Environmental Health

On this page
🌍 The Environmental Health Matrix: Where Planet Meets Patient
Environmental health operates at the critical interface between human activity and disease burden, transforming invisible exposures into measurable health outcomes. Understanding this matrix requires mastering the dose-response relationship, exposure pathways, and population-level risk assessment-concepts that predict everything from individual cancer risk to pandemic emergence patterns.
The environmental disease paradigm follows a predictable sequence: Source → Pathway → Receptor → Effect. Industrial emissions (source) travel through air currents (pathway), reach vulnerable populations (receptor), and trigger respiratory disease (effect). This framework applies universally-whether analyzing lead poisoning in children, heat-related mortality in urban islands, or vector-borne disease emergence in changing climates.
The Environmental Health Burden Landscape
Environmental risk factors demonstrate remarkable heterogeneity across disease categories and geography. In India, environmental risks account for 26% of disease burden, exceeding the global average by 3 percentage points.
- Communicable Diseases
- Unsafe water, sanitation, hygiene (WASH): 60% of diarrheal disease burden
- Indoor air pollution: 35% of acute respiratory infections in children <5 years
- Vector habitats: 100% of malaria, dengue, chikungunya transmission
- Standing water breeding sites: 80% of urban dengue cases
- Peri-domestic mosquito resting sites: 70% of malaria transmission
- Non-Communicable Diseases
- Ambient air pollution: 25% of ischemic heart disease, 24% of stroke
- Occupational carcinogens: 8-10% of all cancers globally
- Lead exposure: 12.4% of intellectual disability burden
- Blood lead >5 μg/dL: associated with 3-5 point IQ decline
- Prenatal lead exposure: 7-fold increased ADHD risk
- Injuries and Mental Health
- Road traffic environment: 40% of injury burden in urban India
- Noise pollution: 5% of ischemic heart disease in high-exposure areas
- Climate disasters: 3-fold increase in PTSD, depression in affected populations
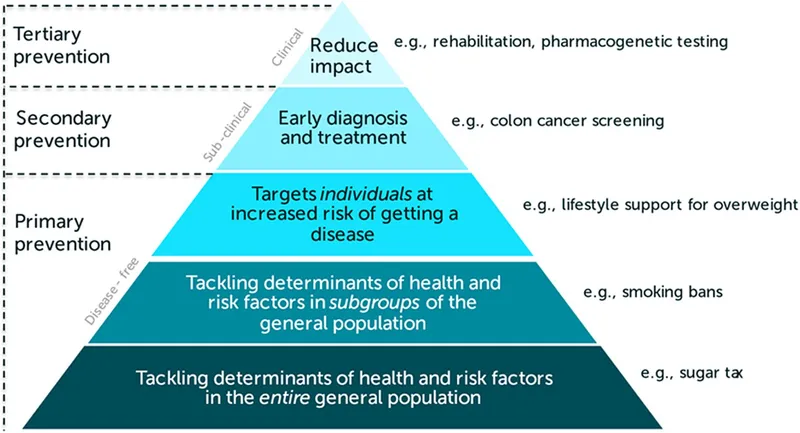
📌 Remember: SHAPE defines environmental health scope-Sanitation, Housing, Air quality, Pollution control, Exposure assessment. Each domain requires specific measurement tools, regulatory thresholds, and intervention strategies.
Exposure Assessment Architecture
Quantifying environmental exposures demands understanding biomarkers, environmental monitoring, and modeling techniques. The exposure science hierarchy progresses from crude ecological measures to sophisticated personal exposure assessment.
- Environmental Monitoring Levels
- Ambient monitoring: Fixed-site measurements (regulatory compliance)
- PM2.5 monitors: capture 24-hour or annual averages
- Noise dosimeters: measure Leq (equivalent continuous sound level)
- Water quality stations: test monthly or quarterly for contaminants
- Personal exposure: Individual-level measurement devices
- Wearable PM monitors: detect real-time exposure variability
- Noise badges: record 8-hour time-weighted averages
- Biological monitoring: blood lead, urinary metabolites
- Biomarkers of exposure: Internal dose indicators
- Lead in blood: half-life 30 days (blood), 20-30 years (bone)
- Cotinine (nicotine metabolite): half-life 16-20 hours
- Mercury in hair: integrates 3-month exposure history
- Ambient monitoring: Fixed-site measurements (regulatory compliance)
⭐ Clinical Pearl: Biomarker selection depends on exposure timeline-volatile organic compounds require immediate urine sampling (half-life <24 hours), while bone lead reflects lifetime exposure. For acute poisoning investigations, measure parent compounds; for chronic exposure surveillance, use stable metabolites with longer half-lives.
