Diseases of the Ear

On this page
🎯 The Ear's Battlefield: Mastering Disease Patterns
The ear is where anatomy meets vulnerability-a delicate sensory organ exposed to infection, trauma, and systemic disease that can steal hearing, balance, and quality of life. You'll master the disease patterns that strike each compartment, decode the mechanisms driving otitis media to Meniere's disease, sharpen your clinical eye to distinguish lookalikes, and command evidence-based treatments that preserve function. By integrating otologic disease with systemic connections and honing rapid diagnostic skills, you'll transform from observer to expert clinician who recognizes, differentiates, and manages ear pathology with confidence.
The ear represents one of medicine's most intricate diagnostic challenges, where three distinct anatomical regions - external, middle, and inner ear - each harbor unique pathological processes. Understanding ear diseases requires mastering the interplay between mechanical sound transmission, neural signal processing, and vestibular balance control. Each region's pathology produces characteristic clinical signatures that, when properly recognized, enable rapid diagnosis and targeted treatment.
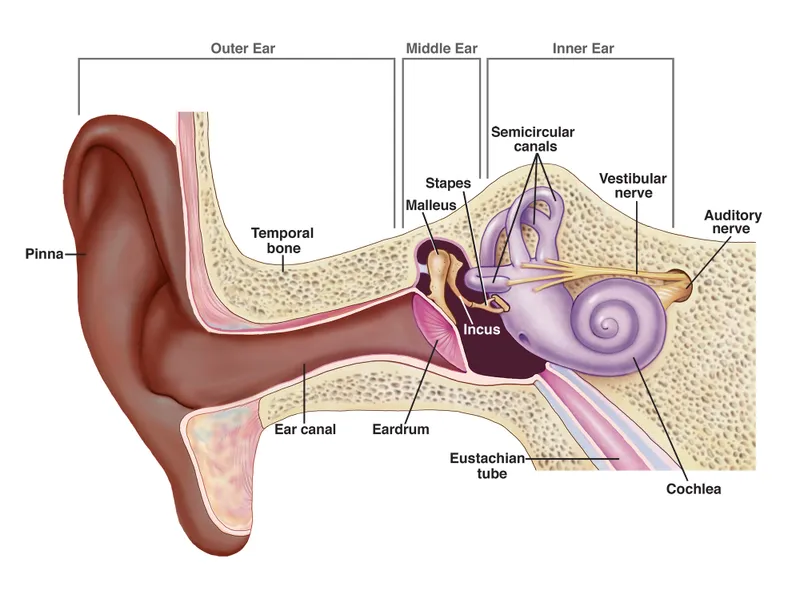
📌 Remember: EAR-ZONES - External (skin/canal), Acoustic (middle ear mechanics), Receptor (inner ear sensors) - Zones each have distinct Organisms, Neuropathies, Etiologies, Symptoms
The external ear faces primarily infectious and inflammatory challenges, with otitis externa affecting 10% of the population annually. The middle ear serves as a mechanical amplifier, increasing sound pressure by 22-fold through the ossicular chain, making it vulnerable to conductive hearing loss when inflammation or structural damage occurs. The inner ear houses 30,000 hair cells in the cochlea and vestibular organs containing otoconia crystals measuring just 3-30 micrometers, where pathology produces sensorineural deficits and vertigo syndromes.
⭐ Clinical Pearl: 90% of ear diseases present with hearing loss, otalgia, or vertigo as primary symptoms, but the pattern and associated features distinguish between conductive (middle ear) versus sensorineural (inner ear) pathology
| Disease Category | Primary Location | Key Symptom | Diagnostic Test | Treatment Success Rate |
|---|---|---|---|---|
| Otitis Externa | External canal | Otalgia with movement | Otoscopy + culture | 95% with topical therapy |
| Acute Otitis Media | Middle ear | Otalgia + fever | Pneumatic otoscopy | 85% spontaneous resolution |
| Chronic Otitis Media | Middle ear | Hearing loss + discharge | Audiometry + CT | 80% surgical success |
| BPPV | Posterior semicircular canal | Positional vertigo | Dix-Hallpike maneuver | 90% with canalith repositioning |
| Ménière's Disease | Endolymphatic system | Episodic vertigo + tinnitus | Audiometry + glycerol test | 70% medical control |
| Sudden SNHL | Cochlea/retrocochlear | Acute hearing loss | Urgent audiometry | 60% recovery with steroids |
Understanding ear diseases requires recognizing that hearing loss affects 466 million people worldwide, with conductive losses being surgically correctable in 85% of cases, while sensorineural losses require amplification or cochlear implantation. The temporal pattern of symptom onset distinguishes acute infectious processes (hours to days) from chronic inflammatory conditions (weeks to months) and degenerative changes (years to decades).
