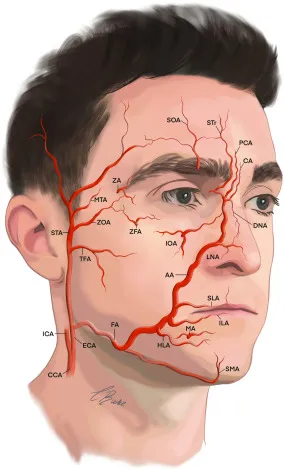
Dermal Fillers - Puffy Problems & Pinpoint Fixes
- Early Complications (<2 wks):
- Common: Erythema, edema, pain, bruising (resolve spontaneously).
- Tyndall effect: Bluish hue with superficial Hyaluronic Acid (HA) fillers.
- Nodules: Inflammatory or non-inflammatory lumps.
- ⚠️ Vascular Occlusion (VO): Critical! Signs: immediate pain, blanching, livedo reticularis, dusky discoloration. EMERGENCY!
- Delayed Complications (>2 wks):
- Granulomas (foreign body reaction), biofilms (persistent infection), filler migration.
- Management Highlights:
- Tyndall effect: Hyaluronidase (10-30 IU).
- Nodules (HA): Massage; if persistent, hyaluronidase.
- Granulomas: Intralesional steroids (e.g., Triamcinolone 5-10 mg/mL), 5-FU.
- VO (HA Fillers): 📌 H.A.R.M.E.D. protocol: Hyaluronidase (high dose, e.g., 150-1500 IU, repeat until reperfusion), Aspirin (325 mg), Refer (ophthalmology if vision changes), Massage, Elevate (controversial), Dilators (topical nitroglycerin). Warm compress.
⭐ Immediate, aggressive high-dose hyaluronidase is the cornerstone for managing HA filler-induced vascular occlusion to prevent tissue necrosis or blindness.
Neurotoxins - Frozen Frowns & Fixes
BoNT blocks ACh release → muscle paralysis. Effects: 3-4 months.
- Common Complications & Management:
- Overcorrection (Frozen look, Spock brow):
- Spock brow: Micro-BoNT to lateral frontalis.
- Undercorrection/Asymmetry: Touch-up after 2 weeks.
- Ptosis (eyelid droop):
- Common significant issue.
- Rx: Apraclonidine 0.5% / Phenylephrine 2.5% drops (Müller's muscle).
- Resolves spontaneously.
- Diffusion: Diplopia, dysphagia (rare, supportive).
- Injection site: Pain, bruising (cold compress), headache.
- Overcorrection (Frozen look, Spock brow):
- Prevention:
- Precise anatomy, dose, placement.
- Avoid levator palpebrae proximity.

⭐ Ptosis post-glabellar BoNT: due to levator palpebrae superioris diffusion. Rx: apraclonidine 0.5% drops.
Energy Devices - Zap Traps & Zap-Backs
- Common Complications (Zap Traps) & Management (Zap-Backs):
- Thermal Injury (Burns): Superficial/deep. Manage with immediate cooling, emollients, topical antibiotics (e.g., mupirocin), non-adherent dressings.
- Pigmentary Changes:
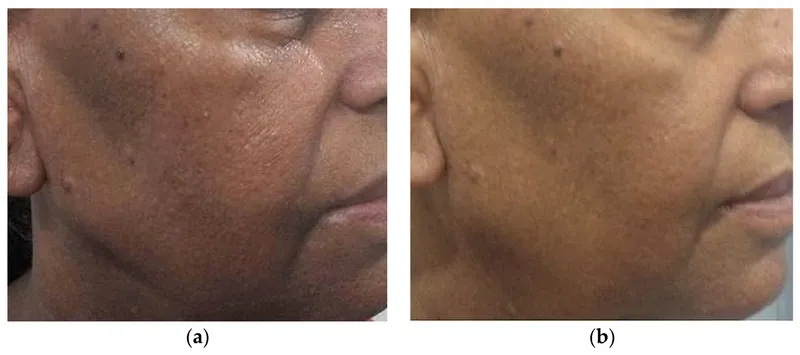
- Post-Inflammatory Hyperpigmentation (PIH): Frequent in Indian skin (Fitzpatrick types IV-VI). Strict sun protection (SPF >30), hydroquinone 2-4%, topical retinoids, azelaic acid, low-fluence Q-switched Nd:YAG laser.
- Hypopigmentation: Often delayed, challenging. Options: topical corticosteroids (if inflammatory), excimer laser (308 nm), targeted phototherapy, microneedling, medical tattooing (camouflage).
- Scarring (Atrophic, Hypertrophic): Silicone gel/sheets, intralesional triamcinolone acetonide (10-40 mg/mL), fractional lasers (ablative/non-ablative), pulsed dye laser for erythematous scars.
- Infection: Herpes simplex virus (HSV) reactivation common with perioral/full-face resurfacing. Prophylactic antivirals (e.g., acyclovir 400 mg BID) starting 1 day prior.
- Ocular Injury: Corneal/retinal damage. Mandatory, wavelength-specific eye protection for patient & operator.
- Paradoxical Hypertrichosis: ↑ finer hair growth post-laser hair removal. Adjust fluence, spot size, cooling; consider longer pulse durations.
⭐ For Fitzpatrick skin types IV-VI, always prioritize longer wavelengths (e.g., Nd:YAG 1064 nm, Diode 810 nm) and effective epidermal cooling during laser procedures to minimize risk of PIH and burns.
Peels & Needles - Surface Setbacks & Solutions
- Chemical Peels:
- Complications: PIH (most common, esp. darker skin), infection (HSV reactivation), scarring (esp. deep peels), persistent erythema, allergic contact dermatitis, milia.
- Management: Strict photoprotection (PIH), prophylactic antivirals (HSV risk), topical steroids/silicone (scars), gentle cleansers.
- Microneedling:
- Complications: Common: transient erythema, edema, petechiae. Rare: infection (bacterial/fungal), granulomas, PIH, tram-track scarring (improper technique/pressure).
- Management: Cool compresses, topical antibiotics (if infection), sun avoidance, proper technique.
⭐ Prophylactic acyclovir is recommended for patients with a history of herpes simplex undergoing facial peels to prevent reactivation.
High‑Yield Points - ⚡ Biggest Takeaways
- Filler vascular occlusion: EMERGENCY. Management: High-dose hyaluronidase, warm compress, massage.
- Botulinum toxin: Eyelid ptosis (most common), eyebrow asymmetry. Management: Apraclonidine drops for ptosis.
- Lasers/Chemical Peels: Post-Inflammatory Hyperpigmentation (PIH) especially in darker skin types (Fitzpatrick IV-VI).
- Infections: Herpetic reactivation (prophylaxis for ablative procedures), bacterial cellulitis.
- Granulomas/Nodules: Delayed hypersensitivity to fillers; manage with IL steroids, 5-FU, or excision.
- Tyndall Effect: Bluish discoloration from superficial HA filler placement; treat with hyaluronidase.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

