Non-Communicable Diseases

On this page
🌍 The Silent Epidemic: Understanding Non-Communicable Disease Fundamentals
Non-communicable diseases now claim more lives globally than all infectious diseases combined, yet they develop silently over years before symptoms emerge. You'll master how these conditions-from diabetes to cardiovascular disease to cancer-originate at the cellular level, learn to recognize their subtle early patterns, and build systematic frameworks for distinguishing between overlapping presentations. By understanding the interconnected web linking metabolic, cardiovascular, and inflammatory pathways, you'll develop the clinical reasoning to detect, differentiate, and manage NCDs with precision and confidence.
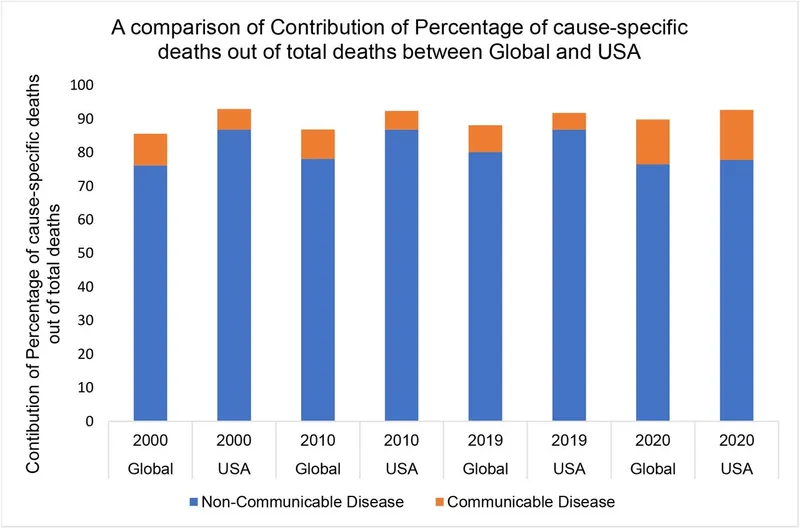
📌 Remember: MAIN NCDs - Mental health disorders, Accidents/injuries, Ischemic heart disease, Neoplasms (cancer). These four categories encompass 85% of NCD-related deaths globally.
The epidemiological transition in developing countries like India creates a "double burden" - persistent infectious diseases alongside rapidly rising NCDs. Urban populations show 3-4 times higher NCD prevalence compared to rural areas, with cardiovascular disease leading at 27% of total deaths, followed by chronic respiratory diseases at 11%, cancer at 9%, and diabetes at 3%.
- Primary NCDs by Global Impact
- Cardiovascular diseases: 17.9 million deaths annually (31% of global mortality)
- Cancers: 9.3 million deaths (17% of global mortality)
- Lung cancer: 1.8 million deaths (highest cancer mortality)
- Colorectal cancer: 935,000 deaths (second highest)
- Chronic respiratory diseases: 4.1 million deaths (7% of global mortality)
- COPD: 3.2 million deaths (90% of respiratory NCD deaths)
- Asthma: 495,000 deaths (affects 339 million people globally)
- Diabetes: 1.5 million deaths (3% of global mortality)
| NCD Category | Global Deaths (millions) | India Deaths (%) | Peak Age Group | Economic Impact (% GDP) | Preventable (%) |
|---|---|---|---|---|---|
| Cardiovascular | 17.9 | 27 | 45-69 years | 2.6 | 80 |
| Cancer | 9.3 | 9 | 55-75 years | 1.2 | 40 |
| Respiratory | 4.1 | 11 | 60+ years | 0.8 | 70 |
| Diabetes | 1.5 | 3 | 40-60 years | 0.5 | 90 |
| Mental Health | 0.8 | 2.5 | 15-45 years | 1.0 | 60 |
💡 Master This: The "4x4 NCD Framework" - 4 main diseases (CVD, cancer, diabetes, chronic respiratory) share 4 common risk factors (tobacco, alcohol, unhealthy diet, physical inactivity), requiring 4 intervention levels (individual, community, health system, policy), measured by 4 key indicators (mortality, morbidity, risk factors, health system response).