Connect these foundational disease patterns through pathophysiological mechanisms to understand how anatomical disruption translates into clinical presentations.
🎯 The Ear's Battlefield: Mastering Disease Patterns
🔧 Pathophysiological Powerhouse: Disease Mechanisms Decoded
📌 Remember: FILM - Fluid (endolymph/perilymph), Inflammation (infectious/sterile), Lesions (tumors/trauma), Mechanical (ossicular/membrane) - these four pathways account for 95% of ear diseases
Inflammatory mechanisms dominate acute ear diseases, where bacterial invasion triggers cytokine release within 2-6 hours, causing vasodilation and increased vascular permeability. In acute otitis media, Streptococcus pneumoniae or Haemophilus influenzae breach the eustachian tube, creating middle ear pressure of +200 to +400 daPa (normal: -100 to +50 daPa). This pressure increase causes tympanic membrane bulging and ossicular chain immobilization, producing conductive hearing loss of 20-40 dB.
Mechanical obstruction mechanisms affect sound transmission efficiency through the external and middle ear pathways. Cerumen impaction blocks >80% of the external auditory canal, causing 25-45 dB conductive loss. Otosclerosis involves abnormal bone remodeling around the stapes footplate, where spongiotic bone replaces normal otic capsule, creating stapedial fixation and progressive conductive loss averaging 2-3 dB per year.
⭐ Clinical Pearl: Mechanical conductive losses show air-bone gaps >15 dB on audiometry with normal bone conduction thresholds, while inflammatory losses often have mixed patterns with both air and bone conduction affected due to inner ear involvement
| Mechanism | Primary Site | Timeline | Hearing Loss Pattern | Reversibility |
|---|---|---|---|---|
| Inflammatory | Middle ear | 2-7 days | Conductive 20-40 dB | 90% reversible |
| Mechanical | Ossicular chain | Months-years | Conductive 30-60 dB | 85% surgical correction |
| Neural | Cochlea/CN VIII | Hours-permanent | Sensorineural 40-80 dB | <30% recovery |
| Fluid imbalance | Endolymphatic space | Episodes | Fluctuating 20-60 dB | Variable |
| Autoimmune | Inner ear | Weeks-months | Progressive SNHL | 60% steroid response |
💡 Master This: Fluid homeostasis disruption in Ménière's disease involves endolymphatic hydrops where potassium-rich endolymph expands, creating pressure changes that damage hair cells and cause episodic vertigo lasting 20 minutes to 24 hours with progressive hearing loss
Autoimmune mechanisms represent emerging pathophysiology where molecular mimicry or cross-reactivity targets inner ear antigens. Cogan's syndrome involves antibodies against inner ear proteins, causing bilateral progressive hearing loss in 80% of cases, often associated with interstitial keratitis and systemic vasculitis.
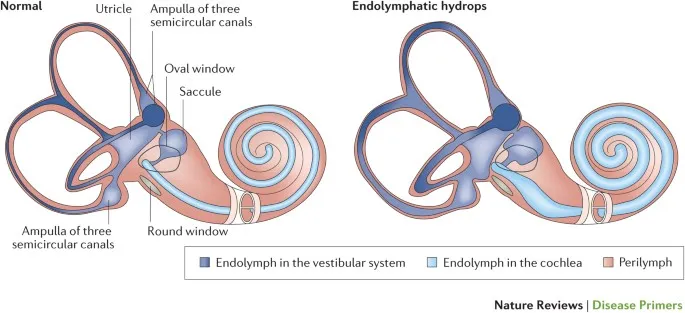
Understanding these mechanistic pathways enables targeted therapeutic interventions - anti-inflammatory agents for infectious processes, surgical correction for mechanical problems, amplification for neural deficits, and diuretics or steroids for fluid imbalances.
