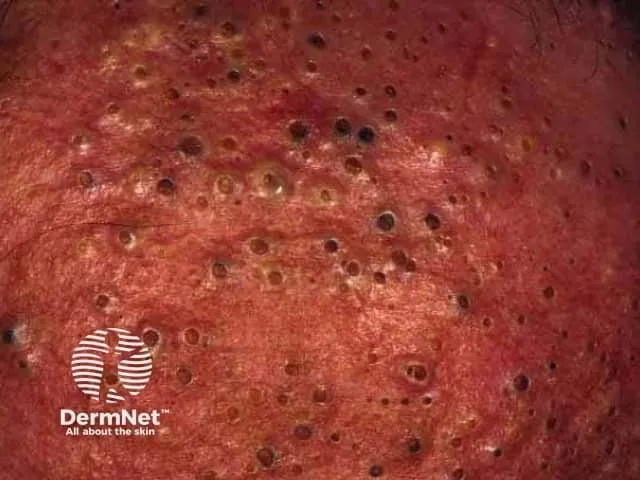
Occupational Acne - Job-Related Zits
- Acneiform eruption from workplace chemical exposure.
- Causative Agents:
- Oils (mineral, cutting).
- Coal tar (pitch, creosote).
- Halogenated hydrocarbons (dioxins, PCBs) → Chloracne.
- Features: Comedones, papules, pustules, cysts on exposed areas.
- Key: Remove exposure; treat like acne vulgaris.
⭐ Occupational acne is a specific form of acneiform eruption directly caused by workplace exposure to certain chemicals.
Occupational Acne - Workplace Culprits
📌 Oily Tars Halt Complexions (Oils, Tars, Halogenated compounds)
- Oils: Insoluble cutting oils, mineral oils, petroleum derivatives.
- Mechanism: Direct follicular occlusion, potent comedogenicity.
- Tars: Coal tar, pitch, creosote.
- Mechanism: Induce follicular hyperkeratosis; may cause photosensitivity.
- Halogenated Aromatic Hydrocarbons: Dioxins (TCDD), Polychlorinated Biphenyls (PCBs), Chloronaphthalenes.
- Mechanism: Alter sebaceous gland function (metaplasia), severe follicular hyperkeratosis, inflammation.
- Result: Chloracne.
⭐ Chloracne, caused by halogenated aromatic hydrocarbons (e.g., dioxins, PCBs), is the most severe and persistent form of occupational acne.
- Others:
- Heavy greases, waxes, chlorinated paraffins.
- Persistent friction/pressure (acne mechanica).

Occupational Acne - Spotting Job Acne
Caused by workplace exposure to acnegenic agents. Key types include:
| Type | Morphology | Distribution |
|---|---|---|
| Oil Acne | Comedones (open/closed), papules, pustules, cysts. Monomorphic. | Exposed areas (face, arms), clothing-covered (thighs, buttocks). |
| Tar Acne | Prominent comedones, papules, pustules. | Exposed areas (face, V-neck, forearms, scrotum). |
| Chloracne | Straw-colored cysts, open comedones, nodules. Less inflammation. | Malar, retroauricular, axillae, groin. Spares nose. |
⭐ Lesions in occupational acne are typically monomorphic (e.g., predominantly comedones in oil acne) and often found on exposed areas and sites of friction with contaminated clothing.
Occupational Acne - Confirming the Cause
⭐ A meticulous occupational history detailing exposures, temporal relationship of symptoms to work, and improvement away from work is paramount for diagnosis.
- Diagnostic Steps:
- Occupational History: Identify workplace exposures (oils, tars, halogens), tasks, symptom link to work.
- Clinical Exam: Note lesion morphology (comedones, inflammatory lesions) and distribution (exposed/occluded sites).
- Patch Testing: Rarely needed; for suspected allergic component.
- Rule out DDx. (See below)
- Key Differential Diagnoses:
- Acne vulgaris (compare onset, distribution)
- Rosacea (no comedones, flushing)
- Bacterial folliculitis (monomorphic, itchy)
- Steroid acne (monomorphic, steroid history)
- Drug-induced acne (medication link)
Occupational Acne - Workplace Skin Shield
Caused by workplace exposure to oils, tars, greases, or chlorinated hydrocarbons (chloracne). Presents with comedones, papules, pustules, cysts on exposed or friction-prone areas.
- Management:
- Prevention: 📌 SHIELD
- Substitute hazards
- Hygiene (frequent washing)
- Isolate process
- Engineering controls (ventilation)
- Learn (educate workers)
- Don PPE (gloves, aprons)
- Treatment:
- Remove from exposure.
- Topical: retinoids, antibiotics.
- Systemic: antibiotics; isotretinoin (severe/chloracne).
- Prevention: 📌 SHIELD
⭐ Primary prevention through elimination/substitution of causative agents, engineering controls, and appropriate personal protective equipment (PPE) is the most effective strategy.
oka
High‑Yield Points - ⚡ Biggest Takeaways
- Occupational acne arises from workplace contact with comedogenic agents like oils, tars, and cutting fluids.
- Chloracne, a severe type, is from chlorinated hydrocarbons (dioxins, PCBs), presenting with straw-colored cysts.
- Lesions appear in areas of direct contact with irritants, like forearms and face.
- Key features: comedones (blackheads, whiteheads), inflammatory papules, and pustules.
- Removing exposure to the causative agent is crucial for management.
- Prevention includes protective gear and strict workplace hygiene practices.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more