Pathophysiology of Allergic Rhinitis: Overview - Sneezing Storm Intro
Allergic Rhinitis (AR) is an IgE-mediated nasal mucosal inflammation triggered by allergen exposure, manifesting as paroxysmal sneezing, watery rhinorrhea, nasal itching, and congestion.
⭐ The Allergic Rhinitis and its Impact on Asthma (ARIA) guidelines classify AR based on duration (Intermittent/Persistent) and severity (Mild/Moderate-Severe), guiding stepwise management.
ARIA Classification:
- Duration of Symptoms:
- Intermittent: < 4 days/week OR < 4 consecutive weeks.
- Persistent: > 4 days/week AND > 4 consecutive weeks.
- Severity of Symptoms:
- Mild: Normal sleep; No impairment of daily activities, sport, leisure; No troublesome symptoms.
- Moderate-Severe: One or more of: Abnormal sleep; Impairment of daily activities, sport, leisure; Troublesome symptoms.
Common Allergens (Indian Context):
- Pollen (e.g., Parthenium, grasses)
- House Dust Mites (e.g., Dermatophagoides pteronyssinus, D. farinae)
- Fungi (e.g., Aspergillus, Alternaria)
- Animal dander
- Cockroach allergens
Pathophysiology of Allergic Rhinitis: Key Players & Sensitization - The Allergy Army
- Key Cells (The Allergy Army):
- Antigen Presenting Cells (APCs)
- Th2 lymphocytes
- B-cells (→ Plasma cells)
- Mast cells
- Eosinophils
- Basophils
- Key Mediators (The Weapons):
- IgE
- Histamine
- Leukotrienes ($LTC_4, LTD_4, LTE_4$)
- Prostaglandins ($PGD_2$)
- Cytokines (IL-4, IL-5, IL-9, IL-13, TNF-α)
- Chemokines
Sensitization: Priming the Army
⭐ Th2 lymphocytes are pivotal, releasing IL-4 (promotes IgE synthesis by B cells), IL-5 (recruits/activates eosinophils), and IL-13 (↑ IgE, mucus secretion, airway hyperresponsiveness).

Pathophysiology of Allergic Rhinitis: Early Phase Reaction - Phase 1 Assault
- Trigger: Allergen re-exposure.
- Mechanism: Allergen cross-links IgE on sensitized mast cells → Degranulation.
- Mediators Released:
- Pre-formed (minutes):
- Histamine: Sneezing, itching, rhinorrhea, nasal congestion (vasodilation, ↑ vascular permeability).
- Tryptase, Proteases, Heparin.
- Newly Synthesized (minutes-hours):
- Leukotrienes ($LTC_4, LTD_4, LTE_4$): Potent bronchoconstrictors, ↑ vascular permeability, mucus secretion, chemotaxis.
- Prostaglandin $D_2$ ($PGD_2$).
- Platelet-Activating Factor (PAF).
- Pre-formed (minutes):
- Clinical: Onset 5-30 minutes; lasts 1-3 hours.
⭐ Histamine, released from mast cell granules during the early phase, is the primary mediator of acute symptoms like sneezing, pruritus, and watery rhinorrhea, acting on H1 receptors.
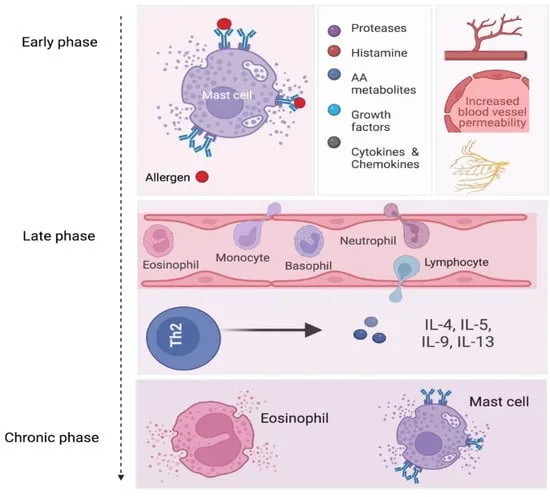
Pathophysiology of Allergic Rhinitis: Late Phase & Chronic Features - Phase 2 Siege
- Onset & Duration:
- Starts: 4-8 hours post-allergen.
- Peaks: 12-24 hours.
- Lasts: 24-48 hours or longer.
- Mechanism:
- Infiltration & activation of inflammatory cells: Eosinophils, basophils, Th2 cells, neutrophils, monocytes.
- Driven by chemokines & cytokines from early phase.