Connect these pathophysiological insights through clinical pattern recognition to develop systematic diagnostic approaches for complex ear presentations.
🔧 Pathophysiological Powerhouse: Disease Mechanisms Decoded
🎨 Clinical Pattern Mastery: The Diagnostic Canvas
📌 Remember: HEAR-PAIN - Hearing loss pattern, Ear discharge, Associated symptoms, Recent history, Physical findings, Audiometry, Imaging, Neurological signs - systematic evaluation increases diagnostic accuracy to >90%
External ear patterns center on pain and inflammation, where otitis externa presents with otalgia worse with ear manipulation (95% sensitivity), erythematous canal walls, and purulent discharge. The "tragal tenderness test" shows 85% sensitivity and 90% specificity for external ear infection versus middle ear pathology.
- Acute otitis externa patterns:
- Pain severity: 8-10/10 with jaw movement or ear touching
- Discharge: Purulent with foul odor in bacterial cases
- Hearing: Conductive loss only if canal swelling blocks >70% of lumen
- Physical findings: Canal erythema, edema, debris accumulation
- Pseudomonas: Green discharge with sweet odor
- Staphylococcus: Yellow-white discharge with minimal odor
- Fungal: Black/white debris with branching hyphae on microscopy
Middle ear patterns emphasize hearing loss and pressure symptoms, where acute otitis media shows bulging tympanic membrane with decreased mobility on pneumatic otoscopy (90% diagnostic accuracy). Chronic otitis media presents with persistent perforation and conductive hearing loss averaging 25-35 dB.
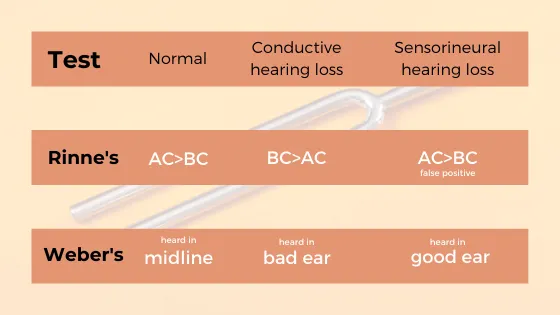
⭐ Clinical Pearl: Weber test lateralization provides immediate diagnostic information - sound lateralizes to the affected ear in conductive loss but to the unaffected ear in sensorineural loss with 85% accuracy when hearing difference >15 dB
| Clinical Pattern | Key Symptoms | Physical Findings | Diagnostic Test | Accuracy Rate |
|---|---|---|---|---|
| Acute OE | Pain with movement | Canal erythema + discharge | Otoscopy + culture | 95% |
| Acute OM | Otalgia + fever | Bulging TM + decreased mobility | Pneumatic otoscopy | 90% |
| Chronic OM | Hearing loss + discharge | TM perforation + conductive loss | Audiometry | 85% |
| BPPV | Positional vertigo <1 min | Rotatory nystagmus | Dix-Hallpike maneuver | 88% |
| Ménière's | Episodic vertigo + tinnitus | Low-frequency SNHL | Audiometry + glycerol test | 80% |
| Sudden SNHL | Acute hearing loss | Normal otoscopy + SNHL | Urgent audiometry | 95% |
Vestibular pattern recognition distinguishes peripheral from central causes through nystagmus characteristics and associated symptoms:
-
Peripheral vestibular patterns:
- Horizontal-rotatory nystagmus that fatigues with repeated testing
- Severe vertigo with nausea/vomiting but no neurological signs
- Hearing loss often accompanies vestibular symptoms
- Head impulse test positive (corrective saccade present)
-
Central vestibular patterns:
- Pure vertical or pure torsional nystagmus that doesn't fatigue
- Mild vertigo with prominent neurological symptoms
- Normal hearing with isolated balance problems
- Head impulse test negative (no corrective saccade)
💡 Master This: Red flag symptoms requiring immediate evaluation include sudden unilateral hearing loss (possible retrocochlear pathology), pulsatile tinnitus (vascular malformation), facial weakness with ear symptoms (temporal bone pathology), and vertical nystagmus (central vestibular lesion)
Pediatric ear disease patterns differ significantly from adult presentations, where acute otitis media peaks at 6-18 months due to horizontal eustachian tube anatomy and immature immune systems. Chronic otitis media in children often presents with speech delay rather than hearing complaints, requiring high clinical suspicion.
