Muscle Metabolism - Fueling the Flex
- Immediate Energy (0-10s): ATP-PCr system. $PCr + ADP \leftrightarrow ATP + Creatine$. Enzyme: Creatine Kinase.
- Short-Term Energy (10s - ~2min): Anaerobic glycolysis. Glucose $\rightarrow$ Pyruvate $\rightarrow$ Lactate. Key enzyme: PFK-1. Rapid ATP, yields 2 ATP/glucose.
- Long-Term Energy (>2min): Aerobic metabolism (Oxidative Phosphorylation).
- Sources: Glucose (glycogen, blood), Fatty Acids (FAs), Ketone Bodies (KBs), Amino Acids (AAs).
- Key enzymes/carriers: PDH (Pyruvate to Acetyl-CoA), CPT-1 (FA transport into mitochondria).
- Yield: ~32 ATP/glucose; ~100+ ATP/FA.
- Fuel Stores: Muscle glycogen (local use), Intramuscular Triglycerides (IMTGs), Adipose TGs (via blood).
- Fiber Types & Fuel Preference:
- Type I (slow-twitch): Aerobic, $\uparrow$mitochondria, $\uparrow$myoglobin, FA preference.
- Type IIx (fast-twitch): Anaerobic/Glycolytic, $\downarrow$mitochondria, glycogen preference.
- Key Regulation: Insulin (anabolic, promotes storage); Epinephrine (catabolic, mobilizes fuels during exercise). 📌 Fuel Hierarchy (recruitment order): Phosphocreatine $\rightarrow$ Glucose (Anaerobic/Aerobic) $\rightarrow$ Fatty Acids $\rightarrow$ Ketone Bodies/Amino Acids.
⭐ McArdle Disease (Glycogen Storage Disease Type V / Myophosphorylase deficiency): Impaired muscle glycogenolysis $\rightarrow$ exercise intolerance, muscle cramps, and "second wind" phenomenon after rest or with glucose intake.
Muscle Metabolism - Muscle on the Move
- Energy Sources & Timeline:
- Immediate (0-10s): ATP, Phosphocreatine ($PCr + ADP \leftrightarrow ATP + Cr$). Creatine Kinase.
- Short-term (10s-2min): Anaerobic glycolysis (glucose/glycogen → lactate). Rapid ATP, lactate accumulation.
- Long-term (>2min): Aerobic oxidation (glucose, fatty acids, ketone bodies, BCAAs). Sustained ATP.
- Fuel Choice by Intensity:
- Rest: Mainly fatty acids (~85%), glucose (aerobic).
- Light/Moderate Exercise: Blood glucose, muscle glycogen, then ↑fatty acids (aerobic).
- Intense Exercise (Sprint): Phosphocreatine, then anaerobic glycolysis from muscle glycogen (lactate↑).
- Prolonged Exercise (Marathon): Fatty acids become primary fuel as glycogen is depleted. "Hitting the wall".
- Key Inter-Organ Cycles:
- Cori Cycle: Muscle lactate → Liver (gluconeogenesis) → Glucose → Muscle. Recycles lactate to glucose.
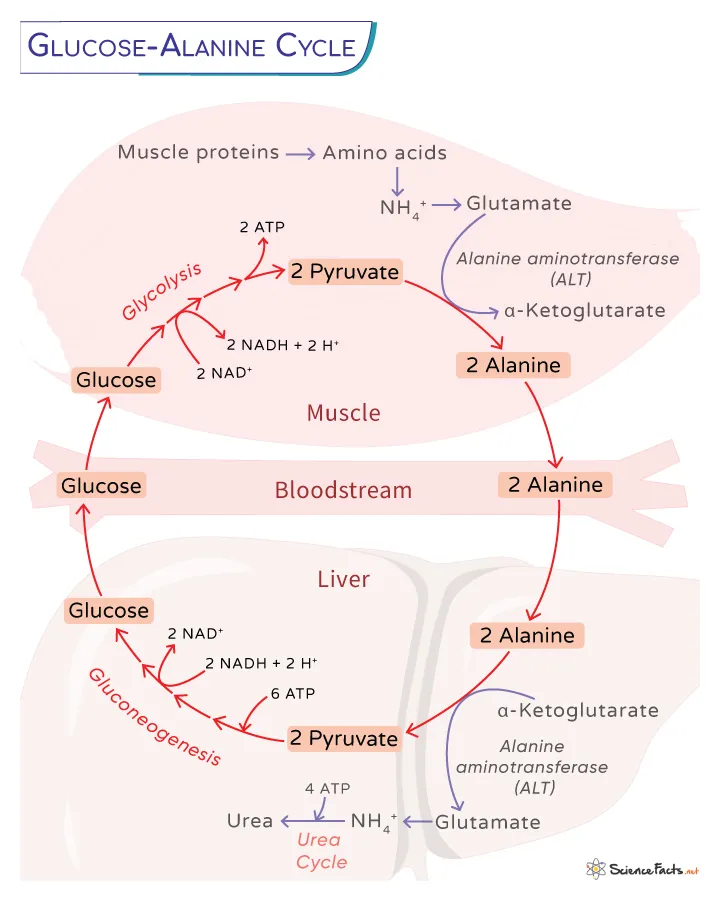
- Glucose-Alanine Cycle: Muscle pyruvate + $NH_4^+$ (from amino acids) → Alanine → Liver (gluconeogenesis + urea cycle) → Glucose → Muscle. Removes muscle $NH_4^+$.
