Overview & Gastric Digestion - Gastric Gauntlet
- Protein Digestion: Breakdown of dietary proteins into absorbable amino acids & small peptides.
- Key Sites: Stomach (initiation), Small Intestine (completion).
- Gastric Gauntlet (Stomach Phase):
- Food entry stimulates gastrin release.
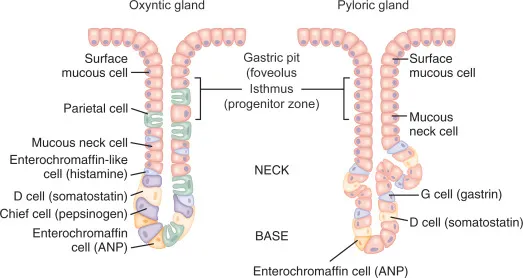
- Parietal Cells: Secrete HCl.
- Lowers gastric pH to 1.5-2.5.
- Denatures proteins (unfolds $2^\circ$/$3^\circ$ structures).
- Activates pepsinogen to pepsin.
- Chief Cells: Secrete Pepsinogen (inactive zymogen).
- Activated by HCl (pH < 5) & autocatalysis by pepsin.
- Pepsin: Endopeptidase, cleaves peptide bonds (prefers aromatic AAs: Phe, Tyr, Trp).
- Products: Large polypeptides, some oligopeptides.
- Limited digestion; prepares chyme for duodenum.
⭐ HCl not only activates pepsinogen but also provides the acidic environment optimal for pepsin activity (pH 1.5-3.5).
Intestinal Proteolysis - Pancreatic PowerPlay
Acidic chyme in duodenum stimulates S cells to release Secretin (↑ pancreatic $HCO_3^-$ for neutralization) and I cells to release Cholecystokinin (CCK) (↑ pancreatic enzyme secretion, gallbladder contraction). Pancreatic zymogens are crucial.
- Pancreatic Endopeptidases: Hydrolyze internal peptide bonds, producing smaller peptides.
- Trypsin: Specific for C-terminal of Lysine (Lys), Arginine (Arg).
- Chymotrypsin: Specific for C-terminal of Phenylalanine (Phe), Tyrosine (Tyr), Tryptophan (Trp), Leucine (Leu), Methionine (Met).
- Elastase: Specific for C-terminal of small, neutral amino acids like Alanine (Ala), Glycine (Gly), Serine (Ser).
- Pancreatic Exopeptidases: Remove one amino acid at a time from the C-terminus.
- Carboxypeptidase A: Cleaves C-terminal aromatic (Phe, Tyr, Trp) & neutral aliphatic AAs.
- Carboxypeptidase B: Cleaves C-terminal basic AAs (Lys, Arg).
⭐ Trypsin is the master activator of pancreatic proteases. Its deficiency (e.g., hereditary pancreatitis, cystic fibrosis) severely impairs protein digestion.
Absorption Mechanisms - Nutrient Gateway
- Location: Duodenum & Jejunum.
- Absorbable forms: Free amino acids (AAs), di- & tri-peptides.
- Amino Acid (AA) Absorption (Lumen → Enterocyte):
- Secondary active transport, Na⁺-dependent.
- Apical membrane: Specific carriers for different AA classes (neutral, acidic, basic, imino acids).
- E.g., SLC transporters (Solute Carrier family).
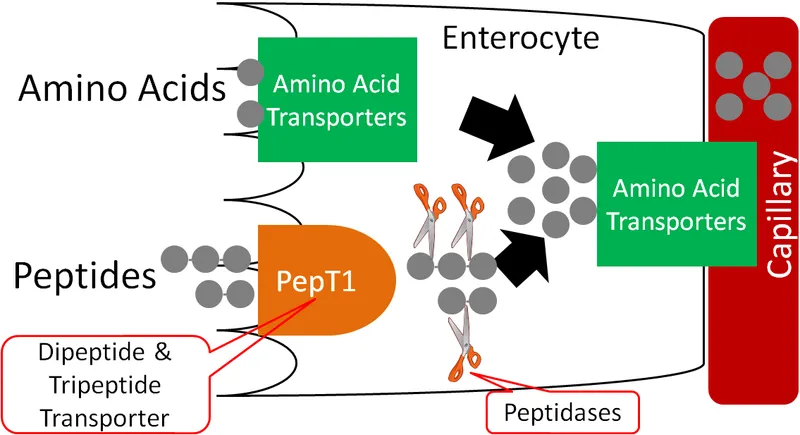
- Di- & Tri-peptide Absorption (Lumen → Enterocyte):
- PEPT1 transporter (H⁺-cotransporter); higher capacity & faster than AA transporters.
- Inside enterocyte: Cytosolic peptidases hydrolyze peptides to free AAs.
- Basolateral Transport (Enterocyte → Portal Blood):
- Facilitated diffusion & Na⁺-independent carriers transport AAs into portal circulation.
- Clinical Notes:
⭐ Hartnup disease: Defective neutral AA transporter (e.g., for tryptophan), leading to pellagra-like symptoms (dermatitis, diarrhea, dementia).
- Cystinuria: Defective dibasic AA (Cystine, Ornithine, Lysine, Arginine) transporter in kidney & intestine. 📌 Mnemonic: COLA. Leads to cystine kidney stones.
Clinical Tie-ins - Digestion Derailments
- Pancreatic Insufficiency: (Chronic pancreatitis, Cystic Fibrosis)
- Reduced enzyme (trypsin, chymotrypsin) secretion → protein maldigestion (azotorrhea).
- Celiac Disease:
- Gluten enteropathy → villous atrophy → impaired nutrient absorption.
- Hartnup Disease:
- Defect in neutral amino acid transporter (SLC6A19) in intestine & kidney.
- ↓ Tryptophan absorption → pellagra-like features (dermatitis, diarrhea, dementia).
- Cystinuria:
- Defect in dibasic amino acid transporter (COLA - Cystine, Ornithine, Lysine, Arginine).
- Poor cystine reabsorption → cystine kidney stones.
⭐ Hartnup disease: Niacin (B3) supplementation is beneficial as tryptophan, a niacin precursor, is malabsorbed.
High‑Yield Points - ⚡ Biggest Takeaways
- Pepsin (activated by HCl in stomach) initiates protein digestion.
- Enteropeptidase (brush border) activates trypsinogen to trypsin, key pancreatic activator.
- Pancreatic enzymes (e.g., trypsin, chymotrypsin) yield oligopeptides, di- & tripeptides.
- Amino acids are absorbed by Na+-dependent cotransporters; di/tripeptides by PepT1 (H+-dependent, faster).
- Hartnup disease: Defective neutral amino acid (e.g., tryptophan) transport.
- Cystinuria: Defective transport of COLA (Cysteine, Ornithine, Lysine, Arginine).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

