Health Program Implementation - Action Stations!
- Core Idea: Turning health plans into real-world health services and results.
- Why it Matters: Connects policy to impact; ensures smart use of resources.
- Action Steps (📌 POAC):
- Planning: Detailed roadmaps, resource budgeting (funds, staff, supplies).
- Organizing: Building teams, defining roles, setting up communication.
- Actuating (Directing/Leading): Motivating teams, guiding execution.
- Controlling: Monitoring progress, quality checks, course correction.
- Essential Elements:
- Supervision & Monitoring: Regular oversight.
- Evaluation: Measuring success (effectiveness, efficiency, impact).
- Community Engagement: Involving people for sustainability.

⭐ The "INPUT-PROCESS-OUTPUT-OUTCOME-IMPACT" (IPO-OI) framework is fundamental for structuring the monitoring and evaluation of health programs.
Health Program Implementation - Phase Parade
Successful health program implementation unfolds through a sequence of critical phases. This systematic approach ensures efficient resource use and achievement of health objectives. 📌 Mnemonic: P-R-E-M-E
- Planning:
- Core: Needs assessment, setting clear objectives, strategy formulation.
- Logistics: Activity scheduling, detailed budgeting.
- Resource Mobilization:
- Acquiring inputs: Securing funds, skilled personnel, materials, and infrastructure.
- Execution (Implementation):
- Action phase: Putting the developed plan into operation.
- Key activities: Staff training, service delivery, community engagement.
- Monitoring:
- Continuous tracking: Program activities and outputs against set targets.
- Enables timely corrective actions if deviations occur.
- Evaluation:
- Systematic assessment: Judging program effectiveness, efficiency, impact, relevance, and sustainability.
- Common types: Formative, Process, Summative (Impact/Outcome).
⭐ Regular monitoring and periodic evaluation are crucial for adaptive management, ensuring accountability, and guiding future program improvements.
Health Program Implementation - Obstacle Odyssey
- Common Barriers:
- Resource Constraints: Funds, personnel (HRH crisis), supplies (3Ms: Money, Manpower, Material).
- Accessibility Issues: Geographic (remote areas), financial (OOP expenditure), social (caste, gender).
- Community Factors: Low awareness, cultural beliefs, poor health-seeking behavior, lack of participation.
- Management Deficiencies: Weak planning, poor supervision, inadequate Monitoring & Evaluation (M&E), lack of intersectoral coordination.
- Political & Governance: Unstable commitment, corruption, policy-implementation gap.
- Strategic Solutions:
- Decentralized Planning: Bottom-up approach, community needs assessment.
- Capacity Building: Training, skill development for workforce.
- IEC/BCC: Enhance awareness, promote Behaviour Change Communication.
- Intersectoral Collaboration: Health in All Policies approach.
- Robust M&E: Regular tracking, feedback loops, use of Health Management Information System (HMIS).
- Community Participation: Involvement of ASHA, Village Health Committees (VHCs).
- Supply Chain Management: Ensure availability of drugs & supplies.
⭐ The "implementation gap" refers to the frequent disconnect between well-formulated health policies and their actual execution on the ground, a major hurdle in achieving health goals.
Health Program Implementation - Impact Trackers
- Monitoring & Evaluation (M&E): Essential for tracking progress, ensuring accountability, and guiding improvements in health programs.
- Monitoring: Continuous tracking of inputs (e.g., funds, staff), activities (e.g., training), and outputs (e.g., people trained).
- Uses Health Management Information Systems (HMIS).
- Evaluation: Periodic assessment of outcomes (e.g., behavior change) and impact (e.g., ↓morbidity).
- Types: Formative, Summative, Process, Impact.
- Key Indicators: Quantifiable measures to assess performance.
- Input, Process, Output, Outcome, Impact.
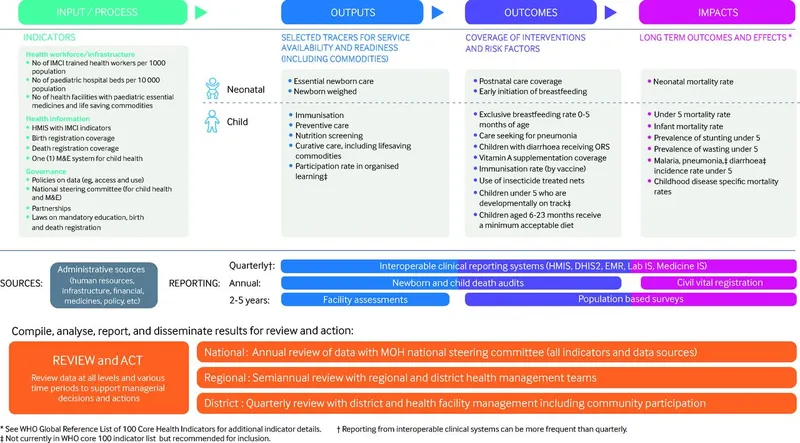
- Input, Process, Output, Outcome, Impact.
⭐ HMIS is a key tool for monitoring health programs, providing data for decision-making and course correction during implementation.
High‑Yield Points - ⚡ Biggest Takeaways
- Effective planning requires situational analysis, priority setting, and resource mobilization.
- Implementation fidelity means adherence to the program's original design.
- Monitoring & Evaluation (M&E) tracks inputs, processes, outputs, outcomes, and impact for timely adjustments.
- Active community participation is crucial for program ownership and long-term sustainability.
- Inter-sectoral coordination (e.g., with WCD, education) enhances program reach and effectiveness.
- Supportive supervision emphasizes mentoring and problem-solving over inspection.
- Efficient logistics and supply chain ensure uninterrupted service delivery.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

