Genetic Disorders and Biochemical Pathology

On this page
🧬 Genetic Disorders and Biochemical Pathology: The Molecular Detective's Arsenal
You'll master the art of molecular detective work, tracing how single genetic mutations cascade through biochemical pathways to produce complex clinical syndromes. This lesson builds your diagnostic framework from gene to bedside-connecting DNA defects to enzyme dysfunction, metabolic derangements to organ failure, and laboratory patterns to treatment strategies. By integrating genetics, biochemistry, and clinical reasoning, you'll develop the systematic approach needed to recognize, differentiate, and manage inherited metabolic disorders with precision and confidence.
🧬 Genetic Disorders and Biochemical Pathology: The Molecular Detective's Arsenal
🔬 Foundation Mastery: The Genetic-Biochemical Connection Matrix
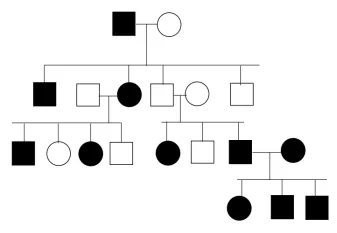
Fundamental Classification Framework
-
Single Gene Disorders (>10,000 known conditions)
- Autosomal dominant: 50% transmission risk per pregnancy
- Autosomal recessive: 25% affected offspring risk
- X-linked: 50% risk for male offspring from carrier mothers
- Penetrance varies: 60-90% for most dominant conditions
- Expressivity: Variable clinical severity within families
-
Chromosomal Disorders (1 in 150 live births)
- Numerical abnormalities: Trisomy 21 (1 in 700 births)
- Structural rearrangements: Deletions, duplications, translocations
- Critical region size: >5 Mb typically causes recognizable syndromes
- Microdeletions: <3 Mb often cause specific phenotypes
📌 Remember: MATCH - Mendelian inheritance, Autosomal patterns, Transmission risks, Chromosomal abnormalities, Hereditary biochemical defects
| Disorder Type | Prevalence | Biochemical Marker | Diagnostic Threshold | Clinical Onset |
|---|---|---|---|---|
| PKU | 1:10,000 | Phenylalanine | >6 mg/dL | Neonatal |
| Galactosemia | 1:30,000 | Galactose-1-P | >20 mg/dL | First weeks |
| MSUD | 1:185,000 | Branched-chain AA | >4 mg/dL | Days 4-7 |
| Homocystinuria | 1:344,000 | Homocysteine | >15 μmol/L | Months-years |
| Tyrosinemia I | 1:100,000 | Succinylacetone | >2 μmol/L | Infancy |
💡 Master This: Biochemical phenotypes often precede clinical symptoms by weeks to months, making laboratory screening the cornerstone of early intervention strategies that can prevent irreversible organ damage.
The biochemical approach to genetic disorders relies on understanding how gene mutations disrupt normal metabolic pathways, creating characteristic accumulation or deficiency patterns that serve as diagnostic fingerprints. This foundation enables systematic evaluation of suspected genetic conditions through targeted biochemical analysis.
🔬 Foundation Mastery: The Genetic-Biochemical Connection Matrix
⚙️ Metabolic Pathway Disruption: The Biochemical Cascade Architecture
Biochemical Disruption Patterns
-
Substrate Accumulation Disorders
- Phenylalanine in PKU: >20 mg/dL (normal <2 mg/dL)
- Galactose in galactosemia: >40 mg/dL (normal <5 mg/dL)
- Branched-chain amino acids in MSUD: >10x normal levels
- Leucine toxicity threshold: >4 mg/dL
- Neurological damage occurs within 72 hours of elevation
-
Product Deficiency Syndromes
- Glucose production defects: Hypoglycemia <40 mg/dL
- Urea cycle disorders: Hyperammonemia >100 μmol/L
- Fatty acid oxidation defects: Hypoketotic hypoglycemia
- Carnitine deficiency: <20 μmol/L (normal 25-50 μmol/L)
- Acylcarnitine elevation: >5x upper reference limit
📌 Remember: TOXIC - Toxic substrate accumulation, Organ damage progression, Xenobiotic pathway disruption, Intermediate metabolite buildup, Cascade amplification effects
| Pathway Type | Primary Defect | Accumulating Substrate | Deficient Product | Time to Symptoms |
|---|---|---|---|---|
| Amino Acid | Enzyme absence | Specific amino acid | Downstream products | Hours-days |
| Carbohydrate | Enzyme deficiency | Sugar intermediates | Glucose/energy | Minutes-hours |
| Lipid | Transport defect | Fatty acids | ATP/ketones | Hours-days |
| Urea Cycle | Enzyme mutation | Ammonia | Urea | Hours |
| Organic Acid | Cofactor defect | Organic acids | CoA derivatives | Days-weeks |
💡 Master This: Metabolic decompensation follows predictable triggers including fasting >12 hours, febrile illness >38.5°C, protein loads >2 g/kg/day, and catabolic stress, making prevention strategies highly effective when properly implemented.
