Otosclerosis: Definition & Epi - Bone Gone Rogue
- Definition: Abnormal bone remodeling in otic capsule, leading to stapes fixation.
- Etiology:
- Genetic: Autosomal dominant (AD), variable penetrance.
- ?Measles virus.
- Epidemiology:
- Age: Peak 20-40 years.
- Sex: F > M (2:1); pregnancy can worsen.
- Race: Caucasians most affected.
- Prevalence: Clinical 0.3-0.4%; Histological ~10%.
- Bilateral ~80%.
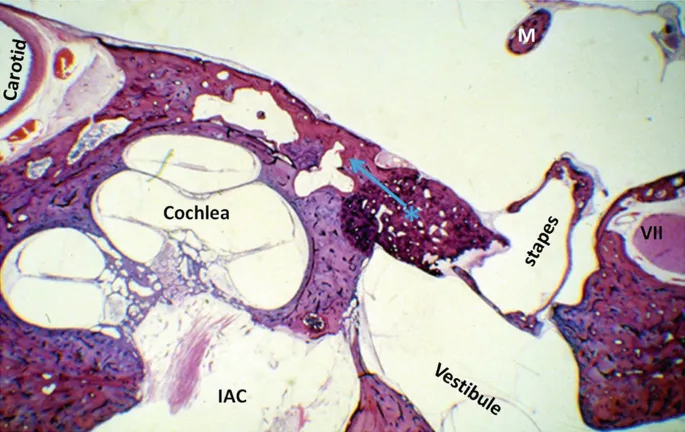
⭐ Most common cause of bilateral conductive hearing loss in young adults with a normal tympanic membrane.
Otosclerosis: Pathophysiology - The Bony Culprit
- Localized bony dystrophy of the otic capsule; often autosomal dominant inheritance with incomplete penetrance.
- Pathological process involves two phases:
- Otospongiosis phase: Active resorption by osteoclasts, vascular proliferation, immature woven bone formation (spongy, vascular bone).
- Otosclerotic phase: Deposition of dense, lamellar, sclerotic bone by osteoblasts, less vascular.
- Primary lesion typically at fissula ante fenestram (anterior to oval window).
- Mechanism: Imbalance in bone remodeling. Possible triggers include measles virus (leading to ↑ IL-6, ↑ TNF-α).
- Results in stapes footplate fixation → conductive hearing loss.

⭐ Schwartze's sign (flamingo pink hue on promontory due to increased vascularity) indicates active otospongiosis stage of the disease process and is a sign of good prognosis for stapedectomy surgery if hearing loss is significant enough to warrant it and the patient is a good candidate for surgery and desires it and understands the risks and benefits of the procedure and alternative treatments such as hearing aids or observation or no treatment at all if the hearing loss is mild and not bothersome to the patient or if the patient has other medical conditions that make surgery too risky or if the patient prefers not to have surgery for personal reasons or if the patient is not a good candidate for surgery for other reasons such as poor cochlear reserve or active infection or other contraindications to surgery or anesthesia or if the patient has unrealistic expectations about the outcome of surgery or if the patient is not able to comply with postoperative care instructions or if the patient has a history of previous unsuccessful ear surgery or if the patient has a history of keloid formation or other wound healing problems or if the patient has a history of autoimmune disease or other systemic conditions that may affect healing or increase the risk of complications or if the patient is pregnant or breastfeeding or if the patient is taking medications that may interfere with healing or increase the risk of bleeding or other complications or if the patient has a history of radiation therapy to the head and neck or if the patient has a history of trauma to the ear or temporal bone or if the patient has a history of Meniere's disease or other inner ear disorders that may be exacerbated by surgery or if the patient has a history of chronic ear infections or cholesteatoma or other middle ear pathology that may need to be addressed before or during surgery or if the patient has a history of Eustachian tube dysfunction or other conditions that may affect middle ear ventilation and pressure regulation or if the patient has a history of allergies or sensitivities to medications or materials that may be used during surgery or if the patient has a history of bleeding disorders or is taking anticoagulant or antiplatelet medications or if the patient has a history of immunosuppression or is taking immunosuppressive medications or if the patient has a history of diabetes or other metabolic disorders that may affect healing or increase the risk of infection or if the patient has a history of smoking or alcohol abuse or drug abuse or other lifestyle factors that may affect healing or increase the risk of complications or if the patient has a history of psychological or psychiatric conditions that may affect their ability to cope with surgery or postoperative care or if the patient has a history of unrealistic expectations or dissatisfaction with previous medical or surgical treatments or if the patient has a history of litigation or legal issues related to medical care or if the patient has a history of noncompliance with medical advice or treatment recommendations or if the patient has a history of poor social support or lack of access to transportation or other resources that may be needed for postoperative care or follow-up visits or if the patient has a history of financial constraints or lack of insurance coverage that may limit their access to surgery or postoperative care or if the patient has a history of cultural or religious beliefs or practices that may conflict with surgery or postoperative care or if the patient has a history of language barriers or communication difficulties that may affect their ability to understand information or provide informed consent or comply with instructions or if the patient has a history of cognitive impairment or dementia or other conditions that may affect their ability to understand information or provide informed consent or comply with instructions or if the patient has a history of physical limitations or disabilities that may affect their ability to undergo surgery or postoperative care or if the patient has a history of advanced age or frailty or other factors that may increase the risk of surgery or anesthesia or if the patient has a history of personal preference for nonsurgical treatment options or if the patient has a history of fear or anxiety about surgery or anesthesia or if the patient has a history of previous negative experiences with surgery or anesthesia or if the patient has a history of lack of trust or confidence in the surgeon or the medical team or if the patient has a history of seeking multiple opinions or changing doctors frequently or if the patient has a history of unrealistic demands or expectations or if the patient has a history of personality disorder or other mental health conditions that may affect their ability to form a therapeutic relationship with the surgeon or the medical team or if the patient has a history of substance abuse or addiction or if the patient has a history of chronic pain or other symptoms that may be unrelated to otosclerosis or if the patient has a history of malingering or factitious disorder or other conditions that may involve feigning or exaggerating symptoms for secondary gain or if the patient has a history of somatization disorder or other conditions that may involve experiencing physical symptoms without a clear medical explanation or if the patient has a history of conversion disorder or other conditions that may involve neurological symptoms without a clear medical explanation or if the patient has a history of hypochondriasis or other conditions that may involve excessive worry or fear about health or illness or if the patient