Antihistamines: Intro & MOA - Histamine's Kryptonite
- Antihistamines: Drugs that counteract histamine, a pivotal mediator in allergic and inflammatory skin conditions.
- Histamine's Role in Skin:
- Released by mast cells & basophils.
- Induces key symptoms: pruritus (itching), urticaria (hives), angioedema.
- Causes vasodilation and increased vascular permeability.
- Mechanism of Action (MOA):
- Primarily H1 receptor antagonists: Competitively block histamine binding.
- H1 receptors mediate wheal, flare, and itching.
- Newer agents may also be inverse agonists, stabilizing inactive H1 receptors.
⭐ Antihistamines primarily block H1 receptors; they do not inhibit histamine synthesis or release from mast cells or basophils at therapeutic concentrations typically used for allergy relief, though some may have mast cell stabilizing properties at higher concentrations or with prolonged use (e.g., ketotifen, olopatadine).
Antihistamines: Classification - Sedating vs Selective
- Two main groups: First-generation (sedating) & Second-generation (selective/non-sedating).
| Feature | First-Generation (Sedating) | Second-Generation (Selective/Non-sedating) |
|---|---|---|
| CNS Penetration | High (lipophilic); crosses BBB | Low (lipophobic; P-gp substrates) |
| Sedation | Common, significant | Minimal to none (standard doses) |
| Anticholinergic Effects | Prominent (dry mouth, etc.) | Minimal to none |
| Duration of Action | Shorter (4-6 hrs) | Longer (12-24 hrs) |
| H1 Receptor Selectivity | Lower; also muscarinic, α-adrenergic, serotonergic | Higher for peripheral H1; less off-target |
| Examples (Dermatology) | Hydroxyzine, Diphenhydramine, Chlorpheniramine, Promethazine | Cetirizine, Levocetirizine, Fexofenadine, Loratadine, Desloratadine, Bilastine, Rupatadine |
Antihistamines: Clinical Uses - Itch & Rash Busters
- Urticaria (Acute & Chronic): First-line treatment.
- Chronic Spontaneous Urticaria (CSU): Second-gen H1 preferred; up-dose (up to 4x) before considering omalizumab.
- Pruritus: Symptomatic relief in eczema, drug eruptions, insect bites.
- Atopic Dermatitis: Adjunctive for itch, especially nocturnal (sedating 1st gen often beneficial).
- Other Key Uses:
- Allergic Contact Dermatitis (for associated pruritus).
- Dermographism (highly effective).
- Physical Urticarias (e.g., Cold Urticaria - Cyproheptadine can be useful).
- Mastocytosis (for itch and flushing).
- Anaphylaxis (adjunct to epinephrine; H1 + H2 blockers).
⭐ > For Chronic Spontaneous Urticaria (CSU), guidelines recommend updosing second-generation H1-antihistamines up to four times the licensed dose before considering add-on therapies like omalizumab.
- Agent Choice:
- 2nd Gen (Less/Non-sedating): Cetirizine, Levocetirizine, Fexofenadine, Loratadine, Bilastine. Preferred for daytime use.
- 1st Gen (Sedating): Hydroxyzine, Diphenhydramine, Chlorpheniramine. Useful for nocturnal itch; caution for anticholinergic side effects. 📌 "Hydroxyzine Hides your Itch".
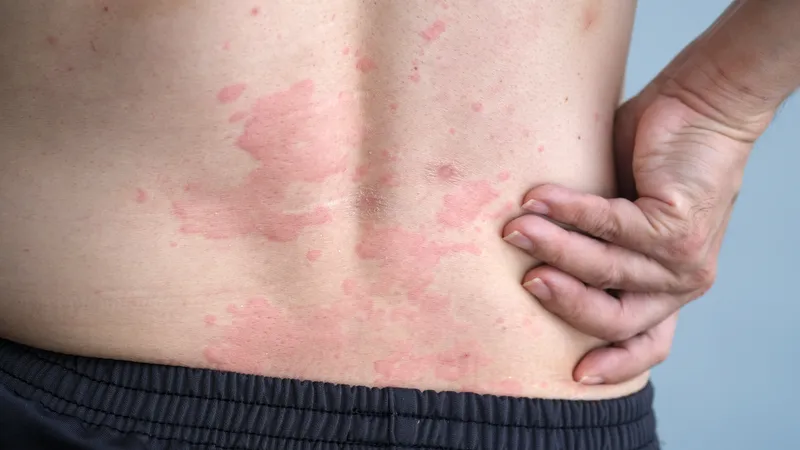
Antihistamines: Adverse Effects - Cautions & Caveats
- 1st Generation (e.g., Hydroxyzine):
- Sedation, impaired cognition ⚠️
- Anticholinergic: dry mouth, urinary retention, blurred vision
- Paradoxical excitation (children)
- 2nd Generation (e.g., Cetirizine, Fexofenadine):
- Less sedation; Fexofenadine least.
- Cetirizine/Levocetirizine: mild sedation (high doses).
- Headache, mild dry mouth.
- Cautions & Caveats:
- Elderly: ↑ risk sedation, falls, anticholinergic effects (prefer 2nd gen).
- Pregnancy: Most 2nd gen Cat B (Cetirizine, Loratadine).
- Lactation: 2nd gen preferred (less sedation).
- Renal/Hepatic impairment: Dose adjustment needed.
- Narrow-angle glaucoma, BPH: Caution (1st gen anticholinergic).
- Avoid alcohol/CNS depressants (with 1st gen).
- Drug interactions (CYP450): Loratadine with inhibitors (macrolides, azoles).
⭐ Fexofenadine, active metabolite of terfenadine, lacks its cardiotoxic risk.
High‑Yield Points - ⚡ Biggest Takeaways
- H1 antihistamines are the cornerstone for managing urticaria and dermatitis-associated pruritus.
- First-generation agents (e.g., chlorpheniramine, hydroxyzine) cause significant sedation and anticholinergic side effects.
- Second-generation agents (e.g., cetirizine, loratadine, fexofenadine) are less sedating and generally preferred.
- Hydroxyzine is particularly useful for psychogenic pruritus due to its anxiolytic properties.
- Ketotifen uniquely combines H1 antagonism with mast cell stabilization.
- Topical doxepin can be used for localized pruritus; systemic doxepin for refractory urticaria.
- Consider drug rotation if tachyphylaxis (tolerance) develops with chronic use.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

