Vitamins A & D Deficiencies - Sight & Strength Woes
-
Vitamin A (Retinol): "Sight"
- Xerophthalmia. Earliest: Nyctalopia.
- Signs: Conj. xerosis (X1A), Bitot’s spots (X1B).
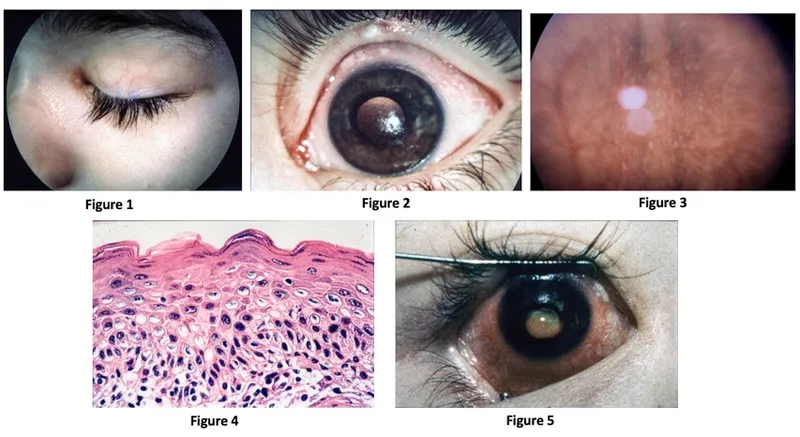 Corneal xerosis (X2), Keratomalacia (X3).
Corneal xerosis (X2), Keratomalacia (X3). - Serum Retinol: < 20 µg/dL.
- Prophylaxis (<5 yrs): 100,000 IU (6-12mo), 200,000 IU (>12mo) q6mo.
⭐ WHO Xerophthalmia: XN (Night blind), X1A (Conj. xerosis), X1B (Bitot's), X2 (Corneal xerosis), X3A/B (Keratomalacia), XS, XF.
-
Vitamin D (Calciferol): "Strength"
- Deficiency: Rickets (children), Osteomalacia (adults).
- Rickets: Craniotabes, Rachitic rosary, Harrison's sulcus, Bowed legs/Knock knees.

- Biochemistry: ↓ Serum Ca, ↓ P; ↑ ALP, ↑ PTH.
- Serum $25(OH)D$: Deficiency < 20 ng/mL (or < 50 nmol/L).
- Rx: High dose Vit D (600,000 IU Stoss).
B-Complex & C Deficiencies - Energy & Repair Crew
| Vit | CoE Form | Deficiency | Key Features |
|---|---|---|---|
| B1 (Thiamine) | TPP | Beriberi, Wernicke-Korsakoff | Polished rice; Wernicke's triad (ataxia, confusion, ophthalmoplegia); heart failure |
| B2 (Riboflavin) | FAD, FMN | Ariboflavinosis | Angular stomatitis, cheilosis, glossitis 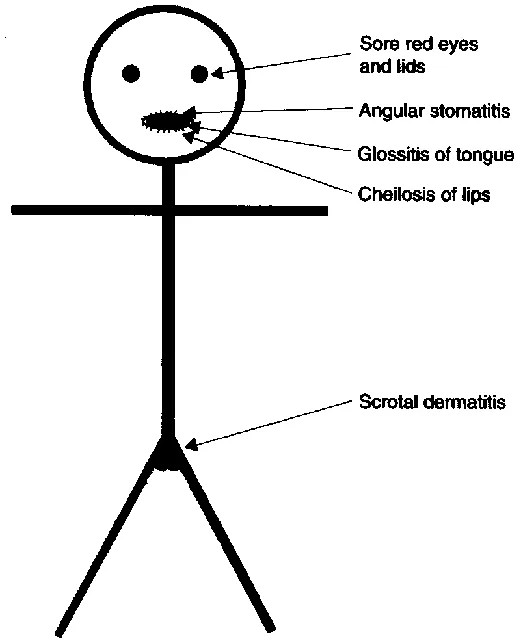 |
| B3 (Niacin) | NAD, NADP | Pellagra | 📌 3Ds: Dermatitis (Casal's necklace), Diarrhea, Dementia 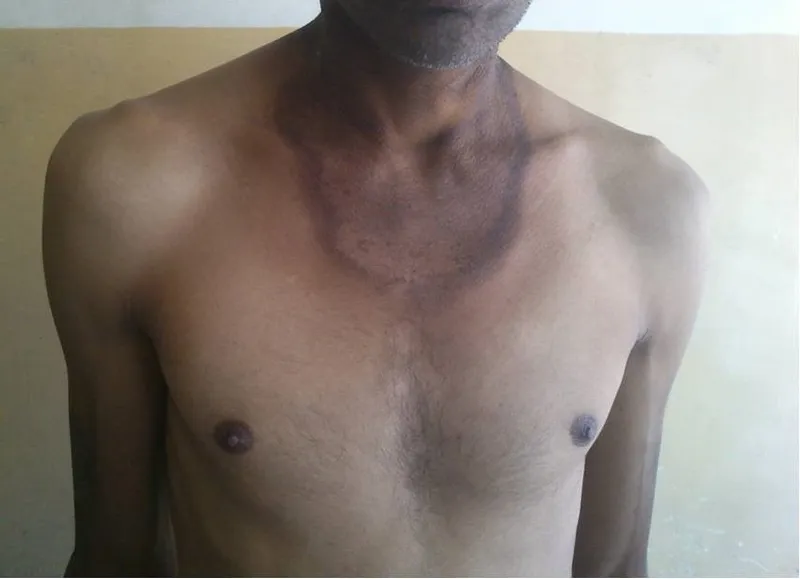 |
| B5 (Pantothenic Acid) | CoA | Burning feet syndrome | Paresthesia (toes), burning feet |
| B6 (Pyridoxine) | PLP | Neuropathy, Anemia (Sideroblastic) | Isoniazid; convulsions (infants); peripheral neuropathy |
| B7 (Biotin) | Biocytin | (Rare) Avidin toxicity | Raw egg white ingestion; alopecia, dermatitis |
| B9 (Folate) | THF | Megaloblastic anemia, NTDs | ↑Homocysteine; glossitis; NO neurological sx |
| B12 (Cobalamin) | Methylcobalamin | Megaloblastic anemia, Neuropathy | Pernicious anemia; SACD (neurological sx); vegan diet; ↑MMA & Homocysteine |
Iron & Iodine Deficiencies - Vitality & Growth Guards
⭐ Iron deficiency is the most common nutritional deficiency worldwide.
