Acne and Related Disorders

On this page
🎯 The Acne Arsenal: Mastering Dermatology's Most Common Battlefield
Acne affects nearly every patient you'll encounter, yet its deceptively simple appearance masks a complex interplay of sebaceous gland biology, microbial ecology, and immune dysregulation. You'll master how follicular obstruction triggers Cutibacterium acnes proliferation and inflammatory cascades, then learn to distinguish comedonal from cystic presentations and match each phenotype to evidence-based treatments-from retinoids that normalize keratinization to antibiotics targeting bacterial overgrowth. By integrating pathophysiology with clinical pattern recognition, you'll transform acne from a cosmetic nuisance into a treatable disease you can confidently manage.
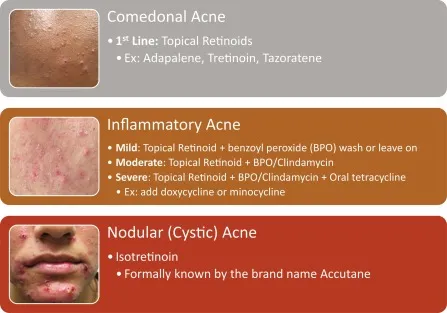
Acne vulgaris affects 85% of adolescents and 40% of adults, making it dermatology's most prevalent condition. Understanding acne's multifactorial pathogenesis - from pilosebaceous unit dysfunction to inflammatory cascades - provides the foundation for targeted therapeutic interventions that achieve 90%+ improvement rates when properly implemented.
📌 Remember: PASH - Pilosebaceous unit dysfunction, Androgen sensitivity, Sebum hypersecretion, Hyperkeratinization. These four pillars drive every acne presentation, with Cutibacterium acnes amplifying inflammation through TLR-2 activation and IL-1β upregulation.
The acne spectrum encompasses 12 distinct clinical variants, from simple comedonal presentations to severe nodulocystic disease requiring systemic intervention. Each variant demands specific therapeutic approaches, with treatment success rates varying from 70-95% depending on severity, patient compliance, and combination therapy protocols.
| Acne Severity | Lesion Count | Inflammatory Component | First-Line Treatment | Success Rate | Timeline |
|---|---|---|---|---|---|
| Mild Comedonal | <20 lesions | Minimal | Topical retinoids | 85-90% | 8-12 weeks |
| Moderate Papular | 20-50 lesions | Moderate | Combination therapy | 80-85% | 12-16 weeks |
| Severe Nodular | >50 lesions | Extensive | Systemic + topical | 75-80% | 16-24 weeks |
| Nodulocystic | >100 lesions | Severe | Isotretinoin | 90-95% | 20-24 weeks |
| Acne Fulminans | Confluent | Systemic | Steroids + isotretinoin | 70-75% | 24-36 weeks |
- Hormonal Influences: Androgens increase sebum production by 500% during puberty
- DHT binding to sebocyte receptors triggers 5α-reductase upregulation
- DHEA-S levels correlate with acne severity (r=0.73, p<0.001)
- Late-onset acne (>25 years) suggests PCOS in 40% of women
- Inflammatory Cascade: C. acnes triggers TLR-2/4 activation
- IL-1β levels increase 15-fold in inflammatory lesions
- TNF-α upregulation drives comedone rupture and scarring
- Biofilm formation reduces antibiotic efficacy by 80%
💡 Master This: Acne pathogenesis follows the "Four-Factor Model" - follicular hyperkeratinization creates microcomedones, androgen-stimulated sebum provides bacterial nutrients, C. acnes proliferation triggers inflammation, and immune dysregulation perpetuates the cycle. Breaking any component interrupts the entire cascade.
Understanding acne's complex interplay between genetics, hormones, and environmental factors enables precision medicine approaches that target specific pathogenic mechanisms, setting the foundation for exploring how pilosebaceous unit dysfunction initiates the inflammatory cascade.
