Cancer Pain Fundamentals - The Painful Truth
- Prevalence: Affects 50-80% of cancer patients, severely impacting Quality of Life (QoL).
- Etiology: Tumor invasion/compression, treatment side-effects (chemo, radio, surgery), paraneoplastic syndromes.
- Types: Nociceptive (somatic, visceral), neuropathic; often mixed.
- Assessment: Crucial. Use PQRST mnemonic (📌). Scales: Numeric Rating Scale (NRS 0-10), Visual Analog Scale (VAS), Brief Pain Inventory (BPI).
⭐ The WHO three-step analgesic ladder is a cornerstone of cancer pain management, guiding stepwise opioid and adjuvant use. oka
WHO Ladder & Basics - Stepping Up Relief
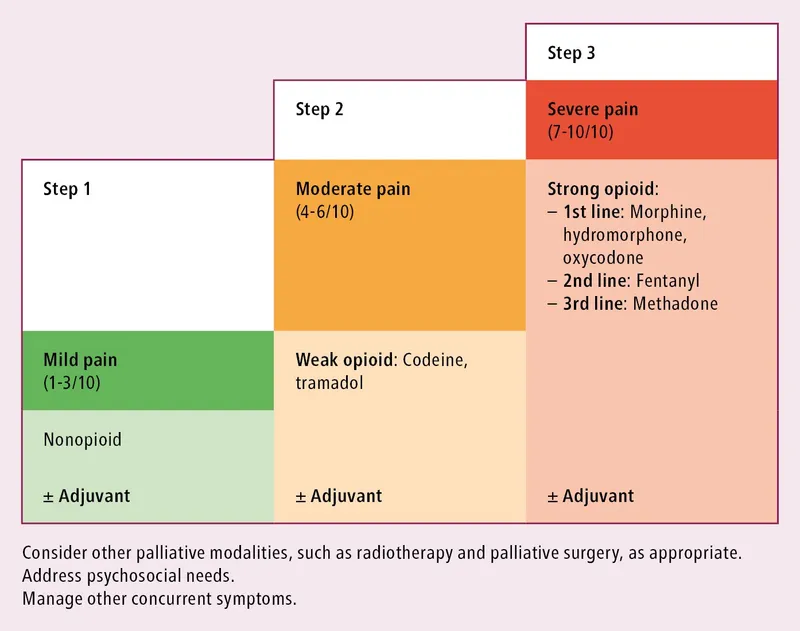
WHO 3-step ladder: Key principles are "By the mouth", "By the clock", "By the ladder", and individualized therapy.
- Step 1 (Mild Pain): Non-opioid (e.g., Paracetamol, NSAID) ± Adjuvant.
- Step 2 (Moderate Pain): Weak opioid (e.g., Tramadol, Codeine) ± Non-opioid ± Adjuvant.
- Step 3 (Severe Pain): Strong opioid (e.g., Morphine, Fentanyl) ± Non-opioid ± Adjuvant.
- Adjuvants (e.g., Gabapentinoids, TCAs) for specific pain types.
⭐ Prophylactic laxatives (e.g., senna + docusate) should be prescribed with opioids to prevent constipation.
Opioid Arsenal - Potent Painkillers
- Morphine: Gold standard (PO, IV, SC).
- M6G (active metabolite, renal excretion).
- SE: Nausea, constipation, sedation, resp. depression.
- Fentanyl: Potent (80-100x morphine).
- Patch (stable chronic pain), transmucosal (BTcP).
- Safer in renal failure.
- Methadone: Long, variable T½. Mu-agonist, NMDA antagonist (neuropathic pain).
- ⚠️ QT prolongation risk; careful titration.
- Tapentadol: Mu-agonist & NRI (Norepinephrine Reuptake Inhibitor).
- ↓ constipation compared to other opioids.
- Buprenorphine: Partial mu-agonist.
- Ceiling effect on respiratory depression.
- Sublingual, transdermal routes.
- Tramadol: Weak mu-agonist, SNRI.
- Max dose 400mg/day.
- Seizure risk; serotonin syndrome risk.
⭐ M6G (morphine's active metabolite) accumulates in renal failure; consider dose ↓ or switch opioid (e.g., to fentanyl or methadone).
Adjuvants & Co-analgesics - Helper Meds
- Purpose: Enhance opioid efficacy, manage specific pain types (neuropathic, bone), reduce opioid side effects.
- Neuropathic Pain:
- Antidepressants: Amitriptyline (10-25 mg HS), Duloxetine (30-60 mg OD).
- Anticonvulsants: Gabapentin (start 100-300 mg), Pregabalin (start 25-75 mg).
- Bone Pain:
- NSAIDs (use cautiously).
- Corticosteroids: Dexamethasone (4-8 mg BD) for inflammation, nerve compression.
- Bisphosphonates (e.g., Zoledronic acid), Denosumab.
- Other Key Adjuvants:
- Ketamine (low dose): Refractory neuropathic pain, opioid-induced hyperalgesia.
⭐ For neuropathic cancer pain, gabapentinoids (Gabapentin, Pregabalin) and TCAs (Amitriptyline) are often first-line adjuvants.
Interventional Strategies - Beyond Pills
- Neurolytic Blocks: Chemical (alcohol) or thermal ablation.
- Celiac plexus (pancreatic, upper GI cancer).
- Superior hypogastric plexus (pelvic pain).
- Ganglion Impar (perineal, coccygeal pain).
- Intrathecal Drug Delivery (IDDS): Refractory pain; opioids, ziconotide.
- Spinal Cord Stimulation (SCS): Neuropathic pain.
- Vertebroplasty/Kyphoplasty: Painful vertebral fractures.
- Cordotomy: For intractable unilateral somatic pain.
⭐ Celiac plexus neurolysis offers significant pain relief for 60-90% of patients with pancreatic cancer pain.
High‑Yield Points - ⚡ Biggest Takeaways
- The WHO analgesic ladder (non-opioid → weak opioid → strong opioid) is fundamental for cancer pain management.
- Opioids (e.g., morphine, fentanyl) are central; titrate to effect and proactively manage side effects like constipation.
- Adjuvant analgesics (gabapentinoids, TCAs, corticosteroids) are crucial for neuropathic or bone pain.
- Non-opioid analgesics (NSAIDs, paracetamol) are used for mild pain or as adjuncts; monitor NSAID toxicity.
- Interventional techniques (nerve blocks, neurolysis, spinal opioids) are considered for severe, refractory pain.
- Address breakthrough pain with short-acting opioids; regular pain assessment and reassessment are vital for effective therapy.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