Understanding pathway disruption patterns enables prediction of clinical presentations, optimal timing for intervention, and selection of appropriate monitoring parameters for long-term management of genetic metabolic disorders.
⚙️ Metabolic Pathway Disruption: The Biochemical Cascade Architecture
🎯 Pattern Recognition Mastery: The Clinical-Biochemical Correlation Framework
Systematic Recognition Patterns
-
Neurological Presentation Patterns
- Progressive developmental delay + specific odors
- MSUD: Maple syrup urine odor + encephalopathy
- PKU: Musty odor + intellectual disability
- Isovaleric acidemia: Sweaty feet odor + ketoacidosis
- Seizures + metabolic acidosis combinations
- Organic acidemias: pH <7.25 + anion gap >20
- Urea cycle defects: Ammonia >150 μmol/L + respiratory alkalosis
- Progressive developmental delay + specific odors
-
Hepatic Dysfunction Clusters
- Hepatomegaly + hypoglycemia patterns
- GSD Type I: Severe hypoglycemia + lactic acidosis
- Hereditary fructose intolerance: Post-fructose hypoglycemia
- Fatty acid oxidation defects: Hypoketotic hypoglycemia
- Liver dysfunction + specific metabolite elevation
- Tyrosinemia I: Succinylacetone >2 μmol/L + AFP elevation
- Galactosemia: Galactose-1-P >20 mg/dL + cataracts
- Hepatomegaly + hypoglycemia patterns
📌 Remember: CLUES - Clinical phenotype, Laboratory abnormalities, Unique odors, Enzyme deficiency patterns, Specific metabolite signatures
| Clinical Pattern | Key Biochemical Markers | Diagnostic Threshold | Confirmatory Test | Treatment Response |
|---|---|---|---|---|
| Intellectual disability + seizures | Phenylalanine | >6 mg/dL | PAH gene analysis | Phenylalanine-restricted diet |
| Cataracts + hepatomegaly | Galactose-1-P | >20 mg/dL | GALT enzyme activity | Galactose-free diet |
| Ketoacidosis + odor | Organic acids | >100 μmol/L | Urine organic acids | Protein restriction |
| Hypoglycemia + hepatomegaly | Glucose response | <40 mg/dL fasting | Enzyme analysis | Frequent feeding |
| Hyperammonemia + alkalosis | Ammonia | >100 μmol/L | Urea cycle enzymes | Nitrogen restriction |
💡 Master This: "See ketoacidosis with unusual odor, think organic acidemia; see hypoglycemia without ketones, think fatty acid oxidation defect; see hyperammonemia with respiratory alkalosis, think urea cycle disorder" - these pattern combinations enable rapid diagnostic triage.
Pattern recognition mastery transforms complex genetic presentations into systematic diagnostic approaches, enabling rapid identification and appropriate management of rare but treatable metabolic conditions.
🎯 Pattern Recognition Mastery: The Clinical-Biochemical Correlation Framework
🔍 Systematic Discrimination: The Differential Diagnosis Architecture
Quantitative Discrimination Framework
-
Amino Acid Disorder Differentiation
- PKU vs. Benign hyperphenylalaninemia
- PKU: Phenylalanine >20 mg/dL + Phe:Tyr ratio >3:1
- BH4 deficiency: Phenylalanine >6 mg/dL + Low biopterin
- Benign: Phenylalanine 2-6 mg/dL + Normal Phe:Tyr ratio
- MSUD vs. Other branched-chain disorders
- Classic MSUD: Leucine >4 mg/dL + Alloisoleucine present
- Variant forms: Leucine 2-4 mg/dL + Stress-induced elevation
- PKU vs. Benign hyperphenylalaninemia
-
Organic Acid Discrimination Patterns
- Methylmalonic vs. Propionic acidemia
- MMA: Methylmalonic acid >1000 μmol/L + B12 responsiveness testing
- PA: 3-OH-propionic acid >100 μmol/L + Biotin trial
- Isovaleric vs. Glutaric acidemia
- IVA: Isovalerylglycine >50 μmol/L + Sweaty feet odor
- GA-I: Glutaric acid >100 μmol/L + Macrocephaly
- Methylmalonic vs. Propionic acidemia
📌 Remember: DIFFER - Discriminatory metabolites, Interference patterns, Functional enzyme tests, Family studies, Enzyme activity ratios, Responsiveness to cofactors
| Disorder Pair | Primary Discriminator | Secondary Marker | Quantitative Threshold | Clinical Distinguisher |
|---|---|---|---|---|
| PKU vs BH4 deficiency | Biopterin levels | Dihydropteridine reductase | <2 nmol/L vs normal | Neurological progression |
| GSD I vs III | Glucose response | Lactate elevation | No response vs partial | Muscle involvement |
| MCAD vs LCAD | Acylcarnitine profile | C8 vs C14-C18 | >2 μmol/L specific chain | Age of presentation |
| Tyrosinemia I vs II | Succinylacetone | Tyrosine levels | Present vs absent | Liver vs eye involvement |
| MMA vs PA | Methylmalonic acid | Propionylcarnitine | >1000 vs <100 μmol/L | B12 responsiveness |
💡 Master This: Cofactor responsiveness testing distinguishes vitamin-responsive variants from enzyme-deficient forms in >80% of cases, with B12 for MMA, biotin for organic acidemias, and BH4 for PKU variants showing >50% metabolite reduction in responsive patients.