🎯 The Acne Arsenal: Mastering Dermatology's Most Common Battlefield
🔬 Pilosebaceous Powerhouse: The Acne Engine Room
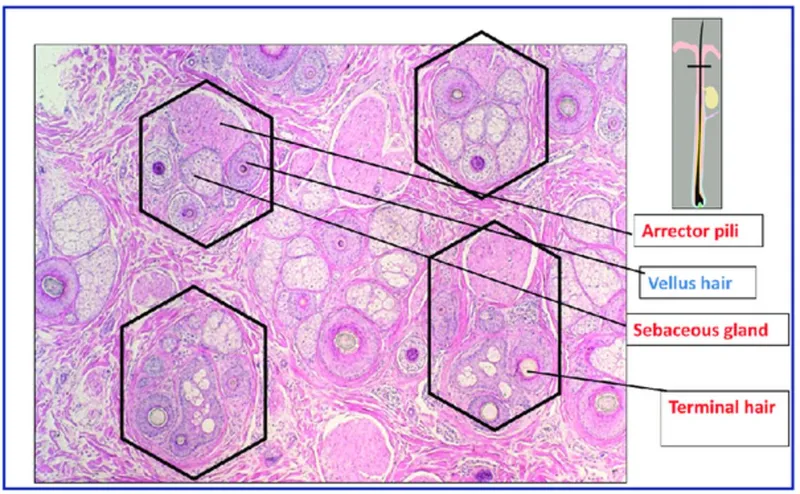
The pilosebaceous unit represents acne's ground zero, where 4 critical pathogenic processes converge to create the perfect inflammatory storm. Each unit contains 2-6 sebaceous lobules producing 1-2mg sebum daily, with androgen receptors concentrated 10-fold higher than surrounding tissue, explaining acne's predilection for face, chest, and back regions.
📌 Remember: FISH - Follicular hyperkeratinization, Increased sebum production, Sbacterial proliferation, Host inflammatory response. These sequential events create the pathogenic cascade, with each step amplifying the next through positive feedback loops.
Follicular hyperkeratinization initiates acne development through abnormal keratinocyte differentiation and reduced desquamation. Normal follicular turnover occurs every 14 days, but acne-prone follicles show 50% reduced shedding with 3-fold increased keratin production, creating the microcomedone foundation for all subsequent lesions.
| Process | Normal State | Acne-Prone State | Key Mediators | Clinical Impact |
|---|---|---|---|---|
| Keratinocyte Turnover | 14 days | 21-28 days | Retinoids, AHA | Microcomedone formation |
| Sebum Production | 1-2mg/day | 3-8mg/day | Androgens, IGF-1 | Bacterial proliferation |
| Desquamation | Regular shedding | 50% reduction | Salicylic acid | Pore obstruction |
| Inflammation | Minimal | 15-fold ↑ IL-1β | Antibiotics, steroids | Lesion progression |
| Bacterial Load | 10³ CFU/follicle | 10⁶ CFU/follicle | Antimicrobials | Biofilm formation |
- Sebaceous Gland Hyperplasia: Androgen stimulation increases gland size by 200-400%
- 5α-reductase activity converts testosterone to potent DHT
- Sebocyte proliferation rate increases 5-fold during puberty
- Sebum composition changes: increased squalene (40% vs 25% normal)
- Linoleic acid deficiency (<15% vs 25% normal) impairs barrier function
- Comedogenesis Mechanism: Abnormal keratinization creates follicular plugs
- Corneocyte cohesion increases 3-fold in acne-prone follicles
- Reduced filaggrin expression impairs normal desquamation
- Microcomedones form 2-4 weeks before visible lesions appear
⭐ Clinical Pearl: Microcomedones represent acne's earliest detectable change, appearing 2-4 weeks before clinical lesions. Dermoscopy reveals these 0.1-0.3mm structures in 90% of acne-prone patients, explaining why effective treatment requires 8-12 weeks to show visible improvement.
💡 Master This: The pilosebaceous unit functions as an integrated endocrine organ responding to systemic hormonal signals while maintaining local inflammatory control. Disruption of this delicate balance through androgen excess, barrier dysfunction, or microbial dysbiosis triggers the pathogenic cascade that transforms normal follicles into inflammatory lesions.
The pilosebaceous unit's complex regulatory mechanisms set the stage for understanding how Cutibacterium acnes exploits this disrupted environment to establish pathogenic biofilms and trigger the immune responses that define inflammatory acne presentations.
🔬 Pilosebaceous Powerhouse: The Acne Engine Room
🦠 Cutibacterium Chronicles: The Bacterial Battlefield
📌 Remember: BITE - Biofilm formation, Immune activation, Toxin production, Enzymatic tissue damage. C. acnes pathogenicity depends on these four mechanisms, with biofilm-embedded bacteria showing 1000-fold increased antibiotic resistance compared to planktonic forms.
