Maternal and Child Health

On this page
🏥 Maternal Health Fortress: The Protective Shield System
Maternal and child health forms an interconnected fortress where prevention, early recognition, and systematic intervention determine outcomes across generations. You'll master the protective mechanisms that safeguard pregnancy, decode clinical patterns that signal danger, and build diagnostic frameworks that distinguish normal adaptation from pathology. Through evidence-based algorithms and integrated care systems, you'll develop the clinical judgment to navigate complex scenarios from preconception through childhood, transforming theoretical knowledge into decisive action that protects two lives simultaneously.
📌 Remember: MOTHERS - Maternal mortality, Obstetric care, Timing of interventions, High-risk identification, Emergency preparedness, Reproductive health, Safe delivery practices
The MCH framework operates on three critical levels: individual clinical care, health system strengthening, and population-level interventions. Each level requires specific competencies and evidence-based protocols that directly impact outcomes.
-
Individual Level (60-80% of outcomes determined here)
- Skilled birth attendance: reduces maternal mortality by 50-60%
- Emergency obstetric care: prevents 75% of maternal deaths
- Quality antenatal care: decreases complications by 40-50%
- Early detection protocols (first trimester screening)
- Risk stratification systems (high/moderate/low risk categories)
- Evidence-based intervention timing (specific gestational age thresholds)
-
Health System Level (20-30% impact on population outcomes)
- Referral networks: 24/7 emergency transport systems
- Blood bank availability: 100% coverage for obstetric emergencies
- Skilled provider density: minimum 2.3 per 1000 population (WHO standard)
-
Population Level (10-15% direct impact, 40% long-term influence)
- Education programs: secondary education reduces maternal mortality by 50%
- Nutrition interventions: iron-folic acid supplementation prevents 20% of maternal deaths
- Family planning access: contraceptive prevalence above 70% correlates with <100 maternal deaths per 100,000 live births
⭐ Clinical Pearl: Countries achieving <50 maternal deaths per 100,000 live births consistently demonstrate >90% skilled birth attendance, >95% antenatal care coverage, and <5% unmet contraceptive need.
| MCH Component | Coverage Target | Mortality Impact | Cost-Effectiveness | Implementation Priority |
|---|---|---|---|---|
| Skilled Birth Attendance | >90% | 50-60% reduction | $1-3 per DALY | Immediate |
| Emergency Obstetric Care | 100% availability | 75% preventable deaths | $5-15 per DALY | Critical |
| Family Planning | >70% CPR | 30% mortality reduction | $0.50-2 per DALY | Foundation |
| Antenatal Care (4+ visits) | >95% | 40% complication reduction | $2-8 per DALY | Essential |
| Postnatal Care (48hrs) | >90% | 60% neonatal deaths | $3-10 per DALY | Urgent |
Understanding these foundational principles prepares you to master the specific mechanisms that drive maternal and child health outcomes through targeted interventions and system-level improvements.
🏥 Maternal Health Fortress: The Protective Shield System
🔄 The Reproductive Continuum: Life-Cycle Health Architecture
📌 Remember: CYCLES - Contraception planning, Young adult preparation, Conception optimization, Labor management, Early postpartum care, Spacing between pregnancies
The continuum operates through interconnected physiological systems that must be understood mechanistically to predict and prevent complications:
-
Hormonal Regulation System
- HPO axis maturation: 2-8 years from menarche to regular ovulation
- Fertility window: peak at 20-24 years, 50% decline by 35 years
- Pregnancy hormones: hCG rises 100-fold, progesterone increases 10-fold
- First trimester: rapid hormonal adaptation (0-12 weeks)
- Second trimester: physiological stability (13-27 weeks)
- Third trimester: preparation for delivery (28-40 weeks)
-
Metabolic Adaptation System
- Pregnancy metabolism: 20% increase in basal metabolic rate
- Glucose tolerance: insulin resistance develops by 24-28 weeks
- Calcium demands: 1200mg daily requirement, 30% increase from baseline
- Iron requirements: 27mg daily, 3-fold increase during pregnancy
-
Cardiovascular Adaptation System
- Blood volume expansion: 40-50% increase by 32-34 weeks
- Cardiac output: increases 30-50% above pre-pregnancy levels
- Blood pressure changes: 5-10mmHg decrease in second trimester
- Postpartum recovery: 6-12 weeks for complete cardiovascular normalization
⭐ Clinical Pearl: Women with <18 months inter-pregnancy interval have 40% higher risk of preterm birth, 60% higher risk of low birth weight, and 25% higher maternal mortality compared to 18-59 month spacing.
