Hyperpigmentation Basics - Setting the Scene
- Pathophysiology: ↑ melanin deposition; epidermal (superficial), dermal (deep), or mixed.
- Key Initial Step: Identify and manage underlying triggers (e.g., post-inflammatory, drugs).
- Sun Protection: Cornerstone. Daily broad-spectrum SPF >30 (ideally 50).
- Counseling: Stress patience; improvement takes weeks to months (~8 weeks minimum).
- Approach: Combination therapy often yields best results by targeting multiple pathways.
⭐ Wood's lamp: Differentiates pigment depth-epidermal enhances, dermal doesn't.
Topical Agents - Creamy Combatants

| Agent | MoA | Conc. | Key SEs/Pearls |
|---|---|---|---|
| Hydroquinone (HQ) | Tyrosinase inhibitor | 2-4% | Ochronosis, dermatitis. 📌 HQ Ochronosis: A NO-NO! |
| Retinoids | ↑ Cell turnover, ↓ melanosome transfer | Tret. 0.025-0.1% | Irritation, photosensitivity. Start low. |
| Azelaic Acid | Tyrosinase inhibitor, anti-melanocyte | 15-20% | Mild irritation. Pregnancy safe. |
| Kojic Acid | Chelates Cu in tyrosinase | 1-4% | Dermatitis, photosensitive, unstable. |
| Ascorbic Acid (Vit C) | Antioxidant, ↓ dopaquinone | 5-20% | Unstable (L-form), irritation. |
| Niacinamide (Vit B3) | ↓ Melanosome transfer | 2-5% | Well-tolerated, anti-inflammatory. |
Chemical Peels - Exfoliation Elevation
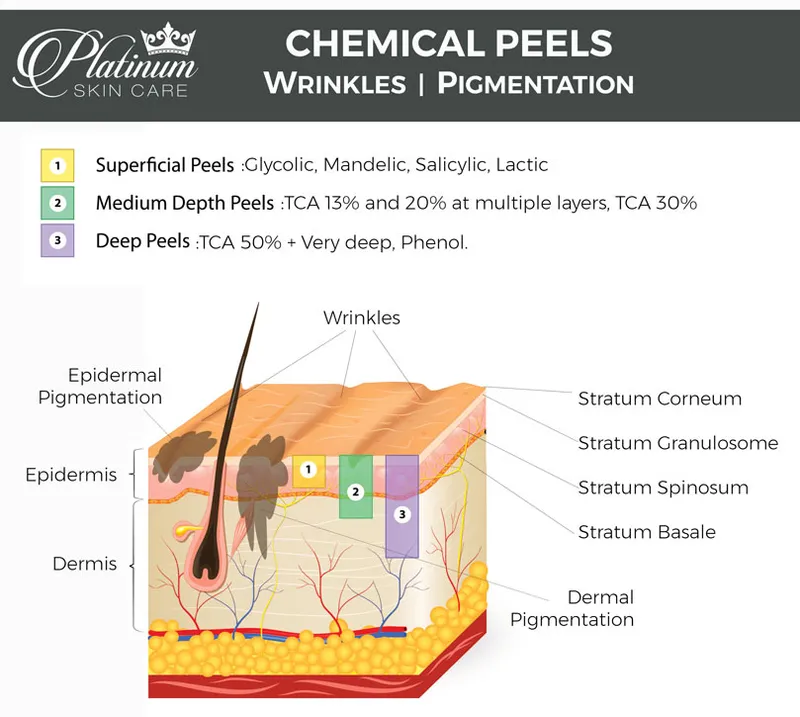
| Peel Type | Depth | Indications for Pigment | Key Considerations for Indian Skin |
|---|---|---|---|
| Glycolic Acid (GA) | Superficial | Melasma, PIH, freckles | 20-35%, priming vital. ⚠️ PIH risk. |
| Salicylic Acid (SA) | Superficial (Lipophilic) | PIH (acne), oily skin | Good for acne + PIH. Less irritant. |
| TCA | Sup (10-25%), Med (30-35%) | Lentigines, AK, deep melasma (cautious) | 10-15% common. Patch test. ⚠️ High PIH risk. |
| Jessner's Peel | Superficial | Melasma, PIH, photodamage | Often combined. ⚠️ Resorcinol concerns. |
Laser & Light - Precision Pigment Pulverizers
- Principle: Selective photothermolysis (heat) or photoacoustic (sound) effects target melanin.
- Common Modalities:
| Device | MoA | Target | Best for | Indian Skin Pearls |
|---|---|---|---|---|
| QS Nd:YAG | Photothermal | Melanosomes | Dermal (Ota), Tattoos | 1064nm safer, ↓PIH; 532nm epidermal |
| Picosecond | Photoacoustic | Melanosomes | Stubborn dermal, Tattoos, Melasma, PIH | ↓PIH risk vs QS; good for LPP |
| IPL | Photothermal (Broadband) | Melanin | Superficial (Freckles, Lentigines) | ↑PIH risk; careful selection, filters needed |
⭐ Picosecond lasers, with ultra-short pulses, minimize thermal damage, reducing PIH risk-critical for Indian skin types prone to hyperpigmentation.
Systemic & Sunscreen - Holistic Hyperpigmentation Help
- Key Systemic Agents:
- Tranexamic Acid: Oral (250mg BD - 500mg BD) or topical (2-5%); inhibits plasmin, reducing melanogenesis.
- Glutathione: Oral/IV; antioxidant, may lighten skin by converting eumelanin to pheomelanin (efficacy varies).
- Vitamin C: Oral/topical; antioxidant, inhibits tyrosinase.
- Photoprotection (Pillar of Management): 📌 SPF: Sun Protection First!
- Broad-spectrum: Covers UVA (aging) & UVB (burning).
- SPF: 30-50 minimum; PA rating: +++ or ++++.
- Visible Light Protection (VLP): Crucial for Indian skin types; often achieved with tinted sunscreens containing iron oxide.
- Consistent application & reapplication (every 2-3 hours).
⭐ For melasma, strict photoprotection including protection against visible light is paramount to prevent recurrence and worsening.

High‑Yield Points - ⚡ Biggest Takeaways
- Topical agents like hydroquinone, retinoids, and azelaic acid are first-line.
- Broad-spectrum sunscreen is ESSENTIAL for all hyperpigmentation management.
- Chemical peels (e.g., glycolic acid) treat superficial pigmentation.
- Q-switched lasers (e.g., Nd:YAG) target deeper dermal pigment and resistant cases.
- Tranexamic acid (oral/topical) is effective for melasma.
- Combination therapies often yield superior results.
- Address underlying inflammation in Post-Inflammatory Hyperpigmentation (PIH) and ensure photoprotection.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