Understanding NCD epidemiology reveals critical patterns: 80% of premature heart disease, stroke, and diabetes cases are preventable through risk factor modification. The economic burden reaches $47 trillion globally by 2030, with India losing $4.58 trillion over two decades due to NCDs and mental health conditions.
Connect these foundational NCD patterns through comprehensive risk factor analysis to understand how modifiable behaviors and environmental exposures drive disease development across populations.
🌍 The Silent Epidemic: Understanding Non-Communicable Disease Fundamentals
⚙️ The NCD Mechanism Matrix: How Silent Diseases Develop

📌 Remember: CHAOS mechanism - Chronic inflammation, Hypertension, Atherosclerosis, Oxidative stress, Systemic insulin resistance. These five pathways interconnect to drive 85% of NCD pathophysiology.
- Shared Pathophysiological Pathways
- Insulin Resistance Cascade
- Affects 25% of global population
- Increases CVD risk by 2-4 fold
- Precedes diabetes by 10-15 years
- Links to metabolic syndrome in 60% of cases
- Chronic Inflammatory Response
- IL-6 levels >2 pg/mL predict cardiovascular events
- TNF-α elevation correlates with insulin resistance
- CRP >3 mg/L indicates high cardiovascular risk
- Affects endothelial function within 5-10 years
- Oxidative Stress Mechanisms
- ROS production exceeds antioxidant capacity
- DNA damage accumulates over 20-30 years
- Mitochondrial dysfunction reduces cellular energy by 30-50%
- Lipid peroxidation accelerates atherosclerosis
- Insulin Resistance Cascade
| Mechanism | Biomarker | Normal Range | Disease Risk Threshold | Clinical Significance | Time to Disease |
|---|---|---|---|---|---|
| Inflammation | CRP | <1 mg/L | >3 mg/L | CVD risk x2-3 | 5-10 years |
| Insulin Resistance | HOMA-IR | <2.5 | >4.0 | Diabetes risk x5 | 10-15 years |
| Oxidative Stress | 8-OHdG | <15 ng/mL | >25 ng/mL | Cancer risk x2 | 15-25 years |
| Endothelial Function | FMD | >10% | <5% | CVD events x3 | 3-7 years |
| Metabolic Dysfunction | HbA1c | <5.7% | >6.5% | Complications x4 | 5-10 years |
⭐ Clinical Pearl: Epigenetic modifications account for 60-80% of NCD risk beyond genetics. DNA methylation changes from lifestyle factors can be reversed through intervention, explaining why lifestyle modification prevents 80% of premature CVD and diabetes.
💡 Master This: The "Decade Rule" - Most NCDs require 10-30 years of risk factor exposure before clinical manifestation. Subclinical disease appears 5-15 years before symptoms, creating a critical intervention window where aggressive risk factor modification can prevent or reverse disease progression.
Cellular senescence emerges as a unifying aging mechanism, with senescent cells secreting inflammatory cytokines that accelerate multiple NCDs. Telomere shortening correlates with biological aging and predicts cardiovascular events with hazard ratio 1.3-1.8.
Understanding these mechanistic pathways enables targeted pattern recognition frameworks that identify high-risk individuals before clinical disease develops.
⚙️ The NCD Mechanism Matrix: How Silent Diseases Develop
🎯 Pattern Recognition Mastery: The NCD Detection Framework
📌 Remember: SCREEN approach - Systematic population screening, Clinical risk assessment, Risk factor clustering, Early biomarker detection, Evidence-based thresholds, Networked care coordination. This framework captures 90% of high-risk individuals before clinical events.