Dose-Response Relationships and Threshold Concepts
Environmental toxicology distinguishes between threshold and non-threshold effects, fundamentally shaping regulatory standards and risk assessment.
- Threshold Effects (most non-cancer outcomes)
- Reference Dose (RfD): daily exposure unlikely to cause harm over lifetime
- Threshold Limit Value (TLV): occupational exposure limit for 8-hour workday
- Safety margin: typically 10-1000 fold below observed effect level
- Uncertainty factor 10×: animal-to-human extrapolation
- Uncertainty factor 10×: intra-human variability
- Modifying factors: 1-10× based on data quality
- Non-Threshold Effects (carcinogens, mutagens)
- Linear no-threshold (LNT) model: any exposure carries proportional risk
- Cancer slope factor: risk per unit dose over lifetime
- 1 in 10,000 lifetime cancer risk: typical regulatory target
- Drinking water standards: 10⁻⁴ to 10⁻⁶ cancer risk
- Air toxics: 1 in 1 million excess lifetime cancer risk
💡 Master This: The threshold vs. non-threshold distinction drives entirely different regulatory approaches. Threshold pollutants (CO, SO₂, Pb for non-cancer effects) have "safe" ambient standards. Non-threshold carcinogens (benzene, formaldehyde, ionizing radiation) have "acceptable risk" standards-recognize this conceptual divide to understand why some pollutants have zero permissible limits while others have specific numeric standards.

The Exposure-Disease Latency Spectrum
Environmental diseases demonstrate variable latency periods between exposure and clinical manifestation, complicating outbreak investigation and requiring different surveillance strategies.
| Latency Category | Time to Disease | Example Exposures | Surveillance Method | Investigation Challenge |
|---|---|---|---|---|
| Acute | Minutes to hours | CO poisoning, chlorine gas | Emergency department syndromic | Exposure still present, source identifiable |
| Subacute | Days to weeks | Lead toxicity, pesticide poisoning | Poison control registries | Recent exposure recall, biomarkers detectable |
| Chronic | Months to years | Asbestosis, silicosis | Occupational health records | Cumulative exposure reconstruction needed |
| Latent | Decades | Mesothelioma, radiation cancer | Cancer registries | Exposure history difficult, multiple confounders |
| Transgenerational | Next generation | Endocrine disruptors, epigenetics | Birth defects surveillance | Parental exposure assessment, mechanism uncertain |
⭐ Clinical Pearl: Latency periods predict investigation feasibility-acute exposures (<24 hours) allow direct source identification, while latent diseases (>10 years) require sophisticated exposure modeling and often yield only population-level associations, not individual causation. In medicolegal cases, this distinction determines burden of proof.
Understanding these temporal relationships connects environmental monitoring data to disease surveillance, enabling predictive modeling. Elevated air pollution on Day 0 predicts emergency department visits for asthma exacerbation within 24-48 hours (lag effect), while occupational asbestos exposure requires 20-40 years before mesothelioma diagnosis.
🌍 The Environmental Health Matrix: Where Planet Meets Patient
🏭 The Pollution Paradigm: From Molecules to Morbidity
Environmental pollutants follow predictable pathways from emission source through environmental fate and transport to human exposure and biological effect. Mastering this cascade reveals why identical emissions cause different health impacts depending on meteorology, geography, and population vulnerability-knowledge that transforms raw monitoring data into actionable public health intelligence.
The pollution-to-disease pathway operates through five critical stages: emission, dispersion, transformation, exposure, and dose. Industrial SO₂ emissions (stage 1) disperse based on wind patterns and stack height (stage 2), oxidize to sulfate particles (stage 3), reach residential areas (stage 4), and deposit in respiratory tract (stage 5). Each stage offers intervention opportunities-source control, urban planning, exposure reduction, or clinical treatment.
Major Pollutant Categories and Health Fingerprints
Environmental pollutants demonstrate characteristic "health fingerprints"-specific organ systems, populations, and disease patterns that enable exposure identification from clinical presentation alone.