- Metabolic Shifts:
⭐ McArdle Disease (GSD Type V): Muscle glycogen phosphorylase deficiency. Causes exercise intolerance, painful cramps, myoglobinuria. Characteristic: no rise in blood lactate after ischemic exercise. "Second wind" phenomenon seen.
Muscle Metabolism - Regulators & Roadblocks
- Key Hormonal Regulators:
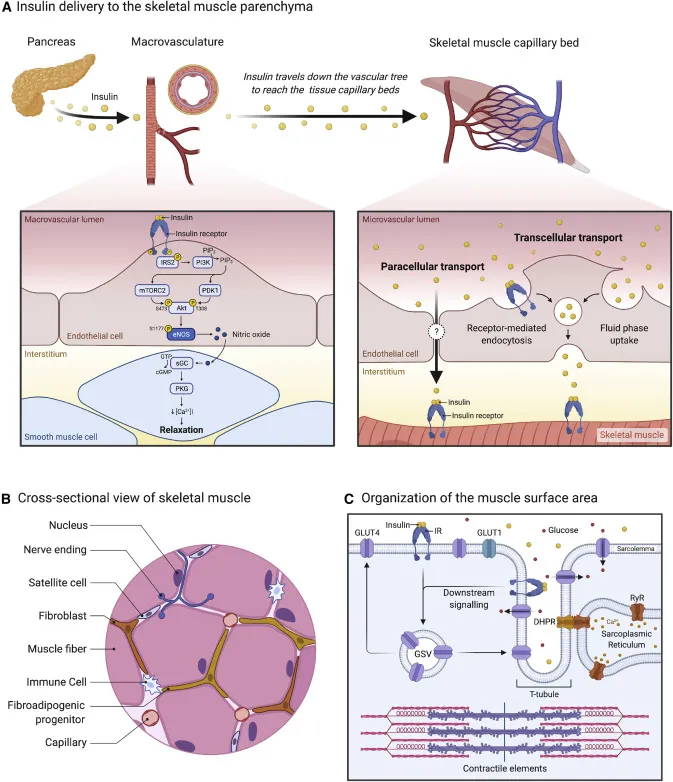
- Insulin: Anabolic. ↑ GLUT4 translocation (glucose entry), ↑ glycogen & protein synthesis.
- Epinephrine: Catabolic (stress/exercise). ↑ Glycogenolysis (β-receptors, cAMP), ↑ lipolysis (HSL).
- Cortisol: Catabolic (chronic). ↑ Protein breakdown, induces insulin resistance.
- AMPK: Cellular energy sensor (exercise). Activated by ↑ AMP:ATP ratio.
- Effects: ↑ GLUT4 uptake & glycolysis, ↑ FA oxidation; ↓ protein & glycogen synthesis.
- Metabolic Roadblocks (Disorders):
- McArdle's Disease (GSD V): Myophosphorylase (muscle glycogen phosphorylase) defect.
- Features: Exercise intolerance, cramps, myoglobinuria; no ↑ blood lactate post-ischemic exercise.
⭐ "Second wind" phenomenon due to switch to fatty acids/proteins.
- Carnitine Deficiency: Impaired LCFA transport into mitochondria (carnitine shuttle defect).
- Results in: ↓ β-oxidation, muscle weakness, cardiomyopathy, hypoglycemia.
- Insulin Resistance: ↓ Muscle glucose uptake despite insulin; key in Type 2 DM.
- McArdle's Disease (GSD V): Myophosphorylase (muscle glycogen phosphorylase) defect.
High‑Yield Points - ⚡ Biggest Takeaways
- Resting muscle: Primarily uses fatty acids.
- Short, intense exercise: Creatine phosphate, then anaerobic glycolysis (lactate).
- Prolonged exercise: Aerobic oxidation of glucose & fatty acids.
- Cori Cycle: Muscle lactate → liver gluconeogenesis → muscle glucose.
- Glucose-Alanine Cycle: Muscle alanine → liver gluconeogenesis & urea cycle.
- AMPK: Key energy sensor, activates catabolism; Insulin: Promotes glucose uptake (GLUT4) & glycogen synthesis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

