Insulin & Receptor - The Initial Handshake
- Insulin:
- Source: Pancreatic $\beta$-cells.
- Nature: Peptide hormone (51 amino acids; A & B chains).
- Key Stimuli for Release:
- ↑ Blood glucose (major trigger, e.g., >100 mg/dL or >5.5 mmol/L).
- Amino acids (leucine, arginine).
- Incretins (GLP-1, GIP).
- Insulin Receptor (IR):
- Type: Receptor Tyrosine Kinase (RTK).
- Structure: Heterotetramer ($2\alpha, 2\beta$). 📌 Mnemonic: Alpha Outside (binds insulin), Beta Below (transmembrane) & Busy (kinase activity).
- $\alpha$-subunits: Extracellular, insulin binding.
- $\beta$-subunits: Transmembrane, intrinsic tyrosine kinase.
- Location: Liver, muscle, adipose tissue (high density).
⭐ The insulin receptor is unique as it's a pre-formed (αβ)₂ dimer, unlike other RTKs that dimerize upon ligand binding.
Signaling Cascade - Domino Effect Inside
- Receptor autophosphorylation → IRS (Insulin Receptor Substrate) protein phosphorylation.
- IRS acts as a docking hub for SH2-domain proteins.
- Key Downstream Pathways:
- 1. PI3K-Akt Pathway (Mainly Metabolic):
- IRS → PI3K activation.
- PI3K: $PIP_2$ → $PIP_3$ (second messenger).
- $PIP_3$ recruits PDK1 & Akt (PKB).
- Activated Akt →
- ↑ GLUT4 translocation (muscle/adipose).
- ↑ Glycogen synthesis, ↓ Gluconeogenesis.
- ↑ Protein synthesis, ↑ Lipogenesis.
- 2. Ras-MAPK Pathway (Mainly Mitogenic/Growth):
- IRS/Shc → Grb2-SOS complex.
- SOS activates Ras (GTP-binding protein).
- Ras → Raf → MEK → ERK (MAPK).
- ERK (to nucleus) → Gene expression changes (cell growth, proliferation).
- 1. PI3K-Akt Pathway (Mainly Metabolic):
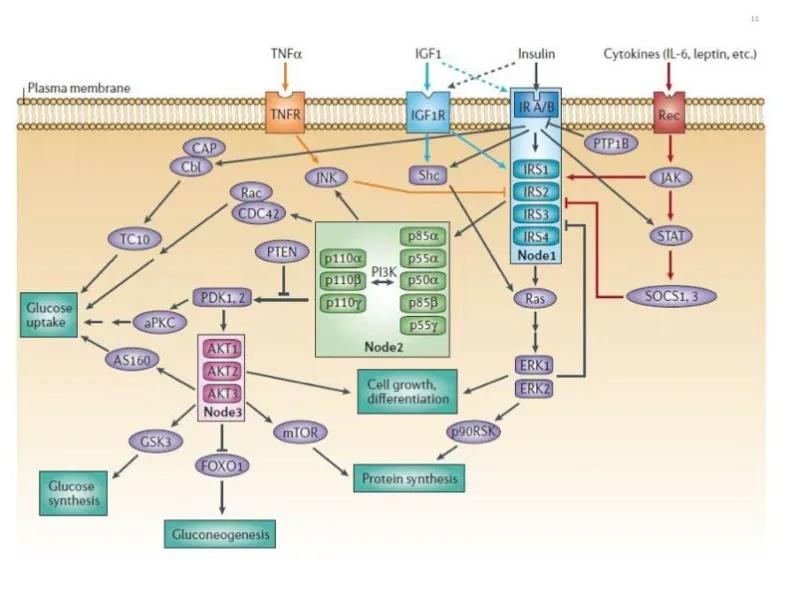
⭐ $PIP_3$ acts as a crucial second messenger, recruiting Akt and PDK1 to the plasma membrane, a key step in insulin's metabolic actions.
Metabolic Actions - Sweet Results & More
- Overall: Anabolic hormone promoting fuel storage.
- Carbohydrate Metabolism (↓ Blood Glucose):
- ↑ Glucose uptake: GLUT4 translocation (muscle, adipose tissue).
- ↑ Glycogen synthesis (liver, muscle): Activates glycogen synthase.
- ↓ Glycogenolysis: Inhibits glycogen phosphorylase.
- ↑ Glycolysis (liver): Induces glucokinase, PFK-1, pyruvate kinase.
- ↓ Gluconeogenesis (liver): Represses PEPCK, FBP-1, G6Pase.
- Lipid Metabolism (Anti-lipolytic, Lipogenic):
- ↑ Triglyceride synthesis (adipose, liver): Activates Acetyl-CoA carboxylase, ↑ LPL.
- ↓ Lipolysis (adipose): Inhibits Hormone-Sensitive Lipase (HSL).
- ↓ Ketogenesis (liver).
- Protein Metabolism (Anabolic):
- ↑ Amino acid uptake & protein synthesis.
- ↓ Protein catabolism.
- Electrolyte Balance:
- ↑ K+ uptake into cells (via Na+/K+ ATPase stimulation).
⭐ Insulin is a key regulator of Hormone-Sensitive Lipase (HSL); its inhibition by insulin prevents triglyceride breakdown in adipocytes, reducing free fatty acid release.
Regulation & Dysregulation - Pathway Control Issues
- Signal Termination Mechanisms:
- Protein Tyrosine Phosphatases (PTPs, e.g., PTP1B) dephosphorylate Insulin Receptor (IR) & IRS proteins.
- Serine/Threonine (Ser/Thr) kinases (e.g., JNK, IKK, PKC) phosphorylate IRS (inhibitory effect).
- Suppressor of Cytokine Signaling (SOCS) proteins promote IRS degradation.
- Insulin receptor internalization & subsequent degradation.
- Dysregulation & Pathophysiology:
- Insulin Resistance (IR):
- Decreased cellular responsiveness to insulin.
- Key Causes: Genetic defects, chronic inflammation (↑IRS Ser/Thr phosphorylation), obesity (↑Free Fatty Acids, TNF-α).
- Type 2 Diabetes Mellitus (T2DM):
- Develops from progressive IR combined with β-cell dysfunction.
- Characterized by hyperglycemia; often initial hyperinsulinemia.
- Insulin Resistance (IR):
⭐ Ser/Thr phosphorylation of IRS proteins (e.g., by JNK or IKK) is a critical molecular mechanism contributing to insulin resistance development in states like obesity and inflammation.
High‑Yield Points - ⚡ Biggest Takeaways
- Insulin binds to a Tyrosine Kinase Receptor (RTK), causing autophosphorylation.
- IRS proteins are crucial adaptors, activating the PI3K/Akt pathway for metabolic effects.
- GLUT4 translocation to membranes of muscle and adipose tissue is a key outcome.
- The MAPK pathway is also activated, mediating mitogenic effects (e.g., growth).
- Insulin is anabolic: ↑glycogen synthesis, ↑lipogenesis, ↑protein synthesis.
- Insulin is anti-catabolic: ↓gluconeogenesis, ↓glycogenolysis, ↓lipolysis.
- PTEN phosphatase opposes PI3K signaling, a key negative regulator.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

