ERAS PreOp Intro - Foundation First
- Goal: Optimize patient physiological & psychological state before surgery.
- Aims: ↓ surgical stress response, ↓ complications, ↑ recovery speed, ↓ hospital stay.
- Core: Proactive identification & mitigation of modifiable risk factors (e.g., anemia, malnutrition, poor glycemic control).
- Emphasizes patient education, shared decision-making, and prehabilitation (exercise, nutrition).
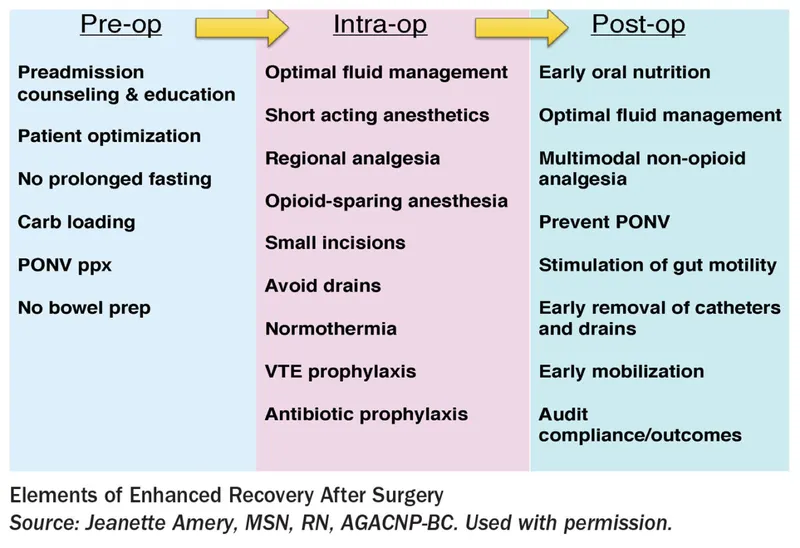
⭐ Preoperative optimization is a cornerstone of ERAS, aiming to make patients "fitter for surgery" and improve outcomes significantly across various surgical specialties an Indian context focus on resource stratification for implementation is key for NEET PG aspirants to understand practical applicability for diverse settings
Risk & Patient Prep - Spot & Support
- Spot Risks Systematically:
- Comorbidities: Cardiac, pulmonary, renal, DM (Target HbA1c < 8%).
- Functional Capacity: METs (aim > 4), 6MWT.
- Nutritional Status: Screen (MUST/NRS-2002); Albumin < 3.0 g/dL, Wt loss > 10%.
- Frailty: CFS, gait speed.
- Anemia: Hb < 10-12 g/dL.
- Support & Optimize Proactively:
- Patient Education & Shared Decisions.
- Prehabilitation: Exercise, nutrition (protein ↑), anxiety ↓.
- Smoking/Alcohol Cessation: Min 4 weeks prior. 📌 S.T.O.P. (Smoking Tobacco Optimization Program).
- Anemia Correction: Iron, EPO.
- Medication Review.
⭐ Preoperative anemia (Hb < 10 g/dL) is an independent risk factor for increased morbidity and mortality; aggressive correction is key.
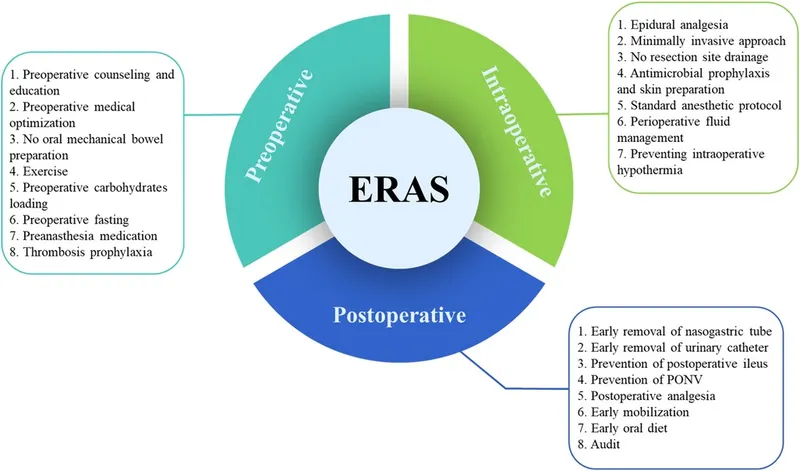
PeriOp Nutrition - Fueling Finesse
- Goal: Optimize physiological status, ↓surgical stress, ↓insulin resistance, enhance recovery.
- Carbohydrate (CHO) Loading:
- Non-diabetics: Complex CHO drink. 50g evening before & 50g (e.g., 400ml of 12.5% solution) 2 hrs pre-op.
