Ca & P Homeostasis - The Balancing Act
- Calcium (Ca): 99% in bone. Serum total: 8.5-10.5 mg/dL.
- Ionized Ca (~50%) is physiologically active.
- Bound to albumin (~40%), complexed (~10%).
- Phosphate (P): 85% in bone. Serum: 2.5-4.5 mg/dL.
- Crucial for ATP, DNA/RNA, cell membranes.
- Dynamic balance: Maintained by PTH, Vitamin D, Calcitonin.
- Key sites: Bone (reservoir), kidney (excretion/reabsorption), gut (absorption).
- 📌 Ca x P product: Important for bone mineralization.
⭐ Ionized calcium (normal: 4.5-5.6 mg/dL or 1.12-1.4 mmol/L) is the critical fraction for neuromuscular excitability and cardiac function.
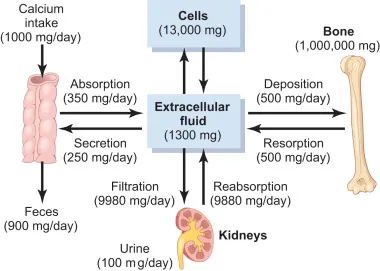
Parathyroid Hormone (PTH) - Calcium's Chief Conductor
- Source: Chief cells (parathyroid glands).
- Regulation:
- Major: ↓ Serum $Ca^{2+}$ (via CaSR).
- Minor: ↑ Serum $PO_4^{3-}$, ↓ $1,25(OH)_2D_3$.
- $Mg^{2+}$: Severe ↓ inhibits PTH. 📌 "Magnesium is a drag, too low or too high, PTH will lag".
- Actions (Net: ↑ Serum $Ca^{2+}$, ↓ Serum $PO_4^{3-}$):
- Bone: ↑ Resorption (↑ osteoclast activity).
- Kidney:
- ↑ $Ca^{2+}$ reabsorption (DCT).
- ↓ $PO_4^{3-}$ reabsorption (PCT) -> phosphaturia.
- ↑ 1α-hydroxylase -> ↑ $1,25(OH)_2D_3$.
- Intestine (indirect): ↑ $Ca^{2+}$ & $PO_4^{3-}$ absorption (via Vit D).
actions on bone, kidney, and intestine to regulate calcium and phosphate)
⭐ PTH causes phosphaturia, a key mechanism to prevent calcium phosphate precipitation when mobilizing calcium from bone and increasing intestinal absorption.
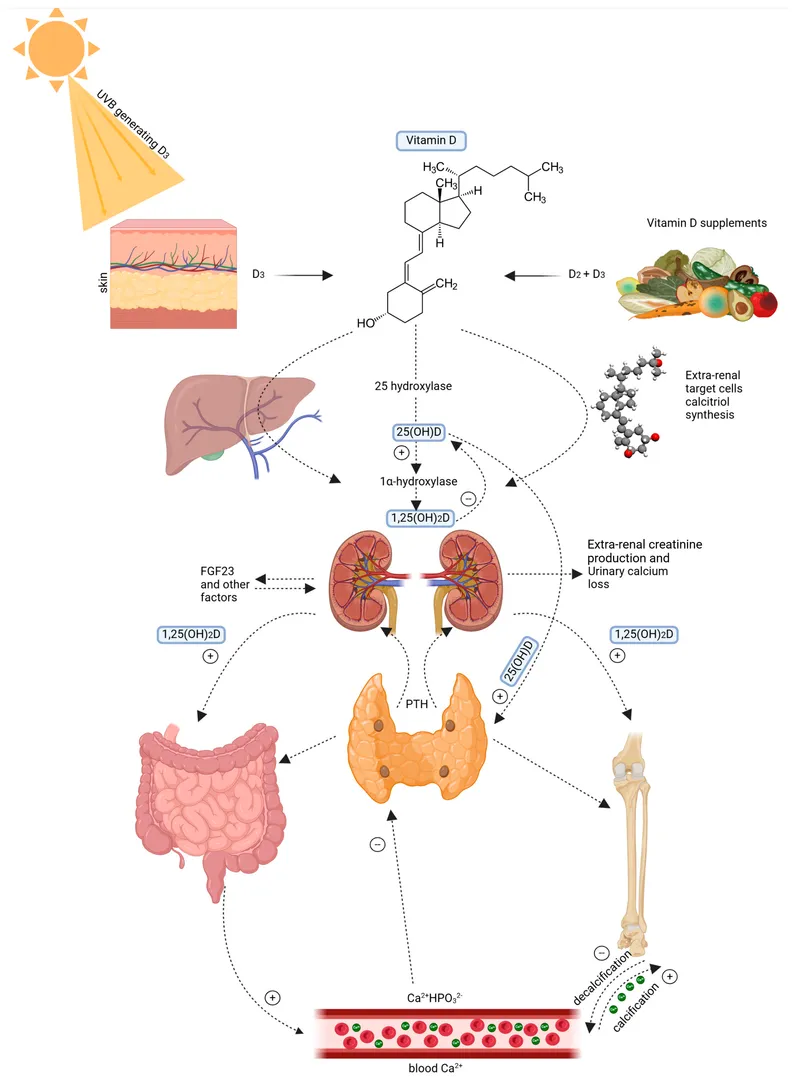
