UV Radiation & Skin - Sunny Side Effects
- UV Spectrum & Penetration:
- UVC (100-280 nm): Mostly ozone-absorbed.
- UVB (280-320 nm): Epidermis. 📌 "B" for Burn, DNA damage, Vit D.
- UVA (320-400 nm): Dermis. 📌 "A" for Aging, Tanning.
- UVA1 (340-400 nm); UVA2 (320-340 nm, also erythrogenic).
- Acute Skin Damage:
- Sunburn (Erythema): UVB primary. Peaks 12-24 hrs.
- Tanning: Immediate Pigment Darkening (IPD) (UVA), Delayed Tanning (UVB/UVA).
- Chronic Skin Damage:
- Photoaging: Wrinkles, solar elastosis, lentigines (UVA > UVB).
- Photocarcinogenesis: Actinic keratosis, Squamous Cell Carcinoma (SCC), Basal Cell Carcinoma (BCC), Melanoma (UVB major, UVA contributes).
⭐ UVB is approximately 1000 times more erythemogenic than UVA radiation.
Sunscreens Explained - Shield Up Science
- Types & Mechanisms:
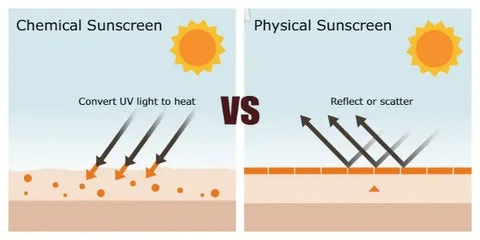
- Physical (Mineral): ZnO, TiO2. Reflect/scatter UV. Broad spectrum. Good for sensitive skin.
- Chemical (Organic): Oxybenzone, Avobenzone. Absorb UV, convert to heat.
- Hybrid: Combine physical & chemical filters.
- Efficacy Measures:
- SPF (Sun Protection Factor): UVB protection. Min. SPF 30 (~97% UVB block) recommended.
- PA System: UVA protection (e.g., PA+, PA++, PA++++). Prevents photoaging.
- Broad Spectrum: Essential for UVA/UVB coverage.
- Application Essentials:
- Amount: 2 mg/cm². (📌 Teaspoon Rule: ~1/2 tsp for face/neck).
- Timing: Apply 15-30 min before sun exposure.
- Reapply: Every 2-3 hrs; after swimming/sweating.
- Water Resistance: Check label (40/80 min).
⭐ "Broad Spectrum" designation indicates protection against both UVA (aging) and UVB (burning) rays, which is critical for comprehensive skin protection.
Beyond Sunscreen - Shade & Smarts
- Physical Barriers are Key:
- Clothing:
- Darker colors, tightly woven fabrics (e.g., denim, polyester) offer superior protection.
- Look for Ultraviolet Protection Factor (UPF) >30; UPF 50+ is excellent.
- Hats: Broad-brimmed (>3 inches or 7.5 cm) shielding face, ears, and neck.
- Sunglasses: UV 400 label, wrap-around design to block 99-100% UVA/UVB rays.
- Clothing:
- Smart Sun Habits:
- Seek shade: Especially during peak UV intensity (10 AM - 4 PM).
- Be mindful of reflective surfaces: Sand, water, snow ↑ UV exposure.
- Additional Shields:
- UV-protective window films for cars/homes.

- UV-protective window films for cars/homes.
⭐ Wetting a fabric usually ↓ its UPF value, especially cotton. Dry clothing is more protective.
Special Cases - Sensitive Skin Savvy
- Children:
- < 6 months: Primarily shade & protective clothing. Physical sunscreens (ZnO, TiO₂) if unavoidable on small, exposed areas.
-
6 months: Broad-spectrum, water-resistant SPF ≥ 30 (physical preferred). Reapply q2h.
- Photosensitive Disorders (e.g., SLE, Porphyrias, XP):
- Strict, year-round photoprotection essential.
- High SPF (50+), broad-spectrum (UVA-PF critical).
- Visible light protection (e.g., tinted iron oxide) for some conditions.
- XP: Meticulous UV protection; high skin cancer risk.
- Drug-Induced Photosensitivity:
- Identify/stop culprit. Key drugs: Tetracyclines (Doxycycline), NSAIDs, Thiazides, Sulfonamides, Amiodarone. 💡 Advise strict broad-spectrum photoprotection.
- Post-Procedure Skin (lasers, peels):
- Strict sun avoidance. Gentle, physical sunscreens.
⭐ For children < 6 months, the primary photoprotection strategy is avoidance of direct sun exposure and use of protective clothing; sunscreens are secondary and physical blockers preferred.
High‑Yield Points - ⚡ Biggest Takeaways
- Sun Protection Factor (SPF) primarily measures protection against UVB-induced erythema.
- Broad-spectrum sunscreens offer protection against both UVA and UVB radiation.
- Physical sunscreens (e.g., zinc oxide, titanium dioxide) work by reflecting and scattering UV light.
- Chemical sunscreens (e.g., oxybenzone, avobenzone) absorb UV radiation and convert it to heat.
- Photopatch testing is crucial for diagnosing photoallergic contact dermatitis from sunscreens.
- UPF (Ultraviolet Protection Factor) in clothing indicates UV protection; UPF 50+ is recommended.
- Advise sunscreen application 15-30 minutes before sun exposure, with reapplication every 2-3 hours.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

