Neonatal & Infantile Acne - Tiny Pimple Tales
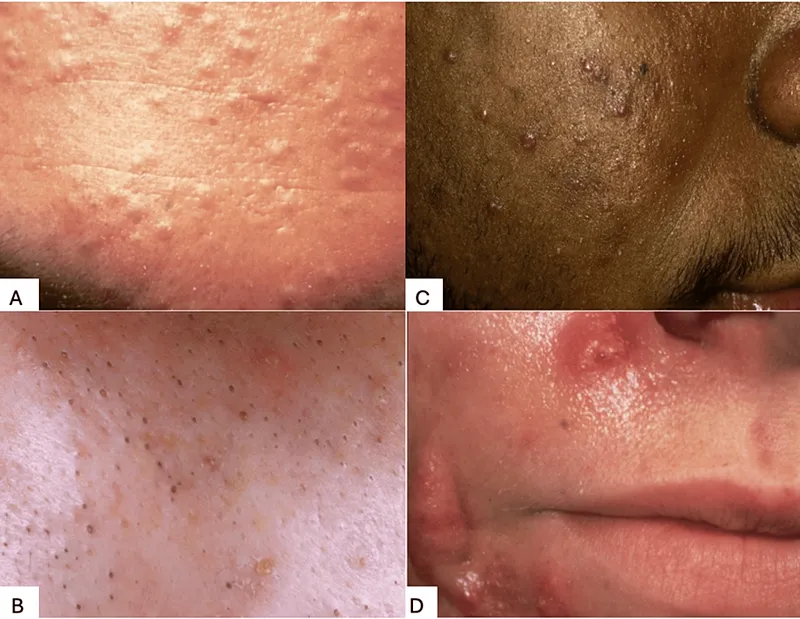
- Neonatal Acne
- Onset: Birth to 6 weeks.
- Etiology: Maternal androgens; Malassezia spp. involvement.
- Lesions: Inflammatory papules/pustules; NO comedones. Face, scalp.
- Course: Usually self-resolves; minimal scarring.
- Tx: Gentle cleansing; topical ketoconazole if needed.
- Infantile Acne
- Onset: 6 weeks to 12 months.
- Etiology: Endogenous androgens (infant's ↑ DHEA-S).
- Lesions: Comedones (key feature!), papules, pustules, nodules.
- Course: More persistent; higher risk of scarring.
- Tx: Topical benzoyl peroxide, retinoids. Oral antibiotics if severe.
⭐ Infantile acne features comedones, has a higher scarring risk than neonatal acne, and may predict more severe adolescent acne.
Acne in Pregnancy & Lactation - Safe Bump Care
- Goal: Safe symptom control, prioritizing fetal/neonatal well-being.
- Safe Topical Options (Pregnancy Category):
- Azelaic acid (B)
- Benzoyl peroxide (C, limited use)
- Clindamycin (B)
- Erythromycin (B)
- Glycolic acid (low conc., AHA)
- Safe Systemic Options (Severe Cases, Pregnancy Category):
- Oral Erythromycin (B)
- Cephalexin (B)
- Zinc
- ⚠️ Strictly Avoid (Teratogenic/Adverse Effects):
- Topical: All Retinoids (Tretinoin, Adapalene, Tazarotene)
- Systemic:
- Oral Isotretinoin (Absolute contraindication, Cat X)
- Tetracyclines (e.g., Doxycycline, Minocycline - Cat D)
- Hormonal therapies (Spironolactone, OCPs)
- Lactation:
- Most topicals generally safe.
- Systemic: Erythromycin considered safe; others with caution.
⭐ Oral isotretinoin (Cat X) is absolutely contraindicated in pregnancy due to severe teratogenicity.
PCOS & Hormonal Acne - Endocrine Eruptions
- PCOS: Key cause. Features: irregular menses, hirsutism, acne.
- Rotterdam criteria (2 of 3): Oligo/anovulation, hyperandrogenism (clinical/biochemical), polycystic ovaries on USG.
- Acne: Mandibular, persistent, perimenstrual flares.
- Hormonal Acne Pattern: "U-zone" (jawline, chin, neck).
- Associated: SAHA syndrome (Seborrhea, Acne, Hirsutism, Alopecia).
- Workup:
- Hormones: Testosterone (total/free), DHEAS, LH/FSH.
- Pelvic USG.
- Management Principles:
- Target androgens: OCPs (e.g., ethinylestradiol + drospirenone/cyproterone acetate).
- Anti-androgen: Spironolactone (50-100 mg/day, max 200 mg). ⚠️ Monitor K+.
- Insulin resistance: Metformin.
- Standard acne therapies as adjuncts.
⭐ Spironolactone is particularly effective for adult female acne with jawline distribution and premenstrual flares.
Drug-Induced & Occupational Acne - Triggered Breakouts
- Drug-Induced Acne (Acne Medicamentosa):
- Sudden onset, monomorphic lesions (papulopustules, few comedones).
- Often on trunk, upper arms.
- Causative Drugs (📌 "PIMPLES"):
- Phenytoin
- Isoniazid, Iodides
- Medications like antiepileptics (Carbamazepine - not fitting M well, but often grouped)
- Puromycins, Protease inhibitors
- Lithium
- EGFR inhibitors (e.g., Cetuximab), Epidermal growth factor receptor inhibitors
- Steroids (systemic/topical), Androgens, Anabolic steroids, ACTH.
- Others: Halogens (bromides, iodides), high-dose Vit B2, B6, B12, Dactinomycin.
- Occupational Acne:
- Exposure to insoluble, follicle-occluding substances.
- Chloracne: From halogenated aromatic hydrocarbons (e.g., dioxins, PCBs). Presents with straw-colored cysts, open/closed comedones; typically retroauricular, malar, axillary, groin.
- Oil Acne: Cutting oils, petroleum products. Comedones, inflammatory papules on exposed areas (forearms, thighs).
- Tar Acne: Coal tar derivatives. Comedones, folliculitis.
- Acne Mechanica: Due to friction/pressure (e.g., helmets, straps).
⭐ Chloracne is a severe form of acne caused by exposure to halogenated aromatic compounds (like dioxins) and is characterized by numerous open comedones and straw-colored cysts, often resistant to therapy.

High‑Yield Points - ⚡ Biggest Takeaways
- Neonatal acne: Onset 2-4 weeks, comedones absent, typically self-resolving.
- Infantile acne: Begins 3-6 months, comedones present, may scar; consider endocrine workup if severe.
- Acne in pregnancy: Topical azelaic acid, benzoyl peroxide are safer. Strictly avoid retinoids, tetracyclines.
- Steroid acne: Monomorphic papulopustules, no comedones, follows steroid use.
- Acne fulminans: Severe, ulcerative acne with systemic symptoms (fever, arthralgia); requires systemic steroids first.
- Drug-induced acne: Often monomorphic, caused by steroids, lithium, phenytoin, isoniazid, EGFR inhibitors.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

