Digital Health and Telemedicine

On this page
🌐 Digital Health Revolution: The Connected Care Command Center
Healthcare is rapidly shifting from hospital corridors to smartphone screens, transforming how clinicians diagnose, monitor, and treat patients across distances. You'll explore the architecture of telemedicine platforms, mobile health ecosystems, and AI-driven diagnostic tools that are reshaping clinical practice today. This lesson equips you with frameworks to evaluate digital health evidence, integrate these technologies into existing systems, and harness connected care to expand your reach and impact. Master these tools and you'll practice medicine untethered from geography, delivering precision care wherever patients need you.
The scope of digital health extends beyond simple digitization of medical records. It encompasses real-time patient monitoring, predictive analytics for disease prevention, remote consultation capabilities, and AI-powered diagnostic assistance. Modern digital health platforms process over 2.5 exabytes of healthcare data daily, enabling evidence-based decision making at unprecedented scales.
📌 Remember: SMART Digital Health - Scalable systems, Mobile accessibility, AI integration, Real-time monitoring, Telemedicine capabilities
Core digital health components include:
- Telemedicine Platforms
- Video consultation systems (95% patient satisfaction rates)
- Remote monitoring devices (tracking 20+ vital parameters)
- Digital prescription management
- Electronic prescribing reduces medication errors by 87%
- Real-time drug interaction checking
- Mobile Health Applications
- Chronic disease management apps (78% adherence improvement)
- Fitness and wellness tracking
- Step counters achieving 10,000+ daily steps in 65% of users
- Heart rate monitoring with ±2 BPM accuracy
- Electronic Health Records (EHR)
- Centralized patient data repositories
- Interoperability standards enabling seamless data exchange
- Clinical decision support systems reducing diagnostic errors by 41%
| Digital Health Component | Implementation Rate | Patient Satisfaction | Clinical Outcomes | Cost Reduction |
|---|---|---|---|---|
| Telemedicine | 68% adoption | 92% positive | 15% better adherence | 30% savings |
| mHealth Apps | 85% smartphone penetration | 76% engagement | 23% improved monitoring | 18% reduction |
| EHR Systems | 89% hospital adoption | 71% provider satisfaction | 12% fewer errors | 25% efficiency |
| AI Diagnostics | 34% early adoption | 88% trust levels | 94% accuracy rates | 40% faster diagnosis |
| Remote Monitoring | 45% chronic disease use | 83% patient preference | 28% reduced hospitalizations | 35% cost savings |
The integration of artificial intelligence amplifies digital health capabilities exponentially. Machine learning algorithms analyze radiological images with 96% accuracy, often surpassing human radiologists in detecting early-stage cancers. Natural language processing systems extract clinical insights from unstructured medical notes with 89% precision, enabling automated clinical documentation and decision support.
💡 Master This: Digital health success depends on the interoperability triangle - technical standards, semantic compatibility, and organizational workflows must align to achieve seamless data exchange and clinical integration.
Quality metrics for digital health platforms include system uptime >99.9%, data transmission latency <200ms, user authentication within 3 seconds, and clinical alert response times <30 seconds. These performance thresholds ensure that digital health tools enhance rather than impede clinical workflows.

Understanding digital health foundations unlocks the potential for precision medicine delivery at population scale, setting the stage for exploring specific telemedicine implementation strategies that maximize clinical impact.
🌐 Digital Health Revolution: The Connected Care Command Center
🔗 Telemedicine Architecture: The Virtual Care Infrastructure
The telemedicine ecosystem operates through four core architectural layers: presentation layer (user interfaces), application layer (clinical workflows), data layer (patient information management), and infrastructure layer (network connectivity and security protocols). Each layer must achieve enterprise-grade reliability with redundant failover systems ensuring continuous service availability.