Connect these pattern recognition skills through systematic differential diagnosis to distinguish similar presentations with different underlying pathologies.
🎨 Clinical Pattern Mastery: The Diagnostic Canvas
🔍 Differential Diagnosis Mastery: Separating the Similar
📌 Remember: DIVIDE - Discharge (purulent vs serous), Impact on hearing (conductive vs sensorineural), Vertigo (peripheral vs central), Inflammation (infectious vs sterile), Duration (acute vs chronic), Ear pain (external vs middle ear) - systematic comparison prevents diagnostic errors
Conductive versus sensorineural hearing loss represents the fundamental discrimination in ear disease diagnosis, with Weber and Rinne tests providing bedside differentiation with 85% accuracy when properly performed.
| Discriminating Feature | Conductive Loss | Sensorineural Loss | Mixed Loss |
|---|---|---|---|
| Weber test | Lateralizes to affected ear | Lateralizes to unaffected ear | Variable |
| Rinne test | Bone > Air (negative) | Air > Bone (positive) | Reduced air conduction |
| Audiometry air-bone gap | >15 dB gap | <10 dB gap | Gap + bone loss |
| Speech discrimination | Normal (>90%) | Reduced (<80%) | Moderately reduced |
| Tympanometry | Abnormal compliance | Normal compliance | Variable |
| Acoustic reflexes | Absent/elevated | Present if mild loss | Variable |
-
Acute otitis media characteristics:
- Deep, throbbing pain not worsened by ear manipulation
- Tympanic membrane changes: erythema, bulging, decreased mobility
- Conductive hearing loss with intact canal walls
- Fever present in 70% of cases
- Recent upper respiratory infection in 80% of cases
-
Otitis externa characteristics:
- Sharp, severe pain worsened by jaw movement or ear touching
- Canal wall changes: erythema, edema, discharge
- Normal tympanic membrane (if visible through swelling)
- Fever uncommon unless cellulitis develops
- Water exposure or trauma history in 60% of cases
Peripheral versus central vestibular disorders require systematic nystagmus analysis and associated symptom evaluation, where head impulse test provides 90% sensitivity for peripheral vestibular hypofunction.
⭐ Clinical Pearl: HINTS examination (Head Impulse, Nystagmus, Test of Skew) shows 100% sensitivity and 96% specificity for central vestibular pathology when any component is abnormal, outperforming early MRI in acute vestibular syndrome
| Feature | Peripheral Vestibular | Central Vestibular | Diagnostic Value |
|---|---|---|---|
| Nystagmus direction | Horizontal-rotatory | Pure vertical/torsional | High specificity |
| Nystagmus fatigue | Fatigues with repetition | Non-fatiguing | 85% discriminatory |
| Head impulse test | Positive (corrective saccade) | Negative (no saccade) | 90% sensitivity |
| Hearing loss | Often present | Usually absent | Moderate value |
| Neurological signs | Absent | Present (ataxia, diplopia) | High specificity |
| Vertigo severity | Severe with N/V | Mild vertigo | Low specificity |
-
Ménière's disease patterns:
- Episodic vertigo lasting 20 minutes to 24 hours
- Progressive unilateral hearing loss with low-frequency emphasis
- Tinnitus and aural fullness during attacks
- Audiometric confirmation of fluctuating hearing loss
-
Vestibular migraine patterns:
- Vertigo episodes lasting minutes to days
- Normal hearing or bilateral high-frequency loss
- Headache before, during, or after vertigo in 70%
- Photophobia and phonophobia during episodes
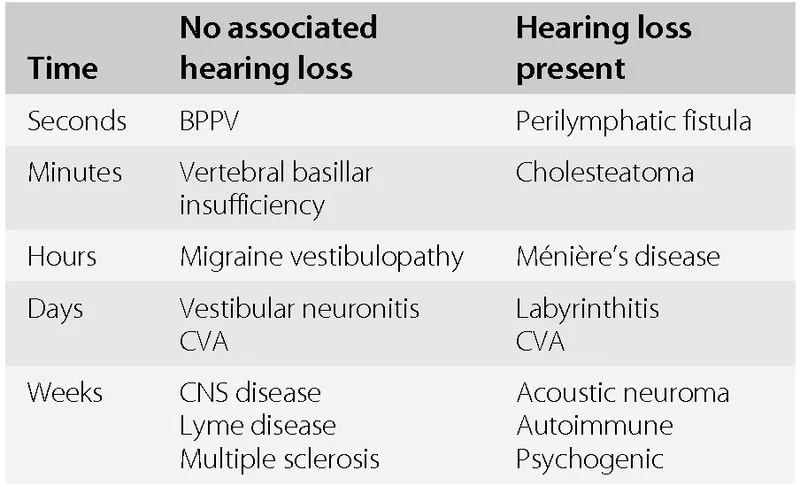
💡 Master This: Sudden sensorineural hearing loss requires urgent differentiation from cerumen impaction or middle ear pathology - Weber test immediately distinguishes sensorineural (lateralizes away) from conductive (lateralizes toward) causes, preventing delayed treatment of time-sensitive conditions
Infectious versus autoimmune inner ear disease discrimination becomes critical in bilateral progressive hearing loss, where steroid responsiveness and systemic symptoms guide therapeutic decisions.