- High-Yield Pattern Recognition Frameworks
- Metabolic Syndrome Clustering
- Waist circumference: >102 cm (men), >88 cm (women)
- Blood pressure: ≥130/85 mmHg or treatment
- Fasting glucose: ≥100 mg/dL or diabetes
- HDL cholesterol: <40 mg/dL (men), <50 mg/dL (women)
- Triglycerides: ≥150 mg/dL
- ≥3 criteria = 5-fold diabetes risk, 2-fold CVD risk
- Cardiovascular Risk Stratification
- Low risk: <10% 10-year CVD risk
- Intermediate risk: 10-20% 10-year CVD risk
- High risk: >20% 10-year CVD risk
- Very high risk: Established CVD or diabetes with complications
- Cancer Screening Thresholds
- Cervical: Age 21-65 years, Pap every 3 years
- Breast: Age 50-74 years, mammography every 2 years
- Colorectal: Age 45-75 years, colonoscopy every 10 years
- Lung: Age 50-80 years, ≥20 pack-year smoking history
- Metabolic Syndrome Clustering
| Risk Pattern | Clinical Presentation | Screening Test | Threshold Value | Sensitivity (%) | Specificity (%) |
|---|---|---|---|---|---|
| Pre-diabetes | Asymptomatic obesity | HbA1c | 5.7-6.4% | 85 | 92 |
| Hypertension | Headache, dizziness | BP measurement | ≥140/90 mmHg | 95 | 88 |
| Dyslipidemia | Family history CVD | Lipid profile | LDL >130 mg/dL | 78 | 85 |
| COPD | Chronic cough, dyspnea | Spirometry | FEV1/FVC <0.7 | 90 | 95 |
| Depression | Mood changes, fatigue | PHQ-9 | Score ≥10 | 88 | 85 |
The "Iceberg Phenomenon" describes how clinical NCDs represent only 20% of total disease burden, with 80% existing as subclinical disease or undiagnosed cases. Population screening using risk scores identifies high-risk individuals with positive predictive value 60-80%.
💡 Master This: The "30-3-0.3 Rule" for NCD screening efficiency - 30% of population needs screening, 3% will have positive results requiring follow-up, 0.3% will have serious disease requiring immediate intervention. This ratio optimizes resource allocation and cost-effectiveness.
Artificial intelligence and machine learning algorithms now achieve 85-95% accuracy in predicting cardiovascular events using routine clinical data, ECG patterns, and retinal photographs. Digital biomarkers from wearable devices detect atrial fibrillation with sensitivity >95%.
These pattern recognition frameworks enable systematic discrimination between different NCD presentations and risk profiles.
🎯 Pattern Recognition Mastery: The NCD Detection Framework
🔍 Systematic NCD Discrimination: The Differential Matrix
Chest pain exemplifies the diagnostic challenge - cardiovascular, respiratory, gastrointestinal, and musculoskeletal NCDs can present identically. Acute coronary syndrome accounts for only 15-25% of chest pain presentations, but missing this diagnosis carries mortality risk >10% within 30 days.
📌 Remember: HEART score for chest pain - History (0-2 points), ECG (0-2 points), Age (0-2 points), Risk factors (0-2 points), Troponin (0-2 points). Score 0-3 = 1.7% ACS risk, Score 4-6 = 20.3% ACS risk, Score 7-10 = 72.7% ACS risk.
- Systematic Discrimination Frameworks
- Dyspnea Differential Matrix
- Cardiac causes: Heart failure (BNP >400 pg/mL), coronary disease (troponin elevation)
- Pulmonary causes: COPD (FEV1/FVC <0.7), asthma (reversible obstruction)
- Systemic causes: Anemia (Hb <10 g/dL), thyroid disease (TSH abnormal)
- Deconditioning: Exercise intolerance without objective abnormalities
- Fatigue Syndrome Discrimination
- Depression: PHQ-9 score ≥10, anhedonia, sleep disturbance
- Hypothyroidism: TSH >10 mIU/L, cold intolerance, weight gain
- Diabetes: HbA1c ≥6.5%, polyuria, polydipsia
- Heart failure: BNP >100 pg/mL, orthopnea, edema
- Chronic kidney disease: eGFR <60 mL/min, proteinuria, anemia
- Dyspnea Differential Matrix
| Symptom Complex | Primary NCD | Key Discriminator | Diagnostic Test | Threshold Value | Specificity (%) |
|---|---|---|---|---|---|
| Chest Pain | Acute MI | Troponin elevation | High-sens troponin | >14 ng/L | 95 |
| Dyspnea | Heart Failure | Volume overload | BNP | >400 pg/mL | 90 |
| Fatigue | Depression | Mood symptoms | PHQ-9 | ≥10 points | 88 |
| Weight Loss | Cancer | Constitutional symptoms | CT imaging | Mass lesion | 98 |
| Cognitive Decline | Dementia | Memory impairment | MoCA | <26 points | 87 |
⭐ Clinical Pearl: "Common things occur commonly" - 80% of NCD presentations represent 20% of diagnoses. Diabetes, hypertension, depression, and COPD account for 60% of primary care NCD visits, but atypical presentations of common diseases cause more diagnostic errors than rare diseases.