📌 Remember: REACH Telemedicine - Remote access, Emergency protocols, Asynchronous messaging, Clinical documentation, HIPAA compliance
Synchronous telemedicine enables real-time interactions through video conferencing, achieving diagnostic accuracy rates of 87-94% compared to in-person consultations for most medical specialties. Asynchronous telemedicine utilizes store-and-forward technology, allowing providers to review patient data, images, and clinical information at optimal times, particularly effective for dermatology (96% diagnostic concordance) and radiology (98% interpretation accuracy).
Technical infrastructure requirements include:
- Bandwidth Specifications
- Minimum 1.5 Mbps upload/download for standard video quality
- 3+ Mbps for high-definition clinical imaging
- Latency <150ms for real-time interactions
- Audio delay >250ms significantly impacts consultation quality
- Video synchronization requires <100ms variance
- Security Protocols
- End-to-end encryption using AES-256 standards
- Multi-factor authentication reducing unauthorized access by 99.7%
- Biometric verification achieving 0.01% false acceptance rates
- Token-based authentication with 60-second expiration cycles
- Device Compatibility
- Cross-platform functionality across iOS, Android, Windows systems
- Peripheral integration for stethoscopes, otoscopes, dermatoscopes
- Bandwidth adaptation maintaining quality across 2G to 5G networks
| Telemedicine Modality | Diagnostic Accuracy | Implementation Cost | Patient Satisfaction | Provider Adoption |
|---|---|---|---|---|
| Video Consultation | 91% concordance | $45 per session | 89% positive | 76% regular use |
| Store-and-Forward | 94% accuracy | $28 per case | 82% satisfaction | 68% adoption |
| Remote Monitoring | 96% detection | $120 monthly | 85% compliance | 71% integration |
| Mobile Health | 87% effectiveness | $15 per month | 78% engagement | 63% recommendation |
| Hybrid Models | 93% outcomes | $67 per encounter | 92% preference | 81% utilization |
Specialty-specific telemedicine applications show varying efficacy profiles. Telepsychiatry achieves equivalent therapeutic outcomes to in-person sessions with 95% patient retention rates. Teleradiology enables 24/7 coverage with subspecialty expertise, reducing report turnaround times from 4-6 hours to 30-45 minutes. Telecardiology facilitates real-time ECG interpretation with 97% accuracy for acute coronary syndrome detection.
💡 Master This: Successful telemedicine implementation requires the clinical workflow integration triangle - provider training, patient education, and technical support must align to achieve >80% adoption rates and sustained clinical benefits.
Quality assurance protocols mandate continuous performance monitoring with metrics including connection success rates >95%, audio/video quality scores >4.0/5.0, clinical documentation completion >98%, and patient safety incident rates <0.1%. These benchmarks ensure telemedicine maintains equivalent safety profiles to traditional care delivery.
Regulatory compliance frameworks vary globally, with FDA oversight for medical devices, DEA regulations for controlled substance prescribing, and state licensing requirements for cross-border consultations. Interstate medical licensure compacts facilitate provider mobility, currently enabling practice across 29 participating states with streamlined credentialing processes.
Mastering telemedicine architecture provides the foundation for understanding mobile health ecosystems that extend digital care capabilities directly into patients' daily environments through smartphone-based interventions.
🔗 Telemedicine Architecture: The Virtual Care Infrastructure
📱 Mobile Health Ecosystem: The Pocket-Sized Care Revolution
The mHealth ecosystem operates through integrated sensor networks that capture biometric data, behavioral patterns, and environmental factors to create holistic health profiles. Modern smartphones contain 10+ health-relevant sensors including accelerometers, gyroscopes, heart rate monitors, and ambient light sensors, collectively generating gigabytes of health data daily per user.