- Key Player: Eosinophils
- Release: Toxic proteins (Major Basic Protein - MBP, Eosinophil Cationic Protein - ECP), leukotrienes, cytokines.
- Effects: Epithelial damage, chronic inflammation.
- Clinical Manifestations:
- Predominant: Sustained nasal congestion.
- Systemic: Fatigue, malaise.
- Local: Nasal hyperreactivity.
- Nasal Priming: Repeated allergen exposure ↓ reaction threshold.
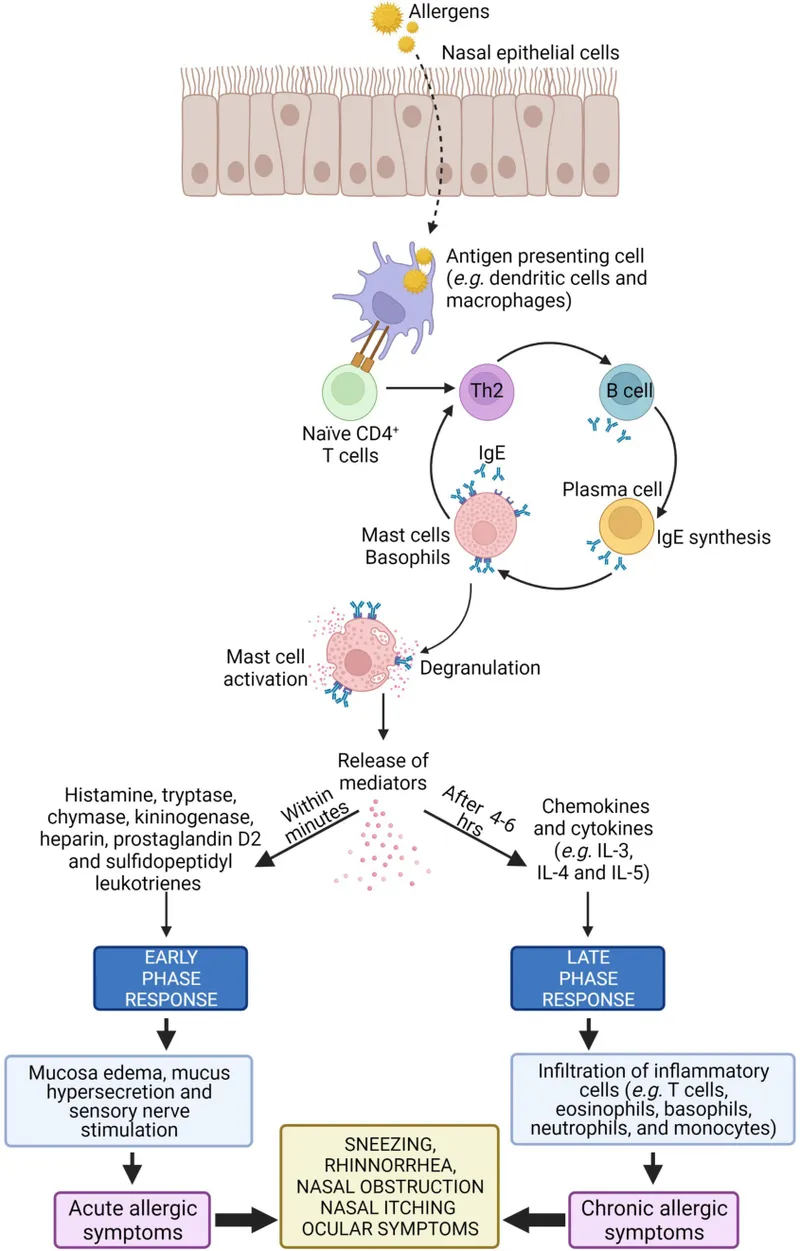
⭐ The late-phase reaction, characterized by a significant influx of eosinophils, is responsible for persistent symptoms, particularly nasal congestion, and contributes to nasal hyperreactivity.
High‑Yield Points - ⚡ Biggest Takeaways
- IgE-mediated Type I hypersensitivity is the core mechanism.
- Sensitization: Allergen exposure → IgE production → IgE coats mast cells.
- Early Phase (minutes): Re-exposure → mast cell degranulation → histamine release → acute symptoms.
- Late Phase (4-8 hours): Eosinophil and lymphocyte infiltration → sustained inflammation and congestion.
- Th2 cells orchestrate via IL-4 (IgE switching), IL-5 (eosinophil recruitment/activation), IL-13 (mucus).
- Key mediators: Histamine (sneezing, itching, rhinorrhea), Leukotrienes (nasal blockage).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