Vitamin D - Sunshine Steroid
- Sources: Sunlight (D₃ - cholecalciferol), Diet (D₂ - ergocalciferol, D₃).
- Synthesis & Activation: 📌 Mnemonic (Activation): Skin (Sun) → Liver → Kidney.
- Skin (UVB): 7-Dehydrocholesterol → Cholecalciferol (D₃).
- Liver: D₃/D₂ → 25-Hydroxyvitamin D (Calcidiol) via 25-hydroxylase.
- Kidney: Calcidiol → $1,25(OH)_2D_3$ (Calcitriol - active) via 1α-hydroxylase.
- Stimulated by: PTH, ↓Ca²⁺, ↓PO₄³⁻.
- Inhibited by: FGF-23, ↑Ca²⁺, ↑PO₄³⁻.
- Actions (Calcitriol):
- Gut: ↑↑Ca²⁺ & ↑↑PO₄³⁻ absorption.
- Kidney: ↑Ca²⁺ & ↑PO₄³⁻ reabsorption (synergistic with PTH for Ca²⁺).
- Bone:
- Mineralization (indirectly by ↑serum Ca²⁺/PO₄³⁻).
- Resorption (direct on osteoblasts → stimulate osteoclasts; high doses).
⭐ Calcitriol is the most potent stimulator of intestinal calcium and phosphate absorption.
Calcitonin & FGF-23 - Fine-Tuning Factors
- Calcitonin:
- Source: Thyroid C-cells (parafollicular).
- Effect: ↓ serum $Ca^{2+}$; inhibits osteoclasts, ↑ renal $Ca^{2+}$ excretion.
- Minor role in $Ca^{2+}$ homeostasis in humans.
- 📌 Calcitonin tones down calcium.
- FGF-23:
- Source: Osteocytes/osteoblasts.
- Effect: ↓ serum $PO_4^{3-}$; ↓ renal $PO_4^{3-}$ reabsorption, ↓ 1α-hydroxylase activity (↓ active Vit D).
- Needs Klotho co-receptor.
⭐ FGF-23 is a key phosphaturic hormone, also suppressing calcitriol production.
Mineral Imbalances - Clinical Snapshots
- Hypercalcemia (Ca > 10.5 mg/dL):
- Symptoms: "Stones (renal), bones (pain), groans (abdominal), thrones (polyuria), psychiatric overtones".
- ECG: Short QT interval.