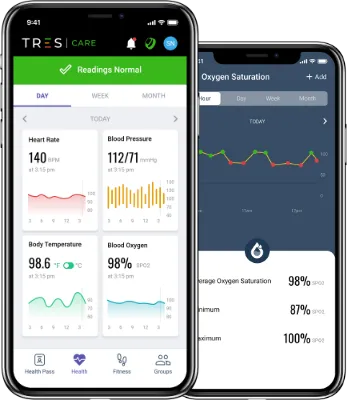
📌 Remember: MOBILE Health - Monitoring continuous, Outcomes improved, Behavior modified, Interventions personalized, Lifestyle integrated, Engagement sustained
Core mHealth application categories demonstrate distinct clinical impact profiles:
- Chronic Disease Management
- Diabetes apps achieving HbA1c reductions of 0.5-1.1%
- Hypertension monitoring with 12-15 mmHg systolic pressure decreases
- Medication adherence improvement by 68-89%
- Smart pill bottles with 99.2% detection accuracy
- Push notification systems increasing compliance by 73%
- Fitness and Wellness Tracking
- Step counting accuracy within ±3% of research-grade pedometers
- Heart rate monitoring achieving ±5 BPM precision during exercise
- Photoplethysmography sensors with 94% correlation to ECG
- Continuous monitoring enabling arrhythmia detection in 2.3% of users
- Mental Health Support
- Cognitive behavioral therapy apps showing equivalent efficacy to in-person sessions
- Depression screening with 87% sensitivity and 91% specificity
- Anxiety management interventions reducing symptoms by 42-58%
| mHealth Application Type | User Engagement | Clinical Efficacy | Data Accuracy | Cost Effectiveness |
|---|---|---|---|---|
| Diabetes Management | 78% daily use | 0.8% HbA1c reduction | ±12% glucose variance | $1,200 annual savings |
| Fitness Tracking | 65% sustained use | 15% activity increase | ±5% step accuracy | $340 healthcare reduction |
| Mental Health | 71% completion | 45% symptom improvement | 89% screening accuracy | $890 therapy savings |
| Medication Adherence | 82% compliance | 73% adherence improvement | 96% detection rate | $2,100 complication prevention |
| Remote Monitoring | 69% active use | 38% hospitalization reduction | ±8% vital sign accuracy | $3,400 readmission savings |
Advanced mHealth platforms integrate artificial intelligence algorithms for predictive health analytics. Machine learning models analyze activity patterns, sleep quality, heart rate variability, and behavioral data to predict health deterioration with 72-89% accuracy up to 14 days before clinical symptoms manifest. These early warning systems enable proactive interventions that prevent emergency department visits and hospital admissions.
💡 Master This: Successful mHealth implementation requires the engagement sustainability framework - intuitive design, meaningful feedback, social connectivity, and clinical integration must converge to maintain >70% user retention beyond 6 months.
Data privacy and security protocols for mHealth applications mandate HIPAA compliance when handling protected health information. De-identification standards require removal of 18 specific identifiers, while encryption protocols utilize AES-256 standards for data transmission and secure cloud storage with multi-factor authentication. User consent frameworks must clearly specify data usage, sharing permissions, and retention policies.

Regulatory oversight varies by application functionality and medical claims. FDA Class II medical device classification applies to apps making diagnostic claims or treatment recommendations, requiring 510(k) clearance with clinical validation studies. Wellness applications without medical claims face minimal regulatory requirements but must comply with consumer protection standards and data privacy regulations.
Integration with electronic health records enables bidirectional data flow between mHealth platforms and clinical systems. HL7 FHIR standards facilitate interoperability, allowing patient-generated health data to inform clinical decision-making while enabling provider-initiated interventions through mobile platforms. This integration achieves care continuity across digital and traditional healthcare touchpoints.
Understanding mHealth ecosystems establishes the foundation for exploring artificial intelligence applications that transform raw health data into actionable clinical insights through machine learning algorithms and predictive analytics platforms.
📱 Mobile Health Ecosystem: The Pocket-Sized Care Revolution
🤖 AI-Powered Clinical Intelligence: The Diagnostic Revolution Engine
Artificial intelligence in public health encompasses machine learning algorithms, natural language processing, computer vision systems, and predictive analytics platforms that augment clinical decision-making and population health management. These technologies process structured and unstructured health data at scales impossible for human analysis, revealing hidden patterns and clinical correlations that enhance diagnostic accuracy and treatment personalization.