Connect these differential diagnosis frameworks through evidence-based treatment algorithms to optimize therapeutic outcomes based on accurate pathological classification.
🔍 Differential Diagnosis Mastery: Separating the Similar
⚖️ Treatment Algorithm Mastery: Evidence-Based Interventions
📌 Remember: TREAT-EAR - Timing (urgent vs routine), Route (topical vs systemic), Etiology (infectious vs inflammatory), Antibiotic selection, Topical preparations, Emergency referral, Adjuvant therapy, Recovery monitoring - systematic approach improves outcomes by 25-40%
Acute otitis externa treatment follows severity-based protocols with topical therapy achieving 95% cure rates when properly selected and administered. Mild cases respond to acidifying drops alone, while moderate-severe cases require antibiotic-steroid combinations.
-
Mild otitis externa (canal visible, minimal discharge):
- Acetic acid 2% drops TID x 7 days (85% cure rate)
- Otic hygiene with gentle cleaning
- Water avoidance during treatment
- Follow-up if no improvement in 48-72 hours
-
Moderate otitis externa (canal narrowed, moderate discharge):
- Ciprofloxacin-dexamethasone drops BID x 7 days (92% cure rate)
- Wick placement if canal <50% patent
- Oral analgesics for pain control
- Re-evaluation at 3-5 days
-
Severe otitis externa (canal occluded, severe pain):
- Wick placement with antibiotic-steroid drops QID
- Oral antibiotics if cellulitis present
- Narcotic analgesics for 48-72 hours
- ENT referral if no response in 72 hours
Acute otitis media treatment has evolved toward selective antibiotic use based on age, severity, and risk factors, with watchful waiting appropriate in selected cases showing similar outcomes to immediate antibiotics.
| Patient Category | Immediate Antibiotics | Watchful Waiting | Success Rate |
|---|---|---|---|
| <6 months | Always indicated | Not recommended | 90% cure |
| 6-24 months | If severe or bilateral | If mild + unilateral | 85% either approach |
| >2 years | If severe symptoms | If mild-moderate | 80% spontaneous resolution |
| Immunocompromised | Always indicated | Contraindicated | Variable |
| Recurrent AOM | Immediate treatment | Not appropriate | Requires prophylaxis |
Sudden sensorineural hearing loss represents an otologic emergency requiring immediate steroid therapy within 72 hours for optimal outcomes, with recovery rates declining significantly after 2 weeks.
-
Primary treatment protocol:
- Prednisone 1 mg/kg (max 80 mg) daily x 7 days, then taper
- Intratympanic steroids if contraindications to oral steroids
- Audiometry at 2 weeks and 3 months
- MRI with gadolinium if no recovery or retrocochlear signs
-
Salvage therapy (if <50% recovery at 2-4 weeks):
- Intratympanic steroid injections (4 mg/mL dexamethasone)
- Weekly injections x 3-4 treatments
- Additional 15-20% recovery rate with salvage therapy
Ménière's disease treatment follows stepped approach from dietary modification to surgical intervention, with medical management controlling symptoms in 70-80% of patients.
