents most serious complication with 15-20% mortality.
💡 Master This: Tumor surveillance becomes critical in long-standing Sjögren's syndrome due to 40-fold increased lymphoma risk. MALT lymphoma develops in 5-10% of patients, typically 10-15 years after initial diagnosis. Persistent unilateral enlargement or hard masses require immediate biopsy.
Quality of Life Integration addresses functional impairment beyond medical management. Severe xerostomia affects nutrition (difficulty swallowing), dental health (increased caries), speech (voice changes), and sleep (frequent awakening). Multidisciplinary care involving dentistry, nutrition, speech therapy, and psychology improves patient outcomes significantly.
⭐ Clinical Pearl: Dental prophylaxis becomes essential in chronic xerostomia patients due to 10-fold increased caries risk. Fluoride supplementation, antimicrobial rinses, and frequent dental visits prevent tooth loss that compounds functional impairment.
Connect these systemic relationships through comprehensive care models to understand long-term management strategies and outcome optimization.
🔗 Sialadenitis: The Systemic Integration Network
🎯 Sialadenitis: The Clinical Mastery Arsenal
Essential Clinical Thresholds for immediate decision-making include pain severity >7/10 indicating severe inflammation, fever >101°F suggesting bacterial infection, mouth opening <35mm warning of deep space involvement, and facial nerve weakness requiring urgent surgical consultation. Bilateral involvement in adults raises systemic disease probability to >80%.
📌 Remember: RAPID assessment priorities - Recognize severity (pain, fever, swelling), Assess airway (trismus, neck swelling), Palpate glands (consistency, discharge), Identify complications (nerve weakness, abscess), Determine disposition (outpatient vs admission)
Quick Reference Treatment Matrix guides immediate therapeutic decisions based on presentation patterns. Unilateral parotid + purulent discharge + fever = bacterial sialadenitis requiring amoxicillin-clavulanate 875/125mg twice daily. Bilateral parotid + dry eyes + arthritis = Sjögren's syndrome needing rheumatology referral and symptomatic management.
| Clinical Scenario | Immediate Action | Antibiotic Choice | Duration | Follow-up | Red Flags |
|---|---|---|---|---|---|
| Mild Unilateral | Conservative care | Consider if no improvement 48hr | N/A initially | 48-72 hours | Worsening pain/swelling |
| Moderate Bacterial | Amoxicillin-clavulanate | 875/125mg BID | 7-10 days | 3-5 days | Facial nerve symptoms |
| Severe/Toxic | Hospital admission | IV ampicillin-sulbactam | 7-14 days | Daily monitoring | Airway compromise |
| Recurrent Episodes | Specialist referral | Culture-guided | Variable | 2-4 weeks | Malignancy concern |
| Bilateral Chronic | Autoimmune workup | Avoid unless infected | N/A | 1-2 weeks | Lymphoma signs |
Complication Recognition Framework identifies warning signs requiring immediate escalation. Abscess formation presents with fluctuant masses, skin erythema, and systemic toxicity. Deep space infection causes trismus, neck swelling, and potential airway compromise. Facial nerve involvement suggests malignancy or severe inflammation requiring urgent evaluation.
- Emergency Consultation Criteria:
- Airway compromise: Stridor, voice changes, difficulty swallowing
- Facial nerve weakness: Any degree of facial asymmetry
- Sepsis signs: Hypotension, altered mental status, organ dysfunction
- Systolic BP <90 mmHg or MAP <65 mmHg
- Heart rate >100 bpm with temperature >100.4°F
- Respiratory rate >20 or PaCO2 <32 mmHg
⭐ Clinical Pearl: Parotid massage should be avoided during acute bacterial infection due to bacteremia risk - positive blood cultures occur in 15-20% of severe cases. Gentle massage appropriate only during recovery phase or chronic management.
Patient Education Essentials improve compliance and prevent recurrence. Hydration goals of 2-3 liters daily increase salivary flow by 40-60%. Oral hygiene with antimicrobial rinses reduces bacterial load by 80-90%. Smoking cessation improves salivary function and reduces infection risk by 50%.
Long-term Monitoring Strategy tracks treatment response and identifies complications. Symptom resolution should occur within 48-72 hours of appropriate antibiotic therapy. Persistent symptoms beyond 7 days require reassessment for resistant organisms, complications, or alternative diagnoses.
💡 Master This: Recurrent sialadenitis (>4 episodes annually) requires specialist evaluation for underlying causes - ductal abnormalities (30%), autoimmune disease (25%), systemic conditions (20%), medication effects (15%), idiopathic (10%).
Quality Metrics for clinical excellence include diagnostic accuracy >90%, appropriate antibiotic selection >95%, complication recognition within 24 hours, and patient satisfaction scores >85%. Unnecessary imaging should remain <20% of cases through effective clinical assessment.
Evidence-Based Outcomes demonstrate treatment effectiveness when protocols are properly implemented. Conservative management succeeds in 85-90% of mild cases. Appropriate antibiotics achieve cure rates >95% in bacterial infections. Early intervention prevents complications in >98% of cases.
⭐ Clinical Pearl: Antibiotic resistance patterns vary geographically - MRSA prevalence ranges from 10-40% in community-acquired sialadenitis. Local antibiograms guide empirical therapy, while culture results direct targeted treatment in severe or recurrent cases.
Professional Development Framework builds expertise through systematic case review, outcome tracking, and continuous education. Pattern recognition improves with experience - expert clinicians achieve >95% diagnostic accuracy compared to 70-80% for novice practitioners. Multidisciplinary collaboration enhances complex case management and patient outcomes.
🎯 Sialadenitis: The Clinical Mastery Arsenal
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app





