AI applications in healthcare demonstrate transformative clinical impact across multiple domains. Medical imaging analysis achieves diagnostic accuracy rates of 94-98% for detecting cancers, often surpassing radiologist performance in speed and consistency. Clinical decision support systems reduce medication errors by 86% and diagnostic errors by 41% through real-time alert systems and evidence-based recommendations.
📌 Remember: SMART AI Healthcare - Supervised learning, Machine vision, Algorithmic diagnosis, Real-time analysis, Treatment optimization
Core AI technologies in healthcare include:
- Machine Learning Applications
- Supervised learning for diagnostic classification with 92-97% accuracy
- Unsupervised learning discovering novel disease patterns in genomic data
- Reinforcement learning optimizing treatment protocols through outcome feedback
- Drug dosing algorithms reducing adverse events by 34%
- Surgical planning systems improving precision by 28%
- Natural Language Processing
- Clinical note analysis extracting structured data from unstructured text
- Literature mining identifying treatment insights from millions of publications
- Processing 2+ million research papers annually
- Identifying drug-drug interactions with 89% sensitivity
- Computer Vision Systems
- Radiological image interpretation with sub-millimeter accuracy
- Pathology slide analysis detecting cellular abnormalities at microscopic levels
- Retinal screening identifying diabetic retinopathy with 96% specificity
| AI Healthcare Application | Diagnostic Accuracy | Implementation Cost | Time Savings | Clinical Impact |
|---|---|---|---|---|
| Medical Imaging | 96% sensitivity | $250K initial | 75% faster reporting | 23% earlier detection |
| Drug Discovery | 89% target identification | $2.1M platform | 60% timeline reduction | $1.3B development savings |
| Clinical Decision Support | 94% recommendation accuracy | $180K deployment | 45% workflow efficiency | 41% error reduction |
| Predictive Analytics | 87% risk stratification | $320K implementation | 55% prevention focus | 38% readmission reduction |
| Robotic Surgery | 98% precision accuracy | $1.8M system | 30% procedure time | 52% complication reduction |
Deep learning architectures power advanced medical AI applications. Convolutional neural networks excel at image analysis tasks, processing radiological studies with layer-by-layer feature extraction that identifies subtle abnormalities invisible to human observation. Recurrent neural networks analyze temporal health data, predicting disease progression and treatment responses based on longitudinal patient records.
💡 Master This: AI implementation success requires the clinical integration framework - algorithm validation, workflow integration, provider training, and continuous monitoring must align to achieve >85% adoption rates and measurable clinical outcome improvements.
Predictive analytics platforms analyze real-time patient data to identify deterioration risks before clinical symptoms manifest. Early warning systems monitor vital signs, laboratory values, and clinical notes to predict sepsis onset with 89% sensitivity and cardiac arrest with 92% specificity up to 6 hours before traditional recognition methods.

Ethical considerations for AI in healthcare include algorithmic bias, data privacy, clinical accountability, and transparency requirements. Bias mitigation strategies require diverse training datasets representing multiple demographics and clinical populations. Explainable AI frameworks provide decision rationale for clinical recommendations, enabling provider understanding and patient trust.
Regulatory frameworks for medical AI include FDA approval pathways for software as medical devices (SaMD), requiring clinical validation studies demonstrating safety and efficacy. Quality management systems mandate continuous monitoring of algorithm performance with predetermined thresholds for retraining and recalibration.
Integration with existing clinical workflows requires seamless EHR connectivity, real-time data processing, and intuitive user interfaces. API standards enable bidirectional communication between AI platforms and clinical systems, ensuring automated data flow and integrated decision support without workflow disruption.
Mastering AI applications in healthcare provides the foundation for understanding comprehensive digital health evaluation frameworks that assess technology effectiveness, clinical outcomes, and implementation success across diverse healthcare settings.