💡 Master This: Chronic otitis media with cholesteatoma requires surgical intervention within 6-12 months of diagnosis, as conservative management leads to progressive bone erosion and potential intracranial complications in 15-20% of untreated cases
Vestibular rehabilitation therapy shows 85% improvement in chronic dizziness when properly prescribed, with specific exercises targeting individual vestibular deficits based on diagnostic testing results.
Connect these evidence-based treatment protocols through multi-system integration to understand complex interactions between ear pathology and systemic diseases.
⚖️ Treatment Algorithm Mastery: Evidence-Based Interventions
🔗 Systems Integration Hub: The Connected Ear
📌 Remember: EAR-SYSTEMS - Endocrine (diabetes/thyroid), Autoimmune (vasculitis/RA), Renal (diuretics/ototoxicity), Systemic infections, Youth/aging, Stroke/neurologic, Tumors, Emotion/psychiatric, Medications, Sleep disorders - ear symptoms often reflect systemic disease
Cardiovascular-otologic connections manifest through shared vascular supply and autonomic innervation, where hypertension affects inner ear microcirculation and sudden hearing loss may herald cardiovascular events. Pulsatile tinnitus indicates vascular pathology in 85% of cases, requiring systematic vascular evaluation.
- Cardiovascular causes of ear symptoms:
- Hypertension: Inner ear ischemia → progressive SNHL in 40% of uncontrolled cases
- Atherosclerosis: Vertebrobasilar insufficiency → episodic vertigo + neurologic signs
- Arteriovenous malformations: Pulsatile tinnitus + objective bruit in 90%
- Carotid stenosis: Ipsilateral pulsatile tinnitus + cervical bruit
- Doppler studies show >70% stenosis in symptomatic patients
- Surgical correction resolves tinnitus in 80% of cases
Endocrine-otologic interactions involve metabolic effects on inner ear function, where diabetes mellitus causes microvascular damage and thyroid disorders affect hearing sensitivity. Diabetic patients show 2-fold increased risk of hearing loss, with HbA1c >7% correlating with accelerated presbycusis.
| Endocrine Condition | Otologic Manifestation | Mechanism | Prevalence |
|---|---|---|---|
| Diabetes mellitus | Progressive SNHL | Microvascular damage | 40% of diabetics |
| Hypothyroidism | Low-frequency hearing loss | Myxedematous changes | 25% of cases |
| Hyperthyroidism | Tinnitus + hyperacusis | Increased metabolism | 15% of cases |
| Addison's disease | Sudden SNHL | Autoimmune cross-reactivity | 10% of cases |
| Cushing's syndrome | Chronic otitis media | Immunosuppression | 20% of cases |
⭐ Clinical Pearl: Bilateral sudden sensorineural hearing loss suggests systemic disease in 60% of cases - autoimmune, infectious (syphilis, Lyme), neoplastic (leukemia, carcinomatous meningitis), or ototoxic causes require immediate investigation
Neurologic-otologic integration involves shared neural pathways where central nervous system pathology produces peripheral symptoms. Acoustic neuromas account for 85% of cerebellopontine angle tumors, presenting with unilateral hearing loss in 95% and tinnitus in 85% of cases.
- Central causes of peripheral symptoms:
- Multiple sclerosis: Sudden hearing loss in 10%, vertigo in 50%
- Migraine: Vestibular symptoms in 40%, hearing loss in 15%
- Stroke: Acute vertigo with AICA infarction, hearing loss rare
- Temporal lobe epilepsy: Auditory hallucinations, vertigo as aura
Medication-induced ototoxicity represents preventable hearing loss affecting >500,000 patients annually, where aminoglycosides, loop diuretics, and chemotherapy agents cause dose-dependent and often irreversible damage.
💡 Master This: Ototoxicity monitoring requires baseline audiometry before high-risk medications, with serial testing during treatment - >15 dB decline at any frequency or >10 dB decline at two consecutive frequencies indicates significant ototoxicity requiring dose modification
Psychiatric-otologic connections involve bidirectional relationships where hearing loss increases depression risk by 2.4-fold, while anxiety disorders exacerbate tinnitus perception and vestibular symptoms. Cognitive behavioral therapy improves tinnitus-related distress by 40-60% in controlled trials.
Sleep disorder-otologic interactions reveal how sleep apnea affects inner ear function through intermittent hypoxia, while hearing loss disrupts sleep architecture and circadian rhythms. CPAP therapy improves sudden hearing loss recovery by 25% in sleep apnea patients.
