Phototherapeutic Agents - Ray Foundations
- Light Basics: Phototherapy utilizes specific UV & visible light wavelengths.
- UV Radiation (UVR) Types:
- UVA (320-400 nm): Deeper penetration. 📌 Think Aging.
- UVA1: 340-400 nm
- UVA2: 320-340 nm
- UVB (290-320 nm): More erythemogenic. 📌 Think Burning, Vitamin B (D synthesis).
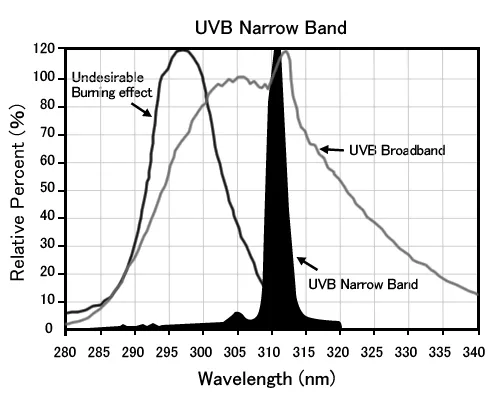
- Broadband (BB-UVB): 290-320 nm
- Narrowband (NB-UVB): 311-313 nm
- UVC (100-290 nm): Germicidal, mostly ozone-filtered.
- UVA (320-400 nm): Deeper penetration. 📌 Think Aging.
- Mechanism: DNA damage, immunomodulation, antiproliferative effects.
- Principle: Grotthuss-Draper law (light must be absorbed for effect).
⭐ The optimal therapeutic range for Narrowband UVB (NB-UVB) is 311-313 nm.
Phototherapeutic Agents - Psoralen Power Play

- Psoralens: Photosensitizing furocoumarins (e.g., 8-MOP, 5-MOP).
- PUVA Therapy: Psoralen + UVA radiation (320-400 nm).
- Mechanism: Psoralens intercalate DNA. UVA activates → covalent DNA photoadducts (cross-links) with pyrimidines → inhibits DNA replication, cell division.
- Administration: Oral 8-MOP (0.4-0.6 mg/kg) 1.5-2 hrs pre-UVA. Topical forms available.
- Indications: Severe psoriasis, vitiligo, CTCL, severe atopic dermatitis.
- Side Effects:
- Acute: Nausea (oral), phototoxicity (erythema, blisters), pruritus.
- Chronic: Premature skin aging (PUVA lentigines), pigment changes, cataracts.
⭐ Long-term PUVA therapy significantly increases the risk of squamous cell carcinoma (SCC), particularly in fair-skinned individuals.
Phototherapeutic Agents - Spectrum Specifics
- UVB Therapy: Utilizes ultraviolet B light; no systemic photosensitizer needed, unlike PUVA.
- Broadband UVB (BB-UVB): Wavelength 290-320 nm.
- Effective for psoriasis, atopic dermatitis.
- Higher risk of erythema, burning compared to NB-UVB.
- Narrowband UVB (NB-UVB): Wavelength 311-313 nm.
- More effective for psoriasis, vitiligo; deeper penetration.
- Lower erythemogenic potential, allowing higher doses.
- Preferred UVB modality for many conditions.
- Broadband UVB (BB-UVB): Wavelength 290-320 nm.
⭐ The Goeckerman regimen, combining crude coal tar application with UVB phototherapy, is a highly effective treatment for severe psoriasis.
Phototherapeutic Agents - Targeted Light Strike
Photodynamic Therapy (PDT): Photosensitizer + Light + O₂ → Reactive Oxygen Species (ROS) → Selective cell kill.
- Mechanism: Photosensitizer (drug) activated by light → Energy transfer to O₂ → ROS (e.g., singlet oxygen $^1O_2$) → Targeted cell destruction.
- Photosensitizers:
- Pro-drugs: Aminolevulinic acid (ALA), Methyl aminolevulinate (MAL).
- Direct: Porphyrins (e.g., Photofrin®), Chlorins.
- Light Sources: Lasers, LEDs. Wavelength matched to photosensitizer (e.g., Blue light ~417 nm for superficial; Red light ~630-635 nm for deeper).
- Indications: Actinic keratoses, Bowen's disease, superficial BCC, acne.
⭐ Aminolevulinic acid (ALA) used in PDT is a pro-drug that is preferentially converted to the photosensitizer Protoporphyrin IX in neoplastic cells.

Phototherapeutic Agents - Guarding the Glow
- PUVA (Psoralen + UVA):
- 8-MOP + UVA → DNA adducts, ↓cell division.
- Uses: Psoriasis, vitiligo, Mycosis Fungoides (MF).
- SE: Phototoxicity, nausea, ↑Squamous Cell Carcinoma (SCC) risk.
- UVB Therapy:
- NB-UVB (311-313 nm): Preferred for psoriasis, vitiligo, atopic dermatitis.
- Action: Induces DNA damage, immunosuppression.
- SE: Erythema, sunburn.
- Excimer Laser: 308 nm (XeCl) for targeted therapy of localized lesions.
⭐ Patients undergoing PUVA therapy must use UV-blocking eye protection for at least 24 hours post-treatment due to psoralen photosensitivity.
High‑Yield Points - ⚡ Biggest Takeaways
- PUVA (Psoralen + UVA) treats psoriasis, vitiligo, CTCL; high photocarcinogenesis risk.
- NB-UVB (311-313 nm) is first-line for psoriasis, vitiligo; safer than PUVA.
- BB-UVB (290-320 nm) is less effective than NB-UVB for psoriasis.
- Acute side effects: Erythema, pruritus, blistering. Chronic: Skin cancer.
- 8-Methoxypsoralen (8-MOP) is the standard psoralen for PUVA.
- Photodynamic Therapy (PDT): Photosensitizer + light for actinic keratoses, superficial BCCs.
- UVA1 (340-400nm) for atopic dermatitis, localized scleroderma.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