The transition from commensal to pathogenic C. acnes involves sophisticated molecular mechanisms that exploit the altered follicular environment. Biofilm formation occurs within 24-48 hours of follicular obstruction, creating 3D bacterial communities protected by extracellular polymeric substances that reduce antimicrobial penetration by 90%.
| Phylotype | Acne Association | Virulence Factors | Antibiotic Resistance | Clinical Significance |
|---|---|---|---|---|
| IA1 | High (80% inflammatory) | CAMP factor, lipases | Moderate-High | Primary inflammatory driver |
| IA2 | Moderate (60% lesions) | Hyaluronidase | Moderate | Secondary inflammatory role |
| IB | Low (30% lesions) | Limited virulence | Low-Moderate | Opportunistic pathogen |
| IC | Variable (40% lesions) | Sialidase, proteases | Low | Geographic variation |
| II | Protective (10% lesions) | Anti-inflammatory | Minimal | Commensal protection |
- Surface layer: Metabolically active, antibiotic-sensitive
- Middle zone: Reduced metabolism, moderate resistance
- Deep core: Dormant persister cells, 1000x antibiotic resistance
- Quorum sensing coordinates biofilm maturation via autoinducer-2
- Virulence Factor Expression: Strain-specific pathogenic mechanisms
- CAMP factor: Synergistic hemolysis, immune cell activation
- Lipases: Sebum degradation, free fatty acid production
- Hyaluronidase: Tissue penetration, spreading factor
- Sialidase: Mucin degradation, epithelial barrier disruption
⭐ Clinical Pearl: Antibiotic resistance in C. acnes has increased 10-fold over 20 years, with 60% of strains showing resistance to clindamycin and 40% to erythromycin. Combination therapy with benzoyl peroxide reduces resistance development by 95% through oxidative bacterial killing that prevents resistance gene expression.
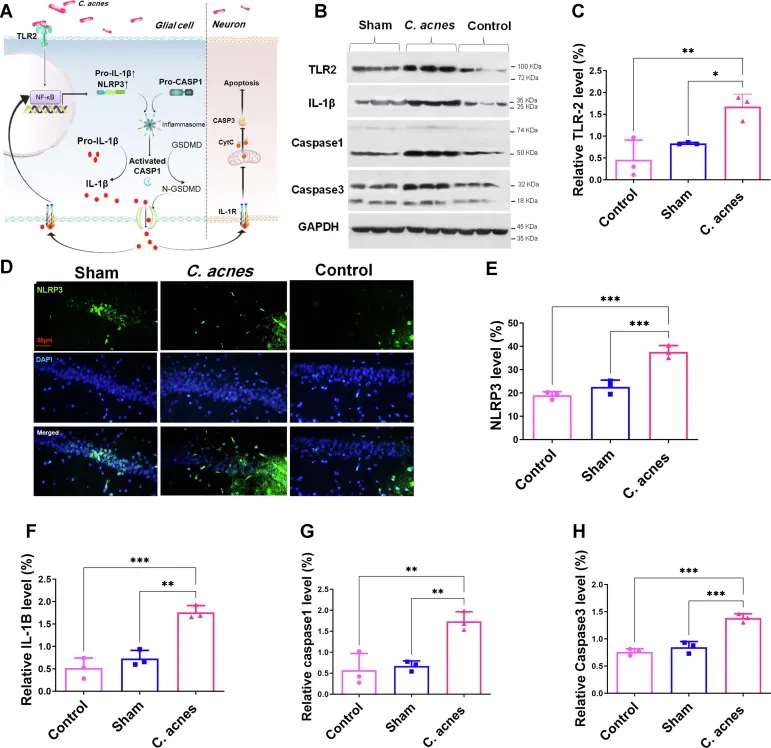
💡 Master This: C. acnes pathogenicity results from strain-specific virulence factors interacting with host immune dysfunction rather than simple bacterial overgrowth. Understanding phylotype differences enables precision antimicrobial therapy targeting pathogenic strains while preserving protective commensal populations that maintain follicular homeostasis.
The complex interplay between C. acnes virulence and host immunity creates the foundation for understanding how inflammatory cascades transform localized bacterial colonization into the diverse clinical presentations that characterize acne's broad spectrum of severity and morphology.
