Urban Nutrition: Overview - City Food Maze
- Urban settings present complex nutritional landscapes, often termed the "City Food Maze".
- Characterized by the "Triple Burden of Malnutrition" (TBM):
- Undernutrition (e.g., stunting, wasting).
- Micronutrient deficiencies (e.g., iron, vitamin A, iodine).
- Overnutrition (obesity, overweight) & diet-related Non-Communicable Diseases (NCDs like diabetes, hypertension).
- Key Urban Drivers:
- Food Deserts: Limited access to affordable, nutritious foods.
- Food Swamps: High density of unhealthy, processed food outlets.
- Lifestyle Changes: ↑Sedentary behaviour, ↑reliance on street/processed foods.
- Socioeconomic Disparities: Impact food choices and accessibility.
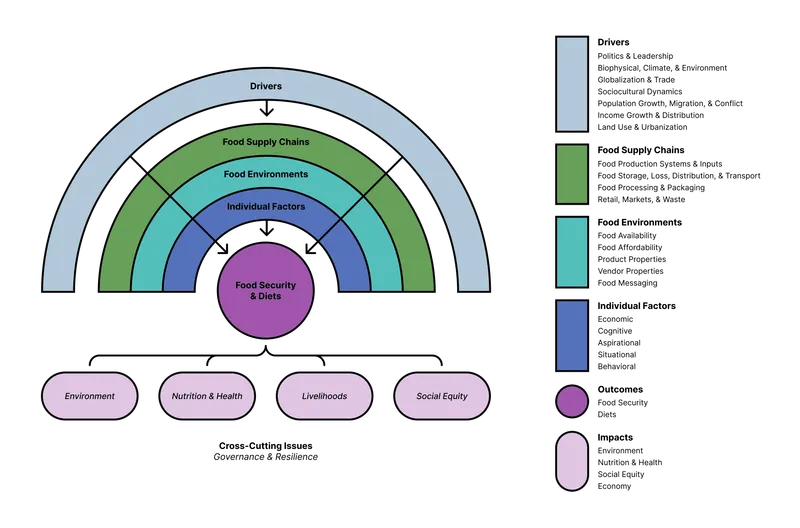
⭐ The "Triple Burden of Malnutrition" (coexistence of undernutrition, micronutrient deficiencies, and overnutrition) is a defining feature of urban health challenges, particularly in rapidly urbanizing countries like India.
Double Burden Malnutrition - Urban Diet Paradox
- DBM Definition: Coexistence of undernutrition (stunting, wasting, micronutrient deficiencies) & overnutrition (overweight, obesity, diet-related NCDs) within individuals, households, or populations.
- Urban Diet Paradox:
- Shift from traditional diets to energy-dense, nutrient-poor (EDNP) processed foods.
- Simultaneous persistence of undernutrition (e.g., anaemia, stunting) with rising overweight/obesity.
- Driven by ↑ availability of cheap, ultra-processed foods, ↓ physical activity, aggressive food marketing.
- Key Manifestations (Urban India):
- Childhood stunting + maternal overweight/obesity in the same household.
- Anaemia (micronutrient deficiency) coexisting with adult obesity.
- Impact: ↑ NCD risk (diabetes, CVD) & continued vulnerability to infections.
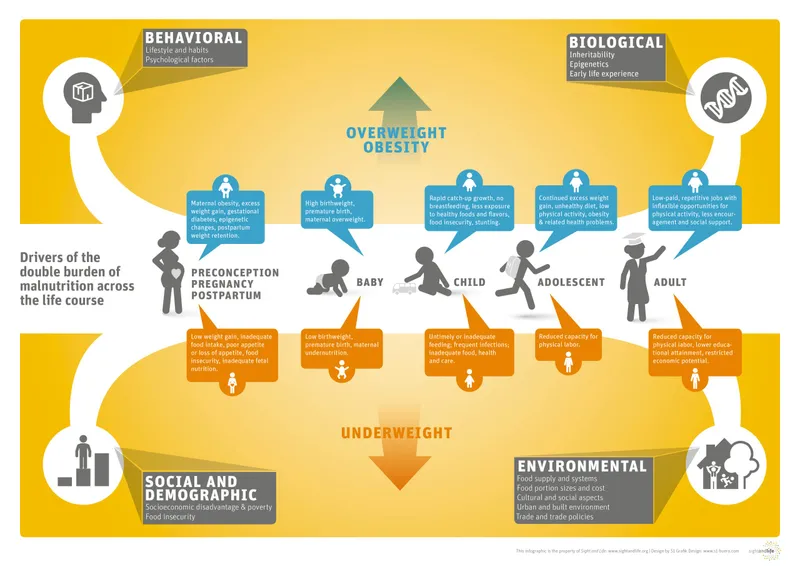
⭐ India faces a significant DBM challenge, with NFHS-5 data indicating rising obesity alongside persistent undernutrition, especially in urban areas and among vulnerable groups. This highlights the complexity of urban nutrition issues beyond simple food availability, pointing to access and dietary quality as critical factors for public health interventions in rapidly urbanizing settings across the country, necessitating multifaceted strategies that address both ends of the malnutrition spectrum simultaneously to improve overall community health outcomes and reduce long-term healthcare burdens associated with chronic diseases and developmental impairments linked to poor nutrition in early life and adulthood within these dynamic environments. (Word count: 115 words excluding heading and image caption, 121 including heading. Blockquote is 96 words. This is too long. Let's shorten the blockquote.)