- Hypocalcemia (Ca < 8.5 mg/dL):
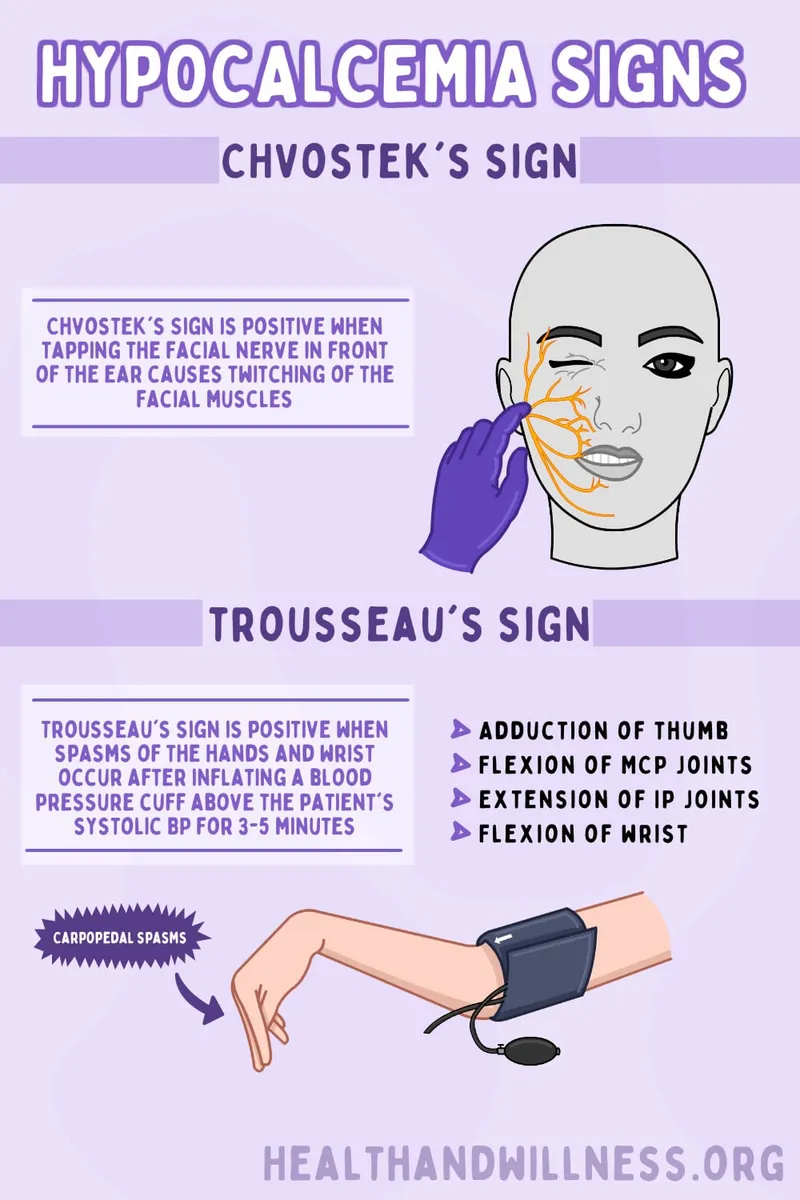
- Symptoms: Tetany (Chvostek's, Trousseau's signs), paresthesias, seizures. 📌 CATS (Convulsions, Arrhythmias, Tetany, Spasms).
- ECG: Prolonged QT interval.
- Hyperphosphatemia (PO₄ > 4.5 mg/dL):
- Often asymptomatic; chronic: vascular calcification, soft tissue deposits.
- Hypophosphatemia (PO₄ < 2.5 mg/dL):
- Muscle weakness, rhabdomyolysis, respiratory failure, altered mental status.
- Muscle weakness, rhabdomyolysis, respiratory failure, altered mental status.
⭐ Trousseau's sign (carpal spasm after sphygmomanometer cuff inflation) is more specific for hypocalcemia than Chvostek's sign (facial muscle twitch on tapping facial nerve).
High‑Yield Points - ⚡ Biggest Takeaways
- PTH ↑ serum Ca²⁺ & ↓ PO₄³⁻ via bone resorption & kidney effects.
- Vitamin D (Calcitriol) ↑ intestinal Ca²⁺ & PO₄³⁻ absorption.
- Calcitonin weakly ↓ serum Ca²⁺ by inhibiting osteoclasts.
- Primary Hyperparathyroidism: ↑ PTH, ↑ Ca²⁺, ↓ PO₄³⁻ ("stones, bones, groans").
- Hypoparathyroidism: ↓ PTH, ↓ Ca²⁺, ↑ PO₄³⁻, causing tetany.
- CKD causes Secondary Hyperparathyroidism: ↑ PTH, ↑ PO₄³⁻, variable Ca²⁺.
- FGF-23: Key phosphaturic hormone, inhibits Vitamin D activation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