- Criteria Air Pollutants (ambient standards established)
- Particulate Matter (PM2.5, PM10)
- PM2.5 penetrates to alveoli: cardiovascular effects dominate
- 10 μg/m³ increase → 4-6% increased mortality
- 25 μg/m³ annual average: WHO interim target-3
- Composition matters: elemental carbon (traffic), sulfates (coal), metals (industry)
- Ozone (O₃)
- Ground-level oxidant: respiratory irritant, no safe threshold
- 8-hour average >100 μg/m³: lung function decrements
- Seasonal peak: summer photochemical reactions
- Asthmatics show effects at 50% lower concentrations
- Carbon Monoxide (CO)
- Hemoglobin affinity 240× oxygen: tissue hypoxia
- COHb >10%: headache, reduced exercise tolerance
- COHb >30%: confusion, syncope, myocardial ischemia
- 8-hour TWA limit: 9 ppm (OSHA)
- Nitrogen Dioxide (NO₂)
- Respiratory irritant: bronchial hyperreactivity
- 40 μg/m³ annual: WHO guideline, EU limit
- Indoor sources (gas stoves): 2-3× higher than outdoor
- Children exposed >30 μg/m³: 20% increased respiratory infections
- Sulfur Dioxide (SO₂)
- Bronchoconstrictive: effects within minutes in asthmatics
- 24-hour average >40 μg/m³: exacerbation threshold
- Coal combustion tracer: declining in most regions
- Lead (Pb)
- Neurotoxic: no safe blood level established (non-threshold)
- Blood Pb >5 μg/dL: CDC reference level for child intervention
- IQ decline: 2-5 points per 10 μg/dL increase
- Sources: paint (pre-1978), industrial emissions, contaminated soil
- Particulate Matter (PM2.5, PM10)

📌 Remember: PONCLS captures criteria pollutants-Particulates, Ozone, Nitrogen dioxide, Carbon monoxide, Lead, Sulfur dioxide. Each has unique emission sources, atmospheric chemistry, exposure routes, and target organs-master these patterns for rapid exposure assessment.
- Water Contaminants (chemical and biological)
- Microbial Pathogens
- E. coli O157:H7: 10-100 organisms sufficient for infection
- Cryptosporidium: chlorine-resistant, <1 μm filtration required
- Fecal coliforms: 0 CFU/100 mL for drinking water (WHO)
- Chemical Contaminants
- Arsenic: 10 μg/L WHO limit, 50 μg/L India standard (many areas exceed)
- Fluoride: 0.5-1.5 mg/L optimal, >4 mg/L causes skeletal fluorosis
- Nitrate: 50 mg/L limit (as NO₃), methemoglobinemia in infants
- Heavy metals: Pb 10 μg/L, Hg 1 μg/L, Cd 3 μg/L (WHO)
- Disinfection By-Products
- Trihalomethanes (THMs): chlorination of organic matter
- 80 μg/L total THMs: US EPA limit
- Bladder cancer risk: 10-20% increase at high exposure
- Microbial Pathogens
⭐ Clinical Pearl: Water contamination produces distinctive outbreak patterns-bacterial pathogens cause acute diarrhea within 24-72 hours affecting entire communities, viral agents (hepatitis A, rotavirus) show person-to-person spread after initial waterborne cases, while chemical contaminants produce chronic effects (arsenicosis, fluorosis) with dose-dependent severity and geographic clustering around contaminated sources.
Pollutant Fate and Transport Mechanisms
Environmental pollutants undergo transformation and movement through air, water, and soil based on physical-chemical properties, creating exposure gradients and hotspots.
-
Atmospheric Dispersion Factors
- Gaussian plume model: concentration decreases with distance, height
- Stack height: 2-3× higher reduces ground-level concentration 4-9×
- Wind speed: doubling wind reduces concentration 50%
- Atmospheric stability: inversion traps pollutants, increases concentration 10×
- Mixing height: vertical extent of dispersion
- Summer daytime: 1500-2000 m (good dispersion)
- Winter morning: 200-300 m (poor dispersion, smog events)
- Deposition mechanisms
- Dry deposition: particles >10 μm settle within km of source
- Wet deposition: rain/snow scavenging, regional to global scale
- Acid rain: SO₂ + NO₂ → H₂SO₄ + HNO₃, pH <5.0
- Gaussian plume model: concentration decreases with distance, height
-
Aquatic Transport Dynamics
- Point source discharge: industrial effluent, sewage outfall
- Dilution factor: 100-1000× within 1 km downstream (flowing water)
- Stratification: density differences prevent mixing in lakes/reservoirs
- Non-point source pollution: agricultural runoff, urban stormwater
- Accounts for 50-80% of surface water contamination
- Seasonal variation: monsoon months show 10× higher loads
- Groundwater contamination
- Flow velocity: 0.5-5 m/day (slow, persistent contamination)
- Pump-and-treat remediation: typically requires 10-30 years
- Plume migration: follows hydraulic gradient, can travel km from source
- Point source discharge: industrial effluent, sewage outfall
💡 Master This: Pollutant persistence determines exposure duration and intervention urgency. Volatile compounds (benzene, trichloroethylene) evaporate within days to weeks, requiring immediate evacuation but enabling natural attenuation. Persistent organic pollutants (PCBs, dioxins) remain for decades, bioaccumulate through food chains, and demand aggressive source removal. Heavy metals (lead, mercury) persist indefinitely, requiring permanent exposure prevention.