- Benefits: ↓thirst, hunger, anxiety; preserves muscle mass; ↓LOS.
- Fasting (NPO) Guidelines (ERAS):
- Clear liquids: Up to 2 hrs pre-op (maintains hydration).
- Solids (light meal): Up to 6 hrs pre-op.
- 📌 "ERAS 2-6": 2h clear, 6h light meal.
- Glycemic Control:
- Aim for pre-op HbA1c < 8%.
- Maintain peri-op blood glucose < 180 mg/dL.
⭐ Preoperative carbohydrate loading significantly reduces postoperative insulin resistance and length of hospital stay.
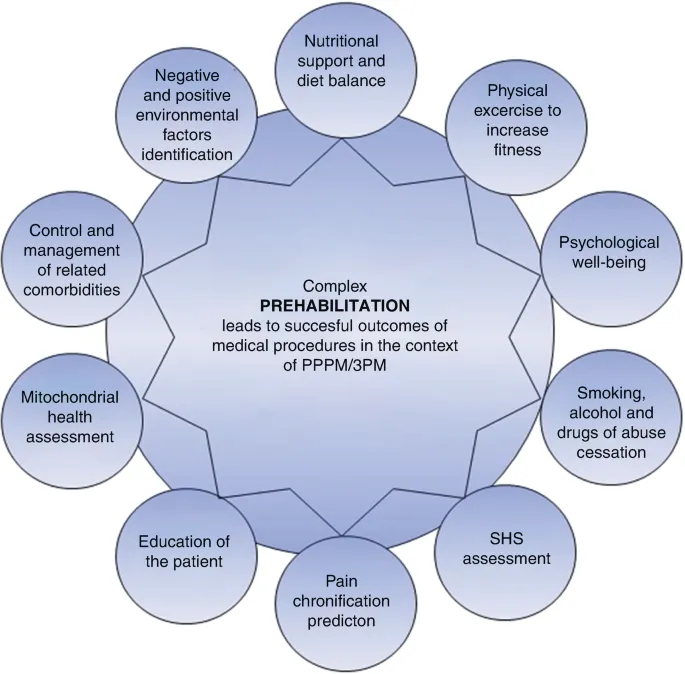
Prehab & Deficiencies - Body Boost
- Prehabilitation ("Prehab"):
- Aim: Enhance functional capacity, build physiological reserve pre-surgery.
- Key elements: Tailored exercise, nutritional support, anxiety reduction.
- Initiate ≥4 weeks before surgery for optimal benefit.
- Correct Deficiencies:
- Anemia: Screen Hb. Treat if Hb <10-12 g/dL (varies). Iron (oral/IV).
- Malnutrition: Screen (MUST/NRS-2002). High-protein diet, ONS.
- Lifestyle Changes:
- Smoking: Cessation ≥4 weeks (ideally 8 weeks) pre-op. 📌 "Quit 4 weeks, heal for weeks!"
- Alcohol: Abstain ≥4 weeks pre-op. Monitor for withdrawal.
⭐ Preoperative anemia (Hb <13 g/dL males, <12 g/dL females) is an independent risk factor for postoperative morbidity.
PreOp Medications - Med Masterclass
- Goal: Minimize risk, ensure stability.
- Continue:
- Beta-blockers (BB), Statins, Anti-epileptics.
- Thyroid meds, most Psych meds, Inhalers.
- Stop/Modify (Timing is key!):
- Antiplatelets: Aspirin (low dose often continued), Clopidogrel: stop 5-7d.
- Anticoagulants: Warfarin: stop 5d (target INR < 1.5), DOACs: stop 24-72h.
- Oral Hypoglycemics: Hold AM surgery. Metformin: hold 24-48h if contrast used.
- ACEi/ARBs, Diuretics: Hold AM surgery.
- MAOIs: Stop 2 weeks.
- Herbal meds: Stop 1-2 weeks.
⭐ Beta-blockers should be continued perioperatively in patients already on them to prevent rebound tachycardia and ischemia, especially in those with CAD.
High-Yield Points - ⚡ Biggest Takeaways
- Patient education and shared decision-making are foundational.
- Nutritional optimization, including immunonutrition, is vital for recovery.
- Smoking cessation (≥4 weeks pre-op) and alcohol abstinence are crucial.
- Anemia correction (Hb >10 g/dL) and strict glycemic control (HbA1c <7-8%) are mandatory.
- Avoid prolonged fasting; clear fluids up to 2 hours pre-op, consider carbohydrate loading.
- Prehabilitation (exercise, physiotherapy) significantly improves functional capacity.
- Medication review and optimization (e.g., anticoagulants, hypoglycemics) are essential.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

