Obesity Overview - Sizing Up the Scale
- Obesity: Excess body fat accumulation posing health risks.
- BMI: $weight (kg) / height (m^2)$.
- WHO: Overweight ≥25 kg/m²; Obese ≥30 kg/m².
- Asian Indians: Overweight ≥23 kg/m²; Obese ≥25 kg/m² (or ≥27.5 kg/m²).
- Waist Circumference (Indian): Men >90 cm; Women >80 cm.
- Waist-to-Hip Ratio: Indicates central obesity; risk marker.
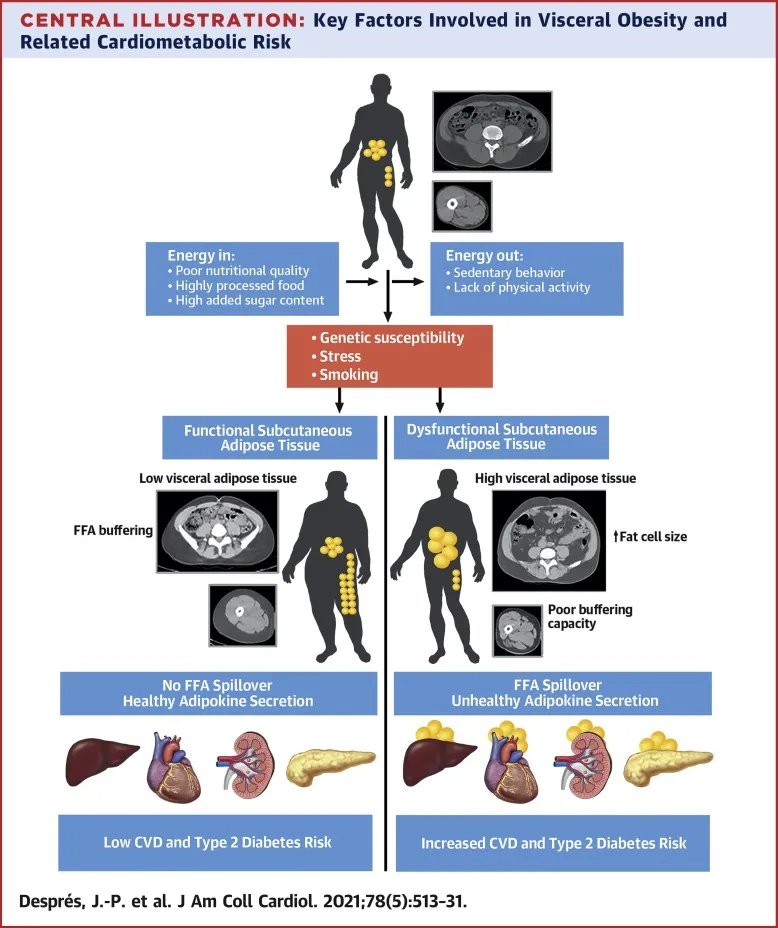
⭐ Asian Indians have a higher percentage of body fat at lower BMIs compared to Western populations, increasing their risk for metabolic syndrome.
Adipose Tissue Talk - Fat's Secret Signals
Adipose tissue: an active endocrine organ releasing adipokines. These signal appetite, insulin sensitivity, and inflammation.
| Adipokine | Source | Key Action(s) in Obesity | Level (Obesity) |
|---|---|---|---|
| Leptin | Adipocytes | Satiety signal. 📌 'Less please!' | ↑ (resistance) |
| Adiponectin | Adipocytes | Insulin-sensitizing, anti-inflammatory. 📌 'Adipo-nice-tin' | ↓ |
| Resistin | Adipocytes, Macrophages | Pro-inflammatory, insulin resistance | ↑ |
| TNF-α | Adipocytes, Macrophages | Pro-inflammatory, insulin resistance | ↑ |
| IL-6 | Adipocytes, Macrophages | Pro-inflammatory, insulin resistance | ↑ |
⭐ Leptin resistance, not deficiency, is the primary issue in most common human obesity.
Brain's Appetite Control - Hunger Games HQ
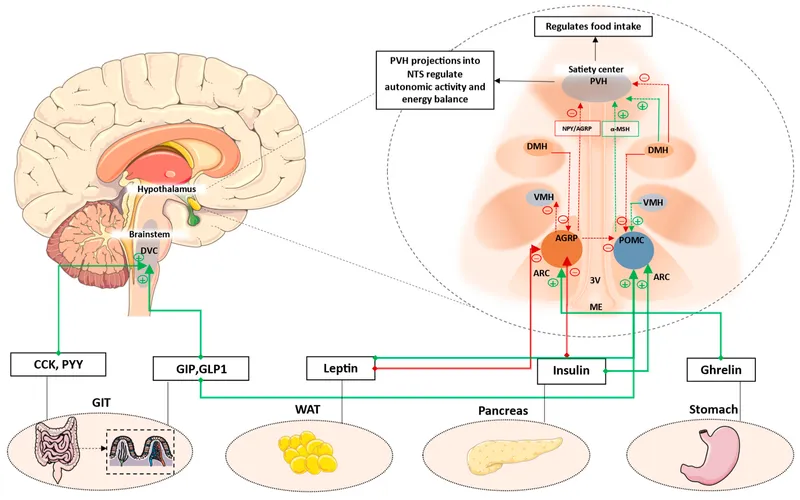
- Hypothalamus (Arcuate Nucleus): Primary appetite regulator.
