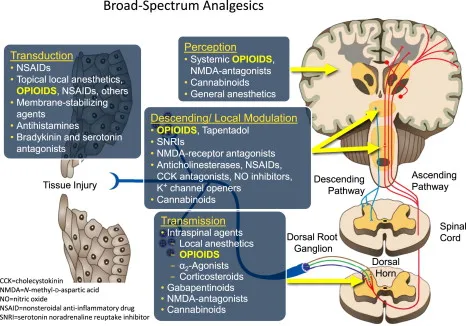
Adjuvant Basics - Pain's Sidekicks
- Definition: Drugs with primary indications other than pain, but enhance analgesia or manage analgesic side effects.
- Purpose:
- Improve efficacy of primary analgesics (opioids, NSAIDs).
- Provide analgesia in specific pain types (e.g., neuropathic).
- Reduce side effects of primary analgesics, allowing dose reduction.
- Key Categories:
- Antidepressants (TCAs, SNRIs)
- Anticonvulsants (Gabapentinoids)
- Corticosteroids
- NMDA Antagonists (Ketamine)
- Alpha-2 Agonists (Clonidine)
⭐ Adjuvant analgesics are primarily indicated for conditions other than pain but provide analgesia in specific pain states, especially neuropathic pain.
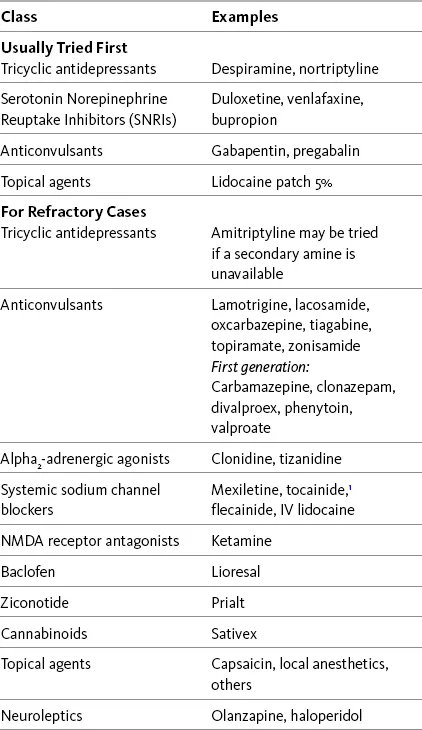
Antidepressants & Anticonvulsants - Nerve Calm Crew
- Antidepressants (Neuropathic Pain)
- TCAs (Amitriptyline, Nortriptyline)
- Mech: ↑NE/5-HT, Na+ block.
- Amitriptyline: 10-25mg HS to 75-150mg.
- SEs: Anticholinergic, sedation. 📌 "Tri-CyclicS": Sedation, Cardiac, antiSlud.
- Nortriptyline: Often better tolerated.
- SNRIs (Duloxetine, Venlafaxine)
- Mech: ↑NE/5-HT.
- Duloxetine: 30-60mg/d (diabetic neuropathy).
- Venlafaxine: 75-225mg/d.
- SEs: Nausea, dizziness.
- TCAs (Amitriptyline, Nortriptyline)
- Anticonvulsants (Neuropathic Pain)
- Gabapentinoids (Gabapentin, Pregabalin)
- Mech: α2δ Ca2+ channel ligand.
- Gabapentin: 100-300mg TDS to 3600mg/d.
- Pregabalin: 25-75mg BD/TDS to 300-600mg/d.
- SEs: Dizziness, somnolence, edema.
- Carbamazepine
- Trigeminal Neuralgia DOC. Dose: 200-1200mg/d.
- ⚠️ Monitor: Agranulocytosis.
- Gabapentinoids (Gabapentin, Pregabalin)
⭐ Amitriptyline (TCA) is often a first-line adjuvant for neuropathic pain, but its anticholinergic side effects limit use; Pregabalin often preferred for better tolerability.
Steroids & NMDA Blockers - Pathway Modulators
-
Corticosteroids (e.g., Dexamethasone, Prednisolone)
- Mechanism: Potent anti-inflammatory; ↓ edema, ↓ ectopic neuronal firing. Inhibit phospholipase A2.
- Uses: Neuropathic pain (nerve compression, tumor infiltration), inflammatory pain, cancer pain.
- Dexamethasone: 4-8 mg BD/TDS for nerve compression pain, then taper.
- Side Effects (long-term): Hyperglycemia, immunosuppression.
⭐ Dexamethasone is particularly useful for pain from nerve compression by tumors due to its potent anti-inflammatory and edema-reducing effects.
-
NMDA Receptor Antagonists (e.g., Ketamine, Memantine)
- Mechanism: Block NMDA receptors in dorsal horn; ↓ central sensitization, wind-up, opioid tolerance.
- Uses: Neuropathic pain, opioid-resistant pain, CRPS, phantom limb pain.
- Ketamine: Sub-anesthetic dose (e.g., 0.1-0.5 mg/kg IV). Risk: psychomimetic effects.
- Memantine: Oral, 5-20 mg/day. Better tolerated, less potent.
α2-Agonists & Topicals - Targeted Relief
- α2-Adrenergic Agonists
- Clonidine: Oral, transdermal, epidural. Reduces sympathetic tone, opioid-sparing.
- Dexmedetomidine: IV. Highly selective. Sedation, analgesia.
- Common Side Effects: Hypotension, bradycardia, sedation.
⭐ Clonidine, an alpha-2 agonist, can potentiate opioid analgesia and reduce opioid requirements, useful in managing chronic pain and opioid tolerance.
- Topical Agents (Local Action, ↓ Systemic AEs)
- NSAIDs (e.g., Diclofenac gel): Osteoarthritis, sprains.
- Capsaicin cream/patch: Neuropathic pain (postherpetic neuralgia). Depletes substance P. 📌 "Capsaicin burns P(ain) away."
- Lidocaine 5% patch: Postherpetic neuralgia, localized neuropathic pain.
High‑Yield Points - ⚡ Biggest Takeaways
- TCAs (amitriptyline) & SNRIs (duloxetine) are first-line for neuropathic pain.
- Gabapentinoids (gabapentin, pregabalin) are crucial for neuropathic pain and fibromyalgia.
- Corticosteroids (dexamethasone) reduce inflammatory and nerve compression pain.
- Ketamine (NMDA antagonist) targets central sensitization and opioid-refractory pain.
- Alpha-2 agonists (clonidine) aid in neuropathic pain and opioid sparing.
- Bisphosphonates (zoledronate) manage cancer-related bone pain.
- Topical lidocaine provides relief for localized neuropathic pain like Postherpetic Neuralgia (PHN).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