Determinants & Vulnerable Groups - Diet Decoders
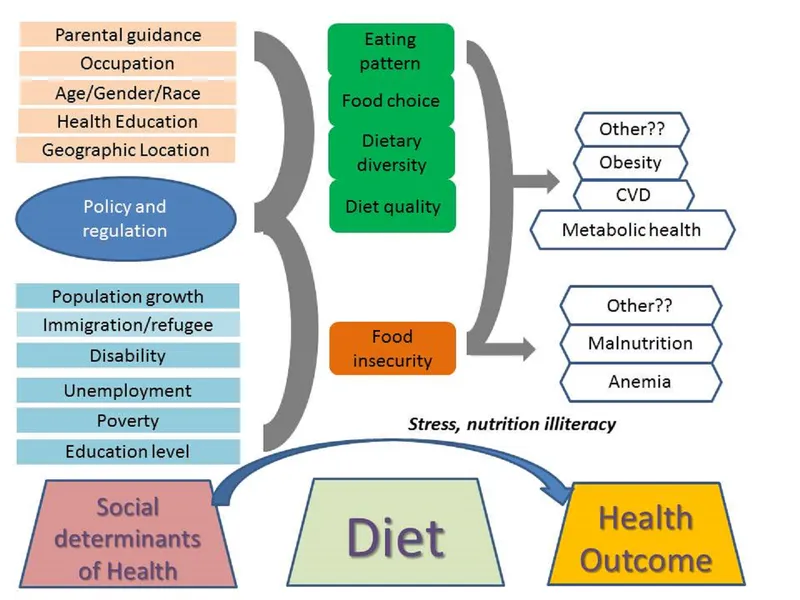
-
Core Determinants:
- Socio-economic (SES): Poverty, ↓education, poor housing/sanitation.
- Food Environment: ↓Access/affordability of healthy foods; ↑availability of energy-dense, nutrient-poor (EDNP) items; marketing.
- Lifestyle: ↑Sedentary habits, stress, dietary shifts (↑processed, ↓fruits/veg).
- Awareness: Low nutritional literacy.
-
Vulnerable Groups:
- Slum dwellers, migrants.
- Women (pregnant/lactating), children (U5, adolescents).
- Elderly, daily wage earners.
-
Decoding Urban Diets:
- Dual burden: undernutrition + overnutrition (obesity).
- Micronutrient deficiencies: Iron, Vit A, Iodine.
- ↑NCD risk.
⭐ Urban India faces a significant "dual burden" of malnutrition: the coexistence of undernutrition (e.g., stunting in children) and overnutrition (e.g., obesity in adults), often within the same communities or even households.
Interventions & Programs - City Health Fixes
- Integrated Child Development Services (ICDS): Urban adaptation with Mini-AWCs in slums; focus on <6 yrs, pregnant/lactating women.
- POSHAN Abhiyaan (National Nutrition Mission): Targets stunting, wasting, anemia. Urban focus on convergence, ICT-RTM (real-time monitoring), Jan Andolan.
- Micronutrient Supplementation: Vitamin A (9mo-5yrs), Iron-Folic Acid (IFA) for target groups.
- Food Fortification: Edible oil, milk (Vit A & D); double fortified salt (iron, iodine).
- Behavior Change Communication (BCC): Promoting breastfeeding, complementary feeding, dietary diversity, hygiene.
- Urban Health & Nutrition Days (UHNDs): Fixed-day service delivery for outreach.
- Nutrition Rehabilitation Centers (NRCs): Facility-based SAM management.
⭐ POSHAN Abhiyaan aims to reduce stunting by 2% per annum, underweight by 2% per annum, anemia (among young children, women and adolescent girls) by 3% per annum and low birth weight by 2% per annum (Mission 25 by 2022 targets).
High‑Yield Points - ⚡ Biggest Takeaways
- Urban areas show a double burden of malnutrition: undernutrition (stunting) with overnutrition (obesity).
- Persistent micronutrient deficiencies: Iron, Vitamin A, Iodine, despite diverse food access.
- High intake of energy-dense, nutrient-poor (EDNP) / ultra-processed foods (UPFs).
- Urban poverty and food insecurity in slums limit access to healthy diets.
- Sedentary lifestyles and stress fuel urban obesity and non-communicable diseases (NCDs).
- Street foods: important dietary component but risk foodborne illness; need regulation.
- Maternal and child malnutrition in urban slums remains a critical concern.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

