Fundamentals of Photobiology: EMS & Light Physics - Radiant Rules
- Electromagnetic Spectrum (EMS): Relevant portions include Ultraviolet (UV), Visible Light, and Infrared (IR).
- UVA: 320-400 nm (📌 A=Aging, Antigenic)
- UVB: 280-320 nm (📌 B=Burning, Blistering, Barrier function)
- UVC: 100-280 nm (📌 C=Carcinogenic, Can't reach Earth)
- Light Physics & Properties:
- Light consists of photons (energy packets) behaving as waves.
- Energy ($E$) is inversely proportional to wavelength ($\lambda$): $E = hc/\lambda$.
- Shorter $\lambda$ = Higher $E$ (e.g., UVC > UVB > UVA).
- Fundamental Laws (Radiant Rules):
- Grotthuss-Draper Law: Light must be absorbed by a chromophore to initiate a photochemical reaction.
- Bunsen-Roscoe Law of Reciprocity: Biological effect is proportional to total energy dose (Intensity × Duration of exposure).
- Inverse Square Law: Radiant intensity decreases proportionally to $1/d^2$ (d=distance from source).

⭐ UVC radiation, though most potent in causing erythema and DNA damage, is almost entirely absorbed by the ozone layer and does not reach the Earth's surface.
Fundamentals of Photobiology: Skin Chromophores - Dermal Light Traps
- Chromophores: Molecules that absorb specific wavelengths of light (UV, visible, infrared).
- Absorption initiates photochemical reactions.
- Major Endogenous Skin Chromophores:
- Melanin: Epidermal; absorbs broadly (UVB > UVA > visible).
⭐ Melanin is the most important endogenous chromophore, providing natural photoprotection by absorbing UV radiation broadly, particularly UVB and UVA.
- Hemoglobin (Hb): Dermal; Oxy-Hb & Deoxy-Hb absorb visible light (peaks in blue, green, yellow).
- Porphyrins: Absorb Soret band (~400 nm) & Q bands (visible).
- Nucleic acids (DNA/RNA): Epidermal; absorb UVB (260 nm peak).
- Urocanic acid: Epidermal; absorbs UVB (270-290 nm).
- Amino acids (tryptophan, tyrosine): Absorb UVB.
- NADH/NADPH, Flavins: Absorb UVA & visible light.
- Melanin: Epidermal; absorbs broadly (UVB > UVA > visible).
- Dermal Light Traps: Dermal structures (e.g., collagen, elastin) scatter light, ↑ path length, ↑ chance of chromophore absorption.
 Mnemonic: 📌 "My Heavy Protein Nucleus Usually Absorbs Nicely" (Melanin, Hemoglobin, Porphyrins, Nucleic acids, Urocanic acid, Amino acids, NADH/NADPH).
Mnemonic: 📌 "My Heavy Protein Nucleus Usually Absorbs Nicely" (Melanin, Hemoglobin, Porphyrins, Nucleic acids, Urocanic acid, Amino acids, NADH/NADPH).
Fundamentals of Photobiology: Photochemical Reactions & Laws - Photon Power Plays
- Laws of Photochemistry:
- Grotthuss-Draper Law (1st): Light must be absorbed by a chromophore for reaction.
⭐ The Grotthuss-Draper Law is fundamental: light must be absorbed by a molecule (chromophore) for a photochemical reaction to occur.
- Stark-Einstein Law (2nd): One photon activates one molecule (primary step).
- Quantum Yield ($ ext{Φ}$): $\frac{\text{Molecules reacted}}{\text{Photons absorbed}}$.
- Photochemical Reactions:
- Type I (O$_2$-independent): Excited chromophore reacts directly with substrate (electron transfer).
- Type II (O$_2$-dependent): Excited chromophore reacts with $ ext{O}_2$ forming ROS (e.g., $ ext{}^1 ext{O}_2$, $ ext{O}_2^{\cdot-}$).
- Crucial for Photodynamic Therapy (PDT).
- Key Players & States:
- Chromophores: Absorb light (melanin, porphyrins, psoralens).
- Energy States: Ground ($S_0$), Excited Singlet ($S_1$), Triplet ($T_1$). $S_1 \rightarrow T_1$ (Intersystem Crossing).

Fundamentals of Photobiology: Skin's Photobiologic Responses - Sunburn & Beyond
-
Acute Responses (Hours to Days):
- Sunburn (Erythema):
- Mediators: Prostaglandins (PGs), histamine, cytokines.
- Peaks 12-24 hrs, resolves ~72 hrs.
- Minimal Erythema Dose (MED): Lowest UV dose for erythema at 24 hrs.
- Tanning:
- Immediate Pigment Darkening (IPD): UVA/Visible; melanin photo-oxidation.
- Delayed Tanning (Melanogenesis): UVB; ↑melanin synthesis; starts 48-72 hrs.
- Epidermal Hyperplasia: Protective thickening.
- Vitamin D Synthesis: UVB converts 7-DHC to Vit D3. $7\text{-DHC} \xrightarrow{UVB} \text{PreVitD}_3 \rightarrow \text{VitD}_3$.
- Sunburn (Erythema):
-
Chronic Responses (Years):
- Photoaging (Dermatoheliosis): Wrinkles, solar elastosis, pigmentary changes.
- Photocarcinogenesis:
- UVB is primary carcinogen.
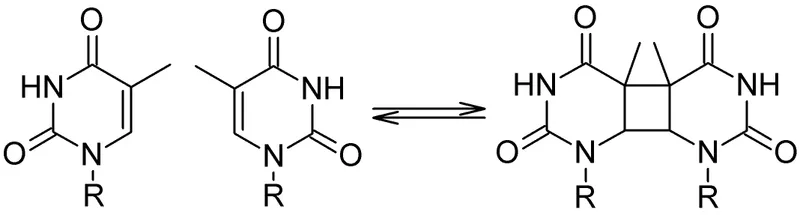
- DNA Damage: Cyclobutane Pyrimidine Dimers (CPDs), (6-4) Photoproducts (6-4PPs). $DNA + UVB \rightarrow CPDs + (6\text{-}4)PPs$.
- Leads to Actinic Keratosis, BCC, SCC, Melanoma.
⭐ UVB-induced cyclobutane pyrimidine dimers (CPDs) are the most common type of DNA damage leading to mutations and skin cancer if not repaired.
High‑Yield Points - ⚡ Biggest Takeaways
- UV radiation: UVA (320-400nm), UVB (290-320nm), UVC (200-290nm); UVB most erythemogenic.
- Skin chromophores (DNA, melanin) absorb UV light, initiating reactions.
- UVB causes direct DNA damage (pyrimidine dimers) and sunburn.
- UVA penetrates deeper, causes photoaging, and indirect DNA damage (ROS).
- Sunburn cells (apoptotic keratinocytes) are a key feature of UVB injury.
- Minimal Erythema Dose (MED) quantifies individual UVB sensitivity.
- Grotthuss-Draper Law: Light must be absorbed for photochemical effect.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