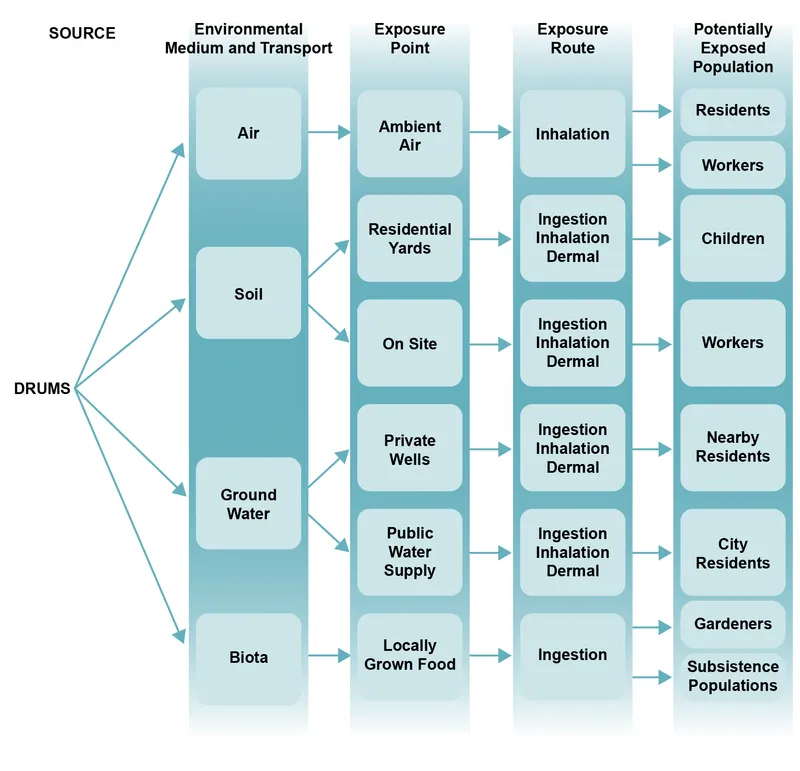
Vulnerable Population Susceptibility Patterns
Identical environmental exposures produce heterogeneous health impacts based on age, physiology, genetics, and social determinants-understanding these modifiers predicts who develops disease and guides targeted interventions.
| Population | Physiologic Vulnerability | Example Exposures | Relative Risk vs Adults | Intervention Priority |
|---|---|---|---|---|
| Infants 0-1 yr | Higher ventilation rate (per kg), immature BBB, hand-to-mouth | Lead paint dust, indoor air pollution | 3-5× higher absorption, 10× higher neurotoxicity | Home environmental assessment, WIC screening |
| Children 1-12 yr | Rapid development, higher food/water intake (per kg), play behaviors | Pesticides, air pollution, contaminated soil | 2-3× higher exposure dose, 5× higher cancer risk (lifetime) | School environment, playground soil testing |
| Pregnant women | Fetal development sensitivity, placental transfer, physiologic changes | Mercury (fish), air pollution, solvents | Fetal effects at maternal levels causing no symptoms | Occupational restrictions, dietary advice |
| Elderly >65 yr | Reduced physiologic reserve, comorbidities, medications | Heat waves, air pollution | 2-4× higher mortality during pollution episodes | Alert systems, cooling centers |
| Occupational | High-dose, prolonged exposure, inadequate protection | Asbestos, silica, pesticides, solvents | 10-100× higher exposure than general population | Engineering controls, PPE, medical surveillance |
⭐ Clinical Pearl: Children's vulnerability stems from three mechanisms-higher exposure per kilogram body weight (drink 2× more water, breathe 50% more air per kg), developmental susceptibility (rapid brain growth, immature detoxification), and longer future lifespan (more time for cancer latency). A 5-year-old exposed to carcinogens faces 10× higher lifetime cancer risk than a 50-year-old receiving identical exposure.
Genetic polymorphisms further modify susceptibility-glutathione-S-transferase (GST) null genotypes show 2-3× higher risk of benzene-related leukemia, while N-acetyltransferase-2 (NAT2) slow acetylators demonstrate increased bladder cancer risk from aromatic amines. Population screening for genetic susceptibility remains controversial but informs occupational placement in high-exposure industries.
🏭 The Pollution Paradigm: From Molecules to Morbidity
🔬 Exposure Assessment Mastery: Measuring the Invisible
Quantifying environmental exposures transforms vague concerns into precise risk estimates, enabling evidence-based interventions and regulatory decisions. Exposure assessment operates across multiple scales-from population-level ambient monitoring to individual biomarker analysis-each approach offering distinct advantages for different public health questions.
The exposure assessment hierarchy progresses from indirect to direct measurement: environmental monitoring (measures pollutant concentration in air/water/soil), exposure modeling (estimates individual contact), biomonitoring (measures internal dose), and effect biomarkers (detects early biological response). A complete exposure assessment integrates multiple approaches, cross-validating findings and building causal inference.
