Fatty Liver & Pathogenesis - Greasy Guts Genesis
- Hepatic Steatosis: Fat accumulation in >5% of hepatocytes.
- NAFLD: Non-Alcoholic Fatty Liver Disease; common with metabolic syndrome.
- AFLD: Alcoholic Fatty Liver Disease; due to chronic alcohol use.
- Pathogenesis - Key Mechanisms: 📌 Mnemonic: Too much IN, too much MADE, too little BURNED, too little SENT OUT.
- ↑ Increased Free Fatty Acid (FFA) influx from adipose tissue/diet.
- ↑ Increased De Novo Lipogenesis (DNL) (hepatic fat synthesis).
- ↓ Decreased FFA β-oxidation (fat breakdown).
- ↓ Decreased VLDL (Very Low-Density Lipoprotein) export; impaired by defects in ApoB-100 synthesis or MTP (Microsomal Triglyceride Transfer Protein) function.
- Key Molecular Regulators:
- Insulin Resistance: Central driver, esp. in NAFLD.
- SREBP-1c (Sterol Regulatory Element-Binding Protein-1c): Activated by insulin; ↑ DNL.
- ChREBP (Carbohydrate Responsive Element-Binding Protein): Activated by carbohydrates; ↑ DNL.

⭐ Insulin resistance is a central pathogenic factor in NAFLD, linking it to metabolic syndrome.
Lipotropic Factors - The De-Greasing Crew
- Definition: Agents that promote fat export from the liver, preventing/correcting hepatic steatosis.
- Key Lipotropic Factors: 📌 Mnemonic: Can My Baby Ingest Folate/B12?
- Choline
- Methionine
- Betaine
- Inositol
- Folic acid & Vitamin B12 (co-factors in methyl transfer)
- Mechanisms of Action:
- Choline: Synthesizes phosphatidylcholine for VLDL particles, essential for exporting triglycerides from hepatocytes.
⭐ Choline is crucial for VLDL assembly and export; its deficiency leads to triglyceride accumulation in the liver.
- Methionine: Provides S-adenosylmethionine (SAMe), a key methyl donor.
- Choline synthesis precursor (transmethylation).
- Glutathione synthesis (antioxidant, protects liver).
- Betaine: Methyl donor; converts homocysteine to methionine, spares choline, supports SAMe.
- Inositol: Phospholipid (phosphatidylinositol) component; involved in cell membranes, signaling, lipid metabolism.
- Choline: Synthesizes phosphatidylcholine for VLDL particles, essential for exporting triglycerides from hepatocytes.

Clinical & Management - Spot & Stop Steatosis
- Clinical Features & Progression:
- Often asymptomatic. May include fatigue, RUQ discomfort, hepatomegaly.
- Spectrum: Simple steatosis (NAFL) → NASH (inflammation, hepatocyte injury) → Fibrosis → Cirrhosis (potential HCC).
- Diagnostic Workup:
- Labs:
- LFTs: ↑ALT > AST (NAFLD); AST:ALT > 2 (AFLD).
- Dyslipidemia (↑TG, ↓HDL).
- Imaging:
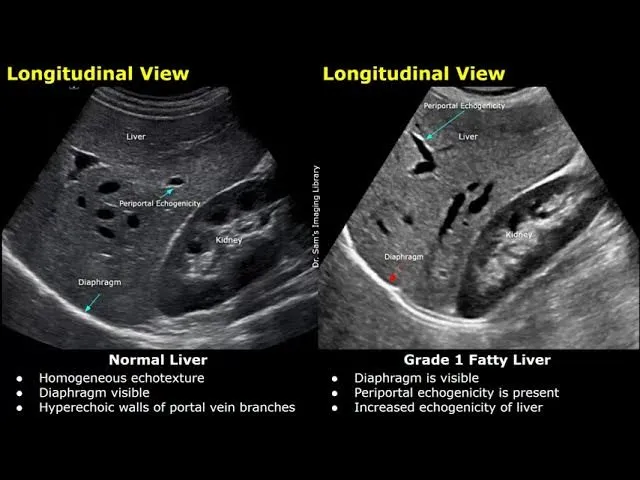
- USG: Hyperechoic liver (initial, screening).
- FibroScan (stiffness for fibrosis), MRI-PDFF (quantifies fat).
- USG: Hyperechoic liver (initial, screening).
- Liver Biopsy: Gold standard for NASH diagnosis, fibrosis staging; not routine for all.
- Labs:
- Management Approach:
- NAFLD:
- Lifestyle modification (cornerstone): Weight loss (7-10%), Mediterranean diet, regular exercise (150 min/wk moderate).
- AFLD: Complete alcohol cessation.
- Lipotropic Factors: (e.g., Choline, Methionine, Vitamin E for biopsy-proven NASH in non-diabetics). Role supplemental, evidence varies.
- NAFLD:
⭐ In NAFLD, ALT is typically higher than AST. In alcoholic liver disease (AFLD), an AST:ALT ratio >2 is characteristic, often with elevated GGT.
High‑Yield Points - ⚡ Biggest Takeaways
- Fatty liver (hepatic steatosis) is characterized by excess triglyceride accumulation in hepatocytes.
- Major causes include chronic alcohol abuse, obesity (NAFLD/NASH), diabetes mellitus, and protein-energy malnutrition.
- Pathophysiology involves an imbalance between hepatic triglyceride synthesis and its secretion as VLDL.
- Lipotropic factors such as choline, methionine, betaine, and inositol prevent or correct fatty liver.
- These factors promote VLDL assembly/secretion (e.g., choline for phosphatidylcholine) or act as methyl donors.
- Deficiency of these factors results in impaired VLDL export and hepatic fat accumulation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

