Perioperative Pain Fundamentals - Setting the Stage
- Perioperative pain: Acute pain occurring before, during, and after surgery.
- Effective management is crucial:
- Reduces complications (e.g., DVT, atelectasis, ileus)
- Improves patient satisfaction & outcomes
- Facilitates early mobilization & faster recovery
- Prevents Chronic Post-Surgical Pain (CPSP)
- Key Pain Types:
- Nociceptive: Activation of nociceptors (somatic, visceral)
- Neuropathic: Lesion or disease of somatosensory nervous system
- Nociplastic: Altered nociception despite no clear evidence of tissue damage or neuropathy (e.g., fibromyalgia)
- Core Principle: Multimodal Analgesia (MMA) - using ≥2 analgesic agents/techniques with different mechanisms.

⭐ Inadequate acute postoperative pain control is a primary risk factor for developing Chronic Post-Surgical Pain (CPSP), which can affect 10-50% of patients after common surgeries, significantly impacting quality of life.
Pre-Op & Intra-Op Game Plan - Pain Blockade Tactics
-
Pre-Op Game Plan:
- Assess: Pain Hx, anxiety, comorbidities, current medications.
- Counsel: Discuss pain management plan, set realistic expectations.
- Pre-emptive Analgesia (PO): 📌 GAP Mnemonic
- Gabapentinoid (e.g., Pregabalin 75-150mg) if high neuropathic risk.
- Acetaminophen (Paracetamol 1g).
- PNSAID (e.g., Etoricoxib 60-120mg).
-
Intra-Op Blockade Tactics:
- Core Principle: Multimodal Analgesia (MMA).
- Regional Anesthesia (RA) - Prioritize when feasible:
- Neuraxial: Epidural (catheter for post-op analgesia), Spinal.
- Peripheral Nerve Blocks (PNBs): Ultrasound-guided (USG) for accuracy (e.g., Brachial plexus, Femoral, TAP block).
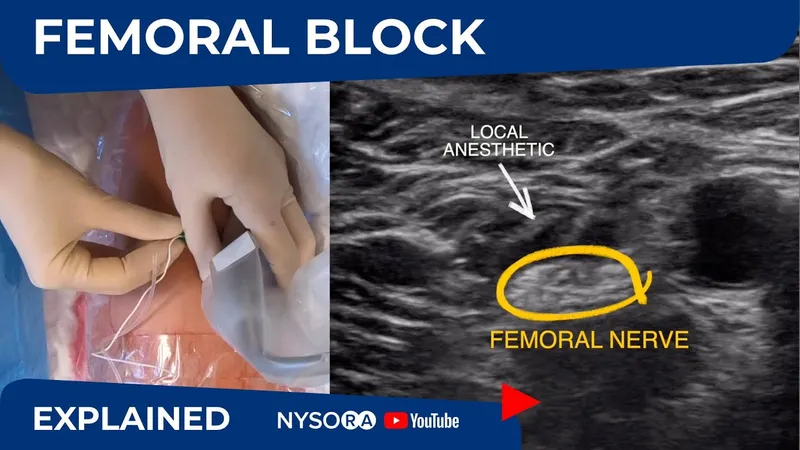
- Systemic Adjuncts (Opioid-Sparing Focus):
- IV Paracetamol 1g.
- IV NSAID (e.g., Ketorolac 30mg).
- Low-dose Ketamine (e.g., 0.25-0.5mg/kg bolus, then 2-5mcg/kg/min infusion).
- IV Lidocaine infusion (e.g., 1.5mg/kg bolus, then 1-2mg/kg/hr).
- Dexamethasone (4-8mg IV) - anti-inflammatory, anti-emetic effects.
⭐ Employing regional anesthesia as part of MMA significantly ↓ opioid needs, enhancing recovery & ↓ adverse effects.
Post-Op Pain Control - The Recovery Blueprint
- Goal: Optimal analgesia, facilitate early mobilization, ↓post-op complications.
- Assessment: Regular pain scores (VAS, NRS); reassess post-intervention. Document findings.
- Multimodal Analgesia (MMA): Core strategy. Synergistic effect, ↓opioid needs & side effects.
- Paracetamol: IV/Oral. Max 4g/day. Foundational.
- NSAIDs/COXIBs: e.g., Ketorolac. ⚠️ GI/Renal/CV risks.
- Opioids: IV PCA (Morphine), Oral (Tramadol). Monitor sedation, N/V. Naloxone for reversal.
- Regional: Epidurals, Nerve blocks (e.g., TAP). Excellent for major surgery.
- Adjuvants: Gabapentinoids, low-dose Ketamine. Target neuropathic elements.
- ERAS Protocols: Emphasize opioid-sparing, early nutrition & ambulation.

⭐ IV Paracetamol 1g Q6H is a cornerstone of opioid-sparing multimodal analgesia, significantly reducing total opioid consumption.
Special Scenarios & Sidekicks - Managing Curveballs
- Opioid-Tolerant: ↑ baseline needs (25-100% more). Multimodal vital (ketamine, regional).
- Chronic Pain Pts: Continue baseline meds. Manage expectations. Multimodal for acute pain.
- Obstructive Sleep Apnea (OSA): High OIRD risk. 📌 STOP-BANG (≥3 high risk). Prefer regional, non-opioids. Cautious opioids, CPAP.
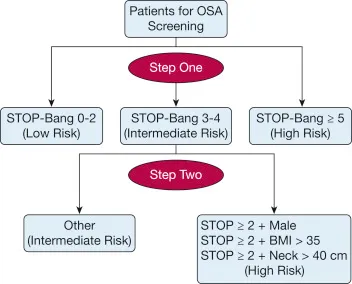
- Elderly: ↓ clearance, ↑ sensitivity. "Start low, go slow." Reduce NSAID/opioid doses (e.g., by 50%).
- Renal Impairment (e.g., GFR <30 mL/min): Avoid morphine, NSAIDs. Fentanyl, paracetamol safer.
- Hepatic Impairment: Paracetamol max 2g/day. Cautious opioid titration (e.g., fentanyl, hydromorphone).
- Acute Pain Service (APS): Consult for complex pain, advanced techniques (e.g., PCA, epidurals).
⭐ For patients on chronic buprenorphine, continue it perioperatively and add short-acting opioids as needed for acute pain; do not abruptly stop buprenorphine due to withdrawal risk and difficult pain control.
High‑Yield Points - ⚡ Biggest Takeaways
- Multimodal analgesia is standard care, combining diverse drug classes for optimal effect.
- Pre-emptive analgesia, administered before incision, aims to minimize central sensitization.
- Regional techniques (epidurals, nerve blocks) offer excellent pain relief and reduce systemic opioid needs.
- NSAIDs and Paracetamol are key opioid-sparing drugs; always check NSAID contraindications.
- Opioids provide potent analgesia; monitor closely for respiratory depression and other side effects.
- Consider Gabapentinoids as adjuvants for neuropathic pain and reducing opioid use.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