Multimorbidity affects 65% of adults >65 years, with average 2.9 chronic conditions per patient. Disease clustering follows predictable patterns: diabetes-hypertension-dyslipidemia (metabolic cluster), COPD-heart failure-depression (cardiopulmonary cluster), arthritis-osteoporosis-depression (musculoskeletal cluster).
💡 Master This: The "Index Disease Principle" - Once one NCD is diagnosed, systematic screening for related conditions increases diagnostic yield 3-5 fold. Diabetes diagnosis should trigger cardiovascular, renal, and ophthalmologic screening. COPD diagnosis should prompt cardiovascular and osteoporosis assessment.
Precision medicine approaches use genetic markers, biomarkers, and clinical phenotypes to distinguish disease subtypes. Type 2 diabetes includes ≥5 distinct subtypes with different progression patterns, complication risks, and treatment responses.
These discrimination frameworks enable evidence-based treatment algorithms that optimize outcomes for specific NCD presentations.
🔍 Systematic NCD Discrimination: The Differential Matrix
⚖️ Evidence-Based NCD Management: The Treatment Algorithm Matrix
Guideline concordance varies dramatically across NCDs - hypertension management achieves 70-80% guideline adherence, while depression treatment shows only 40-50% evidence-based care delivery. Polypharmacy affects 40% of adults >65 years, with average 5.2 medications per patient increasing adverse event risk exponentially.
📌 Remember: SMART treatment goals - Specific targets, Measurable outcomes, Achievable within timeframe, Relevant to patient, Time-bound milestones. Diabetes: HbA1c <7% (general), <6.5% (young/healthy), <8% (elderly/comorbid).
- Evidence-Based Treatment Hierarchies
- Hypertension Management Algorithm
- Stage 1 (130-139/80-89): Lifestyle modification + single agent
- Stage 2 (≥140/90): Lifestyle modification + 2-drug combination
- Resistant (≥3 drugs): Add spironolactone or refer specialist
- Target: <130/80 mmHg (general), <140/90 (elderly >65 years)
- Diabetes Treatment Progression
- First-line: Metformin up to 2000 mg daily
- Second-line: Add SGLT2 inhibitor or GLP-1 agonist (CVD benefit)
- Third-line: Add insulin or sulfonylurea (cost consideration)
- Monitoring: HbA1c every 3 months until target, then every 6 months
- Depression Treatment Algorithm
- Mild: Psychotherapy or watchful waiting
- Moderate: SSRI + psychotherapy
- Severe: Combination therapy + specialist referral
- Treatment-resistant: Switch class or augmentation strategy
- Hypertension Management Algorithm
| NCD Category | First-Line Treatment | Success Rate (%) | Time to Effect | Monitoring Parameter | Target Value |
|---|---|---|---|---|---|
| Hypertension | ACE inhibitor/ARB | 75-85 | 2-4 weeks | Blood pressure | <130/80 mmHg |
| Diabetes | Metformin | 70-80 | 4-8 weeks | HbA1c | <7% |
| Depression | SSRI | 60-70 | 4-6 weeks | PHQ-9 score | <5 points |
| COPD | Bronchodilator | 65-75 | 1-2 weeks | FEV1 | >80% predicted |
| Dyslipidemia | Statin | 80-90 | 6-8 weeks | LDL cholesterol | <70 mg/dL |
Combination therapy principles maximize efficacy while minimizing side effects. Fixed-dose combinations improve medication adherence by 20-30% compared to separate pills. Polypill strategies combining aspirin, statin, and ACE inhibitor reduce cardiovascular events by 30% in high-risk populations.
