Topical Corticosteroids: Intro & MOA - Steroid Superpowers
Synthetic steroids for skin conditions, possessing four key "superpowers":
- Anti-inflammatory
- Immunosuppressive
- Anti-proliferative
- Vasoconstrictive
MOA: Primarily genomic, also non-genomic.
- Genomic: Diffuse into cells, bind cytosolic glucocorticoid receptors. Complex translocates to nucleus.
- Upregulates anti-inflammatory proteins like lipocortin-1 (annexin-1).
- Lipocortin-1 inhibits phospholipase A2, blocking synthesis of prostaglandins & leukotrienes.
- Non-genomic: Rapid, less understood membrane-mediated effects.

⭐ Vasoconstriction (blanching) is the basis of the McKenzie-Stoughton assay for assessing TCS potency.
Topical Corticosteroids: Potency Classification - Strength Spectrum Showdown
| Potency Class | Examples | Key Indications (General) |
|---|---|---|
| I: Very Potent | Clobetasol Propionate 0.05% | Severe dermatoses (psoriasis, recalcitrant eczema); Thick skin |
| II: Potent | Betamethasone Dipropionate 0.05% | Mod-severe dermatoses; Non-facial, non-intertriginous areas |
| III-V: Moderate | Mometasone Furoate 0.1%, Triamcinolone Acetonide 0.1% | Mild-mod dermatoses; Face, flexures (use with caution) |
| VI-VII: Mild | Hydrocortisone 1%, 2.5% | Mildest dermatoses; Sensitive areas (face, eyelids), children |
⭐ Clobetasol propionate 0.05% is a Class I (superpotent) topical corticosteroid.
Topical Corticosteroids: Skin Absorption & Vehicles - Delivery Dynamics
Percutaneous absorption influenced by:
- Occlusion: Greatly ↑ absorption.
- Vehicle: Type impacts penetration.
- Site: E.g., scrotum > forehead > scalp.
- Age: ↑ absorption in young/old.
- Skin Integrity: ↑ if damaged.
| Vehicle | Hydration | Potency | Use For |
|---|---|---|---|
| Ointment | High | High | Dry, thick lesions |
| Cream | Mod | Mod | Versatile, good cosmesis |
| Lotion | Low | Low | Hairy/large areas |
| Gel | Low | Var | Hairy areas, face |
| Foam | Low | Var | Scalp, hairy; easy spread |
| Solution | Low | Var | Scalp, hairy; drying |
Topical Corticosteroids: Clinical Uses & Smart Strategies - Healing Helpers
- Key Indications: Inflammatory & hyperproliferative conditions.
- Eczema/Dermatitis (atopic, contact, seborrheic).
- Psoriasis (localized, non-facial).
- Lichen Planus, Discoid Lupus Erythematosus.
- Vitiligo (often adjunctive).
- Alopecia Areata.
- Rational Use Principles:
- Potency: Use lowest effective potency.
- Duration: Shortest possible; avoid prolonged use.
- Vehicle: Ointments (dry/thick), creams (versatile), lotions/gels (hairy areas).
- Site: Lower potency for face, genitals, intertriginous areas, children.
- Tapering: Gradually reduce frequency/potency to prevent rebound.
⭐ One Fingertip Unit (FTU) is approximately 0.5g and covers an area equivalent to two adult handprints.
Topical Corticosteroids: Adverse Effects - The Caution Zone
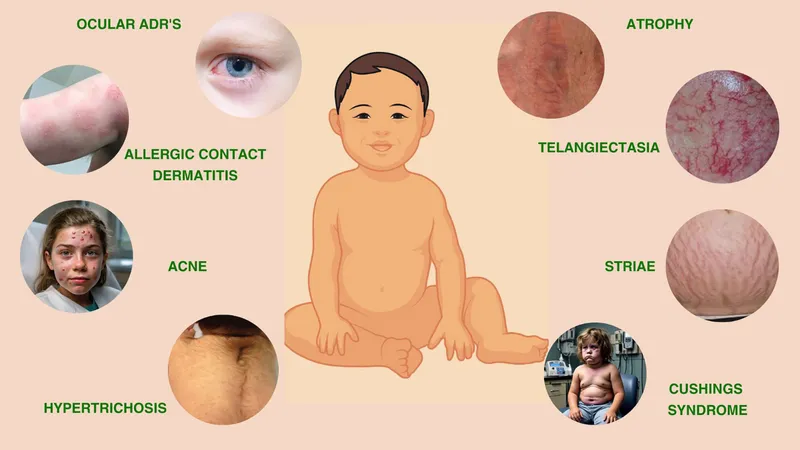
- Local Effects: Common, especially with high potency or prolonged use.
- Skin atrophy, striae (irreversible), telangiectasias, purpura.
- Acneiform eruptions, perioral dermatitis, steroid rosacea.
- Tachyphylaxis (↓ response over time).
- Delayed wound healing, increased skin infections.
- Allergic or irritant contact dermatitis.
- Systemic Effects: Risk ↑ with high potency, large area, occlusion, prolonged use, children.
- Hypothalamic-Pituitary-Adrenal (HPA) axis suppression.
- Iatrogenic Cushing's syndrome.
- Growth retardation (children).
- Hyperglycemia, unmasking latent diabetes.
- Ocular: Cataracts (posterior subcapsular), glaucoma.
⭐ Tachyphylaxis, a diminished response to a drug after repeated use, is a known phenomenon with topical corticosteroids.
High‑Yield Points - ⚡ Biggest Takeaways
- Mechanism: Anti-inflammatory, immunosuppressive, anti-proliferative, vasoconstrictive.
- Potency Classes: Class I (e.g., Clobetasol) is superpotent; Class VII (e.g., Hydrocortisone) is least potent.
- Absorption Factors: ↑ with thin skin (scrotum, eyelids), occlusion, vehicle, and inflamed skin.
- Key Local Side Effects: Skin atrophy, striae, telangiectasias, acneiform eruptions, tachyphylaxis.
- Systemic Side Effects: Risk of HPA axis suppression with high potency, large areas, prolonged use, or occlusion.
- Rational Use: Choose lowest effective potency for shortest duration; consider site and age.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