🦠 Cutibacterium Chronicles: The Bacterial Battlefield
🔥 Inflammatory Inferno: The Immune System's Acne Response
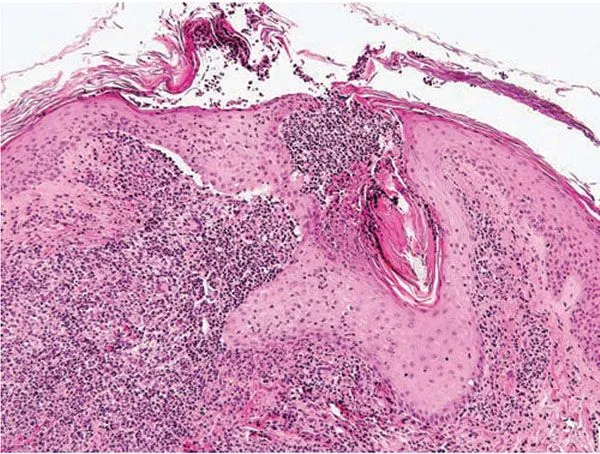
The inflammatory response in acne involves complex immune cascades triggered by multiple stimuli including bacterial antigens, sebum components, and follicular rupture. Toll-like receptor activation initiates inflammatory signaling within minutes, leading to 15-fold increases in IL-1β, 10-fold increases in TNF-α, and sustained elevation of inflammatory markers for weeks to months.
📌 Remember: FIRE - Follicular rupture, Innate immunity activation, Recruited inflammatory cells, Effector molecule release. This sequence transforms sterile comedones into inflammatory lesions, with neutrophil infiltration occurring within 6-12 hours and lymphocyte recruitment following within 24-48 hours.
Pattern recognition receptors (PRRs) serve as the immune system's early warning system, detecting both pathogen-associated molecular patterns (PAMPs) from C. acnes and damage-associated molecular patterns (DAMPs) from follicular disruption. TLR-2 expression increases 5-fold in acne lesions, while TLR-4 activation by lipopolysaccharides drives sustained inflammatory responses.
| Inflammatory Phase | Timeline | Key Mediators | Cellular Response | Clinical Manifestation |
|---|---|---|---|---|
| Initiation | 0-6 hours | IL-1β, TNF-α | Keratinocyte activation | Erythema, warmth |
| Amplification | 6-24 hours | IL-8, CXCL1 | Neutrophil recruitment | Pustule formation |
| Propagation | 1-7 days | IL-17, IFN-γ | T-cell activation | Papule development |
| Resolution | 1-4 weeks | IL-10, TGF-β | Macrophage clearance | Healing vs scarring |
| Chronic | >4 weeks | IL-6, IL-23 | Persistent inflammation | Nodule/cyst formation |
- Complement activation via alternative pathway increases C3a/C5a by 8-fold
- Neutrophil degranulation releases elastase and myeloperoxidase
- Mast cell activation increases histamine and leukotriene release
- Sebocyte TLR-2 expression increases 300% in inflammatory lesions
- Adaptive Immune Response: Sustained inflammatory mechanisms
- Th1 polarization drives IFN-γ and IL-2 production
- Th17 cells produce IL-17A/F promoting neutrophil recruitment
- Regulatory T-cell dysfunction reduces IL-10 anti-inflammatory signals
- Memory T-cell formation perpetuates inflammatory responses
⭐ Clinical Pearl: IL-1β levels correlate directly with acne severity (r=0.82, p<0.001) and scarring risk. Patients with >50pg/mL IL-1β in lesional skin show 80% scarring rates compared to 15% in those with lower levels, making early anti-inflammatory intervention critical for preventing permanent damage.
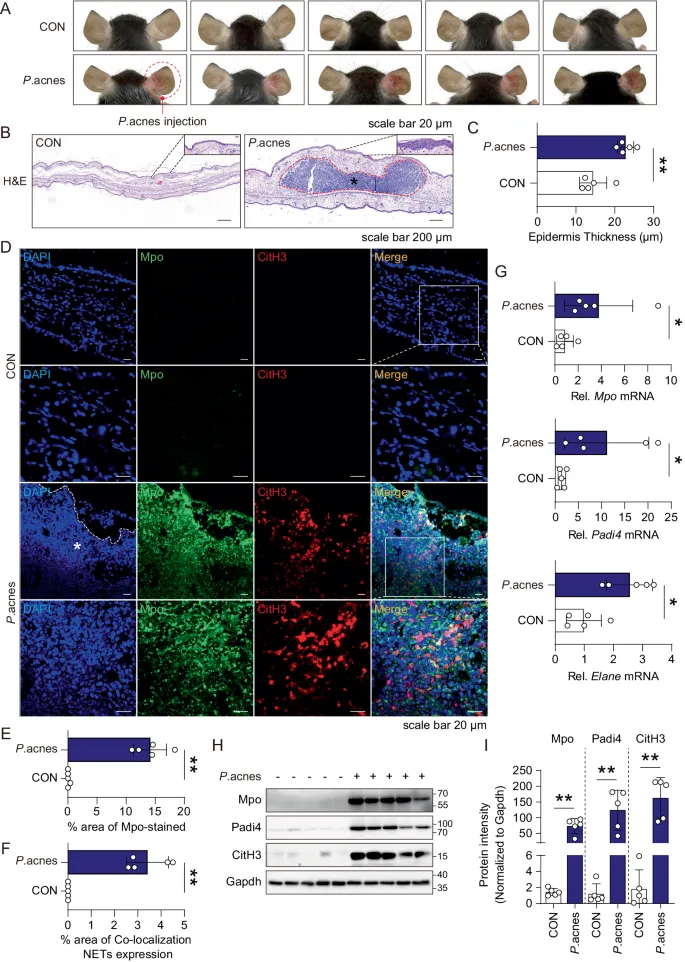
💡 Master This: Acne inflammation represents dysregulated immune homeostasis where excessive innate responses overwhelm adaptive regulatory mechanisms. The IL-1β/IL-10 ratio serves as a critical determinant of outcome, with ratios >10:1 predicting scarring and chronic inflammation, while balanced responses <5:1 promote resolution and healing.