Systematic discrimination enables precise diagnosis of genetic disorders, ensuring appropriate treatment selection and accurate prognostic counseling for families facing complex metabolic conditions.
🔍 Systematic Discrimination: The Differential Diagnosis Architecture
⚖️ Treatment Algorithm Mastery: The Evidence-Based Intervention Framework
Evidence-Based Treatment Protocols
-
Immediate Stabilization Measures
- Hyperammonemia management (Ammonia >150 μmol/L)
- Sodium benzoate: 250-500 mg/kg/day IV
- Sodium phenylacetate: 250-500 mg/kg/day IV
- Arginine: 200-600 mg/kg/day for specific defects
- Hemodialysis if ammonia >500 μmol/L or neurological symptoms
- Metabolic acidosis correction (pH <7.25)
- Sodium bicarbonate: 1-2 mEq/kg to achieve pH >7.35
- Glucose infusion: 10-15 mg/kg/min to prevent catabolism
- Carnitine supplementation: 100-300 mg/kg/day
- Hyperammonemia management (Ammonia >150 μmol/L)
-
Long-term Management Strategies
- Dietary protein restriction protocols
- PKU: Phenylalanine 200-500 mg/day (age-dependent)
- MSUD: Leucine 300-600 mg/day with monitoring
- Urea cycle defects: Protein 0.8-1.2 g/kg/day maximum
- Cofactor supplementation regimens
- BH4-responsive PKU: 5-20 mg/kg/day sapropterin
- B12-responsive MMA: 1-10 mg/day hydroxocobalamin
- Biotin-responsive disorders: 10-40 mg/day biotin
- Dietary protein restriction protocols
📌 Remember: TREAT - Time-sensitive interventions, Restriction protocols, Emergency management, Antidote administration, Targeted supplementation
| Disorder | Emergency Intervention | Success Rate | Long-term Therapy | Monitoring Parameter |
|---|---|---|---|---|
| Hyperammonemia | Dialysis + scavengers | >95% if <24h | Protein restriction | Ammonia <80 μmol/L |
| Severe hypoglycemia | IV glucose + frequent feeds | >98% | Cornstarch therapy | Glucose >70 mg/dL |
| Metabolic acidosis | Bicarbonate + carnitine | >90% | Dietary modification | pH >7.35 |
| Acute encephalopathy | Branched-chain restriction | >85% | Formula therapy | Leucine <4 mg/dL |
| Ketoacidosis | Glucose + bicarbonate | >92% | Protein limitation | Ketones negative |
💡 Master This: Treatment success depends on maintaining metabolite levels within therapeutic ranges: Phenylalanine 2-6 mg/dL for PKU, Leucine <4 mg/dL for MSUD, Ammonia <80 μmol/L for urea cycle defects - exceeding these thresholds increases complication risk exponentially.
Evidence-based treatment algorithms provide systematic approaches to managing genetic disorders, optimizing outcomes through timely intervention and precise metabolic control.