💡 Master This: The "Number Needed to Treat (NNT)" guides treatment decisions - Statins for primary prevention: NNT = 217 over 4 years, Statins for secondary prevention: NNT = 83 over 2 years. Lower NNT indicates more effective intervention requiring fewer patients treated to prevent one adverse outcome.
Precision medicine approaches tailor treatment based on genetic markers, biomarkers, and clinical phenotypes. Pharmacogenomic testing for CYP2D6 and CYP2C19 variants guides antidepressant selection, improving response rates from 60% to 75%.
These evidence-based algorithms enable multi-system integration approaches that address complex comorbidity patterns.
⚖️ Evidence-Based NCD Management: The Treatment Algorithm Matrix
🔗 Multi-System Integration: The NCD Interconnection Web
Cardiometabolic syndrome exemplifies multi-system integration, where insulin resistance drives hypertension, dyslipidemia, and endothelial dysfunction simultaneously. Diabetes increases cardiovascular risk 2-4 fold, while depression doubles diabetes complications and increases cardiovascular mortality by 60%.

📌 Remember: MIND-BODY integration - Metabolic dysfunction, Inflammation cascade, Neurohormonal activation, Depression/anxiety, Behavioral factors, Oxidative stress, Dysregulated immunity, Years of accumulated damage. These eight interconnected systems drive 90% of NCD complexity.
- Critical System Interconnections
- Cardiovascular-Metabolic Axis
- Insulin resistance → endothelial dysfunction → atherosclerosis
- Hyperglycemia → advanced glycation → vascular damage
- Dyslipidemia → oxidized LDL → plaque formation
- Hypertension → arterial stiffness → cardiac remodeling
- Neuro-Endocrine-Immune Network
- Chronic stress → cortisol elevation → metabolic dysfunction
- Depression → inflammatory cytokines → insulin resistance
- Sleep disorders → growth hormone disruption → metabolic syndrome
- Gut microbiome → systemic inflammation → multiple NCDs
- Respiratory-Cardiovascular Integration
- COPD → systemic inflammation → cardiovascular disease
- Sleep apnea → intermittent hypoxia → hypertension
- Pulmonary hypertension → right heart failure → systemic congestion
- Cardiovascular-Metabolic Axis
| System Integration | Primary Mechanism | Secondary Effects | Clinical Manifestation | Intervention Target | Outcome Improvement |
|---|---|---|---|---|---|
| Cardio-Metabolic | Insulin resistance | Endothelial dysfunction | Diabetes + CVD | Metformin + Statin | 40% event reduction |
| Neuro-Psychiatric | Chronic inflammation | Neurotransmitter imbalance | Depression + Diabetes | SSRI + Lifestyle | 30% better control |
| Pulmonary-Cardiac | Hypoxic stress | Pulmonary hypertension | COPD + Heart failure | Bronchodilator + ACE-I | 25% hospitalization ↓ |
| Renal-Cardiovascular | Fluid retention | Pressure overload | CKD + Hypertension | ARB + Diuretic | 35% progression ↓ |
| Musculoskeletal-Metabolic | Physical inactivity | Muscle insulin resistance | Arthritis + Diabetes | Exercise + Metformin | 50% mobility ↑ |
⭐ Clinical Pearl: "Treat one, affect many" - Exercise intervention simultaneously improves cardiovascular fitness (+15%), insulin sensitivity (+25%), mood scores (+30%), bone density (+5%), and cognitive function (+10%). Multi-system benefits explain why lifestyle interventions often outperform single-target medications.
Integrated care models demonstrate superior outcomes compared to disease-specific approaches. Patient-centered medical homes reduce hospitalizations by 20%, emergency visits by 15%, and healthcare costs by 12% while improving patient satisfaction scores by 25%.
