Cosmeceuticals - Skin Deep Science
- Products bridging cosmetics & pharmaceuticals.
- Aim: Enhance skin appearance & provide therapeutic benefits.
⭐ Cosmeceuticals are defined as products with both cosmetic and therapeutic (drug-like) effects, intended to affect skin structure or function.
Comparison: Cosmetics vs. Cosmeceuticals vs. Drugs
| Feature | Cosmetics | Cosmeceuticals | Drugs |
|---|---|---|---|
| Goal | Appearance enhancement | Appearance & physiological benefit | Disease treatment/prevention |
| Action | Surface action | Affects skin structure/function | Alters physiological processes |
| Regulation (India) | D&C Act (as cosmetics) | Often under cosmetic rules; "Quasi-drugs" elsewhere | Strict (CDSCO); clinical trials needed |
- Regulation: In India, largely under cosmetics (Drugs and Cosmetics Act, 1940). No separate legal category for cosmeceuticals.
Cosmeceuticals - Powerhouse Potions
Cosmeceuticals: Bioactive topicals; cosmetic & therapeutic effects.
- Retinoids: Vit A derivatives.
- Mech: Bind RARs. ↑Cell turnover, ↑collagen.
- Tretinoin (0.025%, 0.05%, 0.1% Rx)
- Adapalene (0.1%, 0.3% OTC/Rx)
- Tazarotene (0.05%, 0.1% Rx)
- Retinol, Retinaldehyde (OTC)
- Uses: Acne, photoaging, pigment.
- S/E: 📌 RED BUMPS (Redness, Edema, Dryness, Burning, Urticaria, Peeling, Photosensitivity, Pruritus).
- Vitamin C (L-Ascorbic Acid):
- Antioxidant, photoprotective, ↑collagen.
- Conc: 10-20%.
- Hydroxy Acids:
- AHAs (Glycolic, Lactic): Exfoliate; texture, pigment.
- BHAs (Salicylic): Lipophilic; pores, acne.
- Niacinamide (Vit B3):
- Anti-inflam, barrier repair, sebum.
- Peptides:
- Signal for collagen, elastin.
⭐ Topical tretinoin (all-trans retinoic acid) is a first-generation retinoid, highly effective for acne and photoaging by binding to all RAR subtypes (α, β, γ).
Cosmeceuticals - Shield & Soothe
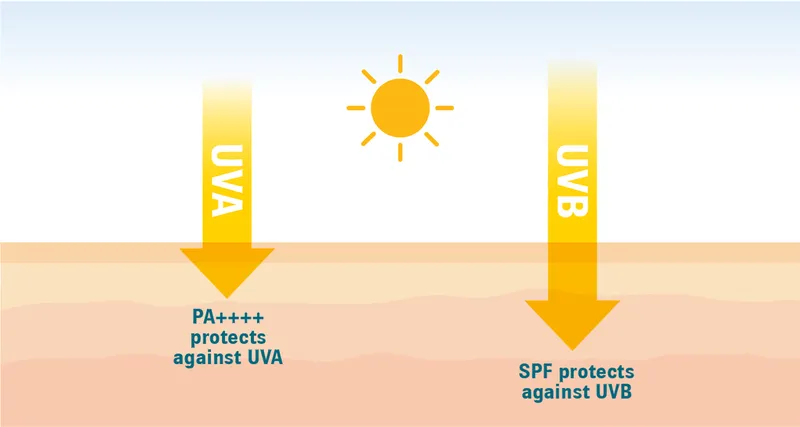
- Sunscreens: Essential for UV protection.
- Physical: Zinc oxide, titanium dioxide. Reflect/scatter UV. Better for sensitive skin.
- Chemical: Oxybenzone, avobenzone. Absorb UV, convert to heat.
- Aim for SPF 30-50, PA+++/++++, broad-spectrum.
⭐ Physical sunscreens like zinc oxide and titanium dioxide work by reflecting and scattering UV radiation and are generally better tolerated by sensitive skin than chemical sunscreens.
- Moisturizers: Hydrate & repair skin barrier.
- Humectants: Glycerin, hyaluronic acid (attract water).
- Emollients: Ceramides, dimethicone (smooth skin).
- Occlusives: Petrolatum, lanolin (prevent water loss).
- Other Antioxidants: Combat free radicals.
- Vitamin C (L-ascorbic acid): Collagen synthesis, photoprotection.
- Vitamin E (Tocopherol): Synergistic with Vit C.
- Niacinamide: Anti-inflammatory, barrier repair.
- Depigmenting Agents: Target hyperpigmentation.
- Hydroquinone: 2-4% (Tyrosinase inhibitor).
- Kojic acid, Azelaic acid, Arbutin: Milder alternatives.
- Retinoids: Increase cell turnover, reduce pigment transfer (e.g., Tretinoin 0.025-0.1%).
Cosmeceuticals - Smart Skin Solutions
Cosmeceuticals: Active ingredients bridging cosmetics & pharmaceuticals for targeted skin concerns.
- Common Applications:
- Acne:
- Exfoliants: Salicylic acid (BHA), AHAs (glycolic).
- Antimicrobials: Benzoyl peroxide.
- Cell regulators: Topical retinoids.
- Anti-inflammatory: Niacinamide.
- Aging:
- Collagen boosters: Retinoids, Vitamin C (L-ascorbic acid), Peptides.
- Antioxidants: Vitamin E, Ferulic acid.
- Hydrators: Hyaluronic acid.
- Hyperpigmentation:
- Tyrosinase inhibitors: Hydroquinone (2-4%), Kojic acid, Arbutin.
- Others: Azelaic acid, Vitamin C, Niacinamide.
- Acne:
⭐ The 'Retinoid Sandwich' method (moisturizer → retinoid → moisturizer) can significantly improve tolerability of topical retinoids, especially in sensitive skin or during initial use.
📌 Always counsel on sunscreen (SPF 30+) with photosensitizing agents like retinoids, AHAs.
High‑Yield Points - ⚡ Biggest Takeaways
- Retinoids (e.g., Tretinoin) are key for anti-aging and acne via RAR/RXR agonism.
- Vitamin C (L-Ascorbic Acid) is a vital antioxidant for collagen synthesis and skin brightening.
- AHAs (e.g., Glycolic acid) exfoliate, improving skin texture; BHAs (e.g., Salicylic acid) target oily pores and acne.
- Niacinamide offers anti-inflammatory, barrier repair, and pigment reduction benefits.
- Sunscreens with broad-spectrum (UVA/UVB) and SPF ≥30 are essential for photoprotection.
- Hyaluronic Acid is a potent humectant for skin hydration.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

