Intro & Definition - Workplace Skin Woes
- Irritant Contact Dermatitis (ICD): A non-immunologic inflammatory skin reaction from direct cytotoxic effects of workplace irritants (e.g., chemicals, detergents, friction).
- Epidemiology: Most common occupational skin disease; high in wet work, manufacturing, agriculture, healthcare sectors.
- Distinction: Unlike Allergic Contact Dermatitis (ACD), ICD doesn't require prior sensitization.
⭐ ICD accounts for approximately 80% of all occupational contact dermatitis cases.
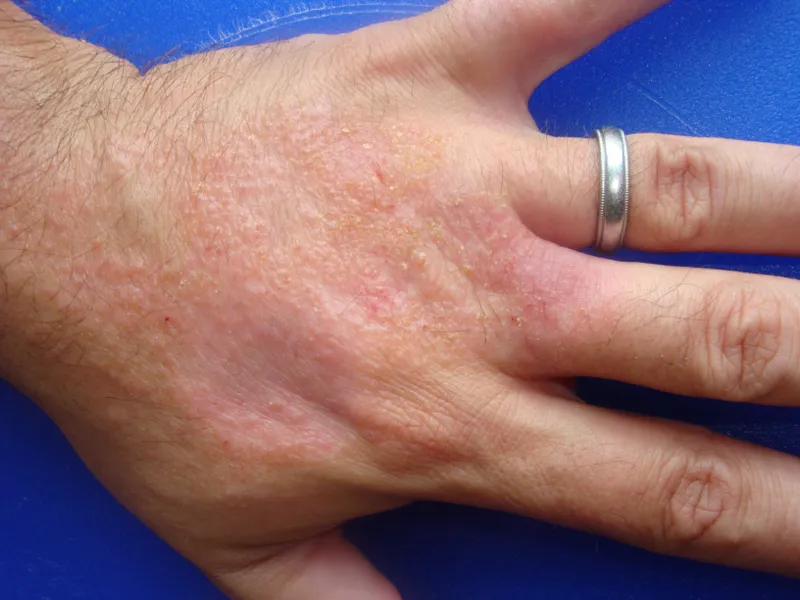
Pathophysiology - Skin's Chemical Clash
- Core Mechanism: Direct cytotoxic damage to keratinocytes.
- Disrupts skin barrier: lipid removal, protein denaturation.
- Irritant Potency Factors:
- ↑ Concentration, extreme pH (e.g., <3 or >10).
- ↑ Duration & frequency of contact.
- Host Susceptibility:
- Pre-existing atopy, site (thin skin), occlusion.
- Manifestations:
- Acute ICD: Single/few exposures to strong irritants.
- Chronic ICD: Repeated exposures to weaker irritants.
⭐ Cumulative ICD results from repeated exposure to weak irritants, often sub-threshold.
Common Irritants - Workplace Hit List
- Strong: Acids (e.g., $H_2SO_4$), Alkalis (e.g., $NaOH$) - Chemical workers, cleaners.
- Weak/Cumulative:
- Soaps/Detergents: e.g., hand sanitizers (healthcare), cleaners.
- Solvents: e.g., degreasers (painters, mechanics).
- Oils (Cutting fluids): e.g., coolants (metalworkers, mechanics).
- Dusts: e.g., cement (construction), wood (carpenters).
- Wet Work: Food handlers, hairdressers. (Hands in water >2 hrs/day)

⭐ Wet work (>2 hrs/day or >20 hand washes/day) is a key risk factor for occupational ICD.
Clinical Features - Rash on the Job
- Symptoms: Itching, burning, pain, dryness, stinging sensation.
- Signs:
- Acute phase: Erythema, edema, vesicles, sometimes bullae.
- Chronic phase: Scaling, lichenification (thickening), fissures.
- Distribution: Primarily hands, forearms; any area of direct irritant contact. 'Site mirrors exposure'.
- Timing: Symptoms characteristically improve when away from work (e.g., weekends, holidays).
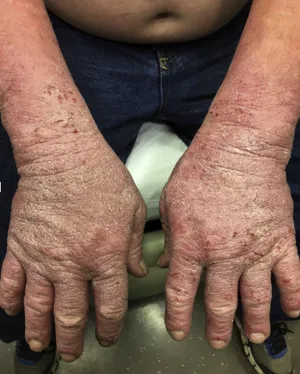
⭐ ICD lesions are typically sharply demarcated, corresponding precisely to the area of irritant contact.
Diagnosis & DDx - Spotting the Irritant
- History: Detailed occupational exposure (type, duration, intensity of irritant), clear temporal link to work.
- Exam: Morphology (erythema, edema, vesicles, bullae, scaling, fissures); distribution on exposed areas (hands, forearms).
- Patch Testing: Crucial to exclude ACD. Often negative or shows weak, non-specific reactions in pure ICD.
- DDx: Allergic Contact Dermatitis, Atopic Dermatitis (may predispose to ICD), Psoriasis, Fungal infections (e.g., Tinea manuum).
⭐ A thorough occupational history is paramount in diagnosing occupational ICD.
 📌 Patch test: ACD (+), ICD (-/weak). Allergy history: ACD (+). Cumulative insults: ICD. History is key.
📌 Patch test: ACD (+), ICD (-/weak). Allergy history: ACD (+). Cumulative insults: ICD. History is key.
Management & Prevention - Workplace Skin Shield
Management:
- Irritant: Identify & avoid/minimize.
- Barrier repair: Emollients.
- Inflammation: Topical corticosteroids (short-term).
- Acute flares: Wet dressings.
Prevention (Hierarchy of Controls):
- Eliminate/Substitute irritants.
- Engineering: Ventilation, enclosure.
- Administrative: Job rotation, training.
- PPE:
- Gloves (e.g., nitrile, vinyl), barrier creams.
- Ensure proper selection & use. 📌 'SKINCARE' (Substitute irritants, Keep skin moisturized, Inform about risks, Note early signs, Cleanse gently, Avoid over-washing, Right PPE, Educate). Patient education: Skin care practices.

⭐ Emollients are the cornerstone of both treatment and prevention of ICD.
High‑Yield Points - ⚡ Biggest Takeaways
- Irritant Contact Dermatitis (ICD) is the most common occupational dermatosis.
- Results from direct cytotoxic damage to skin; non-immunologic mechanism.
- Common culprits: wet work, detergents, solvents, acids, alkalis.
- Presents as erythema, vesicles, scaling, fissures, primarily on hands and forearms.
- Patch test is typically negative, distinguishing it from allergic contact dermatitis.
- Prevention (e.g., PPE, barrier creams) and irritant avoidance are crucial for management.
- Treatment involves emollients and topical corticosteroids for inflammation control.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