| Life Cycle Phase | Duration | Key Health Risks | Critical Interventions | Outcome Metrics |
|---|---|---|---|---|
| Adolescence | 10-19 years | Anemia (42%), Early pregnancy | Iron supplementation, Education | School completion >90% |
| Pre-conception | Variable | Nutritional deficits, Infections | Folic acid, Immunizations | Birth defect reduction 70% |
| Pregnancy | 40 weeks | Hemorrhage, Hypertension, Sepsis | ANC 4+ visits, Skilled delivery | MMR <70 per 100,000 |
| Childbirth | 24-48 hours | Obstructed labor, Bleeding | Emergency obstetric care | CFR <1% for complications |
| Postpartum | 6 weeks | Infection, Depression, Bleeding | PNC within 48 hours | Mortality reduction 60% |
This mechanistic understanding of the reproductive continuum provides the foundation for recognizing patterns and implementing evidence-based interventions that optimize outcomes across the entire maternal and child health spectrum.
🔄 The Reproductive Continuum: Life-Cycle Health Architecture
🎯 Clinical Pattern Recognition: The MCH Diagnostic Matrix
📌 Remember: DANGER - Delay in care, Anemia severity, Nutrition status, Gestational age risks, Emergency signs, Referral criteria
The MCH diagnostic matrix operates through three primary recognition patterns: risk stratification, emergency identification, and intervention timing. Each pattern has specific triggers and evidence-based responses.
-
Risk Stratification Patterns ("See X, Think Y" Framework)
- Age <18 or >35 years → Think: 2-3x higher complication risk
- BMI <18.5 or >30 → Think: 40-60% increased adverse outcomes
- Previous cesarean section → Think: 0.5% uterine rupture risk, VBAC counseling needed
- Low risk criteria: Single previous cesarean, >18 months since delivery, no contraindications
- High risk criteria: >2 previous cesareans, classical incision, <18 months interval
- Success rates: 70-80% VBAC success in appropriate candidates
-
Emergency Recognition Patterns (Immediate Action Required)
- Severe headache + visual changes → Think: Preeclampsia/eclampsia (15% maternal mortality if untreated)
- Heavy bleeding + shock → Think: Postpartum hemorrhage (>500ml vaginal, >1000ml cesarean)
- Prolonged labor + fetal distress → Think: Obstructed labor (5% uterine rupture risk)
- First stage: >20 hours nullipara, >14 hours multipara
- Second stage: >3 hours nullipara, >2 hours multipara
- Fetal distress: FHR <110 or >160, late decelerations, meconium-stained liquor
-
Intervention Timing Patterns (Critical Windows)
- First trimester (0-12 weeks): Folic acid supplementation, genetic screening
- Second trimester (13-27 weeks): Anomaly scan, GDM screening at 24-28 weeks
- Third trimester (28-40 weeks): Growth monitoring, delivery planning
- Preterm prevention: Corticosteroids at 24-34 weeks if delivery likely
- Term delivery: 39-41 weeks optimal timing, <39 weeks increases respiratory complications 5-fold
⭐ Clinical Pearl: The "Rule of 500" - Postpartum hemorrhage >500ml occurs in 5% of deliveries, but accounts for 25% of maternal deaths globally. Early recognition and active management of third stage reduces risk by 60%.
| Clinical Scenario | Recognition Trigger | Immediate Assessment | Evidence-Based Action | Success Metric |
|---|---|---|---|---|
| Severe Preeclampsia | BP >160/110 + proteinuria | Neurological exam, Labs | MgSO4, Delivery planning | Seizure prevention 90% |
| Postpartum Hemorrhage | Blood loss >500ml | Vital signs, Fundal exam | Uterotonic drugs, Massage | Control bleeding 85% |
| Obstructed Labor | Prolonged labor + signs | Partograph, Fetal status | Cesarean section | Reduce mortality 95% |
| Neonatal Asphyxia | Apgar <7 at 5 minutes | Airway, Breathing, Circulation | Resuscitation protocol | Normal outcome 80% |
| Severe Anemia | Hb <7 g/dl in pregnancy | Cardiac status, Symptoms | Blood transfusion | Prevent heart failure 90% |
These pattern recognition frameworks provide the systematic approach needed to analyze complex clinical presentations and implement appropriate evidence-based interventions in maternal and child health practice.
