Acute Pain Management: Intro & Assessment - Ouch Meter Reading
- Acute Pain: Sudden onset, typically <3 months, direct result of tissue injury. Serves a protective biological function.
- Types: Nociceptive (somatic, visceral), Neuropathic.
- Pain Assessment: Crucial for diagnosis, guiding treatment, and monitoring efficacy.
- PQRST Mnemonic (📌): Provocation/Palliation, Quality, Radiation, Severity, Timing.
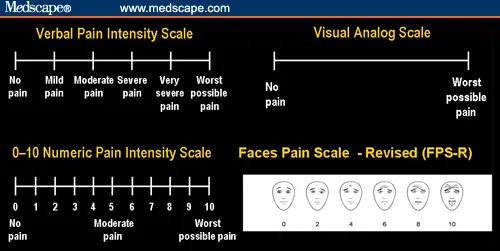
- Self-Report Scales (Gold Standard):
- Numeric Rating Scale (NRS): Score 0 (no pain) to 10 (worst imaginable pain).
- Visual Analog Scale (VAS): 100mm line, patient marks pain level.
- Faces Pain Scale-Revised (FPS-R): For children or those with communication difficulties.
- Behavioral Scales (Non-verbal patients):
- FLACC Scale: Face, Legs, Activity, Cry, Consolability (children 2 months - 7 years).
- CPOT: Critical-Care Pain Observation Tool (adult ICU patients).
⭐ Self-report of pain is the most reliable indicator; always attempt to elicit it if possible, even in challenging patient populations (e.g., mild cognitive impairment).
Acute Pain Management: Pharmacotherapy - Painkiller Parade
- WHO Analgesic Ladder: Guides drug selection.
- Non-Opioids:
- Paracetamol (PCM): Analgesic, antipyretic. Max 4g/day. Risk: Hepatotoxicity.
- NSAIDs (e.g., Ibuprofen, Diclofenac): COX inhibitors; anti-inflammatory.
- Max: Ibuprofen 2.4g/day, Diclofenac 150mg/day.
- S/E: GI ulcers, renal toxicity, ↑CV risk. 📌 NSAID: No pee, Stomach ulcers, Asthma, Increased bleeding, Dyspepsia.
- Weak Opioids:
- Tramadol: Max 400mg/day. SNRI activity; lowers seizure threshold.
- Codeine: Prodrug (CYP2D6 to morphine); antitussive.
- Strong Opioids: Morphine, Fentanyl, Pethidine.
- Morphine: Gold standard. Oral:IV approx 1:3. Active metabolites M6G (analgesic), M3G (neurotoxic).
- Fentanyl: Potent (80-100x morphine). IV, transdermal; rapid onset, short duration.
- Pethidine: Norpethidine (neurotoxic metabolite). Max 600mg/24h for <48h. Avoid in renal failure/elderly.
- S/E: Nausea, vomiting, constipation, sedation, respiratory depression (reverse with Naloxone).
- Adjuvants: Enhance analgesia or treat specific pain types.
- e.g., Gabapentinoids (Gabapentin, Pregabalin) for neuropathic pain; Amitriptyline (TCA); Ketamine (NMDA antagonist) for opioid-sparing.

⭐ Pethidine is contraindicated with MAO inhibitors due to high risk of serotonin syndrome or hypertensive crisis.
Acute Pain Management: Regional Techniques - Zone Defense
- Goal: Localized analgesia by blocking nerve transmission.
- Peripheral Nerve Blocks (PNBs):
- Upper Limb: Interscalene, Supraclavicular, Axillary (Brachial Plexus).
- Lower Limb: Femoral, Sciatic, Popliteal.
- Truncal: TAP (Transversus Abdominis Plane), Paravertebral, Intercostal.
- Neuraxial Analgesia:
- Epidural: Thoracic/Lumbar; continuous via catheter.
- Spinal (Intrathecal): Single shot; rapid, dense block.
- Agents: Local Anesthetics (e.g., Bupivacaine, Ropivacaine); Adjuvants (e.g., epinephrine, dexmedetomidine) prolong duration.
- Benefits: Superior pain relief, opioid-sparing, ↓PONV (Postoperative Nausea and Vomiting), early mobilization.
- Risks: LAST (Local Anesthetic Systemic Toxicity), nerve injury, hematoma, infection.
⭐ Epidural analgesia is a gold standard for labor analgesia and post-thoracotomy pain.
- 📌 LAST early CNS signs: Metallic taste, Numbness (oral/tongue), Tinnitus, Dizziness, Visual disturbances (Mnemonic: My New Telephone Doesn't Vibrate).

Acute Pain Management: Special Contexts & Adjuncts - Tricky Pains & Tricks
- Special Contexts: Post-op (ERAS), Trauma, Burns, Pancreatitis.
- Key Adjuncts (Multimodal Analgesia - MMA):
- Ketamine (low-dose): 0.1-0.3 mg/kg IV; anti-hyperalgesic, useful in opioid tolerance.
- Gabapentinoids (Gabapentin, Pregabalin): Neuropathic pain component.
- IV Lidocaine: 1-2 mg/kg/hr (max 3-5 mg/kg); anti-inflammatory, Na+ channel blocker.
- Alpha-2 agonists (Dexmedetomidine, Clonidine): Opioid-sparing.
- Tricky Pains: Neuropathic pain, Opioid-tolerant patients, Opioid-Induced Hyperalgesia (OIH).
- Tricks & Strategies:
- Preventive & preemptive analgesia.
- Regional anesthesia/analgesia (nerve blocks, epidurals).
- Non-pharmacological: TENS, cryotherapy.
⭐ Low-dose ketamine infusion is a valuable adjunct in managing acute pain in opioid-tolerant patients and can prevent OIH.

High‑Yield Points - ⚡ Biggest Takeaways
- Multimodal analgesia is key: combines NSAIDs, opioids, paracetamol, and regional techniques.
- NSAIDs (e.g., Ketorolac): potent; watch for renal, GI, and bleeding risks.
- Opioids (Morphine, Fentanyl): for severe pain; monitor respiratory depression, sedation, PONV.
- Paracetamol: safe baseline analgesic; vital in multimodal regimens. Max dose 4g/day.
- Regional anesthesia (epidurals, nerve blocks): superior pain relief, opioid-sparing, better outcomes.
- PCA (Patient-Controlled Analgesia): empowers patients, effective opioid titration, improves satisfaction.
- Ketamine (low-dose) and Gabapentinoids are useful adjuncts, reducing opioid needs.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