Connect these multi-system insights through clinical mastery frameworks to develop comprehensive diagnostic and therapeutic approaches for complex ear diseases.
🔗 Systems Integration Hub: The Connected Ear
🎯 Clinical Command Center: Rapid Mastery Arsenal
📌 Remember: MASTER-EAR - Mechanisms (4 pathways), Assessment (systematic exam), Symptoms (pattern recognition), Tests (evidence-based), Emergencies (time-sensitive), Referrals (specialist criteria), EAR-specific protocols, Algorithms (treatment), Recovery (monitoring) - comprehensive framework for clinical excellence
Essential Clinical Thresholds for immediate decision-making:
| Clinical Parameter | Normal Range | Pathological Threshold | Action Required |
|---|---|---|---|
| Hearing loss onset | Gradual | <72 hours | Emergency steroid protocol |
| Air-bone gap | <10 dB | >15 dB | Conductive loss workup |
| Weber lateralization | Midline | Lateralizes | Asymmetric loss present |
| Vertigo duration | None | >20 minutes | Central vs peripheral eval |
| Tympanic membrane mobility | Normal | Decreased/absent | Middle ear pathology |
| Canal wall erythema | Pink | Red + swollen | Otitis externa treatment |
-
30-Second Assessment:
- Weber test → Lateralization pattern
- Rinne test → Conductive vs sensorineural
- Tragal tenderness → External vs middle ear
- Otoscopy → Structural abnormalities
-
2-Minute Focused History:
- Onset timing → Acute vs chronic
- Associated symptoms → Systemic vs local
- Medication history → Ototoxicity risk
- Recent exposures → Infectious causes
⭐ Clinical Pearl: "Rule of 15s" - >15 dB air-bone gap = conductive loss, >15 dB asymmetry = retrocochlear workup, >15 dB decline = ototoxicity, <15 minutes vertigo = BPPV likely - rapid thresholds for clinical decisions
Emergency Recognition Criteria requiring immediate intervention:
-
Sudden sensorineural hearing loss:
- >30 dB loss in <72 hours
- Prednisone 1 mg/kg within 72 hours
- Recovery rate: 60% if treated <72h, 20% if >2 weeks
-
Malignant otitis externa:
- Diabetic + severe otalgia + granulation tissue
- Pseudomonas infection with bone involvement
- Mortality: 20% if untreated, <5% with aggressive therapy
-
Acute mastoiditis:
- Post-auricular swelling + ear protrusion
- CT scan + IV antibiotics + surgical drainage
- Complication rate: 40% without prompt treatment
Treatment Success Optimization through evidence-based protocols:
| Condition | First-Line Treatment | Success Rate | Alternative Options |
|---|---|---|---|
| Otitis externa | Ciprofloxacin-dexamethasone drops | 92% | Acetic acid (mild cases) |
| Acute otitis media | High-dose amoxicillin | 85% | Watchful waiting (selected) |
| BPPV | Canalith repositioning | 90% | Vestibular rehabilitation |
| Sudden SNHL | Oral prednisone | 60% | Intratympanic steroids |
| Ménière's disease | Low-sodium diet + diuretics | 70% | Intratympanic gentamicin |
Clinical Mastery Checklist for comprehensive care:
-
Diagnostic Excellence:
- Pattern recognition → >90% accuracy
- Systematic examination → Missed findings <5%
- Appropriate testing → Cost-effective workup
- Timely referrals → Optimal outcomes
-
Treatment Optimization:
- Evidence-based protocols → Maximum efficacy
- Patient-specific factors → Individualized care
- Monitoring parameters → Early intervention
- Complication prevention → Safety first
Continuous Learning Framework for expertise maintenance:
- Monthly case review → Pattern reinforcement
- Literature updates → Evidence integration
- Multidisciplinary conferences → Systems thinking
- Quality metrics tracking → Performance optimization
This clinical command center provides the essential tools and systematic approaches needed for expert-level ear disease management, enabling rapid diagnosis, evidence-based treatment, and optimal patient outcomes across all clinical presentations.
🎯 Clinical Command Center: Rapid Mastery Arsenal
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app
























