Iron Homeostasis & Dysregulation - Iron's Balancing Act
- Core Principle: Iron balance maintained by regulating absorption, storage, transport.
- Key Players & Regulation:
- Hepcidin: Master regulator (liver hormone); blocks ferroportin.
- Ferroportin: Iron efflux channel (enterocytes, macrophages).
- Transferrin: Transports iron.
- Ferritin: Stores iron.
- Dysregulation Pathways:
- ↑ Hepcidin (e.g., inflammation, Anemia of Chronic Disease - ACD) → ↓ iron absorption/release → ↓ serum iron.
- ↓ Hepcidin (e.g., hemochromatosis, iron deficiency) → ↑ iron absorption/release → ↑ serum iron.
⭐ Hepcidin is the master regulator of iron homeostasis, and its dysregulation is key to many iron disorders (e.g., increased in ACD, decreased in hemochromatosis).

Iron Deficiency Anemia - Running on Empty
Most common global nutritional deficiency.
- Etiology: ↓ intake, ↓ absorption (celiac, gastrectomy, PPIs), ↑ loss (GI bleed, menses), ↑ demand (pregnancy, growth).
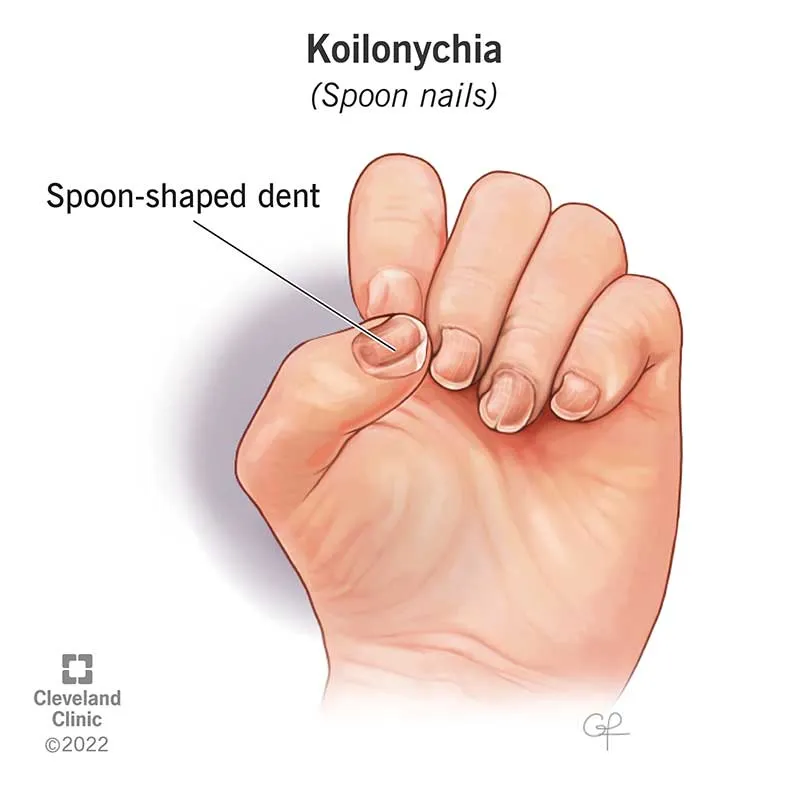
- Clinical: Fatigue, pallor, koilonychia (spoon nails), pica, glossitis, angular stomatitis.
- Labs:
- Microcytic hypochromic (↓ Hb, MCV, MCH, MCHC). ↑ RDW (early).
- ↓ Serum Fe, ↓ Ferritin (<15-30 ng/mL), ↑ TIBC.
- ↓ Transferrin Saturation (<16%).
- PS: Anisopoikilocytosis, pencil cells.
- Rx: Treat cause. Oral iron (ferrous sulfate). Parenteral if severe/malabsorption.
⭐ Plummer-Vinson syndrome (triad: dysphagia, iron-deficiency anemia, esophageal webs) is a classic association with chronic IDA.
Anemia of Chronic Disease - Inflammatory Lock-Up
- Patho: Chronic inflammation → ↑IL-6 → liver ↑hepcidin.
- Hepcidin: Blocks gut iron absorption; traps iron in macrophages → functional iron deficiency despite normal/↑ stores.
- Labs: ↓ Serum Fe, ↓ TIBC, Normal/↑ Ferritin. Normocytic (later microcytic). ↑ESR/CRP.
- Rx: Treat primary disease. ESAs for severe cases. Iron only if true IDA coexists.
⭐ Anemia of Chronic Disease (ACD) is characterized by low serum iron, low TIBC, and normal/high ferritin due to hepcidin-mediated iron sequestration in macrophages.
Iron Overload & Sideroblastic Anemia - Metal & Misfire
- Hereditary Hemochromatosis (HH):
- HFE gene (C282Y, H63D) → ↑ Fe absorption. Fe deposition: liver, pancreas, heart.
- "Bronze diabetes", cirrhosis, cardiomyopathy.
- Labs: ↑ Ferritin (>1000 ng/mL), ↑ Serum Fe, ↑ Transferrin Saturation (>45%), ↓ TIBC.
- Rx: Phlebotomy, iron chelators.
⭐ Hereditary Hemochromatosis is most commonly due to HFE gene mutations (C282Y, H63D) leading to increased iron absorption and deposition in organs like liver, pancreas, and heart (causing 'bronze diabetes').
- Sideroblastic Anemia: Defective heme synthesis → mitochondrial Fe accumulation.
- Types: Congenital (X-linked ALAS2), Acquired (MDS, alcohol, lead, isoniazid).
- Labs: ↑ Serum Fe, ↑ Ferritin. Anemia (often dimorphic). Basophilic stippling (lead).
- BM: Ring sideroblasts (>15%).
- Rx: Pyridoxine (B6), treat cause.

Diagnostic Iron Panel - Unmasking Disorders
Diagnostic iron panel reveals patterns for specific disorders:
| Parameter | IDA | ACD | Iron Overload | Sideroblastic |
|---|---|---|---|---|
| Serum Fe | ↓↓ | ↓/N | ↑↑ | ↑/N |
| TIBC | ↑↑ | ↓/N | ↓/N | N/↓ |
| Transferrin Sat. | ↓↓ (<15%) | ↓/N | ↑↑ (>45-50%) | ↑/N |
| Ferritin | ↓↓ | ↑/N | ↑↑ | ↑/N |
| sTfR | ↑ | N/↓ | N | N |
Transferrin saturation, calculated as $Serum\ Iron / TIBC \times 100%$, is a key diagnostic marker.
⭐ It typically shows <15% in IDA and >45-50% in iron overload, aiding differentiation.
High‑Yield Points - ⚡ Biggest Takeaways
- Iron Deficiency Anemia (IDA): Most common; microcytic hypochromic; ↓ ferritin, ↓ serum Fe, ↑ TIBC.
- Anemia of Chronic Disease (ACD): ↑ Hepcidin blocks iron release; ↓ serum Fe, ↓ TIBC, normal/↑ ferritin.
- Hereditary Hemochromatosis: HFE gene defect; ↑ iron absorption; bronze diabetes, cirrhosis. ↑ Ferritin, ↑ transferrin saturation.
- Sideroblastic Anemia: Defective heme synthesis; ring sideroblasts. Key causes: lead poisoning, INH.
- Plummer-Vinson Syndrome: Triad: IDA, esophageal webs, dysphagia.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more