🎯 Clinical Pattern Recognition: The MCH Diagnostic Matrix
⚖️ Systematic MCH Assessment: The Differential Diagnosis Framework
📌 Remember: COMPARE - Clinical signs, Objective measurements, Maternal history, Physical findings, Assessment tools, Risk factors, Evidence-based criteria
The systematic assessment framework uses three-tier discrimination: physiological vs pathological, mild vs severe complications, and immediate vs delayed interventions. Each tier has specific quantitative thresholds and clinical correlations.
-
Physiological vs Pathological Discrimination
- Blood pressure changes: Normal 5-10mmHg decrease vs >140/90 hypertension
- Weight gain patterns: Normal 11-16kg total vs >2kg/week after 20 weeks
- Fetal movement: Normal >10 movements/12 hours vs <10 requiring assessment
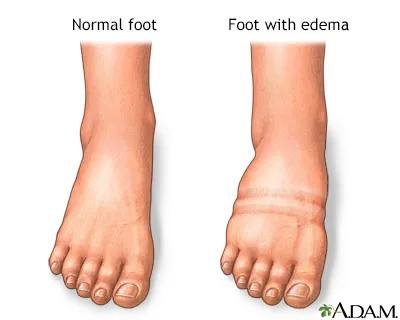
- Physiological edema: Dependent, non-pitting, resolves with rest
- Pathological edema: Facial, pitting, persistent, associated with proteinuria
- Normal fatigue: First/third trimester, improves with rest
- Pathological fatigue: Severe anemia (Hb <10g/dl), cardiac symptoms
-
Severity Stratification Framework
- Mild hypertension: 140-159/90-109 mmHg, no proteinuria, normal symptoms
- Severe hypertension: >160/110 mmHg, proteinuria >300mg/24hr, neurological symptoms
- Anemia classification: Mild 10-10.9 g/dl, Moderate 7-9.9 g/dl, Severe <7 g/dl
- Mild complications: Outpatient management, routine monitoring
- Moderate complications: Increased surveillance, specialist consultation
- Severe complications: Hospital admission, immediate intervention
-
Intervention Urgency Matrix
- Immediate (<30 minutes): Eclampsia, severe hemorrhage, cord prolapse
- Urgent (<4 hours): Severe preeclampsia, fetal distress, placental abruption
- Semi-urgent (<24 hours): Mild preeclampsia, IUGR, oligohydramnios
- Emergency criteria: Maternal compromise, fetal compromise, progressive deterioration
- Monitoring criteria: Stable vital signs, reassuring fetal status, no progression
⭐ Clinical Pearl: Preeclampsia affects 5-8% of pregnancies but accounts for 15% of maternal deaths. The key discriminator is rate of progression - rapid onset (<48 hours) indicates severe disease requiring immediate delivery.
| Condition | Mild Presentation | Moderate Presentation | Severe Presentation | Management Urgency |
|---|---|---|---|---|
| Hypertension | 140-149/90-99 mmHg | 150-159/100-109 mmHg | >160/110 mmHg | Routine/Urgent/Immediate |
| Proteinuria | Trace-1+ dipstick | 2+ dipstick | 3-4+ dipstick | Monitor/Investigate/Deliver |
| Anemia | Hb 10-10.9 g/dl | Hb 7-9.9 g/dl | Hb <7 g/dl | Iron/Investigate/Transfuse |
| IUGR | 10-25th percentile | 5-10th percentile | <5th percentile | Monitor/Surveillance/Deliver |
| Oligohydramnios | AFI 5-8 cm | AFI 2-5 cm | AFI <2 cm | Weekly/Biweekly/Daily |
This systematic discrimination framework enables accurate assessment of complex MCH presentations and appropriate allocation of resources based on evidence-based severity criteria and intervention urgency.
⚖️ Systematic MCH Assessment: The Differential Diagnosis Framework
🚨 Evidence-Based MCH Management: The Treatment Algorithm Matrix

📌 Remember: TREAT - Timing of intervention, Risk-benefit analysis, Evidence level, Alternative options, Target outcomes
The treatment algorithm operates through four integrated decision pathways: emergency management, risk-stratified care, preventive interventions, and outcome optimization. Each pathway has specific evidence grades and success metrics.