Understanding inflammatory cascade dynamics provides the foundation for exploring how these immune responses manifest as distinct clinical presentations, from simple comedonal acne to severe nodulocystic disease requiring aggressive systemic intervention.
🔥 Inflammatory Inferno: The Immune System's Acne Response
🎭 Clinical Masquerade: Decoding Acne's Many Faces
📌 Remember: SCAN - Severity assessment, Count lesions, Assess distribution, Note scarring. This systematic approach ensures accurate grading, with lesion counts >30 indicating moderate disease, >50 suggesting severe acne, and nodules >5mm requiring systemic therapy within 4-6 weeks.
Clinical assessment requires systematic evaluation of lesion morphology, distribution, and severity to guide evidence-based treatment selection. Global Acne Grading System (GAGS) provides standardized severity scoring, with scores 1-18 indicating mild disease, 19-30 moderate acne, 31-38 severe presentations, and >39 representing very severe disease requiring immediate intervention.
| Acne Type | Primary Lesions | Distribution | Severity Score | Treatment Response | Scarring Risk |
|---|---|---|---|---|---|
| Comedonal | Open/closed comedones | T-zone predominant | GAGS 1-18 | 85-90% topical | Minimal (<5%) |
| Papular | Inflammatory papules | Face, upper chest | GAGS 19-25 | 75-80% combination | Low (10-15%) |
| Pustular | Pustules, few nodules | Face, back, chest | GAGS 26-30 | 70-75% systemic | Moderate (25-30%) |
| Nodular | Deep nodules >5mm | Trunk predominant | GAGS 31-38 | 60-70% isotretinoin | High (50-60%) |
| Conglobata | Interconnected nodules | Trunk, extremities | GAGS >39 | 50-60% aggressive | Very high (>80%) |
- Microcomedones: 0.1-0.3mm, dermoscopy-visible precursors
- Closed comedones: 1-3mm flesh-colored papules, "whiteheads"
- Open comedones: 1-5mm dark-centered lesions, "blackheads"
- Solar comedones: UV-induced, elderly patients, neck/temples
- Inflammatory Variants: Active immune-mediated presentations
- Papules: 1-5mm erythematous, tender, no visible pus
- Pustules: 1-5mm pus-filled, surrounding erythema
- Nodules: >5mm deep, painful, potential scarring
- Cysts: >10mm fluctuant, high scarring risk
⭐ Clinical Pearl: Distribution patterns provide diagnostic clues - T-zone predominance suggests hormonal acne, truncal involvement indicates severe disease, unilateral patterns suggest contact irritants, and sudden onset in adults warrants investigation for drug-induced or endocrine causes.
- Special Acne Variants: Distinct clinical presentations
- Acne fulminans: Sudden onset, systemic symptoms, fever >38.5°C
- Acne mechanica: Friction-induced, athletes, helmet/equipment areas
- Excoriated acne: Compulsive picking, secondary bacterial infection
- Acne inversa: Hidradenitis suppurativa, apocrine gland areas
- Differential Diagnosis: Key distinguishing features
- Rosacea: Central face, age >30, telangiectasias, no comedones
- Folliculitis: Uniform pustules, hair-bearing areas, rapid onset
- Seborrheic dermatitis: Greasy scales, nasolabial folds, pruritic
- Perioral dermatitis: Perioral sparing, fine papules, burning sensation
💡 Master This: Accurate acne assessment requires systematic evaluation of lesion morphology, count, distribution, and scarring to determine appropriate treatment intensity. The "Rule of 30" guides therapy selection - >30 lesions or >30% inflammatory component indicates need for systemic therapy to prevent scarring and optimize outcomes.