Environmental Monitoring Strategies and Interpretation
Ambient monitoring provides population exposure estimates but requires sophisticated interpretation to translate environmental concentrations into individual health risk.
- Air Quality Monitoring Networks
- Regulatory monitoring: compliance with National Ambient Air Quality Standards (NAAQS)
- Manual sampling: 24-hour gravimetric PM, 8-hour O₃ by UV photometry
- Continuous analyzers: real-time PM2.5 (beta-attenuation), SO₂ (UV fluorescence)
- Spatial coverage: urban areas require 1 station per 1-2 million population
- Temporal resolution: hourly for gaseous pollutants, 24-hour for particulates
- Source-oriented monitoring: identify emission contributions
- Receptor modeling: chemical mass balance, positive matrix factorization
- Speciation: elemental carbon (diesel), organic carbon (biomass), metals (industry)
- Source apportionment: typically 30-40% vehicular, 20-30% industrial, 15-25% domestic
- Personal exposure monitoring: individual-level assessment
- Wearable sensors: capture microenvironment variability (home, work, commute)
- Time-activity diaries: allocate exposure by location and duration
- Exposure contrast: personal monitoring shows 2-5× higher peak exposures than ambient stations
- Regulatory monitoring: compliance with National Ambient Air Quality Standards (NAAQS)
📌 Remember: STAMP guides air monitoring design-Spatial coverage (where to measure), Temporal resolution (how often), Analytical method (what technique), Microenvironment assessment (personal vs ambient), Pollutant selection (which contaminants). Inadequate attention to any component compromises exposure assessment validity.
- Water Quality Surveillance Architecture
- Source water monitoring: raw water before treatment
- Microbial: total coliforms, E. coli, fecal streptococci
- Chemical: pH, turbidity, heavy metals, pesticides, nitrate
- Frequency: monthly minimum, weekly during monsoon
- Distribution system monitoring: treated water at consumer tap
- Residual chlorine: 0.2-0.5 mg/L free chlorine ensures disinfection
- Coliform testing: 95% of samples must be negative (WHO)
- Sampling density: 1 sample per 5,000 population per month
- Sentinel surveillance: high-risk locations
- Schools, hospitals: vulnerable populations, high consumption
- Outbreak investigation: case-control water source comparison
- Private wells: annual testing minimum, unregulated sources
- Source water monitoring: raw water before treatment

⭐ Clinical Pearl: Water contamination detection requires understanding indicator organisms-total coliforms suggest treatment failure but not necessarily fecal contamination, E. coli confirms recent fecal pollution, while fecal streptococci indicate animal sources. Zero coliform detection doesn't guarantee safety-viruses and protozoa resist chlorination, requiring additional turbidity <1 NTU and adequate contact time (CT value) for pathogen inactivation.
Biomonitoring: From External Exposure to Internal Dose
Biological monitoring measures pollutants or metabolites in human specimens, providing direct evidence of absorption and enabling dose-response analysis.
-
Biomarker Selection Criteria
- Exposure biomarkers: measure absorbed dose
- Blood lead: reflects recent 30-day exposure plus bone stores
- Urinary cotinine: nicotine metabolite, half-life 16-20 hours
- Breath VOCs: real-time exposure to volatile organics
- Effect biomarkers: detect early biological response
- Cholinesterase activity: organophosphate pesticide exposure, 20-30% depression indicates toxicity
- Urinary 8-OHdG: oxidative DNA damage marker
- Micronucleus frequency: genotoxic exposure indicator
- Susceptibility biomarkers: identify vulnerable individuals
- G6PD deficiency: increased oxidative stress susceptibility
- CYP450 polymorphisms: altered metabolism of environmental toxicants
- Exposure biomarkers: measure absorbed dose
-
Biomonitoring Interpretation Framework
- Reference intervals: population background levels
- Blood lead: US geometric mean 0.82 μg/dL (NHANES 2015-16), 95th percentile 1.9 μg/dL
- Mercury: geometric mean 0.8 μg/L blood, 0.5 μg/g hair
- Cadmium: geometric mean 0.3 μg/L blood (non-smokers), 1.0 μg/L (smokers)
- Biological exposure indices (BEIs): occupational guidance values
- Toluene: 0.03 mg/L hippuric acid in urine (end of shift)
- Benzene: 25 μg/g creatinine S-phenylmercapturic acid
- Lead: 30 μg/dL blood (OSHA action level), 50 μg/dL (removal threshold)
- Timing considerations: match sample to exposure kinetics
- Acute poisoning: measure parent compound immediately
- Chronic exposure: use cumulative markers (hair, nails, bone)
- Workplace monitoring: end-of-shift vs end-of-week sampling
- Reference intervals: population background levels
💡 Master This: Biomarker interpretation requires understanding toxicokinetics-blood levels reflect recent exposure and are ideal for acute assessment, urinary metabolites integrate 24-hour exposure and suit workplace monitoring, while hair and nail concentrations represent weeks-to-months cumulative exposure for retrospective investigation. A negative blood lead doesn't exclude past exposure-bone lead stores 90% of body burden but requires specialized X-ray fluorescence measurement.
