Laser Principles - Light Fantastic!
- LASER: Light Amplification by Stimulated Emission of Radiation.
- Key Properties:
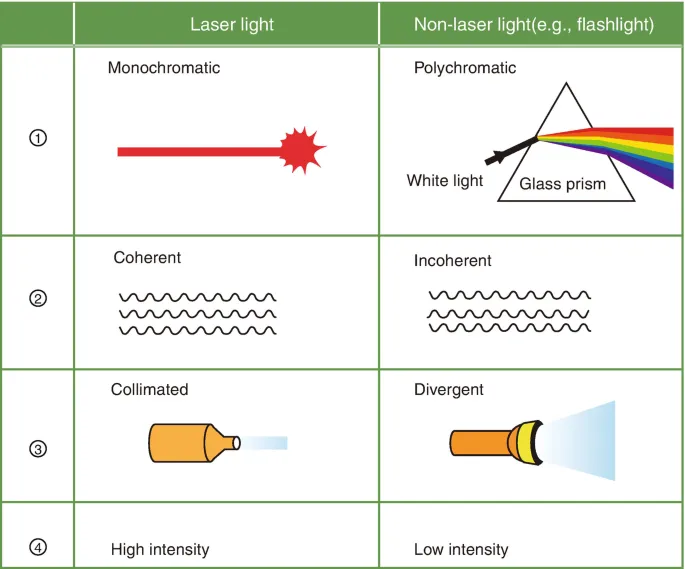
- Monochromaticity: Single wavelength/color. Allows selective targeting of chromophores.
- Coherence: Light waves in phase (spatial & temporal). Enhances power density.
- Collimation: Parallel beams, minimal divergence. Maintains intensity over distance.
- These properties enable precise tissue interaction.
⭐ LASER: Light Amplification by Stimulated Emission of Radiation. Key properties: Monochromaticity, Coherence, Collimation.
Laser-Tissue Interaction - Skin's Reaction
⭐ Selective Photothermolysis: Targets specific chromophores (e.g., melanin, hemoglobin, water) using appropriate wavelength, pulse duration (ideally ≤ Thermal Relaxation Time of target), and fluence to minimize damage to surrounding tissue.
-
Primary Interactions:
- Photothermal: Heat (coagulation, vaporization); most common.
- Photomechanical: Shockwaves (e.g., tattoo removal).
- Photoablative: Vaporization/ablation (precise cutting).
- Photochemical: Chemical reaction (e.g., PDT).
-
Determinants of Effect:
- Target Chromophore: Melanin, Hb, H₂O, ink.
- Wavelength ($ ext{\lambda}$): Governs depth & target absorption.
- Pulse Duration ($t_p$): For selectivity, $t_p ext{ \le TRT}$ (Thermal Relaxation Time).
- Fluence (J/cm²): Energy density.
- Spot Size: Influences penetration depth (larger = deeper).

- Light Propagation in Tissue:
- Absorption (by chromophores): Key for effect.
- Scattering: Influences light distribution & depth.
- Reflection, Transmission.
Dermatology Lasers - Zap Masters
- Laser Types & Primary Targets:
- CO₂ Laser (10600 nm): Ablative. Skin resurfacing, warts, scars, rhinophyma. High water absorption.
- Er:YAG Laser (2940 nm): Ablative. Superficial resurfacing, pigmented lesions. More precise, less thermal damage than CO₂.
- Nd:YAG Laser (1064 nm):
- Q-switched: Tattoo removal (dark inks), pigmented lesions.
- Long-pulsed: Hair removal (darker skin), vascular lesions (deeper vessels).
- Pulsed Dye Laser (PDL) (585 nm, 595 nm): Vascular lesions (port-wine stains, telangiectasias), scars, warts.
⭐ Pulsed Dye Laser (PDL), typically 585 nm or 595 nm, is the gold standard for treating port-wine stains and other superficial vascular lesions like telangiectasias.
- Alexandrite Laser (755 nm): Hair removal (lighter skin), tattoo removal (green/blue inks), pigmented lesions.
- Diode Laser (800-980 nm): Hair removal, vascular lesions.
- Fractional Lasers: Create microscopic treatment zones; ablative or non-ablative. For resurfacing, scars, pigmentation.
📌 Mnemonic: Cold Eskimos Never Prefer Apple Drinks (CO₂, Er:YAG, Nd:YAG, PDL, Alexandrite, Diode for common lasers).
Laser Parameters & Safety - Handle With Care
- Key Parameters:
- Wavelength (nm): Targets specific chromophore (e.g., melanin, Hb); dictates penetration depth.
- Fluence (J/cm²): Energy density ($E/A$); determines thermal effect & therapeutic outcome.
- Pulse Duration (ms, ns, ps): Laser exposure time; vital for selective photothermolysis, matching Thermal Relaxation Time (TRT).
- Spot Size (mm): Diameter of laser beam; larger spots generally penetrate deeper.
- Safety Essentials: (📌 L.A.S.E.R.)
- Light Hazard: MANDATORY wavelength-specific eye protection (patient & all staff).
- Access Control: Restricted area, clear warning signs, Laser Safety Officer (LSO) oversight.
- Smoke Evacuation: Use evacuator for plume (infectious/toxic risk).
- Electrical & Fire Safety: Non-flammable preps, wet drapes, check equipment; avoid O₂ enrichment.
- Responsible Personnel: Trained operators & designated LSO.
⭐ Laser Safety: Mandatory eye protection specific to the laser's wavelength for both patient and operator is the most critical safety measure to prevent irreversible ocular damage. ANSI Z136 standards are key.
- Key Risks: Burns, dyspigmentation (hyper/hypo-), scarring, infection, ocular injury.

High‑Yield Points - ⚡ Biggest Takeaways
- Selective photothermolysis: Specific chromophores absorb distinct laser wavelengths for effect.
- TRT (Thermal Relaxation Time) dictates pulse duration to confine thermal damage.
- Key chromophores: melanin (pigment), oxyhemoglobin (vessels), water (ablative resurfacing).
- Q-switched lasers (nanosecond pulses) effectively treat tattoos and pigmented lesions.
- Pulsed Dye Laser (PDL) (585/595 nm) targets oxyhemoglobin for vascular lesions.
- Ablative lasers (CO2, Er:YAG) target water for skin resurfacing and scar revision.
- Laser safety is crucial: wavelength-specific eye protection mandatory for all present.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