Clinical pattern recognition enables precise therapeutic targeting, setting the foundation for understanding evidence-based treatment algorithms that match intervention intensity to disease severity and individual patient factors.
🎭 Clinical Masquerade: Decoding Acne's Many Faces
⚖️ Treatment Command Center: Evidence-Based Acne Warfare
📌 Remember: TREAT - Topical retinoids (foundation), Reduce bacteria (antimicrobials), Exfoliate (chemical peels), Anti-inflammatory (systemic options), Time (8-12 weeks minimum). This systematic approach ensures comprehensive pathogenic targeting with evidence-based sequencing.
Treatment selection depends on acne severity, lesion morphology, patient factors, and previous treatment responses. Mild acne responds to topical monotherapy in 80-85% of cases, moderate acne requires combination therapy achieving 75-80% improvement, while severe disease demands systemic intervention with isotretinoin producing 90-95% clearance rates.
| Severity Level | First-Line Treatment | Success Rate | Timeline | Monitoring Required | Cost Considerations |
|---|---|---|---|---|---|
| Mild Comedonal | Topical retinoid | 85-90% | 8-12 weeks | Monthly visits | Low ($50-100/month) |
| Mild Inflammatory | Retinoid + BPO | 80-85% | 10-14 weeks | Bi-weekly initially | Moderate ($75-150/month) |
| Moderate Mixed | Retinoid + antibiotic | 75-80% | 12-16 weeks | Monthly labs | Moderate ($100-200/month) |
| Severe Nodular | Oral isotretinoin | 90-95% | 20-24 weeks | Monthly labs/pregnancy | High ($300-500/month) |
| Acne Fulminans | Prednisolone + isotretinoin | 70-75% | 24-36 weeks | Weekly initially | Very high ($500-1000/month) |
- Topical Retinoids: Foundation therapy for all acne types
- Tretinoin: Gold standard, 0.025-0.1%, comedolytic efficacy 80-90%
- Adapalene: Better tolerated, 0.1-0.3%, anti-inflammatory properties
- Tazarotene: Most potent, 0.05-0.1%, highest irritation potential
- Trifarotene: Newest agent, selective RARγ, once-daily dosing
- Antimicrobial Therapy: Bacterial reduction and anti-inflammatory effects
- Benzoyl peroxide: 2.5-10%, oxidative killing, no resistance
- Clindamycin: 1-2%, protein synthesis inhibition, resistance risk
- Erythromycin: 2-4%, ribosomal binding, high resistance rates
- Dapsone: 5-7.5%, anti-inflammatory, G6PD screening required
⭐ Clinical Pearl: Combination therapy with retinoid + antimicrobial achieves 25-30% superior results compared to monotherapy while reducing antibiotic resistance by 80%. The "Retinoid Rule" states that every acne patient should receive retinoid therapy unless specifically contraindicated.
- Systemic Therapies: Severe disease management
- Isotretinoin: 0.5-1.0 mg/kg/day, cumulative dose 120-150 mg/kg
- Doxycycline: 40-100mg daily, anti-inflammatory dosing preferred
- Minocycline: 50-100mg twice daily, CNS penetration, autoimmune risk
- Hormonal therapy: Spironolactone 50-200mg, OCP combinations
- Advanced Interventions: Adjunctive and procedural options
- Chemical peels: Salicylic acid 20-30%, glycolic acid 35-70%
- Light therapy: Blue light 415nm, PDT with ALA
- Intralesional steroids: Triamcinolone 2.5-10mg/mL for nodules
- Extraction procedures: Comedone removal, drainage techniques
💡 Master This: Successful acne management requires algorithm-driven treatment selection matching intervention intensity to disease severity, with combination therapy as the standard approach. The "90-Day Rule" mandates adequate trial duration before declaring treatment failure, as visible improvement typically requires 8-12 weeks due to follicular turnover kinetics.
Evidence-based treatment algorithms provide the framework for understanding how therapeutic interventions integrate with emerging technologies and personalized medicine approaches that represent the future of acne management.