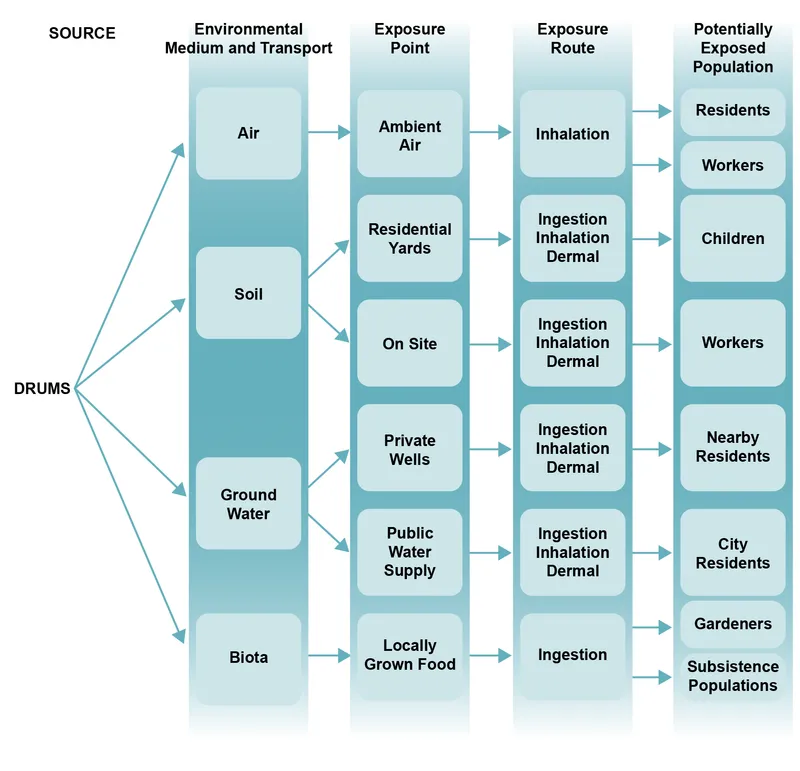
Exposure Modeling and Risk Characterization
When direct measurement is impractical, exposure modeling combines environmental data with population characteristics to estimate individual-level exposure and health risk.
| Modeling Approach | Data Requirements | Output | Uncertainty | Application |
|---|---|---|---|---|
| Microenvironment | Time-activity patterns, pollutant concentrations by location | Individual exposure estimates | Medium (20-50% CV) | Epidemiology, personal exposure prediction |
| Dispersion modeling | Emission rates, meteorology, receptor locations | Ambient concentration fields | High (factor of 2-3) | Regulatory compliance, siting decisions |
| Physiologically-based pharmacokinetic (PBPK) | Exposure dose, physiology, chemical properties | Internal tissue concentrations | Low-Medium (30-100% validation) | Risk assessment, biomarker interpretation |
| Geographic information systems (GIS) | Spatial pollution data, population density | Population exposure distribution | Medium (depends on resolution) | Environmental justice, burden estimates |
| Land-use regression | Monitoring data, traffic, land use predictors | Fine-scale concentration surfaces | Low-Medium (R² 0.6-0.8) | Epidemiology, exposure mapping |
⭐ Clinical Pearl: Exposure modeling enables retrospective exposure assessment for latent diseases (mesothelioma, radiation cancers) where historical measurements don't exist. Job-exposure matrices combine occupational history with industrial hygiene data to estimate cumulative exposure decades earlier-critical for medicolegal cases and epidemiologic studies of occupational disease.
- Risk Characterization Process
- Hazard identification: establish causal relationship (epidemiology, toxicology)
- Dose-response assessment: quantify exposure-disease relationship
- Cancer: slope factor (risk per unit dose), typically 10⁻⁴ to 10⁻⁶ target
- Non-cancer: reference dose (RfD) with uncertainty factors
- Exposure assessment: estimate population exposure distribution
- Risk calculation: integrate dose-response with exposure
- Excess lifetime cancer risk = exposure × slope factor × lifetime
- Hazard quotient = exposure / RfD (>1 indicates concern)
- Uncertainty analysis: characterize confidence bounds
- Monte Carlo simulation: propagate parameter uncertainty
- Sensitivity analysis: identify influential assumptions
The risk characterization framework transforms environmental monitoring data into actionable public health intelligence-a PM2.5 concentration of 35 μg/m³ becomes "500 excess deaths per million population annually" and "3% of total mortality attributable to air pollution," driving regulatory decisions and resource allocation.