has a history of body dysmorphic disorder or other conditions that may involve preoccupation with perceived flaws in appearance or if the patient has a history of obsessive-compulsive disorder or other conditions that may involve repetitive thoughts or behaviors or if the patient has a history of anxiety disorder or other conditions that may involve excessive worry or fear or if the patient has a history of depression or other mood disorders that may affect their motivation or ability to cope with surgery or postoperative care or if the patient has a history of bipolar disorder or other mood disorders that may involve fluctuations in mood or energy or if the patient has a history of schizophrenia or other psychotic disorders that may affect their perception of reality or ability to make decisions or if the patient has a history of intellectual disability or developmental delay or other conditions that may affect their ability to understand information or provide informed consent or comply with instructions or if the patient has a history of autism spectrum disorder or other conditions that may affect their communication or social interaction or sensory processing or if the patient has a history of attention-deficit/hyperactivity disorder or other conditions that may affect their attention or impulsivity or hyperactivity or if the patient has a history of learning disability or other conditions that may affect their ability to read or write or understand information or if the patient has a history of speech or language disorder or other conditions that may affect their ability to communicate or understand information or if the patient has a history of hearing loss or deafness or other conditions that may affect their ability to communicate or understand information or if the patient has a history of vision loss or blindness or other conditions that may affect their ability to read or see information or if the patient has a history of physical disability or mobility impairment or other conditions that may affect their ability to access care or comply with instructions or if the patient has a history of chronic illness or comorbidity or other conditions that may affect their overall health or prognosis or if the patient has a history of terminal illness or palliative care or other conditions that may affect their goals of care or treatment preferences or if the patient has a history of advance directives or living wills or other documents that may express their wishes regarding medical treatment or if the patient has a history of designated healthcare proxy or power of attorney or other individuals who may be authorized to make decisions on their behalf or if the patient has a history of family members or caregivers who may be involved in their care or decision-making or if the patient has a history of cultural or religious beliefs or practices that may influence their decisions or preferences regarding medical treatment or if the patient has a history of personal values or priorities or goals that may influence their decisions or preferences regarding medical treatment or if the patient has a history of previous experiences with the healthcare system or medical providers that may influence their trust or confidence or expectations or if the patient has a history of access to information or resources or support systems that may influence their ability to make informed decisions or cope with illness or treatment or if the patient has a history of socioeconomic status or education level or health literacy or other factors that may influence their understanding or access to care or outcomes or if the patient has a history of geographic location or distance to care or transportation issues or other factors that may influence their access to care or follow-up or if the patient has a history of insurance coverage or financial resources or other factors that may influence their access to care or treatment options or if the patient has a history of legal or ethical issues or concerns related to their care or treatment or if the patient has a history of research participation or clinical trial enrollment or other involvement in medical research or innovation or if the patient has a history of advocacy or activism or other involvement in health-related causes or organizations or if the patient has a history of personal or professional relationships with healthcare providers or researchers or other individuals involved in their care or treatment or if the patient has a history of media exposure or public attention related to their health or illness or treatment or if the patient has a history of social media use or online information seeking related to their health or illness or treatment or if the patient has a history of alternative or complementary medicine use or other non-conventional approaches to health or illness or treatment or if the patient has a history of self-management or self-care practices related to their health or illness or treatment or if the patient has a history of health behaviors or lifestyle choices or risk factors or protective factors that may influence their health or illness or treatment or if the patient has a history of genetic predisposition or family history or other hereditary factors that may influence their health or illness or treatment or if the patient has a history of environmental exposures or occupational hazards or other external factors that may influence their health or illness or treatment or if the patient has a history of developmental stage or life course or aging process or other temporal factors that may influence their health or illness or treatment or if the patient has a history of individual variability or heterogeneity or diversity or other factors that may influence their response to treatment or outcomes or if the patient has a history of patient-reported outcomes or experiences or preferences or values or goals or other subjective factors that may influence their care or treatment or if the patient has a history of shared decision-making or patient engagement or empowerment or activation or other collaborative approaches to care or treatment or if the patient has a history of patient safety or quality improvement or risk management or other system-level factors that may influence their care or treatment or if the patient has a history of health policy or regulation or legislation or other societal-level factors that may influence their care or treatment or if the patient has a history of global health or international collaboration or other transnational factors that may influence their care or treatment or if the patient has a history of emerging technologies or innovations or discoveries or other future-oriented factors that may influence their care or treatment. Schwartze's sign (flamingo pink hue on promontory due to increased vascularity) indicates active otospongiosis stage of the disease process.
