Introduction & Epidemiology - Mask of Mystery
- Definition: Acquired, often symmetric, macular hyperpigmentation on sun-exposed areas, primarily the face.
- Common Names: "Mask of pregnancy" (chloasma).
- Prevalence: Common, especially in Indian populations and individuals with Fitzpatrick skin types III-VI.
- Key Risk Factors (Multifactorial):
- UV radiation (UVA, UVB, visible light) - most important avoidable factor.
- Hormonal influences: Pregnancy (melasma gravidarum), OCPs, HRT.
- Genetic predisposition & positive family history.
- Photosensitizing medications (e.g., phenytoin, tetracyclines).
- Thyroid dysfunction.
- Certain cosmetics.

⭐ Melasma is significantly more common in women (approx. 9:1 female to male ratio) and individuals with Fitzpatrick skin types III-VI.
Pathophysiology - Pigment Party Crashers
- Primary Mechanism: Melanocyte hyperactivity (not proliferation) → ↑ melanogenesis & ↑ melanosome transfer to keratinocytes.
- Hormonal Influence: Estrogen, progesterone receptors, & MSH are key hormonal drivers.
- Signaling Pathways: Stem cell factor (SCF) & Wnt signaling implicated.
- UV Radiation: Major trigger; causes direct melanocyte stimulation, oxidative damage.
- Vascular & Inflammatory: ↑ VEGF, ↑ vascularity, & mast cell activation contribute.
- Genetic Predisposition: Inherited factors increase susceptibility.
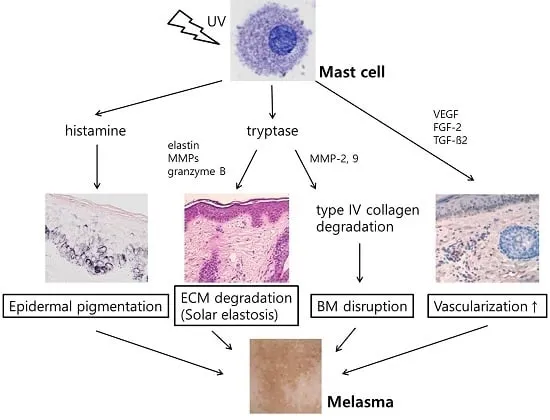
⭐ Recent evidence highlights the role of vascular endothelial growth factor (VEGF) and increased vascularity in melasma pathogenesis, suggesting a link beyond just melanocytes.
Clinical Features & Diagnosis - Spot the Spots
- Symmetric, irregular, light-to-dark brown hyperpigmented macules and patches.
- Common patterns:
- Centrofacial: Forehead, cheeks, nose, upper lip, chin.
- Malar: Cheeks, nose.
- Mandibular: Ramus of mandible.

- Wood's Lamp Examination:
| Melasma Type | Wood's Lamp Finding |
|---|---|
| Epidermal | Accentuated contrast |
| Dermal | No/Less accentuation |
| Mixed | Patches of accentuation |
| Indeterminate | (Dark skin) Inconclusive |
- Differential Diagnosis: Post-inflammatory hyperpigmentation (PIH), Hori's nevus, Riehl's melanosis, drug-induced pigmentation, lentigines.
Management - Fading the Freckles
Cornerstone: Sun Protection
- Broad-spectrum (UVA/UVB, Visible Light, Infrared), SPF ≥30-50, PA+++. Daily, year-round.
Topical Therapy
- First-line:
- Hydroquinone (2-4%, max 5%).
- Triple Combination Cream (TCC): e.g., Kligman's/Modified. Components: Hydroquinone (HQ) + Tretinoin + Corticosteroid.
- 📌 Mnemonic for Kligman's components: "Heavy Tan Sucks" (Hydroquinone, Tretinoin, Steroid).
- Azelaic acid (15-20%).
- Other options: Kojic acid, Niacinamide, Cysteamine, Thiamidol.
⭐ The original Kligman's formula consists of hydroquinone 5%, tretinoin 0.1%, and dexamethasone 0.1%. Modified versions often use lower potency corticosteroids to reduce side effects.
Oral Agents
- Tranexamic acid (250mg BD).
- Others: Glutathione, Polypodium leucotomos extract.
Procedural Options (For refractory melasma)
- Chemical Peels: Superficial (e.g., glycolic acid, salicylic acid, TCA 10-20%).
- Lasers: Q-switched Nd:YAG (low fluence), Picosecond lasers. ⚠️ Use with caution due to Post-Inflammatory Hyperpigmentation (PIH) risk.
- Microneedling with topical application of depigmenting agents.

Stepwise Management Algorithm
Prevention & Prognosis - Sunscreen Savior
- Sun Protection (Year-Round):
- Strict sun avoidance (even indoors, near windows).
- Use broad-spectrum physical blockers: zinc oxide, titanium dioxide.
- Iron oxide for visible light (VL) protection.
- Wear wide-brimmed hats, sunglasses.
- Prognosis & Management:
- High recurrence rate, especially with sun/hormonal triggers.
- Chronic condition: requires long-term maintenance therapy & patient counseling.
- Address modifiable risk factors (e.g., review OCPs).
⭐ Protection against visible light, particularly blue light, often through tinted sunscreens containing iron oxide, is increasingly recognized as crucial in melasma management due to its pigment-inducing effects.
High‑Yield Points - ⚡ Biggest Takeaways
- Melasma: common hyperpigmentation in women, linked to sun exposure & hormonal changes (e.g., pregnancy - chloasma).
- Symmetric, brownish macules/patches on face (centrofacial, malar, mandibular patterns).
- Wood's lamp differentiates epidermal (enhances) vs. dermal (no enhancement) pigment.
- Strict sun protection is cornerstone of management.
- Topicals: Hydroquinone (first-line), Kligman's formula (hydroquinone, tretinoin, steroid).
- Oral tranexamic acid for resistant cases.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