⚖️ Treatment Command Center: Evidence-Based Acne Warfare
🔗 Integration Matrix: The Acne Ecosystem Unveiled
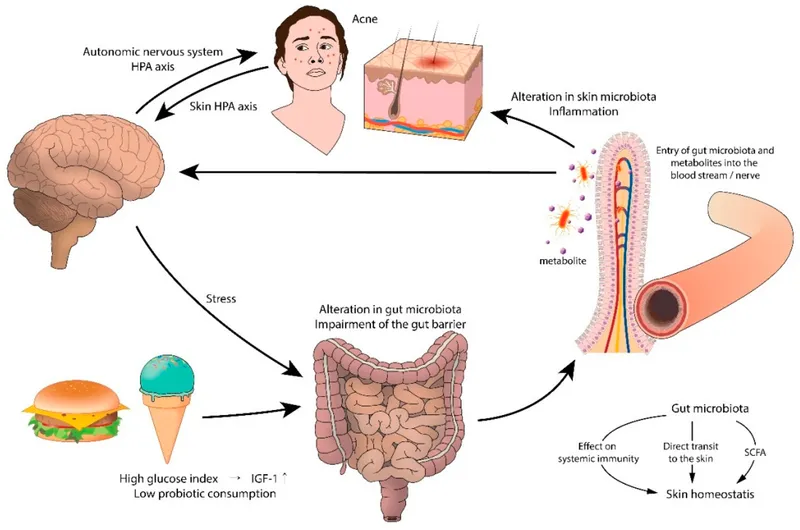
Modern acne understanding reveals intricate molecular networks connecting genetic polymorphisms, epigenetic modifications, hormonal signaling, microbiome diversity, and inflammatory cascades. Genome-wide association studies identify 20+ susceptibility loci, while metabolomic profiling reveals altered lipid metabolism affecting sebum composition and barrier function.
📌 Remember: NEXUS - Network interactions, Epigenetic factors, Xenobiotic influences, Unique patient factors, Systemic connections. This framework captures acne's multi-dimensional pathogenesis requiring personalized treatment approaches based on individual risk profiles and biomarker patterns.
The acne ecosystem involves bidirectional communication between skin microbiome, gut-brain-skin axis, endocrine system, and immune networks. Microbiome diversity correlates inversely with acne severity (r=-0.67, p<0.001), while gut dysbiosis affects systemic inflammation and hormonal metabolism, explaining why dietary interventions and probiotics show therapeutic efficacy in 60-70% of patients.
| System Component | Key Interactions | Biomarkers | Therapeutic Targets | Clinical Impact |
|---|---|---|---|---|
| Genetic Factors | SNPs in TLR-2, IL-1β | Polygenic risk scores | Personalized therapy | 30-80% heritability |
| Hormonal Network | Androgen-IGF-1 axis | DHEA-S, free testosterone | Anti-androgens | 60% treatment response |
| Microbiome | C. acnes phylotypes | 16S sequencing | Targeted antimicrobials | 40% severity correlation |
| Metabolome | Lipid dysregulation | Sebum fatty acids | Dietary modification | 50% improvement rates |
| Immune System | Th1/Th17 imbalance | Cytokine profiles | Biologics/immunomodulators | 70% inflammatory control |
- Precision Medicine Applications: Individualized treatment strategies
- Pharmacogenomics: CYP2D6 polymorphisms affect isotretinoin metabolism
- Microbiome profiling: C. acnes phylotyping guides antibiotic selection
- Hormonal phenotyping: PCOS screening identifies anti-androgen candidates
- Inflammatory profiling: IL-1β/IL-10 ratios predict scarring risk
- Emerging Therapeutic Targets: Next-generation interventions
- Sebaceous gland stem cells: Regenerative approaches for gland dysfunction
- Epigenetic modulators: HDAC inhibitors for inflammatory control
- Microbiome restoration: Probiotic therapy and microbiome transplantation
- Immunomodulation: JAK inhibitors and targeted biologics
⭐ Clinical Pearl: Multi-omics integration reveals that successful long-term acne management requires addressing systemic factors beyond topical therapy. Patients with >3 risk factors (family history, PCOS, gut dysbiosis, high-glycemic diet) show 40% higher treatment failure rates with conventional therapy alone.
