Potassium Balance: Introduction - K+ Kingpin
- $K^+$: Major intracellular cation; vital for cellular homeostasis & function ('Kingpin').
- Normal Serum $K^+$: 3.5-5.0 mEq/L.
- Distribution: ~98% intracellular (ICF), ~2% extracellular (ECF). Maintained by Na+/K+-ATPase.
- ICF $K^+$: ~140 mEq/L.
- ECF $K^+$: ~4 mEq/L.
- Key Roles:
- Maintains resting membrane potential (neuromuscular & cardiac excitability).
- Crucial for cardiac muscle contraction and rhythm.
- Involved in acid-base balance ($K^+$/$H^+$ exchange).
- Regulates intracellular fluid volume & enzyme activity.
- Influences insulin secretion.

⭐ The Na+/K+-ATPase pump is crucial for maintaining the high intracellular K+ concentration (approx. 140 mEq/L) compared to extracellular (approx. 4 mEq/L).
Potassium Balance: Regulation - The Balancing Act
Maintained by: 1. Renal excretion, 2. Transcellular shifts.
- Renal Regulation (DCT/CD - Principal Cells):
- ↑ K+ Secretion: Aldosterone, ↑ Plasma [K+], ↑ Tubular flow (diuretics), Alkalosis.
- ↓ K+ Secretion: Acidosis.
⭐ In the kidneys, the principal cells of the late distal tubule and collecting duct are the primary sites for potassium secretion, regulated mainly by aldosterone and plasma K+ concentration.
- Transcellular Shifts (Na+/K+ ATPase):
- K+ INTO cells (↓ Plasma K+): Insulin, β2-agonists, Alkalosis. 📌 Insulin & Beta-agonists Alkalize K+ IN.
- K+ OUT of cells (↑ Plasma K+): Acidosis, α-agonists, Cell lysis, Hyperosmolarity, Exercise.

Potassium Balance: Hypokalemia - Low K+ Woes
Serum K+ < 3.5 mEq/L.
Etiology:
- ↓ Intake: Starvation.
- Cellular Shift (K+ into cells): Alkalosis, Insulin, β2-agonists.
- ↑ Losses:
- Renal: Diuretics (Loop/Thiazide), Hyperaldosteronism, RTA.
- GI: Diarrhea, Vomiting.
Clinical Features:
- Muscle: Weakness, fatigue, cramps, paralysis.
- GI: Constipation, ileus.
- Cardiac: Arrhythmias, palpitations.
⭐ Hypokalemia potentiates digitalis toxicity by increasing its binding to the Na+/K+-ATPase pump, leading to increased risk of arrhythmias.
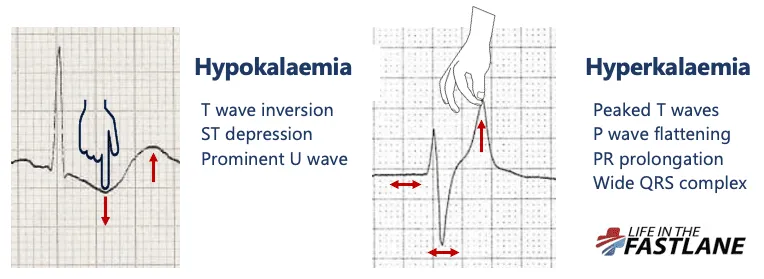
ECG Changes: (Sequence: T↓ → U↑ → ST↓ → PR↑)
- Flattened/inverted T wave
- Prominent U wave
- ST depression
- Prolonged PR interval
- Severe: Ventricular tachycardia/fibrillation (VT/VF).
- 📌 Mnemonic: "Low T, High U, ST low, PR long too."
Management:
- Oral KCl preferred for mild/asymptomatic.
- IV KCl for severe (K+ < 2.5 mEq/L) or symptomatic.
- Max IV rate: 10-20 mEq/hr (peripheral). Max conc: 40 mEq/L (peripheral).
- ⚠️ Always check & correct Mg2+ deficiency (hypomagnesemia impairs K+ repletion).
Potassium Balance: Hyperkalemia - High K+ Alert
Serum K+ > 5.5 mEq/L.
Causes:
- ↑ Intake: Iatrogenic.
