Early Starvation (0-24h) - Fuel Scramble
- Goal: Maintain blood glucose (brain, RBCs).
- Hormones: ↓ Insulin, ↑ Glucagon, ↑ Cortisol, ↑ Epinephrine. (Insulin/Glucagon ratio ↓).
- Fuel Sources & Pathways:
- Liver Glycogenolysis: Primary source for ~12-18h (depletes by ~24h).
- Gluconeogenesis (GNG): Liver (later kidney). Substrates: Lactate, Alanine, Glycerol.
- Lipolysis (Adipose): ↑ FFAs (fuel for muscle/liver) + Glycerol (GNG).
- Muscle Protein Catabolism: → Alanine (GNG).
- Organ Fuel:
- Brain: Glucose.
- Muscle: Switches to FFAs.
- RBCs: Glucose (obligate).
⭐ Liver glycogen is the main glucose source for the first ~12-18h of fasting.
Mid-Starvation (2-24 days) - Fat Burning Fiesta
- Duration: 2-24 days; shift to sustained fat catabolism.
- Hormones: ↓↓↓Insulin, ↑↑Glucagon, ↑Cortisol, ↑Growth Hormone.
- Adipose Tissue: Dominant lipolysis (Hormone-Sensitive Lipase activation). Releases fatty acids (FAs) & glycerol.
- Liver Metabolism:
- ↑↑ FA β-oxidation → abundant Acetyl-CoA.
- ↑↑ Ketogenesis: Acetyl-CoA → ketone bodies (β-hydroxybutyrate, acetoacetate) for brain/muscle.
- Gluconeogenesis persists (glycerol, lactate, amino acids).
- Peripheral Tissue Fuel Use:
- Brain: Adapts to ketone bodies (up to 70% energy), sparing glucose.
- Muscle: Utilizes FAs & ketone bodies; ↓glucose uptake; significant protein sparing.
- Key Outcome: Urea nitrogen excretion ↓, reflecting protein conservation.
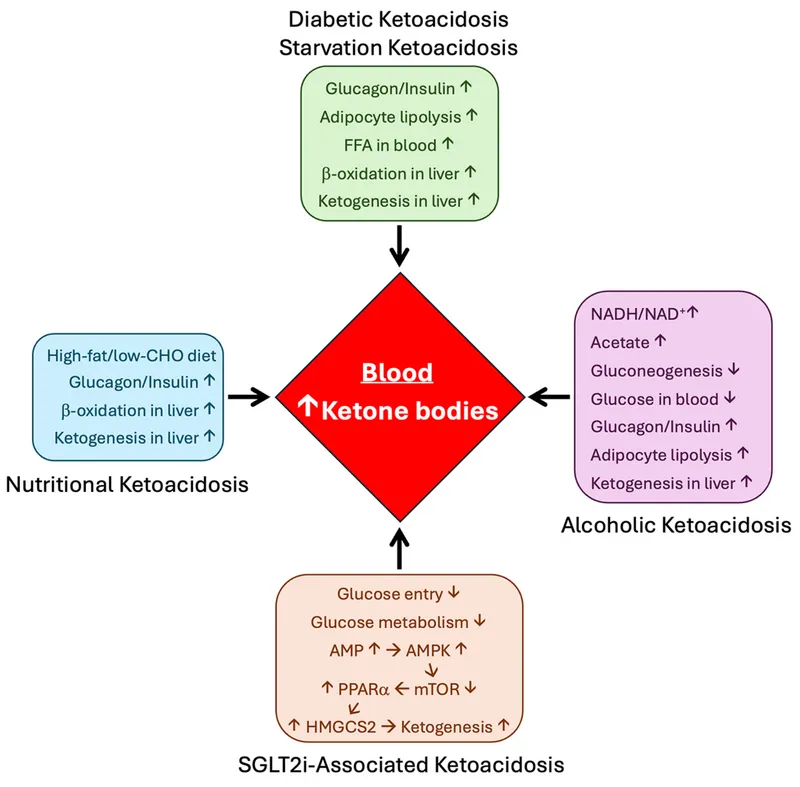
⭐ The brain's ability to switch to ketone bodies as its primary fuel source during prolonged fasting is crucial for sparing muscle protein.
Prolonged Starvation (>24 days) - Protein Predicament
- Fat reserves critically low/exhausted; protein becomes the main endogenous fuel.
- Accelerated proteolysis: structural (muscle) and functional (enzymes, albumin, immunoglobulins) proteins catabolized.
- Results in severe muscle wasting (cachexia).
- ↓ Serum albumin → oncotic edema.
- Compromised immunity (↓ immunoglobulins).
- ↑ Urinary nitrogen (urea) excretion signifies rapid protein breakdown.
- Brain still utilizes ketone bodies, but gluconeogenesis from amino acids is vital for glucose supply.
- Leads to multi-organ dysfunction (respiratory, cardiac) and eventual death.
⭐ The body sacrifices crucial functional proteins once fat stores are depleted; death typically occurs when ~50% of body protein is lost.
Hormonal Regulation - Starvation Conductors
- Primary Goal: Maintain glucose supply to brain & vital organs; conserve protein.
- Key Players & Shifts:
- ↓ Insulin:
- Hallmark of starvation.
- ↓ Glucose uptake (muscle, adipose).
- ↓ Anabolism (glycogenesis, lipogenesis, protein synthesis).
- ↑ Catabolism.
- ↑ Glucagon:
- Dominant catabolic signal.
- ↑ Hepatic glucose output (glycogenolysis, then gluconeogenesis).
- ↑ Lipolysis & ketogenesis.
- ↑ Cortisol:
- Permissive for glucagon & catecholamines.
- ↑ Proteolysis (muscle → amino acids for gluconeogenesis).
- ↑ Lipolysis, ↑ Gluconeogenesis.
- ↑ Growth Hormone (GH):
- ↑ Lipolysis (FFA release).
- ↓ Peripheral glucose utilization.
- Protein-sparing effect.
- ↓ Thyroid Hormones (T3):
- ↓ T4 to T3 conversion.
- ↓ Basal Metabolic Rate (BMR) → energy conservation.
- ↑ Reverse T3 (rT3).
- ↓ Insulin:

⭐ The Insulin:Glucagon ratio is the most critical determinant of metabolic state. A low ratio signals starvation, promoting catabolism and inhibiting anabolism across tissues to ensure glucose availability for the brain and red blood cells.
High-Yield Points - ⚡ Biggest Takeaways
- Early starvation: Relies on glycogenolysis, then gluconeogenesis (alanine, lactate, glycerol).
- Prolonged starvation: Marked by ↑ lipolysis, ↑ fatty acid oxidation, and ↑ hepatic ketogenesis.
- Brain adaptation: Shifts from glucose to ketone bodies (β-hydroxybutyrate > acetoacetate) as primary fuel.
- Protein conservation: Muscle protein breakdown ↓ as brain uses ketones, sparing glucose.
- Key hormones: Insulin ↓, glucagon ↑, cortisol ↑.
- Energy conservation: Basal Metabolic Rate (BMR) ↓.
- Fuel hierarchy: Glucose → Fatty acids → Ketone bodies become crucial.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