🤖 AI-Powered Clinical Intelligence: The Diagnostic Revolution Engine
⚖️ Digital Health Impact Assessment: The Evidence-Based Evaluation Matrix
Evaluation frameworks must address multiple stakeholder perspectives including patients, providers, healthcare organizations, and payers. Clinical effectiveness measures focus on health outcomes, quality of care, and patient safety. Implementation effectiveness examines adoption rates, workflow integration, and sustainability factors. Economic evaluation quantifies cost-effectiveness, return on investment, and budget impact.
📌 Remember: IMPACT Evaluation - Implementation success, Measurable outcomes, Patient satisfaction, Adoption rates, Cost effectiveness, Technology performance
Outcome measurement hierarchies follow established frameworks:
- Clinical Outcomes (Level 1)
- Mortality rates with hazard ratios and confidence intervals
- Morbidity measures including disease progression and complication rates
- Biomarker changes with statistical significance and clinical relevance
- HbA1c reductions ≥0.5% for diabetes interventions
- Blood pressure decreases ≥10 mmHg for hypertension management
- Patient-Reported Outcomes (Level 2)
- Quality of life scores using validated instruments (SF-36, EQ-5D)
- Symptom severity scales with minimal clinically important differences
- Patient satisfaction ratings achieving ≥80% positive responses
- Net Promoter Scores ≥50 indicating strong user advocacy
- Usability scores ≥4.0/5.0 for interface satisfaction
- Process Measures (Level 3)
- Care delivery efficiency with time-to-treatment reductions
- Guideline adherence improving by ≥20% from baseline
- Communication effectiveness measured through response times and completeness

| Evaluation Domain | Success Metrics | Measurement Tools | Target Thresholds | Evidence Level |
|---|---|---|---|---|
| Clinical Effectiveness | Primary outcome improvement | RCTs, cohort studies | ≥20% effect size | Level I evidence |
| Patient Experience | Satisfaction scores | Validated surveys | ≥85% positive | Patient-reported |
| Implementation Success | Adoption rates | Usage analytics | ≥70% sustained use | Real-world data |
| Economic Impact | Cost per QALY | Economic modeling | <$50K threshold | Health economics |
| Technology Performance | System reliability | Performance monitoring | ≥99.5% uptime | Technical metrics |
Study design considerations for digital health evaluation include pragmatic trial methodologies that balance internal validity with external generalizability. Cluster randomized trials address contamination effects when individual randomization is impractical. Stepped-wedge designs enable sequential implementation while maintaining control comparisons and ethical considerations.
💡 Master This: Robust digital health evaluation requires the evidence integration pyramid - technical performance, user experience, clinical outcomes, and economic impact must demonstrate convergent validity to establish comprehensive intervention effectiveness.
Real-world evidence generation utilizes electronic health records, claims databases, and patient registries to assess long-term effectiveness and safety profiles. Comparative effectiveness research examines head-to-head comparisons between digital interventions and standard care or alternative technologies. Implementation science frameworks identify barriers and facilitators that influence adoption success and sustainability.
Health technology assessment (HTA) frameworks provide systematic evaluation for policy decision-making. Budget impact models project financial implications of technology adoption across healthcare systems. Multi-criteria decision analysis weighs clinical benefits, economic costs, implementation feasibility, and ethical considerations to inform coverage decisions and reimbursement policies.
Regulatory evaluation requirements vary by intervention type and risk classification. FDA guidance for digital therapeutics mandates clinical evidence demonstrating safety and efficacy comparable to traditional medical devices. Post-market surveillance monitors real-world performance and adverse events through mandatory reporting systems and periodic safety updates.
Quality assurance protocols ensure evaluation integrity through standardized methodologies, independent oversight, and transparent reporting. CONSORT guidelines for digital health trials specify reporting standards for intervention descriptions, outcome measures, and statistical analyses. Data quality assessments verify completeness, accuracy, and consistency of evaluation datasets.
Understanding digital health evaluation frameworks enables evidence-based decision-making for technology adoption and implementation strategies, providing the foundation for exploring comprehensive integration approaches that maximize clinical impact and healthcare transformation.