-
Emergency Management Protocols (Level 1 Evidence)
- Severe preeclampsia: MgSO4 4-6g IV loading dose, 1-2g/hr maintenance
- Postpartum hemorrhage: Oxytocin 10 IU IM, Tranexamic acid 1g IV within 3 hours
- Eclampsia: MgSO4 4g IV over 5-10 minutes, delivery within 24 hours
- Success rates: MgSO4 prevents 58% of recurrent seizures
- Mortality reduction: Early intervention reduces maternal death by 45%
- Monitoring: Respiratory rate >12/min, urine output >25ml/hr, reflexes present
-
Risk-Stratified Management (Evidence-Based Thresholds)
- GDM management: Target glucose <95mg/dl fasting, <140mg/dl 1-hour post-meal
- Hypertension control: Target BP 130-150/80-100 mmHg (avoid <130/80)
- Anemia treatment: Iron 100-200mg daily, IV iron if Hb <7g/dl or intolerant
- Insulin therapy: Required in 15-30% of GDM cases
- Antihypertensive choice: Methyldopa first-line, Labetalol second-line
- Iron absorption: Enhanced with Vitamin C, reduced with calcium/tea
-
Preventive Intervention Matrix (Population-Level Evidence)
- Folic acid supplementation: 400-800 mcg daily reduces neural tube defects by 70%
- Calcium supplementation: 1.5-2g daily reduces preeclampsia by 55% in high-risk women
- Low-dose aspirin: 75-150mg daily from 12 weeks reduces preeclampsia by 17%
- Target populations: Previous preeclampsia, chronic hypertension, diabetes
- Timing: Before 16 weeks gestation for maximum benefit
- Duration: Continue until delivery for sustained protection
⭐ Clinical Pearl: Corticosteroids for fetal lung maturity (Betamethasone 12mg IM x2 doses, 24 hours apart) reduce neonatal death by 31% and respiratory distress by 34% when given 24-34 weeks gestation.
| Condition | First-Line Treatment | Success Rate | Alternative Options | Monitoring Parameters |
|---|---|---|---|---|
| Severe Preeclampsia | MgSO4 + Delivery | 95% seizure prevention | Phenytoin (less effective) | Reflexes, RR, UOP |
| PPH | Oxytocin + TXA | 85% bleeding control | Ergometrine, PGF2α | Vital signs, Blood loss |
| GDM | Diet + Exercise | 70-85% glucose control | Insulin therapy | Blood glucose, Growth |
| Preterm Labor | Tocolytics + Steroids | 48-hour delay 80% | Bed rest (ineffective) | Contractions, Cervix |
| IUGR | Delivery timing | 90% good outcome | Expectant management | Doppler, BPP, Growth |
This evidence-based treatment framework ensures optimal outcomes through systematic application of proven interventions with quantifiable success rates and appropriate monitoring protocols.
🚨 Evidence-Based MCH Management: The Treatment Algorithm Matrix
🌐 Integrated MCH Systems: The Multi-Dimensional Care Network
📌 Remember: SYSTEMS - Stakeholder coordination, Yield optimization, Synergistic effects, Technology integration, Equity considerations, Monitoring systems, Sustainability planning
The integration operates through five interconnected dimensions: vertical integration (primary to tertiary care), horizontal integration (across sectors), temporal integration (across life course), functional integration (across services), and digital integration (information systems).
-
Vertical Integration Architecture (Care Level Coordination)
- Primary level: Community health workers, basic ANC, normal deliveries (80% of care)
- Secondary level: Comprehensive emergency obstetric care, cesarean sections, blood transfusion
- Tertiary level: High-risk pregnancies, NICU care, subspecialty services (5-10% of cases)
- Referral efficiency: <30 minutes transport time for 90% of population
- Communication systems: 24/7 consultation networks, telemedicine capabilities
- Quality standards: Standardized protocols across all levels, competency-based training
-
Horizontal Integration Matrix (Cross-Sector Collaboration)
- Health sector: Clinical services, emergency care, health promotion
- Education sector: Girls' education (reduces maternal mortality by 50% with secondary completion)
- Nutrition sector: Food security, micronutrient supplementation, growth monitoring
- Social protection: Cash transfers increase facility delivery by 20-40%
- Water/sanitation: Clean water reduces diarrheal deaths by 35%
- Transportation: Emergency transport systems reduce delays by 60%
-
Digital Health Integration (Technology-Enabled Care)
- Electronic health records: Continuity across pregnancy-delivery-postpartum
- Mobile health platforms: Appointment reminders increase ANC attendance by 25%
- Decision support systems: Clinical algorithms improve quality by 30%
- Real-time monitoring: Dashboard systems for population health indicators
- Predictive analytics: Risk scoring algorithms for early intervention
- Quality improvement: Continuous feedback loops for performance optimization
⭐ Clinical Pearl: Integrated care models achieve 30-50% better outcomes compared to fragmented services. Countries with >80% integration scores have <100 maternal deaths per 100,000 live births and <20 neonatal deaths per 1,000 live births.