Otosclerosis: Clinical Features - Hear Ye, Hear Less
- Onset: 20-30 years, F > M (2:1).
- Hearing Loss: Progressive, bilateral (80%), conductive (CHL). Sensorineural (SNHL) or mixed in late stages (cochlear otosclerosis).
- Tinnitus: Common, often precedes hearing loss.
- Vertigo: Uncommon, mild.
- Speech: Soft, monotonous (patient hears own voice loudly via bone conduction).
- Otoscopy: Normal tympanic membrane (TM). Schwartze's sign (flamingo pink hue on promontory) visible in 10% (active phase).
- 📌 Paracusis Willisii.
⭐ Paracusis Willisii: Patient hears better in noisy surroundings (due to Lombard effect).
Otosclerosis: Diagnosis - Test Toolkit
- Tuning Fork Tests:
- Rinne: Negative (BC > AC).
- Weber: Lateralizes to poorer ear (conductive component).
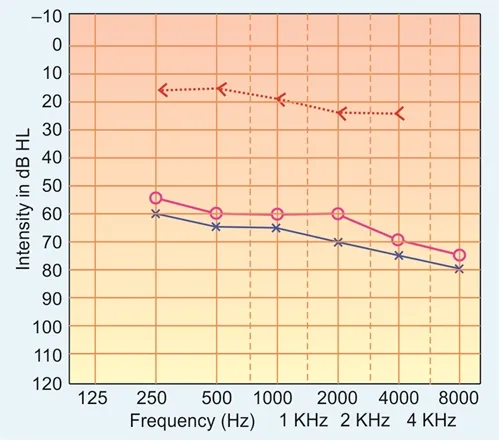
- Pure Tone Audiometry (PTA):
- Conductive hearing loss (CHL), initially low frequencies.
- May show mixed hearing loss in later stages.
-
⭐ Carhart's notch: A dip in bone conduction threshold, typically at 2000 Hz, seen in audiometry.
- Tympanometry:
- Type As (stiffness) curve: Reduced compliance.
- Stapedial Reflex:
- Absent or diphasic (On-Off phenomenon).
- HRCT Temporal Bone (not routine):
- Hypodense foci near fissula ante fenestram (fenestral otosclerosis).
- Assesses cochlear involvement (retrofenestral otosclerosis).
Otosclerosis: Management - Sounding Better
- Conservative/Medical Management:
- Observation: For mild, non-progressive hearing loss.
- Hearing Aids: Primary for patients unwilling/unfit for surgery.
- Sodium Fluoride: 0.5-1 mg/kg/day; aims to mature active foci, controversial efficacy.
- Surgical Management:
- Stapedotomy (preferred over Stapedectomy): Fenestration of stapes footplate, prosthesis insertion.
- Cochlear Implant: For advanced otosclerosis with severe SNHL.
⭐ Stapedotomy/Stapedectomy is the primary surgical treatment, often with excellent results for conductive hearing loss.
High-Yield Points - ⚡ Biggest Takeaways
- Autosomal dominant inheritance, incomplete penetrance; more common in females.
- Affects otic capsule, typically at fissula ante fenestram leading to stapes fixation.
- Painless, progressive, bilateral conductive hearing loss; tinnitus is frequent.
- Paracusis Willisii (hears better in noisy environments) is a classic symptom.
- Schwartze's sign (flamingo-pink hue on promontory) indicates active otospongiosis.
- Audiometry: Carhart's notch (bone conduction dip, usually at 2 kHz).
- Treatment: Stapedotomy with prosthesis; Sodium Fluoride for active otospongiotic disease.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