- POMC/CART neurons: Release α-MSH → satiety (anorexigenic).
- NPY/AgRP neurons: Release NPY/AgRP → hunger (orexigenic).
- Key Peripheral Signals:
- Ghrelin (stomach): Orexigenic; ↑NPY/AgRP. 📌 Ghrelin makes Guts Rumble.
- Leptin (adipose): Anorexigenic; ↑POMC/CART, ↓NPY/AgRP.
- Insulin (pancreas): Anorexigenic (centrally); similar to leptin.
- PYY (ileum/colon): Anorexigenic; ↓NPY/AgRP.
- GLP-1 (ileum): Anorexigenic; ↑POMC/CART.
- CCK (duodenum): Anorexigenic; promotes satiety (vagal/brain).
⭐ Mutations in the MC4R (melanocortin-4 receptor) gene are the most common cause of monogenic human obesity.
Metabolic Mayhem - When Systems Derail
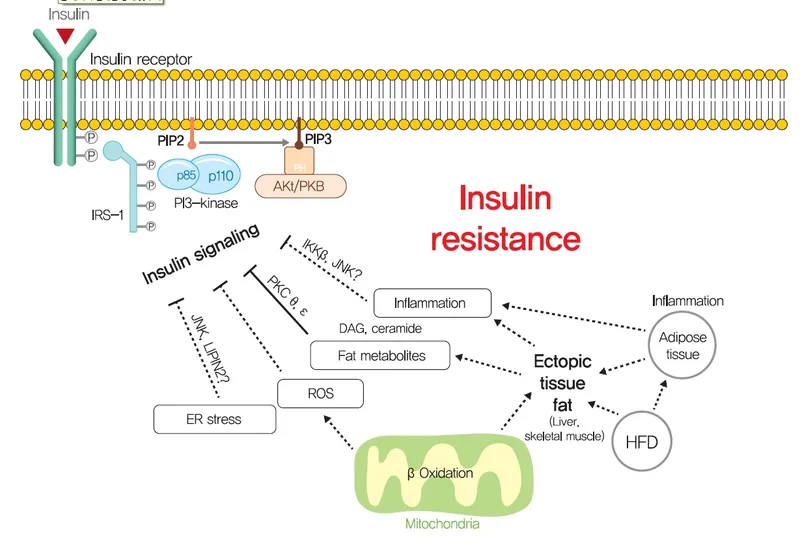
- Insulin Resistance: Central defect in obesity's metabolic fallout.
- Mechanisms: Increased Free Fatty Acids (FFAs), chronic inflammation (e.g., macrophage infiltration in adipose tissue), and impaired post-receptor insulin signaling pathways.
- Dyslipidemia: Abnormal lipid profile.
- Characterized by ↑Triglycerides, ↓HDL-C, and ↑small-dense LDL (sdLDL) particles.
- 📌 Mnemonic: Obese Try Getting High Low-density particles (↑TG, ↓HDL, ↑sdLDL).
- Chronic Low-Grade Inflammation: Systemic inflammation.
- Marked by ↑C-Reactive Protein (CRP) and ↑pro-inflammatory cytokines (e.g., TNF-α, IL-6).
- Ectopic Fat Deposition: Fat storage in non-adipose tissues.
- Examples: Liver (NAFLD - Non-Alcoholic Fatty Liver Disease), muscle, pancreas.
- Oxidative Stress: Imbalance between reactive oxygen species (ROS) production and antioxidant defenses.
⭐ Visceral adiposity is more strongly correlated with insulin resistance and metabolic complications than subcutaneous adiposity. This is a key factor in metabolic syndrome development associated with obesity.
Genetic & Gut Links - Nature & Nurture Mix
- Genetic Factors:
- Monogenic (rare): Mutations in LEP, LEPR, MC4R, POMC genes.
- Polygenic (common): Multiple genes; FTO gene variants are most significant.
- Epigenetics: DNA methylation influences gene expression related to adipogenesis/metabolism.
- Gut Microbiome Links:
- Alterations: e.g., Firmicutes/Bacteroidetes ratio.
- Metabolites: Short-Chain Fatty Acids (SCFAs) production changes.
- Impact: Affects energy extraction and systemic inflammation.
⭐ The FTO gene is the most significant common variant associated with polygenic obesity, influencing energy intake and food preferences.
oka
High‑Yield Points - ⚡ Biggest Takeaways
- Leptin resistance, not deficiency, is central to most human obesity.
- ↓ Adiponectin levels contribute to insulin resistance and a pro-inflammatory state.
- Ghrelin, the hunger hormone, may show blunted postprandial suppression.
- Chronic low-grade inflammation from adipocyte-derived cytokines (e.g., TNF-α, IL-6) is characteristic.
- Insulin resistance and compensatory hyperinsulinemia are key metabolic derangements.
- Ectopic fat deposition (e.g., liver, muscle) drives organ-specific complications.
- Brown Adipose Tissue (BAT) activity and UCP1 influence energy expenditure and thermogenesis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