| Integration Dimension | Key Components | Success Metrics | Implementation Challenges | Evidence Base |
|---|---|---|---|---|
| Vertical (Care Levels) | Referral systems, Protocols | <30min transport 90% | Resource allocation | Strong (RCTs) |
| Horizontal (Sectors) | Multi-sector coordination | 50% mortality reduction | Governance complexity | Moderate (Observational) |
| Temporal (Life Course) | Continuum care | 40% better outcomes | Service fragmentation | Strong (Cohort studies) |
| Functional (Services) | One-stop care | 25% efficiency gain | Staff training needs | Moderate (Implementation) |
| Digital (Information) | Interoperable systems | 30% quality improvement | Technology barriers | Emerging (Pilot studies) |
This integrated systems approach transforms fragmented MCH services into coordinated networks that optimize outcomes through synergistic effects and systematic quality improvement across the entire care continuum.
🌐 Integrated MCH Systems: The Multi-Dimensional Care Network
🎯 MCH Mastery Toolkit: The Clinical Excellence Arsenal
📌 Remember: MASTER - Monitoring systems, Assessment tools, Standard protocols, Target outcomes, Evidence application, Rapid response capabilities
-
Rapid Assessment Arsenal (<5 Minute Evaluations)
- MEWS (Modified Early Warning Score): >3 triggers immediate review
- Partograph: Action line crossed = immediate intervention required
- APGAR scoring: <7 at 5 minutes = resuscitation protocol
- Shock index: HR/SBP >1.0 indicates significant blood loss
- Bishop score: >8 predicts successful induction (90% success rate)
- Ballard score: Gestational age assessment ±2 weeks accuracy
-
Evidence-Based Protocol Library (Immediate Reference)
- WHO Safe Childbirth Checklist: 29 essential practices reduce mortality 10%
- ALSO protocols: Shoulder dystocia, breech delivery, postpartum hemorrhage
- NRP algorithms: Neonatal resuscitation step-by-step protocols
- Magnesium sulfate: 4-6g loading, 1-2g/hr maintenance, monitor reflexes
- Oxytocin protocols: 10 IU IM or 5-10 IU IV for PPH
- Corticosteroids: Betamethasone 12mg IM x2, 24 hours apart
-
Quality Indicator Dashboard (Performance Monitoring)
- Maternal mortality ratio: Target <70 per 100,000 live births
- Skilled birth attendance: Target >90% coverage
- Cesarean section rate: 10-15% optimal range (WHO)
- ANC 4+ visits: Target >95% coverage
- Institutional delivery: Target >90% of births
- Postnatal care: Within 48 hours for >90% of mothers
| Clinical Scenario | Assessment Tool | Time Target | Action Threshold | Success Metric |
|---|---|---|---|---|
| Labor Progress | Partograph | Continuous | Action line crossed | Normal delivery 85% |
| Maternal Deterioration | MEWS | Every 4 hours | Score >3 | Early intervention 90% |
| Neonatal Assessment | APGAR | 1 and 5 minutes | <7 at 5 minutes | Normal outcome 95% |
| Hemorrhage Risk | Shock Index | Real-time | >1.0 ratio | Prevent shock 80% |
| Preterm Risk | Bishop Score | Pre-induction | <6 unfavorable | Avoid failed induction |
💡 Master This: The "MCH Excellence Formula" = Skilled providers + Evidence-based protocols + Quality systems + Emergency preparedness + Continuous improvement. Units achieving >80% on all components have 50% lower mortality rates than average performers.
This comprehensive mastery toolkit provides the essential arsenal for expert-level MCH practice, enabling rapid assessment, evidence-based decisions, and optimal outcomes across the full spectrum of maternal and child health scenarios.
🎯 MCH Mastery Toolkit: The Clinical Excellence Arsenal
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app
























