Pathophysiology & Scar Types - Scar Stories
- Pathophysiology: Chronic inflammation in acne → abnormal wound healing.
- Imbalance: ↑Matrix Metalloproteinases (MMPs) vs. ↓Tissue Inhibitors of Metalloproteinases (TIMPs) → collagen dysregulation.
- Risk factors: Acne severity, duration, manipulation, genetics.
- Scar Types:
- Atrophic (most common): Net collagen loss. 📌 Mnemonic: "RIB" for types.
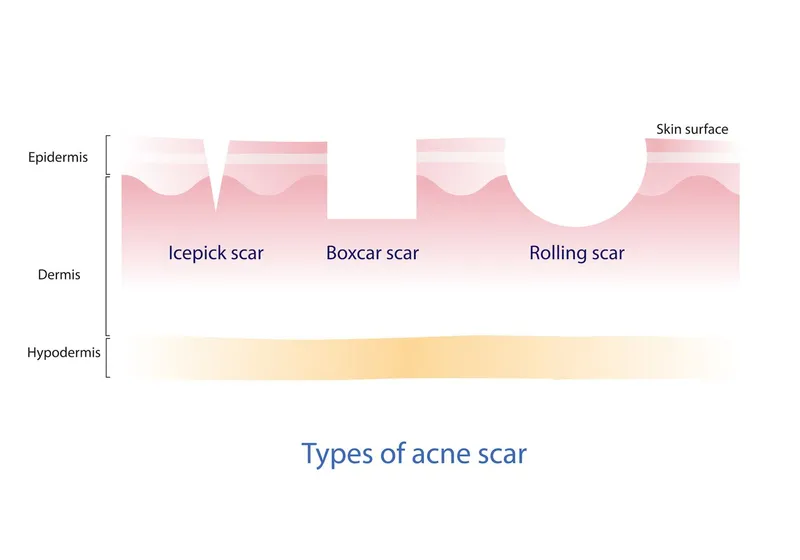
- Icepick: Narrow (<2 mm), deep, V-shaped pits.
- Boxcar: Wider (1.5-4 mm), sharp vertical edges, U-shaped.
- Rolling: Broad (>4-5 mm), undulating, M-shaped, dermal tethering.
- Hypertrophic: Raised, firm, pink/red; remain within original wound margins.
- Keloidal: Raised, rubbery, often symptomatic (itch/pain); extend beyond original wound margins.
 )
)
- Atrophic (most common): Net collagen loss. 📌 Mnemonic: "RIB" for types.
⭐ Atrophic scars (icepick, boxcar, rolling) are the most common type of acne scars, resulting from dermal collagen loss.
Scar Assessment & Prevention - Scene Investigation
- Primary Prevention: Paramount. Focus on minimizing development of disfiguring long-term scarring.
⭐ The most crucial step in preventing acne scarring is early and effective treatment of active acne lesions.
- Strictly avoid manipulating active acne lesions (e.g., picking, squeezing).
- Scar Assessment Protocol:
- Grading Systems:
- Goodman & Baron: Qualitative (Grade 1-4, assessing scar type and severity).
- ECCA Scale: Quantitative, objective score for overall acne scar severity.
- Clinical Description: Thoroughly note scar morphology (icepick, boxcar, rolling, hypertrophic/keloid), precise depth, and anatomical distribution.
- Grading Systems:
Atrophic Scar Treatments - Filling the Gaps
Focus: Restoring volume, stimulating collagen.
-
General Principles: Combination therapy often best for optimal results. Patient selection, managing expectations crucial.
-
Treatment Modalities by Scar Type:
Scar Type Key Treatments Notes Icepick TCA CROSS ($TCA \textbf{70-100}%$), Punch Excision Deep, narrow (<2mm) epithelial tracts; V-shaped. Boxcar Fractional Lasers (CO2, Er:YAG), Punch Excision/Elevation, MNRF Wider (1.5-4mm), round/oval with sharp vertical edges. Rolling Subcision (esp. tethered), Dermal Fillers (HA), MNRF, Fractional Lasers Wider (>4mm), undulating, M-shaped due to dermal tethering. ⭐ TCA CROSS (Chemical Reconstruction Of Skin Scars) is highly effective for icepick scars, utilizing high concentration trichloroacetic acid.
-
Other Options:
- Dermal Fillers: Hyaluronic Acid (HA), autologous fat. Provide immediate but temporary volume.
- Microneedling: Induces collagen via controlled micro-injury. Multiple sessions required.
- Platelet-Rich Plasma (PRP): Adjunctive to other procedures, enhances healing and results.
Hypertrophic/Keloidal Scar Treatments - Calming Overgrowth
- Goal: Flatten scars, reduce symptoms (pain, itch), improve cosmesis.
- First-Line Therapy:
⭐ Intralesional corticosteroids (e.g., triamcinolone acetonide 10-40 mg/mL) are first-line therapy for hypertrophic and keloidal acne scars.
- Triamcinolone acetonide (TAC) $TAC \textbf{10-40 mg/mL}$ every 4-6 weeks.
- Mechanism: ↓inflammation, ↓collagen synthesis, ↓fibroblast proliferation.
- Second-Line/Adjunctive Treatments:
- Silicone Gel Sheeting/Ointments: Applied 12-24 hrs/day for months. ↑Hydration, ↓collagen.
- Intralesional 5-Fluorouracil (5-FU): 50 mg/mL, often with TAC. For resistant/thick keloids.
- Cryotherapy: Often combined with ILCS (cryo before injection enhances penetration).
- Pressure Therapy: E.g., pressure earrings. Requires >24 mmHg for 6-12 months.
- Other Options (Resistant/Combination):
- Surgical Excision: High recurrence alone; combine with adjuvant (e.g., ILCS post-op, radiotherapy).
- Lasers: Pulsed Dye Laser (PDL) for erythema; CO2/Erbium for debulking (cautious use).
- Intralesional Verapamil, Bleomycin.
High‑Yield Points - ⚡ Biggest Takeaways
- Acne scarring, a common sequela, significantly impacts quality of life.
- Main types: atrophic (icepick, boxcar, rolling) and hypertrophic/keloidal.
- Icepick scars: narrow, deep; treated with TCA CROSS (Chemical Reconstruction Of Skin Scars).
- Boxcar scars: wider, sharp edges; managed by punch techniques, subcision, lasers.
- Rolling scars: broad, sloping edges; subcision, microneedling, fillers are effective.
- Hypertrophic/keloidal scars: common on trunk; use intralesional steroids, silicone sheets.
- Early, effective acne treatment is key to prevent scarring; isotretinoin can prevent new lesions and subsequent scarring but does not treat existing scars directly during therapy initiation for severe acne.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