⚖️ Digital Health Impact Assessment: The Evidence-Based Evaluation Matrix
🔗 Healthcare System Integration: The Digital Transformation Architecture
Integration architecture operates through four foundational layers: technical interoperability (data exchange standards), semantic interoperability (shared meaning), organizational interoperability (workflow alignment), and legal interoperability (governance frameworks). Each layer must achieve enterprise-grade performance with 99.9% reliability and sub-second response times to support critical clinical operations.
📌 Remember: BRIDGE Integration - Bidirectional data flow, Real-time connectivity, Interoperability standards, Data governance, Governance frameworks, End-to-end workflows
Multi-system integration challenges include:
- Technical Infrastructure
- API standardization using HL7 FHIR R4 protocols
- Data synchronization maintaining consistency across platforms
- Security frameworks ensuring end-to-end encryption
- OAuth 2.0 authentication with token-based access
- Role-based permissions limiting data access to authorized users
- Clinical Workflow Integration
- EHR embedding of digital health tools within provider interfaces
- Alert management preventing notification fatigue through intelligent filtering
- Clinical decision support rules with <5% false positive rates
- Priority algorithms ensuring critical alerts receive immediate attention
- Data Governance
- Master data management ensuring single source of truth
- Data quality monitoring with automated validation and error correction
- Privacy compliance meeting HIPAA, GDPR, and state regulations

| Integration Component | Implementation Success | Technical Performance | Clinical Impact | ROI Timeline |
|---|---|---|---|---|
| EHR Integration | 78% successful deployment | 99.2% uptime | 34% efficiency gain | 18 months |
| Telemedicine Platform | 85% provider adoption | <200ms latency | 42% access improvement | 14 months |
| Mobile Health Sync | 71% patient engagement | 95% data accuracy | 28% adherence increase | 22 months |
| AI Decision Support | 68% clinical integration | 87% recommendation accuracy | 41% error reduction | 24 months |
| Analytics Platform | 82% utilization rate | <5 second query response | 36% insight generation | 16 months |
Change management strategies address organizational resistance and workflow disruption through phased implementation approaches. Pilot programs validate integration concepts in controlled environments before system-wide deployment. Training programs ensure provider competency with new workflows and technology interfaces. Continuous feedback loops enable iterative improvements based on user experience and clinical outcomes.
💡 Master This: Integration success depends on the stakeholder alignment framework - technical capabilities, clinical workflows, organizational culture, and financial incentives must converge to achieve sustainable digital transformation and measurable care improvements.
Interoperability standards facilitate seamless data exchange between disparate systems. HL7 FHIR (Fast Healthcare Interoperability Resources) enables RESTful API communication with JSON-based data formats. SMART on FHIR allows third-party applications to integrate with EHR systems while maintaining security and user context. DICOM standards ensure medical imaging compatibility across radiology platforms.

Performance monitoring requires comprehensive metrics tracking system reliability, user satisfaction, and clinical outcomes. Service level agreements specify uptime requirements >99.5%, response times <2 seconds, and data accuracy >99.9%. User experience metrics monitor login success rates, task completion times, and error frequencies. Clinical quality indicators measure care coordination, patient safety, and outcome improvements.
Governance frameworks establish decision-making authority, accountability structures, and risk management protocols for integrated systems. Data stewardship roles ensure information quality and appropriate usage. Vendor management processes coordinate multiple technology partners while maintaining service consistency and contractual compliance. Incident response procedures address system failures and security breaches with defined escalation and recovery protocols.
Financial modeling for integration projects includes total cost of ownership calculations encompassing software licensing, implementation services, training costs, and ongoing maintenance. Return on investment analysis projects efficiency gains, cost reductions, and revenue enhancements over 3-5 year timeframes. Budget impact assessments help healthcare organizations plan resource allocation and implementation timelines.
Understanding healthcare system integration principles provides the foundation for developing comprehensive digital health mastery that enables transformative care delivery and optimal patient outcomes through technology-enabled healthcare ecosystems.