⚖️ Treatment Algorithm Mastery: The Evidence-Based Intervention Framework
🔗 Multi-System Integration: The Metabolic Network Architecture
Integrated Network Disruption Patterns
-
Energy Metabolism Integration
- Glycogen storage diseases affecting liver + muscle + heart
- GSD Type I: Hepatic glucose production + renal dysfunction + growth retardation
- GSD Type II: Cardiac muscle + skeletal muscle + respiratory failure
- GSD Type III: Liver fibrosis + cardiomyopathy + myopathy
- Fatty acid oxidation defects spanning multiple tissues
- MCAD deficiency: Hepatic steatosis + cardiomyopathy + skeletal myopathy
- VLCAD deficiency: Rhabdomyolysis + retinal degeneration + neuropathy
- Glycogen storage diseases affecting liver + muscle + heart
-
Detoxification Network Disruptions
- Urea cycle defects creating systemic toxicity
- Hyperammonemia: CNS edema + hepatic dysfunction + coagulopathy
- Secondary effects: Glutamine elevation + BCAA depletion + neurotransmitter imbalance
- Organic acidemias affecting multiple pathways
- Methylmalonic acidemia: Renal tubular acidosis + bone marrow suppression + cardiomyopathy
- Propionic acidemia: Immunodeficiency + osteoporosis + developmental delay
- Urea cycle defects creating systemic toxicity
📌 Remember: NETWORK - Neurological effects, Energy disruption, Toxic accumulation, Waste elimination, Organ dysfunction, Regulatory imbalance, Kinetic pathway interference
| System Integration | Primary Pathway | Secondary Effects | Tertiary Complications | Management Priority |
|---|---|---|---|---|
| Glucose-Lactate-Lipid | Glycogenolysis | Lactic acidosis | Renal dysfunction | Glucose homeostasis |
| Amino Acid-Urea-Neurotransmitter | Protein catabolism | Hyperammonemia | Cerebral edema | Nitrogen elimination |
| Fatty Acid-Ketone-Energy | β-oxidation | Hypoketotic hypoglycemia | Cardiomyopathy | Energy substrate provision |
| Purine-Pyrimidine-DNA | Nucleotide synthesis | Immunodeficiency | Growth retardation | Metabolic balance |
| Heme-Iron-Oxygen | Porphyrin synthesis | Photosensitivity | Neuropathy | Substrate limitation |
💡 Master This: Understanding metabolic network integration enables predictive management - patients with fatty acid oxidation defects require cardiac monitoring every 6 months, ophthalmologic evaluation annually, and exercise restriction to prevent rhabdomyolysis during catabolic stress.
Recent research reveals epigenetic modifications in genetic disorders, where DNA methylation changes affect >200 genes in PKU patients, and microRNA dysregulation contributes to phenotypic variability in 85% of metabolic disorders, opening new therapeutic targets.
Multi-system integration understanding transforms genetic disorder management from single-pathway focus to comprehensive network-based approaches, optimizing outcomes through coordinated multi-organ monitoring and intervention strategies.
🔗 Multi-System Integration: The Metabolic Network Architecture
🎯 Clinical Mastery Arsenal: The Rapid Diagnostic Toolkit
Essential Diagnostic Arsenal
-
Rapid Recognition Triggers
- Neonatal presentations requiring immediate action
- Persistent vomiting + lethargy: Check ammonia within 2 hours
- Unusual odor + encephalopathy: Obtain urine organic acids stat
- Hypoglycemia without ketones: Measure acylcarnitines immediately
- Cataracts + hepatomegaly: Test galactose-1-phosphate urgently
- Childhood presentations with genetic implications
- Developmental regression + organomegaly: Lysosomal enzyme panel
- Recurrent ketoacidosis + specific odors: Organic acid analysis
- Exercise intolerance + myoglobinuria: Fatty acid oxidation studies
- Neonatal presentations requiring immediate action
-
Critical Laboratory Thresholds
- Emergency intervention levels
- Ammonia >150 μmol/L: Initiate scavenger therapy
- Glucose <40 mg/dL with ketones <0.5 mmol/L: Suspect FAO defect
- Lactate >5 mmol/L with normal perfusion: Consider metabolic disorder
- Anion gap >20 with ketones <3 mmol/L: Organic acidemia likely
- Emergency intervention levels
📌 Remember: MASTER - Metabolic emergencies, Abnormal odors, Specific thresholds, Timing critical, Enzyme defects, Rapid intervention protocols
| Clinical Scenario | Immediate Test | Critical Threshold | Emergency Action | Success Rate |
|---|---|---|---|---|
| Neonatal encephalopathy | Ammonia | >100 μmol/L | Protein restriction + scavengers | >90% if <24h |
| Unexplained hypoglycemia | Acylcarnitines | C8 >2 μmol/L | Avoid fasting + MCT oil | >95% prevention |
| Metabolic acidosis + odor | Urine organic acids | >100 μmol/L specific acids | Protein restriction + cofactors | >85% stabilization |
| Hepatomegaly + cataracts | Galactose-1-P | >20 mg/dL | Galactose-free diet | >98% if early |
| Developmental delay + seizures | Phenylalanine | >6 mg/dL | Phenylalanine restriction | >90% if <6 weeks |
💡 Master This: Pattern + Threshold + Action framework enables rapid diagnosis: Recognize the clinical pattern, confirm with specific biochemical thresholds, and implement evidence-based interventions - this systematic approach achieves >90% diagnostic accuracy in genetic disorders.
The clinical mastery arsenal transforms complex genetic disorder evaluation into systematic, time-efficient diagnostic and therapeutic protocols that optimize patient outcomes through rapid, evidence-based decision-making in both emergency and routine clinical settings.
🎯 Clinical Mastery Arsenal: The Rapid Diagnostic Toolkit
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app
