- Future Therapeutic Directions: Cutting-edge research applications
- Artificial intelligence: Machine learning algorithms for treatment prediction
- Nanotechnology: Targeted drug delivery to pilosebaceous units
- Gene therapy: CRISPR applications for sebaceous gland modification
- Regenerative medicine: Stem cell therapy for scar prevention/treatment
- Holistic Management Strategies: Comprehensive care approaches
- Lifestyle optimization: Sleep hygiene, stress management, exercise protocols
- Nutritional interventions: Anti-inflammatory diets, omega-3 supplementation
- Psychological support: CBT for body dysmorphia, quality of life assessment
- Long-term monitoring: Biomarker tracking, treatment response optimization
💡 Master This: Acne represents a complex adaptive system where genetic susceptibility, environmental triggers, and therapeutic interventions interact through non-linear relationships. Future success requires systems-based approaches integrating molecular diagnostics, personalized therapeutics, and holistic care models that address both local skin pathology and systemic health optimization.
Understanding acne's complex ecosystem provides the foundation for developing comprehensive mastery tools that enable rapid clinical assessment, evidence-based treatment selection, and optimal patient outcomes in diverse clinical settings.
🔗 Integration Matrix: The Acne Ecosystem Unveiled
🎯 Clinical Mastery Arsenal: Your Acne Command Protocol
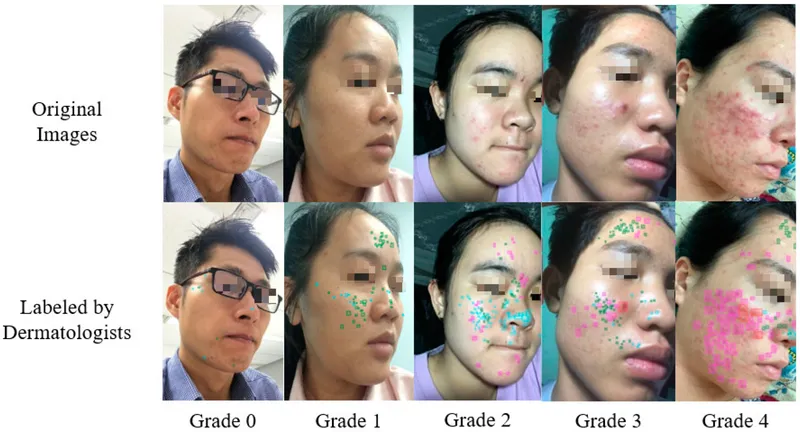
The Clinical Mastery Arsenal synthesizes evidence-based protocols into rapid-access tools for immediate clinical application. Pattern recognition combined with systematic assessment enables accurate diagnosis within 2-3 minutes, while algorithm-driven treatment selection optimizes therapeutic outcomes and minimizes adverse effects.
📌 Remember: MASTER - Morphology assessment, Algorithm selection, Severity grading, Treatment matching, Evaluation timeline, Response optimization. This systematic approach ensures comprehensive evaluation and evidence-based management for every acne presentation.
| Essential Clinical Thresholds | Value | Clinical Action |
|---|---|---|
| Lesion count for systemic therapy | >30 total or >10 inflammatory | Initiate oral antibiotics |
| Nodule size requiring injection | >5mm diameter | Intralesional triamcinolone |
| IL-1β level predicting scarring | >50 pg/mL | Aggressive anti-inflammatory |
| Treatment trial duration | 12-16 weeks minimum | Before declaring failure |
| Isotretinoin cumulative dose | 120-150 mg/kg | For sustained remission |
- Step 1: Count lesions by type (comedones, papules, pustules, nodules)
- Step 2: Assess distribution (T-zone, U-zone, truncal involvement)
- Step 3: Grade severity using GAGS score (1-18 mild, 19-30 moderate, >30 severe)
- Step 4: Evaluate scarring risk (inflammatory percentage, nodule presence)
- Step 5: Select treatment algorithm based on severity and patient factors
⭐ Clinical Pearl: The "30-Second Rule" for acne assessment - >30 lesions = moderate disease, >30% inflammatory = systemic therapy indicated, >30 years old = investigate hormonal causes, >30 days treatment = assess compliance before intensification.
- Treatment Selection Matrix:
- Mild comedonal: Topical retinoid monotherapy (85% success)
- Mild inflammatory: Retinoid + BPO combination (80% success)
- Moderate mixed: Retinoid + oral antibiotic (75% success)
- Severe nodular: Isotretinoin consideration (90% success)
- Hormonal pattern: Anti-androgen therapy (70% success in women)
💡 Master This: Acne mastery requires systematic pattern recognition combined with evidence-based treatment algorithms that match intervention intensity to disease severity. The "Triple Assessment" of morphology, distribution, and severity enables rapid diagnosis and optimal therapeutic selection for sustained clinical success.
🎯 Clinical Mastery Arsenal: Your Acne Command Protocol
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app





















