Vitamin D Synthesis - Sunshine Power-Up
- Skin: UVB (290-315nm) converts 7-Dehydrocholesterol to Cholecalciferol (D3).
- Liver: Cholecalciferol → 25-Hydroxycholecalciferol (Calcidiol) via 25-hydroxylase. Major circulating form.
- Kidney: Calcidiol → 1,25-Dihydroxycholecalciferol (Calcitriol) via 1α-hydroxylase (CYP27B1). Active form.
- 1α-hydroxylase stimulated by: PTH, ↓$Ca^{2+}$, ↓$PO_4^{3-}$.
- Inhibited by: FGF-23, ↑$Ca^{2+}$, ↑$PO_4^{3-}$.
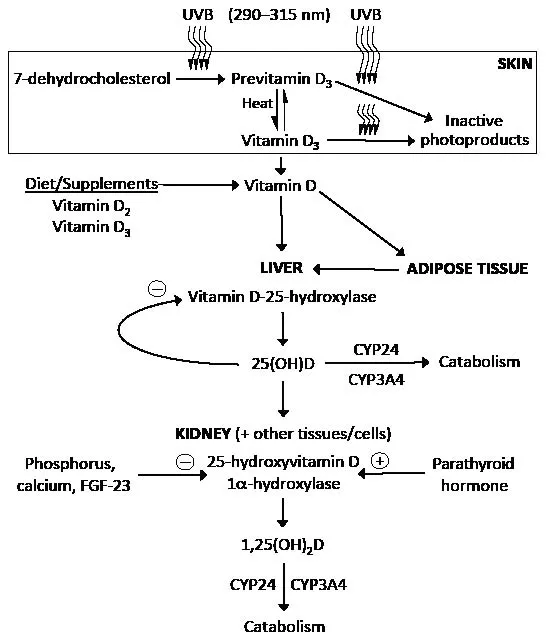
⭐ Renal 1α-hydroxylase (CYP27B1) is the rate-limiting enzyme for Calcitriol production, primarily stimulated by Parathyroid Hormone (PTH).
Vitamin D Actions - Calcium's Best Friend
- Intestine: ↑ absorption of dietary Calcium & Phosphate. Key proteins: Calbindin-D9k, TRPV6.
- Kidney: ↑ reabsorption of Calcium & Phosphate in distal tubules.
- Bone:
- Promotes bone mineralization (indirectly by ↑ Ca & P levels).
- Stimulates osteoclast activity for bone resorption (mobilizes Ca & P from bone).
- Parathyroid Gland: ↓ PTH synthesis & secretion (negative feedback).
- Immune system: Modulatory effects.
 on intestine, kidney, bone, and parathyroid gland)
on intestine, kidney, bone, and parathyroid gland)
⭐ Vitamin D (Calcitriol) induces synthesis of Calbindin, a calcium-binding protein crucial for intestinal calcium absorption.
Calcium Regulation - The Hormonal Trio

- Parathyroid Hormone (PTH): From parathyroids.
- Trigger: ↓ Serum Ca²⁺.
- Actions: ↑ Bone resorption; Kidney: ↑ Ca²⁺ reabsorption, ↓ PO₄³⁻ reabsorption, ↑ Vit D (1α-hydroxylase) activation.
- Net: ↑ Serum Ca²⁺, ↓ Serum PO₄³⁻.
- Vitamin D (Calcitriol): Activated in kidney (by PTH).
- Actions: ↑ Intestinal Ca²⁺ & PO₄³⁻ absorption; ↑ Bone mineralization & resorption; ↑ Renal Ca²⁺ reabsorption.
- Net: ↑ Serum Ca²⁺, ↑ Serum PO₄³⁻.
- Calcitonin: From thyroid C-cells.
- Trigger: ↑ Serum Ca²⁺.
- Actions: ↓ Bone resorption; ↑ Kidney Ca²⁺ excretion.
- Net: ↓ Serum Ca²⁺ (minor role).
⭐ PTH causes phosphaturia (↑ PO₄³⁻ excretion), unlike Vitamin D which ↑ PO₄³⁻ absorption/reabsorption.
Imbalance Issues - When Levels Go Wrong
- Hypocalcemia (↓ $Ca^{2+}$)
- Causes: Vitamin D deficiency, hypoparathyroidism, renal failure, malabsorption.
- Features: Tetany (Chvostek's, Trousseau's signs), paresthesias, muscle cramps, seizures. Cardiac: Prolonged QT interval.
- Chronic: Rickets (children), Osteomalacia (adults).
- Hypercalcemia (↑ $Ca^{2+}$)
- Causes: Hyperparathyroidism, Vitamin D toxicity, malignancy (e.g., PTHrP), granulomatous disease (e.g., sarcoidosis).
- Features: 📌 "Stones (renal calculi), Bones (pain, osteitis fibrosa cystica), Groans (abdominal pain, constipation), Thrones (polyuria, polydipsia), Psychiatric overtones (confusion, fatigue)". Cardiac: Short QT interval.
- Vitamin D Deficiency
- Rickets (children): Defective mineralization of growing bone. Bowing of legs (genu varum/valgum), rachitic rosary, Harrison's sulcus, craniotabes, delayed fontanelle closure.
- Osteomalacia (adults): Defective mineralization of mature bone. Bone pain, muscle weakness, pathological fractures, Looser's zones (pseudofractures).
- Vitamin D Toxicity (Hypervitaminosis D)
- Leads to ↑ $Ca^{2+}$ and ↑ $PO_4^{3-}$.
- Symptoms of hypercalcemia, metastatic calcification of soft tissues.

⭐ Hypercalcemia in sarcoidosis is due to increased extra-renal synthesis of $1,25(OH)_2D$ (calcitriol) by activated macrophages in granulomas.
Clinical Pearls - Diagnose & Treat
- Rickets/Osteomalacia (Vit D def.): ↓Ca²⁺, ↓PO₄³⁻, ↑ALP, ↑PTH. Treat with Vit D (600,000 IU IM single dose or 60,000 IU/week oral for 8 weeks) & calcium.
- Hypervitaminosis D: ↑Ca²⁺, ↑PO₄³⁻, ↓PTH. Symptoms: N/V, polyuria, polydipsia. Treat: stop Vit D, hydration, corticosteroids.
- Hypocalcemia: Chvostek's, Trousseau's signs. Treat acute: IV Calcium gluconate.
- Hypercalcemia: "Stones, bones, groans, thrones, psychiatric overtones". Treat: hydration, bisphosphonates, calcitonin.
⭐ Pseudohypoparathyroidism (Albright's hereditary osteodystrophy) shows end-organ resistance to PTH: ↓Ca²⁺, ↑PO₄³⁻, but ↑PTH levels. Features: short stature, short 4th/5th metacarpals.
High‑Yield Points - ⚡ Biggest Takeaways
- Vitamin D (prohormone) is activated by 25-hydroxylation (liver) then 1α-hydroxylation (kidney) to Calcitriol.
- Calcitriol (1,25-(OH)2D), the active form, significantly ↑ intestinal Ca²⁺ & PO₄³⁻ absorption and also ↑ renal Ca²⁺ reabsorption.
- PTH stimulates renal 1α-hydroxylase; Calcitriol provides negative feedback to PTH.
- Deficiency: Rickets (children), Osteomalacia (adults).
- Toxicity: Hypercalcemia, hypercalciuria, soft tissue calcification.
- Calcitonin from thyroid C-cells opposes PTH action, thereby ↓ blood Ca²⁺ levels.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

