Sclerotherapy: Definition & Goals - Vein Vanish Intro
- Definition: Minimally invasive chemical ablation; sclerosant solution injected into unwanted veins.
- Mechanism: Sclerosant damages endothelium → inflammation, fibrosis → vessel occlusion & resorption.
- Primary Goals:
- Eliminate varicose veins & spider veins (telangiectasias).
- Alleviate symptoms: pain, aching, heaviness, swelling.
- Improve cosmetic appearance.
- Key Indications:
- Varicose veins (CEAP C1-C3).
- Telangiectasias, reticular veins.
- Adjunct for venous malformations; post-surgery residual veins.
- Patient Benefits:
- Outpatient, minimal discomfort & downtime.
- No general anesthesia; quick recovery.
- Safe, effective, cost-efficient.
⭐ Polidocanol (POL) and Sodium Tetradecyl Sulfate (STS) are common FDA-approved sclerosants, widely used.
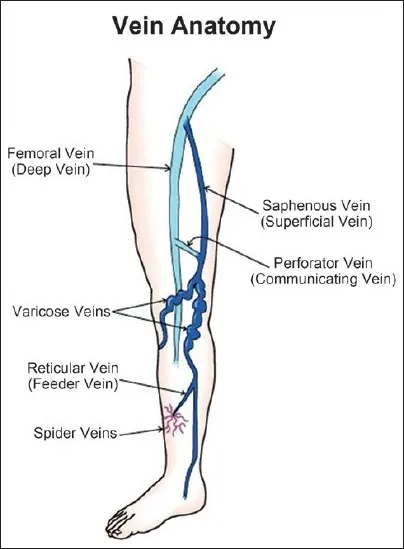
Sclerosants: Types & MOA - Chemical Closure Crew
Sclerosants induce controlled phlebitis and fibrosis. Choice depends on vein size, location, and patient factors.
| Agent | Type | Mechanism of Action (MOA) | Common Conc. | Key Considerations |
|---|---|---|---|---|
| Hypertonic Saline | Osmotic | Dehydrates endothelial cells via osmosis, causing damage. | 18-23.4% | Painful, cramping; high risk of necrosis with extravasation; inexpensive. |
| Polidocanol (POL) | Detergent | Disrupts endothelial cell surface lipids, causing lysis. | 0.25-3% | Anesthetic properties (less pain); lower ulceration risk; rare allergy. |
| Sodium Tetradecyl Sulfate (STS) | Detergent | Damages endothelial cell membrane, leading to thrombosis. | 0.1-3% | Potent; higher risk of hyperpigmentation, telangiectatic matting; allergy. |
| Glycerin (Chromated) | Osmotic/Irritant | Endothelial dehydration & chemical irritation. | 50-75% | Mild; best for small spider veins; less pigmentation; injection can be painful. |
Procedure: Steps & Aftercare - Injection & Instructions
- Pre-Procedure:
- Clinical assessment, Duplex USG mapping.
- Informed consent obtained.
- Aseptic skin preparation.
- Injection Technique:
- Sclerosants: Polidocanol (POL), Sodium Tetradecyl Sulfate (STS). Concentrations vary by vein size.
- Foam preparation (Tessari method: 1 part liquid sclerosant + 4 parts air/CO₂).
- Fine needle (27-30G). Inject small volumes (0.1-0.5 mL per site).
- Technique: Slow injection, observe for vein blanching.
⭐ Foam sclerotherapy (e.g., Tessari method: 1 part sclerosant + 4 parts air) significantly increases surface area contact and efficacy, allowing lower sclerosant volumes compared to liquid form.
- Post-Procedure & Aftercare:
- Immediate: Compression pads/bandages over injection sites.
- Ambulation encouraged immediately post-procedure.
- Compression therapy: Graduated stockings (Class II: 20-30 mmHg) for 2-3 weeks (first 24-72h continuously).
- Avoid: Sun exposure, hot baths, strenuous exercise for 1-2 weeks.
- Follow-up: Typically at 2-4 weeks for assessment.

Adverse Effects & No-Gos - Safety Net Snippets
- Common:
- Hyperpigmentation (hemosiderin; fades), bruising, pain
- Telangiectatic matting, localized urticaria
- Rare/Serious:
- DVT/PE (<1%), anaphylaxis
- Tissue necrosis/ulceration (extravasation, arterial injection)
- Nerve damage (transient sensory)
- Stroke/TIA (PFO + foam), visual disturbances
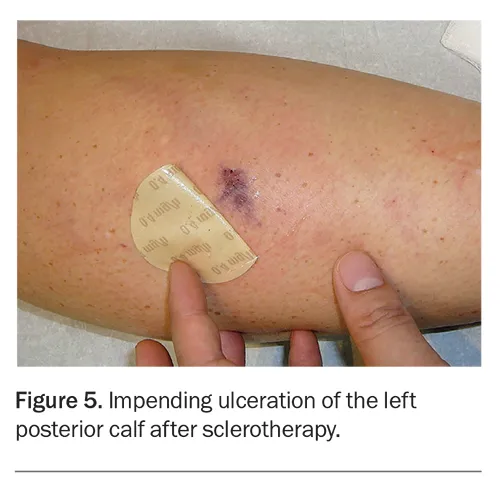
- Absolute Contraindications:
- Sclerosant allergy, acute DVT/PE/thrombophlebitis
- Pregnancy (most Cat C)
- Severe arterial disease (ABI <0.8), acute local infection
- Immobility
- Relative Contraindications:
- Breastfeeding, hypercoagulable states
- Poorly controlled systemic illness (DM)
- History DVT/PE, significant edema, known PFO (foam)
⭐ Hyperpigmentation is the most common adverse effect (up to 30%), often from hemosiderin deposition, increased with higher sclerosant concentration or extravasation.
High‑Yield Points - ⚡ Biggest Takeaways
- Sclerotherapy induces endothelial damage, fibrosis, and eventual vessel occlusion.
- Common sclerosants: Polidocanol (detergent, less pain), Sodium Tetradecyl Sulfate (STS), hypertonic saline.
- Indicated for telangiectasias (spider veins), small varicose veins, and reticular veins.
- Key contraindications: Pregnancy, acute DVT/PE, significant arterial insufficiency, known sclerosant allergy.
- Most common complication: post-inflammatory hyperpigmentation; others include telangiectatic matting, skin necrosis, allergic reactions.
- Compression therapy post-procedure is crucial for optimal results and minimizing complications like DVT_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