| Feature | Iron Deficiency (ID) / Anemia (IDA) | Iodine Deficiency Disorders (IDD) |
|---|---|---|
| Problem | Impaired Hemoglobin (Hb) synthesis, ↓O₂ transport. | ↓Thyroid hormone synthesis, impacting growth & development. |
| Key Indicator | S. Ferritin < 15 ng/mL. Hb cutoffs: Pregnant <11, Non-preg women <12, Men <13 g/dL. | Urinary Iodine Excretion (UIE) < 100 µg/L (population). Neonatal TSH > 5 mIU/L. |
| Clinical | Fatigue, pallor, glossitis, koilonychia. 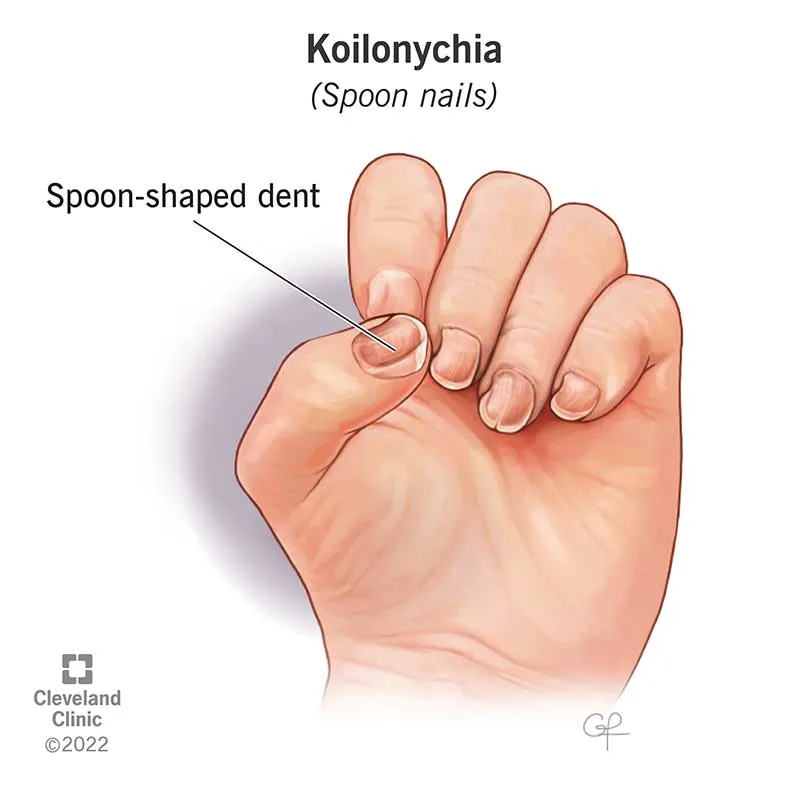 | Goitre, hypothyroidism, cretinism (neurological/myxedematous).  |
| Prevention | Prophylaxis: IFA tablet (Iron 100mg + Folic Acid 0.5mg). Dietary diversification. | Universal Salt Iodization (USI) with $KIO_3$ (≥ 15 ppm at consumer level). |
Other Deficiencies & Programs - Trace Element Tales
- Zinc: Deficiency: Acrodermatitis enteropathica, impaired immunity.
- Diarrhea dose: 10-20 mg for 14 days.

- Diarrhea dose: 10-20 mg for 14 days.
- Fluoride: Optimal water level: 0.5-0.8 ppm. Excess: Dental/Skeletal Fluorosis.
- NPPCF: National Programme for Prevention & Control of Fluorosis.
- Selenium: Deficiency: Keshan disease (cardiomyopathy).
- Copper: Deficiency: Menkes disease (kinky hair).
⭐ Zinc supplementation (10-20 mg for 14 days) significantly reduces duration and severity of acute diarrhea in children.
High‑Yield Points - ⚡ Biggest Takeaways
- Vitamin A deficiency causes night blindness and Bitot's spots.
- Iron deficiency is the most common, leading to microcytic hypochromic anemia.
- Iodine deficiency results in goiter and cretinism.
- Vitamin D deficiency manifests as rickets in children and osteomalacia in adults.
- Vitamin B12 deficiency causes megaloblastic anemia and neurological deficits.
- Folic acid deficiency leads to megaloblastic anemia and neural tube defects.
- Zinc deficiency is linked to growth retardation and impaired immunity.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