💡 Master This: The "Common Pathway Principle" - Targeting shared mechanisms (inflammation, insulin resistance, oxidative stress) provides greater therapeutic efficiency than treating individual diseases separately. Anti-inflammatory interventions benefit cardiovascular disease, diabetes, depression, and cancer simultaneously through common pathway modulation.
Artificial intelligence platforms now integrate multi-omics data (genomics, proteomics, metabolomics) to predict disease trajectories and treatment responses across multiple NCDs simultaneously. Machine learning algorithms achieve 85-90% accuracy in predicting cardiovascular events in diabetic patients using integrated biomarker panels.
These multi-system insights enable comprehensive mastery frameworks that optimize clinical decision-making across complex NCD presentations.
🔗 Multi-System Integration: The NCD Interconnection Web
🎯 Clinical Mastery Arsenal: The NCD Command Center
Clinical decision support systems now achieve 85-95% accuracy in NCD risk prediction, medication optimization, and complication prevention. Electronic health records with integrated algorithms reduce medication errors by 40%, missed diagnoses by 25%, and inappropriate prescribing by 30%.
📌 Remember: MASTER framework - Monitor key metrics, Assess risk factors, Screen systematically, Treat to targets, Educate patients, Review outcomes. This systematic approach achieves optimal NCD control in 80-90% of patients when implemented consistently.
- Essential Clinical Arsenal Components
- Rapid Assessment Tools
- 10-year CVD risk: Pooled Cohort Equations (ACC/AHA)
- Diabetes risk: Finnish Diabetes Risk Score (FINDRISC)
- Depression screening: PHQ-9 (9 questions, 5 minutes)
- COPD assessment: CAT score (8 questions, 3 minutes)
- Frailty evaluation: Clinical Frailty Scale (visual assessment)
- Critical Monitoring Parameters
- Diabetes: HbA1c every 3-6 months, annual eye/foot exams
- Hypertension: Home BP monitoring, annual microalbumin
- Dyslipidemia: Lipid panel every 6-12 months
- Depression: PHQ-9 every visit, suicide risk assessment
- COPD: Spirometry annually, exacerbation frequency
- Treatment Optimization Protocols
- Medication reconciliation at every visit
- Adherence assessment using validated tools
- Side effect monitoring with systematic checklists
- Drug interaction screening via electronic systems
- Rapid Assessment Tools
| Clinical Tool | Application | Time Required | Accuracy (%) | Clinical Impact | Cost-Effectiveness |
|---|---|---|---|---|---|
| CVD Risk Calculator | Primary prevention | 2 minutes | 85-90 | 30% event reduction | High |
| HbA1c Point-of-Care | Diabetes monitoring | 5 minutes | 95-98 | 25% better control | Moderate |
| PHQ-9 Depression | Mental health screening | 3 minutes | 88-92 | 40% diagnosis rate ↑ | High |
| Spirometry | COPD assessment | 10 minutes | 90-95 | 35% early detection | Moderate |
| Medication Review | Polypharmacy management | 15 minutes | 80-85 | 50% adverse events ↓ | Very High |
Quality improvement initiatives demonstrate remarkable NCD outcome improvements: Diabetes collaborative care achieves HbA1c <7% in 75% of patients (vs 45% usual care), Depression collaborative care achieves 50% response rates (vs 25% usual care), Hypertension team-based care achieves BP control in 80% of patients (vs 55% usual care).
💡 Master This: The "Triple Aim Plus" framework - Better health outcomes, improved patient experience, reduced per capita costs, plus provider satisfaction. Successful NCD programs achieve 15-25% improvement across all four dimensions through systematic care redesign and technology integration.
Emerging technologies transform NCD management: Continuous glucose monitoring reduces diabetes complications by 30%, Remote patient monitoring decreases heart failure hospitalizations by 40%, AI-powered medication optimization improves adherence by 25% and reduces adverse events by 35%.
This clinical mastery arsenal provides the foundation for transforming NCD care delivery and achieving optimal patient outcomes across diverse healthcare settings.
🎯 Clinical Mastery Arsenal: The NCD Command Center
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app
