- ↓ Excretion: Renal failure, ACEi/ARBs, K+-sparing diuretics (e.g., Spironolactone), Addison's disease.
- Shift K+ (ICF → ECF): Acidosis, Insulin deficiency (DKA), tissue damage (rhabdomyolysis, burns, tumor lysis), β-blockers, Digoxin toxicity.
- Pseudohyperkalemia (e.g., hemolysis during phlebotomy).
Clinical Features: Muscle weakness, flaccid paralysis, paresthesias, abdominal distension, diarrhea, cardiac arrhythmias.
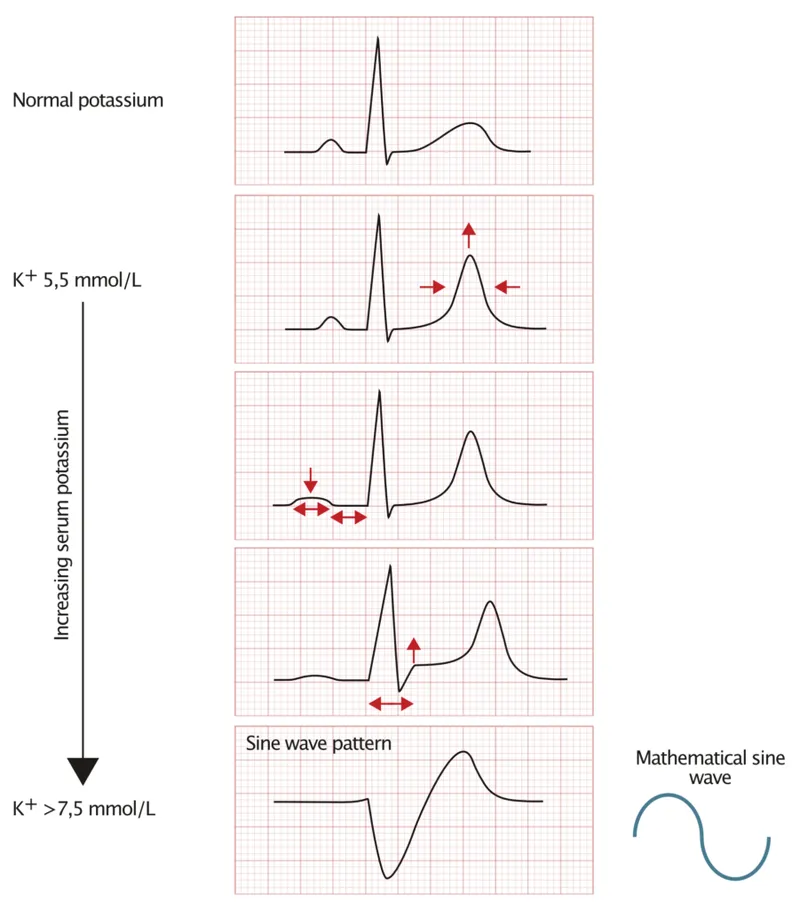
ECG Progression (approximate K+ levels):
-
6.0 mEq/L: Tall, peaked T waves (earliest sign).
-
6.5 mEq/L: PR interval prolongation, P wave flattening or loss.
-
7.0 mEq/L: QRS complex widening.
-
8.0 mEq/L: Sine wave pattern, ventricular fibrillation, asystole.
Management: 📌 Mnemonic "C BIG K Drop"
⭐ IV Calcium gluconate is the first-line emergency treatment for cardiac membrane stabilization in severe hyperkalemia with ECG changes; it does not lower serum K+ levels but protects the heart.
High‑Yield Points - ⚡ Biggest Takeaways
- Major intracellular cation; vital for nerve/muscle excitability & cardiac function.
- Kidneys primarily regulate K+ balance; aldosterone ↑ K+ excretion.
- Insulin & β-agonists shift K+ into cells (↓ serum K+).
- Acidosis (↓pH) shifts K+ out (↑ serum K+); alkalosis (↑pH) shifts K+ in (↓ serum K+).
- Hyperkalemia ECG: Peaked T waves, wide QRS, PR prolongation.
- Hypokalemia ECG: U waves, flat/inverted T, ST depression.
- Loop/thiazide diuretics → hypokalemia; K+-sparing diuretics → hyperkalemia.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