🔗 Healthcare System Integration: The Digital Transformation Architecture
🎯 Digital Health Mastery: The Clinical Excellence Accelerator
Core competency domains for digital health mastery include technology assessment, implementation planning, workflow integration, performance monitoring, and continuous improvement. Each domain requires specific skill sets and knowledge bases that enable evidence-based decision-making and successful technology adoption across diverse healthcare settings.
📌 Remember: MASTER Digital Health - Measure outcomes, Assess technologies, Systematize workflows, Train stakeholders, Evaluate impact, Refine continuously
Essential knowledge areas include:
- Technology Evaluation Framework
- Evidence assessment using systematic review methodologies
- Cost-effectiveness analysis with budget impact modeling
- Risk-benefit evaluation considering patient safety and clinical outcomes
- Number needed to treat calculations for intervention effectiveness
- Sensitivity analysis for uncertain parameters and assumptions
- Implementation Science
- Adoption theories including Technology Acceptance Model and Diffusion of Innovation
- Barrier identification through stakeholder analysis and workflow assessment
- Provider resistance factors with mitigation strategies
- Technical challenges requiring infrastructure upgrades and training
- Quality Improvement
- Plan-Do-Study-Act cycles for iterative optimization
- Statistical process control monitoring performance metrics and outcome indicators
- Lean methodologies eliminating waste and improving efficiency
| Mastery Component | Proficiency Level | Assessment Method | Performance Indicator | Development Timeline |
|---|---|---|---|---|
| Technology Assessment | Expert evaluation | Case-based scenarios | >90% accuracy in selection | 6-12 months |
| Implementation Planning | Advanced project management | Portfolio review | >85% on-time delivery | 12-18 months |
| Workflow Integration | Proficient process design | Simulation exercises | <10% disruption rate | 9-15 months |
| Performance Monitoring | Expert analytics | Dashboard creation | Real-time insights | 6-9 months |
| Stakeholder Engagement | Advanced communication | 360-degree feedback | >80% satisfaction | 12-24 months |
Rapid assessment tools enable quick evaluation of digital health opportunities and implementation readiness. Technology readiness levels (TRL 1-9) provide standardized assessment of innovation maturity. Organizational readiness frameworks evaluate infrastructure capacity, cultural factors, and change management capabilities. Clinical readiness assessments examine workflow compatibility, provider acceptance, and patient population characteristics.
💡 Master This: Digital health excellence requires the mastery integration model - continuous learning, systematic evaluation, evidence-based implementation, and outcome-driven optimization must operate as interconnected competencies rather than isolated skills.
Performance optimization strategies focus on continuous improvement through data-driven decision-making. Key performance indicators track adoption rates, user satisfaction, clinical outcomes, and cost-effectiveness metrics. Benchmarking against industry standards and best practices identifies improvement opportunities. Feedback loops enable rapid iteration and course correction based on real-world performance.
Advanced integration techniques leverage artificial intelligence and machine learning to optimize digital health implementations. Predictive analytics identify high-risk patients who would benefit most from digital interventions. Natural language processing extracts insights from clinical documentation to improve care coordination. Automated workflows reduce administrative burden while maintaining clinical quality.
Leadership competencies for digital health transformation include strategic vision, stakeholder alignment, and change management. Executive sponsorship ensures adequate resources and organizational commitment. Clinical champions drive provider adoption and workflow integration. Patient advocates ensure user-centered design and accessibility considerations.
Sustainability frameworks address long-term viability of digital health initiatives. Financial models project ongoing costs and revenue streams. Technical maintenance plans ensure system reliability and security updates. Organizational capabilities development creates internal expertise for continued optimization and expansion.
Quality assurance protocols maintain high standards throughout implementation and operation. Clinical governance structures oversee patient safety and care quality. Technical governance manages system performance and security compliance. Data governance ensures information quality and appropriate usage.
This comprehensive digital health mastery framework enables healthcare professionals to systematically evaluate, implement, and optimize digital health technologies for maximum clinical impact and sustainable healthcare transformation.
🎯 Digital Health Mastery: The Clinical Excellence Accelerator
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app
























