Definitions & Distinction - Hair Necessities
| Feature | Hirsutism | Hypertrichosis |
|---|---|---|
| Nature | Androgen-dependent; Male-pattern (♀) | Androgen-independent; Any site (♂♀) |
| Hair Type | Terminal (coarse, dark) | Vellus or Terminal |
| Distribution | Face, chest, back (sexual areas) | Generalized or Localized |
Hirsutism: Etiology - Hormone Havoc
Hirsutism: Caused by ↑ androgen production (ovarian/adrenal) or ↑ hair follicle sensitivity to androgens.
- Ovarian (Most Common):
- Polycystic Ovary Syndrome (PCOS): Functional ovarian hyperandrogenism. Often insulin resistance.
- Androgen-secreting tumors: Sertoli-Leydig, hilus cell. Rapid/severe onset is red flag.
- Adrenal:
- Congenital Adrenal Hyperplasia (CAH): Late-onset 21-hydroxylase deficiency most frequent.
- Adrenal tumors (adenoma/carcinoma), Cushing's syndrome (excess cortisol, may ↑ androgens).
- Drug-induced:
- Anabolic steroids, Danazol, certain Progestins (high androgenicity), Phenytoin, Minoxidil.
- Idiopathic Hirsutism:
- Diagnosis of exclusion: normal serum androgens, regular menses. Likely ↑ local 5α-reductase.
📌 Key Causes: PCOS (most common), Congenital Adrenal Hyperplasia (CAH), Ovarian/Adrenal Tumors, Cushing's Syndrome, Drugs.
⭐ Polycystic Ovary Syndrome (PCOS) is the most common cause of hirsutism, accounting for 70-80% of cases.

Hirsutism: Evaluation - Score & Sleuth
- History: Onset (gradual/rapid), progression, menstrual regularity, medications (e.g., OCPs, androgens, valproate), family Hx (PCOS, CAH).
- Examination: Signs of virilization (clitoromegaly, voice deepening, ↑muscle bulk, temporal balding), acanthosis nigricans, galactorrhea, Cushingoid features.
- Ferriman-Gallwey (FG) Score: Assesses 9 androgen-sensitive areas (0-4 each).

- Interpretation:
Score Severity < 8 Normal 8-15 Mild Hirsutism ≥ 16 Moderate/Severe - Hirsutism defined as FG score ≥ 8.
⭐ Rapid onset severe hirsutism + virilization strongly suggests an androgen-secreting neoplasm.
Hirsutism: Management - Taming the Mane
A stepwise approach is key, starting with lifestyle and cosmetic options, then pharmacological if needed.
- Cosmetic/Mechanical: Shaving, waxing, laser, electrolysis, topical eflornithine.
- Pharmacological (Trial for ≥6 months):
- OCPs: Suppress ovarian androgens.
- Antiandrogens:
- Spironolactone 50-200 mg/day (androgen receptor blocker).
- Finasteride 2.5-5 mg/day (5α-reductase inhibitor).
- Combination (OCP + antiandrogen) often superior.
⭐ Oral contraceptive pills (OCPs) are first-line medical therapy for most women with hirsutism, especially those with PCOS.
Hypertrichosis Overview - Fur Real Facts
Hypertrichosis: Excessive hair growth (density, length) anywhere on the body, not androgen-dependent. Affects men and women equally.
- Types:
- Congenital (e.g., Hypertrichosis Lanuginosa Congenita)
- Acquired (e.g., drug-induced, paraneoplastic)
- Generalized or Localized
- Key Causes:
- Drugs: Minoxidil, phenytoin, cyclosporine
- Porphyria Cutanea Tarda
- Anorexia nervosa
- Malignancy (Acquired Hypertrichosis Lanuginosa)
- Management: Address underlying cause; cosmetic (shaving, waxing, laser).
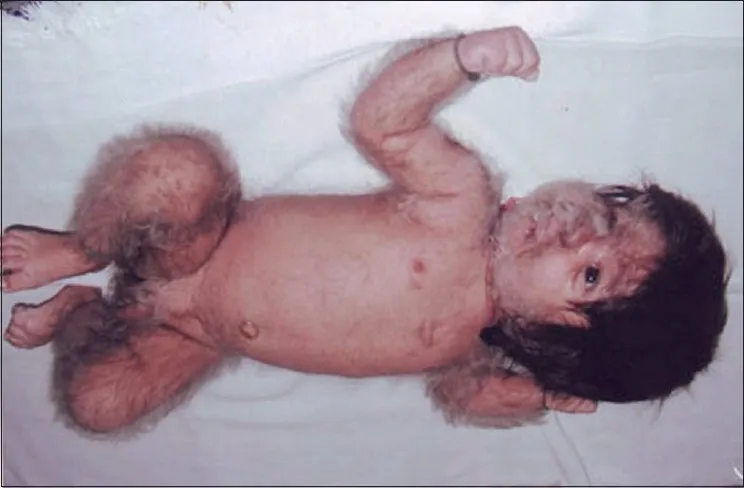
⭐ Acquired hypertrichosis lanuginosa ('malignant down') is a rare but important paraneoplastic sign, often associated with internal malignancies like lung, colon, or breast cancer.
High‑Yield Points - ⚡ Biggest Takeaways
- Hirsutism is excess terminal hair growth in androgen-dependent areas in females; hypertrichosis is generalized, non-androgenic hair growth.
- Polycystic Ovary Syndrome (PCOS) is the most common cause of hirsutism.
- Use the Ferriman-Gallwey score to objectively assess and quantify hirsutism.
- Idiopathic hirsutism presents with normal androgens and regular menses.
- Drugs like minoxidil, phenytoin, and anabolic steroids can cause hirsutism or hypertrichosis.
- Sudden onset with virilization signs (e.g., clitoromegaly) strongly suggests an androgen-secreting tumor.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