🔬 Exposure Assessment Mastery: Measuring the Invisible
🎯 Disease Prevention Architecture: From Surveillance to Intervention
Environmental disease prevention operates through a hierarchical control framework, prioritizing upstream source elimination over downstream exposure reduction or clinical treatment. Understanding this hierarchy enables efficient resource allocation and predicts intervention effectiveness before implementation.
The prevention hierarchy follows source control > environmental engineering > administrative controls > personal protective measures > medical surveillance. Eliminating lead from gasoline (source control) prevents millions of childhood poisonings more effectively than screening programs (medical surveillance), demonstrating the exponential power of upstream interventions.
The Environmental Disease Surveillance Cascade
Environmental health surveillance integrates exposure monitoring, disease tracking, and outbreak investigation into a coherent early-warning system that detects emerging threats before widespread morbidity.
- Syndromic Surveillance Systems
- Real-time disease pattern detection: emergency department chief complaints
- Respiratory syndrome: tracks air pollution episodes, influenza, bioterrorism
- Gastrointestinal syndrome: detects waterborne outbreaks 24-48 hours faster than lab confirmation
- Neurologic syndrome: identifies pesticide poisoning clusters, heavy metal exposure
- Environmental trigger integration: link disease spikes to exposure events
- Air Quality Index (AQI) >200: predicts 15-20% increase in asthma ED visits within 24-48 hours
- Heat index >40°C: 2-3× higher heat stroke admissions, 30-40% increased cardiovascular mortality
- Water turbidity spikes: precede diarrheal outbreaks by 3-7 days
- Spatial analysis: identify geographic clusters
- SaTScan software: detects statistically significant disease clusters
- Childhood leukemia: clustering near industrial sites, hazardous waste
- Cancer registries: geographic analysis reveals environmental hotspots
- Real-time disease pattern detection: emergency department chief complaints
📌 Remember: ALERTS defines environmental surveillance components-Aggregate disease data, Link to exposures, Early warning thresholds, Rapid investigation protocols, Temporal trend analysis, Spatial cluster detection. Effective surveillance requires all six elements functioning in real-time.
- Outbreak Investigation Protocol
- Epidemic curve construction: visualize outbreak dynamics
- Point-source: sharp peak, narrow distribution (contaminated food/water)
- Continuous common source: plateau pattern (ongoing exposure)
- Propagated: successive peaks at incubation interval (person-to-person)
- Case definition: standardize inclusion criteria
- Confirmed: laboratory evidence + clinical + exposure
- Probable: clinical + exposure, no lab
- Suspected: clinical only, under investigation
- Analytical epidemiology: identify exposure-disease associations
- Case-control study: compare exposures between cases and controls
- Cohort study: follow exposed vs unexposed for disease development
- Odds ratio >2.0 or relative risk >2.0: suggests causal association
- Confidence interval excludes 1.0: statistically significant
- Epidemic curve construction: visualize outbreak dynamics
⭐ Clinical Pearl: Environmental outbreak investigation differs from infectious disease outbreaks-geographic clustering around pollution sources is stronger than person-to-person transmission patterns, dose-response gradients (higher exposure → more severe disease) support causality, and temporal relationships between exposure events and disease onset (lag period) provide critical evidence. A cholera outbreak linked to a contaminated well shows tight geographic clustering, while person-to-person spread would show household secondary cases.
Intervention Hierarchy and Effectiveness Metrics
Environmental interventions follow a predictable effectiveness hierarchy, with source elimination achieving 10-100× greater impact than personal protection strategies.
-
Source Control Interventions (most effective)
- Regulatory elimination: ban hazardous substances
- Lead gasoline phase-out: US blood lead declined 75% (1976-1991)
- Asbestos ban: mesothelioma incidence declining 20 years post-ban
- DDT prohibition: environmental persistence but human levels decreased 90%
- Cleaner production: substitute safer alternatives
- Unleaded gasoline: eliminated >90% of childhood lead poisoning
- CFC replacement: ozone layer recovery on track for 2050
- Mercury-free batteries: reduced environmental mercury 50%
- Emission controls: reduce pollutant release
- Catalytic converters: decreased vehicle CO by 90%, NOx by 75%
- Flue gas desulfurization: removes 95% of SO₂ from coal plants
- Electrostatic precipitators: capture >99% of particulate emissions
- Regulatory elimination: ban hazardous substances
-
Engineering Controls (highly effective)
- Water treatment: multi-barrier approach
- Coagulation-flocculation: removes 70-90% of particles, pathogens
- Filtration: >99.9% removal of Giardia, Cryptosporidium (1 μm filters)
- Chlorination: 99.99% bacterial inactivation at 0.5 mg/L residual, 30 min contact
- Advanced treatment: activated carbon (organics), reverse osmosis (dissolved solids)
- Ventilation systems: dilute indoor air pollution
- Air changes per hour (ACH): 8-12 ACH for laboratories, 15-20 ACH for infectious isolation
- Local exhaust: captures 90-95% of contaminants at source
- HEPA filtration: removes 99.97% of particles ≥0.3 μm
- Noise barriers: attenuate sound transmission
- Highway barriers: 10-15 dB reduction for nearby residents
- Building insulation: 20-30 dB reduction with proper design
- Distance doubling: 6 dB reduction for point sources
- Water treatment: multi-barrier approach
💡 Master This: The intervention hierarchy reflects reliability and sustainability-source elimination requires no behavior change and protects entire populations permanently, while personal protective equipment demands continuous compliance, fails unpredictably, and protects only users. When designing environmental health programs, exhaust higher-level interventions before resorting to lower-level approaches. A respirator program (PPE) is the intervention of last resort when source control and ventilation (engineering) are infeasible.
| Intervention Type | Population Protected | Sustainability | Cost-Effectiveness | Example | Failure Mode |
|---|---|---|---|---|---|
| Source elimination | 100% (entire population) | Permanent | High (one-time investment) | Lead gasoline ban | Illegal use, legacy contamination |
| Engineering control | 95-99% (facility/community) | Long-term (maintenance required) | High | Water chlorination | Equipment failure, power outage |
| Administrative control | 50-80% (compliant individuals) | Medium (requires monitoring) | Medium | Exposure time limits | Non-compliance, enforcement gaps |
| Personal protective equipment | 30-70% (users only) | Low (user-dependent) | Low | Respirator use | Improper fit, inconsistent use |
| Medical surveillance | 0% prevention (detects disease) | Ongoing | Low (identifies cases, doesn't prevent) | Blood lead screening | Late detection, irreversible effects |
Regulatory Frameworks and Compliance Monitoring
Environmental health regulations establish enforceable standards, but effectiveness depends on monitoring, enforcement, and penalty structures.
- Standard-Setting Approaches
- Health-based standards: protect public health with adequate safety margin
- NAAQS: set to protect sensitive populations (children, elderly, asthmatics)
- Maximum Contaminant Levels (MCLs): drinking water standards
- Permissible Exposure Limits (PELs): occupational air contaminants
- Technology-based standards: require best available control technology
- BACT (Best Available Control Technology): new sources
- MACT (Maximum Achievable Control Technology): hazardous air pollutants
- RACT (Reasonably Available Control Technology): existing sources
- Risk-based standards: balance health protection with feasibility
- Cancer risk: typically 10⁻⁴ to 10⁻⁶ lifetime excess risk
- Cost-benefit analysis: required for major regulations
- Feasibility assessment: technological and economic considerations
- Health-based standards: protect public health with adequate safety margin
⭐ Clinical Pearl: Regulatory standards represent political compromises, not pure health science-WHO air quality guidelines (health-based) are often 2-3× stricter than national standards (feasibility-adjusted). When assessing environmental health risks, reference health-based guidelines for true safety thresholds, recognizing that legal compliance doesn't guarantee health protection. India's PM2.5 standard (40 μg/m³ annual) exceeds WHO guideline (5 μg/m³) by 8-fold, reflecting feasibility constraints rather than health evidence.
- Compliance and Enforcement Mechanisms
- Self-monitoring and reporting: industry submits emission/effluent data
- Continuous emission monitoring systems (CEMS): real-time pollutant tracking
- Discharge monitoring reports (DMRs): monthly water quality data
- Accuracy: ±20% for most parameters, subject to audit
- Government inspections: verify compliance, investigate complaints
- Routine inspections: annual for major sources, every 2-3 years for minor
- Stack testing: annual or biennial emission measurements
- Violation rates: typically 10-20% of facilities in non-compliance
- Penalties and enforcement: deter violations
- Administrative penalties: ₹10,000-1 lakh per day (India)
- Criminal prosecution: serious or repeat violations
- Facility closure: persistent non-compliance
- Self-monitoring and reporting: industry submits emission/effluent data
The regulatory framework connects environmental monitoring to enforceable action-ambient PM2.5 exceeding NAAQS triggers State Implementation Plan requirements, mandating emission reductions to achieve compliance within 5-10 years. This structure transforms environmental health science into policy action.
[[Chapter
🎯 Disease Prevention Architecture: From Surveillance to Intervention
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app





